THE
ROLE OF LIVER TRANSPLANTATION TECHNIQUES IN THE SURGICAL MANAGEMENT OF
ADVANCED RENAL UROTHELIAL CARCINOMA WITH OR WITHOUT INFERIOR VENA CAVA
THROMBUS
(
Download pdf )
WOLFGANG H. CERWINKA, MURUGESAN MANOHARAN, MARK S. SOLOWAY, GAETANO CIANCIO
Department of Urology (WHC, MM, MSS) and Department of Surgery (GC), Division of Transplantation, University of Miami Miller School of Medicine, Miami, Florida, USA
ABSTRACT
Purpose:
Standard radical nephrectomy for large masses is significantly facilitated
by liver transplantation techniques, which have been successfully employed
over the last ten years at our institution. Large and locally-advanced
urothelial carcinoma of the kidney with or without extension into the
inferior vena cava is rare. The purpose of this study was to present the
surgical management of large and locally-advanced urothelial tumors arising
from the renal pelvis using liver transplantation techniques and to evaluate
patient outcome.
Materials and Methods: Diagnostic work-up
and surgical management of 4 patients with large and locally-advanced
renal urothelial carcinoma were retrospectively reviewed. Two out of four
patients with urothelial carcinoma presented with inferior vena cava thrombus.
Mean tumor size was 11.6 cm. All patients underwent surgery, 2 patients
with the presumed diagnosis of renal cell cancer. Liver transplantation
techniques were an integral part in all radical nephrectomies.
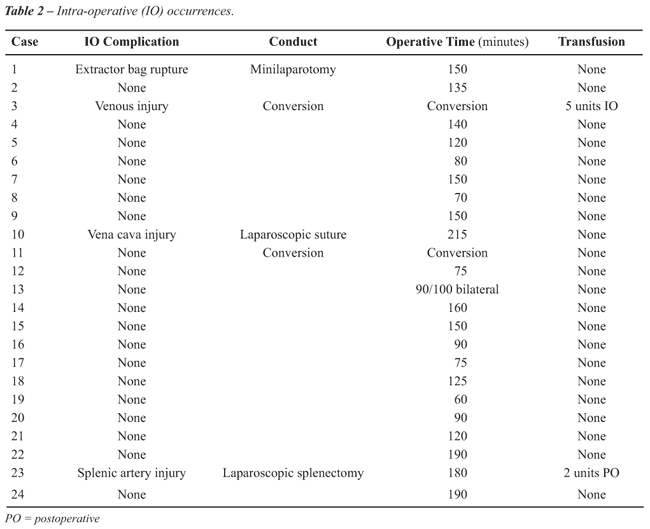
Results: No intraoperative complications
and postoperative mortality occurred. Mean operative time was 7.5 hours,
estimated blood loss was 1.5 L, and an average of 4.8 units of blood was
transfused intraoperatively. Three patients succumbed to cancer recurrence
at a mean postoperative time of 6.3 months; 1 patient is still alive 24
months after surgery.
Conclusions: Large and locally-advanced
renal masses of urothelial origin can be successfully removed by a combination
of radical nephrectomy with liver transplantation techniques. Since long-term
outcome of such patients has been poor, accurate preoperative diagnosis
is essential to consider neoadjuvant treatment and to plan nephroureterectomy.
Key
words: urothelial carcinoma; kidney, nephrectomy; liver transplantation
Int Braz J Urol. 2009; 35: 19-23
INTRODUCTION
Urothelial
carcinoma (UC) of the renal pelvis represents approximately 10% of all
primary renal malignancies and its prognosis correlates with histological
grade and stage (1,2). Advanced disease stages, such as invasion into
renal parenchyma or perirenal fat with or without tumor extension into
the inferior vena cava (IVC) carry a poor prognosis (3). IVC involvement
is rare with only a few cases reported in the literature (4). Extirpation
of these large renal masses poses a particular challenge to the urologic
surgeon because adequate surgical exposure and subsequent nephrectomy
rely on mobilization of adjacent organs such as liver and spleen. In cases
of tumor extension into the IVC, additional exposure of the retrohepatic
and suprahepatic IVC is necessary. Locally-advanced renal cell carcinomas
(RCC) have been safely and completely removed by combining radical nephrectomy
with surgical techniques derived from liver transplantation over the last
ten years at our institution (5).
