ANTIBIOTIC
RESISTANCE AND TREND OF URINARY PATHOGENS IN GENERAL OUTPATIENTS FROM
A MAJOR URBAN CITY
(
Download pdf )
CARLOS R. KIFFER, CAIO MENDES, CARMEN P. OPLUSTIL, JORGE L. SAMPAIO
Section of Microbiology, Fleury Institute, Sao Paulo, SP, Brazil
ABSTRACT
Objective:
We assessed the antimicrobial resistance patterns of pathogens responsible
for urinary tract infections (UTI) in outpatients in São Paulo,
Brazil, as well as the Escherichia coli antimicrobial resistance trend.
Materials and Methods: Outpatients urine
cultures were collected from January 2000 to December 2003. Statistical
analysis considered positive results for one bacterial species with colony
count ≥ 100,000 CFU/mL. Stratification was done on age group and
gender. Statistical tests used included chi-square and the chi-square
test for trend to evaluate differences between susceptibility rates among
age groups and ordering in the E. coli resistance rates per year, respectively.
Results: There were 37,261 positive results
with Enterobacteriaceae isolated in 32,530 (87.3%) and Gram-positive cocci
in 2,570 (6.9%) cultures. E. coli had the highest prevalence (71.6%).
Susceptibility tests were performed in 31,716 cultures. E. coli had elevated
resistance rates (> 30%) to ampicillin, trimethoprim-sulfamethoxazole,
and tetracycline. Significant differences between age groups and ordering
among years were observed.
Conclusions: The use of trimethoprim-sulfamethoxazole
is precluded in the population studied due to elevated resistance rates
(> 30%) among most prevalent pathogens. Significant resistance rate
differences among age groups and years were observed, particularly for
fluoroquinolones. Fluoroquinolones should be used with caution. Nitrofurantoin
should be used as empirical therapy for primary, non-complicated urinary
tract infections.
Key
words: urinary tract infections; drug therapy; drug resistance;
Escherichia coli
Int Braz J Urol. 2007; 33: 42-9
INTRODUCTION
Controlling
the increase in antimicrobial resistance is a major issue confronting
organized health care today. Although multiple factors play a role in
this problem, the selective pressures of inappropriate and widespread
use of antibiotics are considered major contributors. A few studies have
analyzed the antimicrobial resistance patterns of bacteria causing community
acquired urinary tract infections (UTI) (1-5). International resistance
surveillance studies have shown an increasing resistance pattern against
commonly used community antimicrobials (1-6). Surveillance programs may
be valuable tools and may offer important information on bacterial resistance
trends either per geographical location or per disease type in community
or hospital settings (7,8). However, surveillance programs must be stratified
by region and population, not to incur in general and mostly non-applicable
conclusions. Regional studies analyzing community acquired UTI and their
antimicrobial resistance pattern are currently needed in many areas, particularly
major urban centers worldwide because of their specificities on antimicrobial
usage density.
Thus, the goal of this study was to assess
the most frequent pathogens responsible for urinary tract infections (UTI)
in outpatients and their antimicrobial resistance pattern in São
Paulo, Brazil, through consecutive urine samples collected during a four-year
period, from January 2000 to December 2003. Additionally, the study also
aimed at identifying possible resistance trends.
MATERIALS AND METHODS
From
January 2000 to December 2003, routine urine cultures were consecutively
collected at a private medical diagnostic center from patients residing
in the São Paulo city area, Brazil. The city is located in Southeast
Brazil and has around 10,000,000 inhabitants. The private medical diagnostic
center has 12 collection sites distributed over the city area and serves
mostly the population with access to private health care system within
this area. All cultures were collected from outpatients with medical requests
through midstream urine samples, except for children below 2 years old,
who had collections by sterile collector vials. More than one culture
from the same patient was only included in the database if collected more
than 30 days apart.
Urine samples were plated on cystine-lactose-electrolyte-deficient
(CLED), MacConkey and citrate agars (deep slide methodology) up to 20
minutes after collection and then incubated at 37ºC for 18 to 24
hours. Negative urine samples (refrigerated aliquot) after initial 24
hours incubation with abnormal leukocyte count (≥ 30,000/mL) or
bacteriuria on direct non-centrifuged urine microscopic examination were
also cultivated on blood agar and incubated for an additional 24 hours.
