PROSTATE
SPECIFIC ANTIGEN LEVELS FOLLOWING TRANSURETHRAL RESECTION OF THE PROSTATE
(
Download pdf )
ROBERTO C. FONSECA, CRISTIANO M. GOMES, ELTON B. MEIRELES, GERALDO C. FREIRE, MIGUEL SROUGI
Division of Urology, University of Sao Paulo School of Medicine, Sao Paulo, Brazil
ABSTRACT
Objective:
Determine how serum prostate-specific antigen (t-PSA) levels and free
PSA (f/t PSA) ratio change following transurethral resection of the prostate
(TURP).
Materials and Methods: Thirty men with a
mean age of 67.0 ± 4.2 years (range 46 to 84 years) underwent TURP
for BPH between May 2005 and October 2005. Preoperative assessment included
symptom evaluation with the International Prostate Symptom Score (I-PSS)
and the prostate volume estimation by transrectal ultrasound. Total PSA
and f/t PSA ratio were assessed before the procedure, as well as 30, 60
and 180 days after the TURP.
Results: Clinical improvement after TURP,
reflected by I-PSS score, was demonstrated as early as 30 days and remained
stable until the end of the follow-up. Mean t-PSA declined 71% after TURP
and 60 days after surgery the reduction reached its peak, stabilizing
afterwards. It varied from 6.19 ± 7.06 ng/mL before surgery to
1.75 ± 1.66 ng/mL on day 60 (p < 0.001). The mean baseline f/t
PSA ratio was 18.2% ± 3.4% and was not significantly changed at
any given time point in the postoperative period (p = 0.91). There were
also no statistically significant differences in t-PSA or f/t PSA between
patients with and without prostatitis at any time point (p = 0.23). Resected
prostate fragments weighed 29.9 ± 19.6 g, corresponding to 39.1%
of the estimated preoperative prostate volume. Each gram of tissue resected
decreased PSA by 0.15 ± 0.11 ng/mL, while 1% prostate volume resected
led to a reduction of 2.4% ± 0.4% in serum PSA from baseline.
Conclusions: PSA decreases drastically in
patients who undergo TURP. These low levels stabilize within 60 days after
surgery. The f/t PSA ratio did not change, and the finding of chronic
prostatitis did not affect the levels of these variables.
Key
words: prostate-specific antigen; benign prostatic hyperplasia;
transurethral resection of prostate
Int Braz J Urol. 2008; 34: 41-8
INTRODUCTION
Benign
prostatic hyperplasia (BPH) is the most prevalent prostatic pathology,
and transurethral resection of the prostate (TURP) is one of the surgeries
most commonly performed by urologists, and considered the gold standard
for the surgical treatment of BPH.
Prostate-specific antigen (PSA) is a tumor
marker whose role in the diagnosis and follow-up of patients with prostatic
diseases has continuously evolved. PSA behavior after transurethral resection
of the prostate is crucial during patient follow-up. It is known that
serum PSA levels increase temporarily in the first few days following
a TURP procedure, decreasing gradually afterwards and reaching stable
values within 3-6 months (1). However, serum PSA level stabilization apparently
depends on several aspects, namely, patient’s age, PSA levels before
surgery, prostate volume and prostate volume resected. Thus, there is
not a cutoff value established for normal PSA in patients who undergo
TURP (2,3).
Although different factors may affect PSA
reduction after the procedure, an approximate 72% decrease from baseline
is expected, even with a proportionally lower reduction in prostate volume
(2). This occurs because resection affects basically the transition zone
of the prostate, which produces more PSA per gram of tissue (4).
Total serum PSA is found in its free form
and bound to plasma proteins. Clinically, both total PSA (t-PSA) and free
PSA ratio (f/t PSA) are important for the diagnosis and follow-up of prostatic
diseases. In the past few years, great importance has been attributed
to free PSA, which is usually reduced in patients with adenocarcinoma.
Previous studies suggested that f/t PSA ratio tends to remain stable after
TURP in patients with benign prostatic hyperplasia (2,5).
Prostatic inflammation has probably a not
clearly understood impact on PSA levels in the postoperative period. Although
many studies suggest that the presence of prostatic inflammation can contribute
to increasing total PSA levels, the mechanism by which such histological
changes induce the prostatic acinus marker to move to the systemic circulation
is still controversial (6).