Identification of all isolates was done
by VITEK (bioMérieux Inc., Durham, North Carolina, USA) automated
system. Susceptibility testing was performed according to medical requests
and was done by VITEK (bioMérieux, Inc.) automated system for Enterobacteriaceae
and disk diffusion test (Oxoid, Basingstoke, Hampshire, UK) were used
for Gram-positive bacteria and Pseudomonas aeruginosa. The following antimicrobials
were tested against Gram-negative isolates: ampicillin, ceftriaxone, cephalothin,
ciprofloxacin, gentamicin, nalidixic acid, nitrofurantoin, norfloxacin,
tetracycline, and trimethoprim-sulfamethoxazole. The following antimicrobials
were tested against Gram-positive isolates: ciprofloxacin, clindamycin,
erythromycin, nitrofurantoin, oxacillin, penicillin G, tetracycline, trimethoprim-sulfamethoxazole,
and vancomycin (results not fully shown). Interpretative criteria used
were for the respective years CLSI (formerly NCCLS) documents (9-12).
Only positive results with one bacterial
species and a colony count ≥ 100,000 CFU/mL were considered for
descriptive and inferential analysis. Stratification by gender and age
was done, and age groups were divided as following: < 4 years-old;
≥ 4 and < 13 years-old; ≥ 13 and < 60 years-old; and
≥ 60 years-old. In order to investigate possible factors associated
to resistance, E. coli, as the most prevalent microorganism, and its susceptibility
rates to ampicillin, ciprofloxacin, nitrofurantoin, norfloxacin, tetracycline,
and trimethoprim-sulfamethoxazole were defined as the dependent variables.
Age groups were defined as the independent variables. The chi-square test
was used to identify differences between the observed E. coli susceptibility
rates of the six antimicrobials among all four age groups. Additionally,
the Fisher exact test was used to evaluate differences between the observed
resistance rates between < 13 and ³ 60 years old groups (13).
An exact 2-tailed P value was computed, as well as the confidence intervals
around the differences using the normal approximation. Finally, the chi-square
test for trend, as described by Altman 1991 (13), was applied to compare
ordering between E. coli resistance rates to ampicillin, ciprofloxacin,
nitrofurantoin, norfloxacin, tetracycline, trimethoprim-sulfamethoxazole,
and nalidixic acid among the four years (2000 to 2003). P values below
0.05 were considered significant for all tests.
RESULTS
Frequency
of Microorganism Isolation
There were 37,261 positive results and Enterobacteriaceae
were isolated in 32,530 (87.3%) cultures, followed by Gram-positive cocci
with 2,570 (6.9%). E. coli presented the highest prevalence (71.6%), followed
by Klebsiella pneumoniae (6.4%), Proteus mirabilis (6.1%), and Enterococcus
faecalis (4.8%), Pseudomonas aeruginosa (1.8%), Staphylococcus saprophyticus
(1.6%), Enterobacter aerogenes (1.6%), Enterobacter cloacae (1.1%), and
others (5.0%).
Among the positive cultures, 88.8% belonged
to female and 11.2% to male patients. Among the 33,090 UTI in females,
59.2% was detected in the population of ≥ 13 and < 60 years old.
On the other hand, among the 4,171 UTI in males, 54.2% was detected in
the population of ≥ 60 years old. The age group of < 4 years
old contributed with 13.0% of cases in the male and with 4.4% in the female
population.
Table-1 shows the total amount of microorganisms
isolated per age group and gender. Overall, E. coli was the most prevalent
isolate in all groups. K. pneumoniae, although with a significant prevalence,
was more commonly isolated in the population ≥ 13 years old. P.
mirabilis was more prevalent in the population ≥ 13 years old, although
the population < 4 years old also presented a significant prevalence.

Susceptibility Patterns
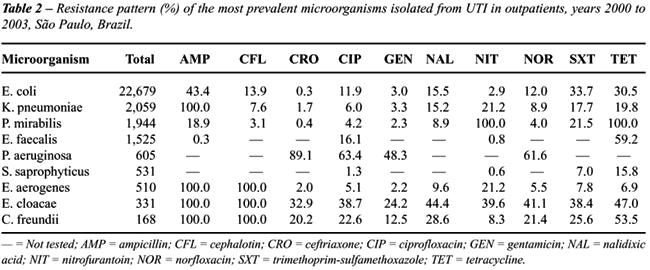
Susceptibility tests were performed in 31,716
cultures. The susceptibility pattern of the most prevalent microorganisms
isolated from UTI in outpatients is described in Table-2. E. coli presented
resistance rate to ampicillin of 43.4%, followed by 33.7% to trimethoprim-sulfamethoxazole