In this study, we analyzed how total PSA
and f/t PSA ratio change with time in patients with BPH who undergo TURP,
as well as the impact of prostatitis on these parameters, in an attempt
to contribute to clarifying some of these important aspects concerning
patient follow-up.
MATERIALS AND METHODS
During
one year, 40 patients with lower urinary tract symptoms associated with
benign prostatic hyperplasia were selected to undergo TURP and evaluated
prospectively. Preoperative assessment included clinical history, physical
examination of the prostate, the International Prostate Symptom Score
(I-PSS), urine culture, measurement of prostatic volume by transrectal
ultrasound of the prostate (TRUS), and determination of t-PSA and f/t
PSA serum levels.
Patients with suspected abnormality on digital
rectal examination or PSA ≥ 4.0 ng/mL underwent prostate biopsy.
Patients with adenocarcinoma were excluded from the study, as well as
those with atypical small acinar proliferation (ASAP) or intra-epithelial
neoplasia, patients on finasteride in the last 6 months, patients with
urinary retention, patients with neurological diseases that could have
an impact on the urinary tract, and those with history of pelvic radiotherapy
or lower urinary tract surgeries. Patients with urinary infection were
treated, and their PSA levels were measured 30 days after a negative urine
culture.
The study protocol was approved by the hospital’s
Research Ethics Committee. All patients were duly informed about the study
and signed the informed consent form. Ten patients were excluded from
the study because they did not return for postoperative assessment.
The TURP was performed according to the
standard technique, and the fragments were immediately weighed and further
analyzed by the same pathologist.
Outcome measures were IPSS, t-PSA and f/t
PSA ratio after 1,3 and 6 months. These parameters in different time points
were correlated with preoperative prostatic volume, total volume of tissue
resected, percentage of volume resected and the histopathological finding
of chronic prostatitis.
The analysis of variance test (ANOVA) and
the Turkey’s test were used to compare serum PSA level variations
at different time points. The Pearson’s correlation coefficient
was used to evaluate the association between patients’ age and the
reduction of PSA levels after TURP. The Student’s t-test was used
to compare PSA level progression in patients with and without chronic
prostatitis. The significance level adopted was 5%. Statistical data were
analyzed using commercially available software.
RESULTS
Patients’
ages ranged from 46 to 84 years (mean 67.0 ± 4 years). Preoperative
IPSS ranged from 18 to 29, mean 22.5 ± 2.9.
Preoperative t-PSA ranged from 0.79 ng/mL
to 33.46 ng/mL, mean 6.19 ± 7.06 ng/mL. Preoperative f/t PSA ratio
ranged from 8.3% to 39.0%, mean 18.2 ± 4.0%.
Baseline prostatic volume, as measured by
TRUS, ranged from 29.0 cc to 130.0 cc, mean 71.8 ± 24.0 cc. Prostate
fragments resected weighed from 11 g to 102 g, mean 29.9 ± 19.6
g. In terms of percentage, the volume resected ranged from 21.6% to 78.4%,
mean 39.1% (Table-1).

On the histopathological examination, 12
patients (40%) were diagnosed with both benign prostatic hyperplasia and
chronic prostatitis, and 18 patients (60%) were diagnosed with benign
prostatic hyperplasia only. There were no statistically significant differences
between patients with and without prostatitis regarding age, IPSS, t-PSA,
f/t PSA ratio and prostate weight resected (Table-2).

Before surgery, mean I-PSS was 22.5 ±
2.9. It changed to 12.6 ± 2.0 on day 30, 11.6 ± 1.6 on day
60, and 11.3 ± 1.8 on day 180 following surgery. At all time points
assessed after surgery, I-PSS values were lower than in the preoperative
period (p < 0.001). There were no significant differences in mean IPSS
after 1, 3 and 6 months (Figure-1).

Before surgery, mean t-PSA was 6.19 ng/mL
± 7.06 ng/mL, decreasing to 2.27 ± 2.20 ng/mL on day 30
(63% reduction from baseline), 1.75 ± 1.66 ng/mL (71% reduction)
on day 60, and 1.79 ± 1.26 ng/mL (71% reduction) on day 180 following
surgery. A significant difference was observed when preoperative t-PSA
was compared with postoperative values on days 30, 60 and 180 (p <
0.001 for all comparisons). A significant difference was also found when
t-PSA on day 30 was compared with t-PSA on days 60 and 180 in the postoperative
period (p = 0.035). There was no statistically significant difference
between mean t-PSA on days 60 and 180 (Figure-2). Age was not associated
with the decline of PSA levels after TURP at all time points assessed
(p = 0.151).