and by 30.5% to tetracycline. Ceftriaxone was the most active agent against
E. coli (99.7% susceptible), with an extremely low resistance rate (0.3%).
Also, E. coli presented low resistance rates to gentamicin and nitrofurantoin
(3.0% and 2.9%, respectively). For K. pneumoniae, the second highest prevalent
pathogen, significant resistance rates were noted to nitrofurantoin, tetracycline,
trimethoprim-sulfamethoxazole and nalidixic acid (21.2%, 19.8%, 17.7%,
and 15.2% respectively), with low resistance rates to ceftriaxone, gentamicin,
and ciprofloxacin (1.7%, 3.3% and 6.0%, respectively). For P. mirabilis,
the third most frequently isolated, considerable rates were observed only
to trimethoprim-sulfamethoxazole and ampicillin (21.5% and 18.9%), apart
from the intrinsic resistances to nitrofurantoin and tetracycline.
Statistics
E. coli was the most frequently isolated
pathogen in all age groups (22,693) and the majority had susceptibility
tests performed (22,679). Table-3 shows E. coli resistance rates to ampicillin,
ciprofloxacin, nitrofurantoin, norfloxacin, tetracycline, trimethoprim-sulfamethoxazole
and the chi-square test with P values for comparisons of proportions among
age groups.

Table-4 shows a test intended to identify
possible ordered resistance rates of the most prevalent microorganism
during the study period. The chi-square test for trend was performed for
comparisons of the ordered differences between E. coli resistance rates
to the described antimicrobials among the four years surveyed, i.e. 2000
to 2003.

COMMENTS
Uncomplicated
UTI are amongst the most common infections in outpatient women with significant
morbidity and health costs (14). This study did not discriminate among
uncomplicated and complicated UTI in the sample evaluated and this could
lead to a case mix with confounding variables in terms of resistance patterns.
However, it should be noted that the vast majority of the samples collected
from adults correspond to clean-catch midstream urine and that it is a
common practice in our area to order urine cultures for uncomplicated
UTI, since results are available no later than 48 hours after sample collection.
Additionally, as stated, only one urine sample per patient in a 30-day
period was entered in the database, diminishing the possibility of frequent
UTI recurrences.
Although the spectrum of agents causing
UTI in outpatients is relatively constant, their susceptibility patterns
are different in different environments. In the present study, among the
22,679 E. coli tested, the resistance rate to trimethoprim-sulfamethoxazole
was 33.7%. Additionally, 11.9% of the E. coli were resistant to ciprofloxacin,
12.0% to norfloxacin and 15.5% to nalidixic acid. Amongst the gram-positive
isolates, E. faecalis presented considerable resistance to ciprofloxacin
(16.1%). Although with a different methodology, the present study demonstrated
similar E. coli resistance rates when compared to the Hummers-Pradier
clinical study (15); nevertheless E. faecalis showed a marked difference
in the resistance rate to ciprofloxacin (82.8%) if compared to the same
study (15). There were also significant differences in the E. coli resistance
rates to trimethoprim-sulfamethoxazole in comparison to recent studies
from other environments, which reported rates from 15-25% in a surveillance
(6) and a clinical study (16), and from around 2-15% on isolates with
a single cross-resistance in another surveillance study (17). This study
showed that nitrofurantoin was very active against isolates of E. coli
and E. faecalis but not against K. pneumoniae, similar to other studies
(6,15-18).
Furthermore, the present study detected
that resistance rates of E. coli, P. mirabilis and K. pneumoniae to ceftriaxone
were 0.3%, 0.4% and 1.7%, respectively. A possible explanation to this
fact might be the presence of Extended Spectrum Beta-Lactamases (ESBL)
in these strains (all of them in the age groups over 4 years old - data
not shown). This finding suggests the existence of non-community acquired
infections among the population under surveillance (possibly but not exclusively
nursing homes and home-care facilities), which may have tests performed
in the present centre. It is worth to mention that ceftriaxone is not
the best screening drug for ESBLs and this was not the objective of this
study. However, this is a relevant finding, since it might indicate that
infections with these types of strains are being detected in outpatients
in Brazil - although further confirmation and stratification for risk
factors are needed.
As seen in Table-3, E. coli resistance rates
for ciprofloxacin and norfloxacin were 24.3% and 24.4% respectively in
the age group of ≥ 60 years old, while it was below 8% for both
drugs in all other age groups. It was also noticed a variation of E. coli
resistance rates to ampicillin and trimethoprim-sulfamethoxazole between
age groups, with higher rates seen in the age groups below 13 years old.