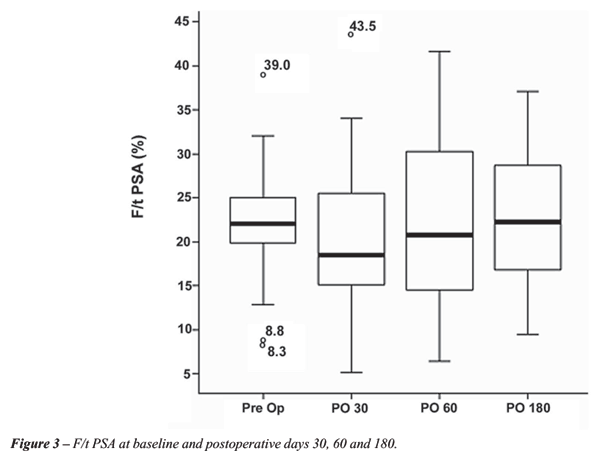
Before surgery, mean f/t PSA ratio was 18.2%
± 3.4%, while in the postoperative period, it changed to 17.8 ±
8.6% on day 30, 18.7 ± 9.9% on day 60, and 21.0 ± 7.5% on
day 180 (Figure-3). There was no significant difference between preoperative
and postoperative f/t PSA ratios at any time point in the postoperative
period (p = 0.910).
Among the patients with prostatitis, preoperative
t-PSA was 8.1 ± 10.2 ng/mL, changing to 2.4 ± 2.3 ng/mL,
1.6 ± 1.0 ng/mL and 1.9 ± 0.9 ng/mL, respectively, on days
30, 60 and 180 following surgery. Among the patients without prostatitis,
t-PSA was reduced from 4.9 ± 3.7 ng/mL to 2.2 ± 2.2 ng/mL,
1.8 ± 2.0 ng/mL and 1.7 ± 1.5 ng/mL, respectively, on days
30, 60 and 180 (Figure-4). There was no statistically significant difference
on t-PSA reduction between patients with and without prostatitis (p =
0.110).

Similarly, f/t PSA ratios in patients with
prostatitis did not differ significantly, at any moment, from f/t PSA
ratios in patients without prostatitis.
In absolute values, the average reduction
in t-PSA (measured at PO 60) was 4.44 ± 6.9 ng/mL, corresponding
to a 71 ± 22.8% reduction compared to baseline. Mean weight of
prostatic tissue resected in the TURP was 29.9 ± 19.6 g, corresponding
to 39.2 ± 13.8% of the estimate ultrasound preoperative prostate
volume. Based on these data, each gram of prostatic tissue resected caused
a mean reduction in total serum PSA of 0.14 ± 0.11 ng/mL, while
1% prostate volume resected led to a reduction of 2.4 ± 0.4% in
serum PSA from baseline.
COMMENTS
Benign
prostatic hyperplasia is one of the most frequent pathologies affecting
men, and its prevalence rises progressively after the age of 40. Transurethral
resection of the prostate is one of the surgeries most performed in men
aged above 50 years. Its effectiveness in relieving symptoms in BPH patients
has been extensively documented, and it is considered the gold standard
for the treatment of BPH (7).
PSA is a valuable tool in the follow-up
of these patients, but it is unknown what is the exact behavior of this
marker following TURP; it probably depends on several factors. Vesey et
al. (3) published one of the first studies evaluating the impact of TURP
on PSA levels. They found a correlation between prostate size and preoperative
PSA, noting that there is a temporary rise in PSA levels in the first
few days following surgery. Oesterling et al. (8) published similar results,
suggesting that one should wait four to six weeks after TURP to make new
PSA measurements. Aus et al. (1) measured PSA levels before surgery and
three months after TURP in 190 patients with BPH. Mean PSA decreased 70%.
After the TURP, 90% of the patients had PSA < 4 ng/mL and 98% had PSA
< 10 ng/mL. The authors concluded that PSA levels should be kept below
4 ng/mL following TURP for BPH.
In a retrospective analysis of patients
who developed prostate adenocarcinoma after TURP for BPH, Wolff et al.
(9) noted that these patients stabilized their PSA levels above 2.0 ng/mL.
Thus, they proposed that patients with either PSA > 2.0 ng/mL or an
early rise in PSA following TURP should be checked for prostate cancer.