As for tetracycline, E. coli resistance rates ranged from 26.6% to 37.3%,
showing generally more elevated resistance levels among all age groups;
although with a particular higher resistance rate seen in the age group
≥ 60 years old. Finally, nitrofurantoin showed low resistance rates
in all age groups, with a higher rate observed for this drug in the group
≥ 60 years old (5.9%).
Additionally, the chi-square test for trend
shown in Table-4 has demonstrated apparently stable resistance rates to
nitrofurantoin, ampicillin, and trimethoprim-sulfamethoxazole (P >
0.5), though extremely higher rates to the latter two drugs. On the other
hand, increasing resistance rates to ciprofloxacin, norfloxacin, and nalidixic
acid (P < 0.0001) have been detected, with approximately 9.0% resistance
to ciprofloxacin and norfloxacin in 2000 and 14.0% in 2003. Surprisingly,
an ordered decline of the resistance rate to tetracycline was observed,
with 35.0% in 2000 and 28.9% in 2003 (P < 0.0001). These data may have
many interpretations, among them a possible changing pattern of antimicrobial
use in the population within the period surveyed, with increased use of
fluoroquinolones and decreased use of other drugs, particularly in the
older population. However, if these findings are due to other factors
different from the suggested ones, such as clonal dissemination, as described
by Manges et al. (19), or methodological limits, remains to be determined
by further studies.
A final remark must be made on the use of
routine antimicrobial susceptibility testing data based on breakpoint
concentrations and the limits imposed by the method. Although this has
been used before and is acceptable (15), detailed shifts or subtle differences
in susceptibility rates may be lost by its use, particularly for agents
where susceptible isolates may cluster near a breakpoint. However, it
is the opinion of the authors that this would be more problematic in cross-sectional
studies, where trends cannot be analyzed and, thus, the same method cannot
be compared throughout a certain period.
CONCLUSIONS
Elevated resistance rates in E. coli from urinary tract infections in outpatients to ampicillin, trimethoprim-sulfamethoxazole, and tetracycline preclude the use of these drugs for empirical treatment in the environment evaluated for all age groups. Instead, nitrofurantoin should be used as empirical therapy for primary, non-complicated urinary tract infections (except in patients with impaired renal function) in outpatients of the greater São Paulo area, Brazil. Thus, there is sufficient indication showing that the E. coli resistance trend for fluoroquinolones is increasing, and although not clarified by this study, possibly linked to higher use of this drug class either by the individual and/or by the population. Due to this trend, this class should be used with caution, particularly if no microbiological documentation is available. At last, resistance prevalence studies may be a useful tool for guiding antimicrobial therapy and helping curb resistance due to selective pressure in community-acquired infections, especially UTI.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Gupta K, Hooton TM, Stamm WE: Increasing antimicrobial resistance and the management of uncomplicated community-acquired urinary tract infections. Ann Intern Med. 2001; 135: 41-50.
- Zhanel GG, Karlowsky JA, Harding GK, Carrie A, Mazzulli T, Low DE, et al.: A Canadian national surveillance study of urinary tract isolates from outpatients: comparison of the activities of trimethoprim-sulfamethoxazole, ampicillin, mecillinam, nitrofurantoin, and ciprofloxacin. The Canadian Urinary Isolate Study Group. Antimicrob Agents Chemother. 2000; 44: 1089-92.
- Goldstein FW: Antibiotic susceptibility of bacterial strains isolated from patients with community-acquired urinary tract infections in France. Eur J Clin Microbiol Infect Dis. 2000; 19: 112-7.
- Bukharie HA, Saeed IM: Antimicrobial Resistance Among Pathogens Causing Acute Uncomplicated UTIs. Infect Med. 2001; 18: 358-62.
- Gupta K, Scholes D, Stamm WE: Increasing prevalence of antimicrobial resistance among uropathogens causing acute uncomplicated cystitis in women. JAMA. 1999; 281: 736-8.
- Jones RN, Kugler KC, Pfaller MA, Winokur PL: Characteristics of pathogens causing urinary tract infections in hospitals in North America: results from the SENTRY Antimicrobial Surveillance Program, 1997. Diagn Microbiol Infect Dis. 1999; 35: 55-63.
- Jones RN: Detection of emerging resistance patterns within longitudinal surveillance systems: data sensitivity and microbial susceptibility. MYSTIC Advisory Board. Meropenem Yearly Susceptibility Test Information Collection. J Antimicrob Chemother. 2000; 46 Suppl T2: 1-8.
- Masterton RG: Surveillance studies: how can they help the management of infection? J Antimicrob Chemother. 2000; 46 Suppl T2:53-8.
- National Committee for Clinical Laboratory Standards. Methods for dilution antimicrobial susceptibility tests for bacteria that grow aerobically, Wayne, Pa; 2000. NCCLS Document M100-S10.
- National Committee for Clinical Laboratory Standards. Methods for dilution antimicrobial susceptibility tests for bacteria that grow aerobically, Wayne, Pa; 2001. NCCLS Document M100-S11.
- National Committee for Clinical Laboratory Standards. Methods for dilution antimicrobial susceptibility tests for bacteria that grow aerobically, Wayne, Pa; 2002. NCCLS Document M100-S12.
- National Committee for Clinical Laboratory Standards. Methods for dilution antimicrobial susceptibility tests for bacteria that grow aerobically, Wayne, Pa; 2003. NCCLS Document M100-S13.
- Altman DG: Practical Statistics for Medical Research. London, Chapman & Hall. 1991, pp. 611.
- Foxman B, Barlow R, D’Arcy H, Gillespie B, Sobel JD: Urinary tract infection: self-reported incidence and associated costs. Ann Epidemiol. 2000; 10: 509-15.
- Hummers-Pradier E, Koch M, Ohse AM, Heizmann WR, Kochen MM: Antibiotic resistance of urinary pathogens in female general practice patients. Scand J Infect Dis. 2005; 37: 256-61.
- Alos JI, Serrano MG, Gomez-Garces JL, Perianes J: Antibiotic resistance of Escherichia coli from community-acquired urinary tract infections in relation to demographic and clinical data. Clin Microbiol Infect. 2005; 11: 199-203.
- Kahlmeter G, Menday P: Cross-resistance and associated resistance in 2478 Escherichia coli isolates from the Pan-European ECO.SENS Project surveying the antimicrobial susceptibility of pathogens from uncomplicated urinary tract infections. J Antimicrob Chemother. 2003; 52: 128-31.
- Farrell DJ, Morrissey I, De Rubeis D, Robbins M, Felmingham D: A UK multicentre study of the antimicrobial susceptibility of bacterial pathogens causing urinary tract infection. J Infect. 2003; 46: 94-100.
- Manges AR, Johnson JR, Foxman B, O’Bryan TT, Fullerton KE, Riley LW: Widespread distribution of urinary tract infections caused by a multidrug-resistant Escherichia coli clonal group. N Engl J Med. 2001; 345: 1007-13.
____________________
Accepted
after revision:
October 11, 2006
_______________________
Correspondence address:
Dr. Carlos R.V. Kiffer
Instituto Fleury, Microbiologia
Avenida General Valdomiro de Lima 508
São Paulo, SP, 04344-903, Brazil
Fax: + 55 11 5014-7601
E-mail: carlos.kiffer@fleury.com.br
This
is an important paper providing susceptibility data on community acquired
urinary tract infections (UTI) from a large population. Such information
is necessary for working out recommendations on empirical treatment of
UTI. Resistant bacterial strains are frequently brought to urology departments
by patients with complicated UTI. Therefore, susceptibility data from
primary health care is also important information for urologists.
From
a European perspective, it is interesting to note that frequently used
drugs like mecillinam and fosfomycin trometamol still seem to be unused
therapeutic weapons.
Dr. Truls
E. Bjerklund Johansen
Chair, European Society for Infections in Urology
Telemark Central Hospital, Urology Section
Porsgrunn, Norway
E-mail: tebj@sthf.no
EDITORIAL COMMENT
Urinary tract infections are among the most common community acquired infections. Whereas in nosocomial urinary tract infections surveillance is frequently performed around the world or even mandatory in some countries, data on outpatients’ urinary tract infections are still scarce. This study investigated more than 37,000 urinary isolates of outpatients in the Sao Paulo urban area. Antibiotics such as trimethoprim/ sulfamethoxazole exhibited high resistant rates, which precludes the use of this substance as primary empiric treatment for outpatient urinary tract infections. Additionally there was a significant increase in fluoroquinolone resistance over the last years to levels where treatment failures might occur in significant cases. Studies like this will help to improve and tailor empiric antibiotic treatment for urinary tract infections in the area of Sao Paulo.
Dr. Florian
M. E. Wagenlehner
Department of Urology
Justus-Liebig-University Giessen
Giessen, Germany
E-mail: wagenlehner@aol.com