The population studied in this series was
similar to the ones in most of the previous studies in terms of age, symptom
severity, free and total PSA, prostate weight and prostate weight resected.
Clinical improvement observed following TURP, as measured by I-PSS, was
quite significant. One month after surgery, the mean reduction of I-PSS
was 44%, stabilizing around 50% within 60 days. Such variation in I-PSS
following TURP is consistent with the results reported by other authors
(10,11).
In this study, mean PSA before surgery was
6.19 ng/mL. Thirty days after TURP, it decreased to 2.27 ng/mL (63%).
After 60 days, it was reduced to 1.75 ng/mL (71% reduction), stabilizing
at this level until day 180. This indicates that t-PSA measurement before
60 days may not reflect postoperative PSA nadir, so it is necessary to
wait at least 2 months after surgery. Apparently, the low PSA levels found
60 days after surgery are sustained for years, resulting in a population
with serum markers similar to those seen in men who did not develop BPH
(12).
In this study, f/t PSA ratio did not change
following surgery. This observation is consistent with literature findings,
which did not show significant variation after TURP (2). In benign prostatic
hyperplasia, t-PSA is mainly produced in the transition zone (4). Free
PSA is produced in the same proportion in both transition and peripheral
zones in these patients. As the transition zone is resected during TURP,
there is a significant reduction in t-PSA, but not in free PSA. As free
PSA is not altered after TURP, this parameter can be used to monitor patients
after surgery, similarly to what is done in the normal population (2).
Prostate inflammation is a common histological
finding in patients with symptomatic BPH without symptoms of chronic prostatitis
or history of acute prostatitis. Clinical significance of chronic prostatitis
in patients with BPH and its impact on PSA levels are not fully understood
(13). Kiehl et al. (6) studied the effect of chronic prostatitis on PSA
levels and demonstrated that, when the inflammatory process reaches glandular
epithelial cells, serum PSA levels rise above cutoff values. They also
noted that increased PSA levels were directly proportional to the severity
of the inflammatory process. This increase in total prostate-specific
antigen levels is well established in literature in patients with acute
prostatitis, but there are controversies regarding chronic prostatitis,
whose influence on PSA levels is not fully understood (14,15). In this
study, 12 (40%) patients had histologically defined chronic prostatitis.
There was no difference between patients with and without prostatitis
concerning age, symptom severity (as measured by I-PSS), mean t-PSA and
f/t PSA. The comparison of t-PSA and f/t PSA levels in patients with and
without prostatitis on days 30, 60 and 180 following surgery did not show
significant differences between the groups. However, due to the limited
size of the studied population, only compelling differences would have
been shown and we cannot affirm that the presence of chronic prostatitis
does not affect serum t-PSA and f/t PSA levels before and after TURP.
Additionally, we did not evaluate the epithelial cell inflammation and
the severity of the inflammatory process, which, according to Kiehl et
al., (4) are the main aspects of chronic prostatitis that can affect PSA.
Stamey et al. (16), estimated that each
gram of prostatic tissue resected reduces PSA levels by 0.3 ng/mL. Lloyd
et al. (17) analyzed preoperative prostate volume, adenoma volume and
the amount of tissue resected, finding a reduction of 0.09 ng/mL in serum
PSA. We found a reduction of 0.14 ng/mL ± 0.2 ng/mL per gram of
prostatic tissue resected in our patients. Marks et al. (5) found a mean
reduction of 0.11 ng/mL in PSA per gram of prostatic tissue resected.
The differences among different series appear to be secondary to differences
in patient populations as well as technical changes in PSA measurement
methods, which used to be enzymatic, but have changed to radioimmunoassay
in the last 15 years.
In terms of percentage, TURP has led to
a 71% decrease in PSA in our series, corresponding to a mean reduction
of 2.4% per each 1% of prostate volume resected. We did not find in medical
literature the estimates of PSA reduction based on the percentage of prostatic
tissue resected, and we believe it could be a quite useful parameter because
it allows for the prediction of mean PSA reduction based on two parameters
that may independently affect postoperative PSA, namely, the preoperative
prostate volume and the prostate volume resected.
CONCLUSIONS
Our results confirm that PSA levels are clearly reduced after TURP, stabilizing after 2 months. Free PSA does not change after surgery, and the presence of chronic prostatitis does not affect postoperative progression of t-PSA and f/t PSA levels. There is not an absolute serum PSA value below which patients undergoing TURP can be surely free of developing cancer, because postoperative PSA depends on several factors like preoperative PSA, prostate volume and prostate volume resected. However, PSA reduction may be estimated based on preoperative prostate volume and prostate volume resected.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Aus G, Bergdahl S, Frosing R, Lodding P, Pileblad E, Hugosson J: Reference range of prostate-specific antigen after transurethral resection of the prostate. Urology. 1996; 47: 529-31.
- Recker F, Kwiatkowski MK, Pettersson K, Piironen T, Lummen G, Huber A, et al.: Enhanced expression of prostate-specific antigen in the transition zone of the prostate. A characterization following prostatectomy for benign hyperplasia. Eur Urol. 1998; 33: 549-55.
- Vesey SG, Goble NM, Stower MJ, Hammonds JC, Smith PJ: The effects of transurethral prostatectomy on serum prostate specific antigen. Br J Urol. 1988; 62: 347-51.
- Scattoni V, Raber M, Montorsi F, Da Pozzo L, Brausi M, Calori G, et al.: Percent of free serum prostate-specific antigen and histological findings in patients undergoing open prostatectomy for benign prostatic hyperplasia. Eur Urol. 1999; 36: 621-30.
- Marks LS, Dorey FJ, Rhodes T, Shery ED, Rittenhouse H, Partin AW, et al.: Serum prostate specific antigen levels after transurethral resection of prostate: a longitudinal characterization in men with benign prostatic hyperplasia. J Urol. 1996; 156: 1035-9.
- Khiel R, Lemos AD, Stavalle JN, Ortiz V: Correlation between chronic prostatitis and prostate-specific antigen values. Int Braz J Urol. 2001; 27: 42-5.
- AUA Practice Guidelines Committee: AUA guideline on management of benign prostatic hyperplasia (2003). Chapter 1: Diagnosis and treatment recommendations. J Urol. 2003; 170: 530-47.
- Oesterling JE, Tekchandani AH, Martin SK, Bergstralh EJ, Reichstein E, Diamandis EP, et al.: The periurethral glands do not significantly influence the serum prostate specific antigen concentration. J Urol. 1996; 155: 1658-60.
- Wolff JM, Boekels O, Borchers H, Jakse G, Rohde D: Altered prostate specific antigen reference range after transurethral resection of the prostate. Anticancer Res. 2000; 20: 4977-80.
- De Nunzio C, Franco G, Iori F, Leonardo C, Minardi V, Laurenti C: Clinical and pressure-flow changes after long-term treatment with alfuzosin SR. Urol Int. 2003; 71: 31-6.
- Rodrigues P, Lucon AM, Freire GC, Arap S: Urodynamic pressure flow studies can predict the clinical outcome after transurethral prostatic resection. J Urol. 2001; 165: 499-502.
- Hammerer PG, McNeal JE, Stamey TA: Correlation between serum prostate specific antigen levels and the volume of the individual glandular zones of the human prostate. J Urol. 1995; 153: 111-4.
- Nickel JC, Downey J, Young I, Boag S: Asymptomatic inflammation and/or infection in benign prostatic hyperplasia. BJU Int. 1999; 84: 976-81.
- Kwak C, Ku JH, Kim T, Park DW, Choi KY, Lee E, et al.: Effect of subclinical prostatic inflammation on serum PSA levels in men with clinically undetectable prostate cancer. Urology. 2003; 62: 854-9.
- Nadler RB, Humphrey PA, Smith DS, Catalona WJ, Ratliff TL: Effect of inflammation and benign prostatic hyperplasia on elevated serum prostate specific antigen levels. J Urol. 1995; 154: 407-13.
- Stamey TA, Yang N, Hay AR, McNeal JE, Freiha FS, Redwine E: Prostate-specific antigen as a serum marker for adenocarcinoma of the prostate. N Engl J Med. 1987; 317: 909-16.
- Lloyd SN, Collins GN, McKelvie GB, Hehir M, Rogers AC: Predicted and actual change in serum PSA following prostatectomy for BPH. Urology. 1994; 43: 472-9.
____________________
Accepted
after revision:
July 24, 2007
_______________________
Correspondence address:
Dr. Cristiano M. Gomes
Hospital das Clínicas, USP
Divisão de Clínica Urológica
Caixa Postal: 11273-9
São Paulo, SP, 05422-970, Brazil
Fax: + 55 11 3069-8081
E-mail: crismgomes@uol.com.br