The purpose of this study was to present
the surgical management of large and locally-advanced urothelial tumors
arising from the renal pelvis employing liver transplantation techniques
and to evaluate patient outcome.
MATERIALS AND METHODS
Four
patients with locally-advanced UC of the renal pelvis (= T3), two with
extension into the IVC, were treated at our institution between 2003 and
2005. Pertinent preoperative work-up (imaging, laboratory), tumor characteristics
(grade, stage), surgical approach, perioperative management, and patient
outcome were reviewed. All four patients underwent standard preoperative
evaluation including abdominal CT scans, chest X-rays or chest CT scans,
and liver function tests. Bone scans and abdominal MRIs were obtained
in 2 patients. Tumor thrombus extent was staged according to the Mayo
Foundation classification (6). Cystoscopy and cytology were performed
in 1 of 3 patients with a history of hematuria.
Liver transplantation techniques, in combination
with nephrectomy for large and locally-invasive renal masses, have been
previously described in detail (5). In brief, a bilateral subcostal incision,
with superior midline T-extension is performed and a Rochard self-retaining
retractor placed. This tri-radiate incision permits access to the liver,
diaphragm, hepatic veins, and suprahepatic IVC and is the favored approach
for orthotopic liver transplantation. Liver and IVC are mobilized in piggyback
fashion. Liver mobilization begins with dissection, ligation and division
of the ligamentum teres. The falciform ligament is then divided by cautery.
This incision is carried around each portion of the divided falciform
ligament to the right superior coronary ligament and divides the left
triangular ligament. The visceral peritoneum on the right side of the
hepatic hilum and the infrahepatic IVC are incised with the right inferior
coronary and hepatorenal ligaments. At this stage, nephrectomy of most
bulky masses can be safely carried out, however, in cases of IVC involvement,
mobilization continues. The liver is gradually rolled to the left using
the same techniques as in liver transplantation. In this fashion, the
infrahepatic, intrahepatic, and suprahepatic portions of the IVC are completely
exposed. The three hepatic veins are identified, their orifices inspected,
and tumor removed. Following the removal of the tumor thrombus and IVC,
the clamp is repositioned below the hepatic veins thus permitting continued
hepatic venous drainage during the removal of the IVC and tumor thrombus.
Exposure of the left kidney begins by mobilization of the descending colon.
The spleen is dissected off the diaphragm and mobilized en bloc with the
pancreas toward the midline. To gain access to the upper pole of the left
kidney the left liver lobe is mobilized. The study was approved by the
Institutional Review Board.
RESULTS
Three
male and one female patient underwent surgery for large but clinically
localized UCs of the renal pelvis; mean age was 65 years (range 59-74).
Preoperative diagnosis was UC in 2 cases: One patient had undergone radical
cystectomy with ileal conduit 6 years earlier suggesting upper tract UC;
another patient underwent cystoscopy showing tumor protruding from the
ureteral orifice. The remaining two patients with IVC thrombus entered
surgery with the presumed diagnosis of RCC.
A bilateral subcostal incision with midline
T-extension was the surgical approach in all 4 cases. Mean operative time
was 7.5 hours, mean estimated blood loss was 1.5 L, and an average of
4.8 units of blood was transfused. Three nephrectomy specimens were bivalved
in the operating room, which changed the diagnosis in one case and ureterectomy
was consequently performed; the remaining specimen was not bivalved and
the ipsilateral ureter was left in situ. Gross examination of the specimens
demonstrated UC arising from the renal pelvis and invasion of the proximal
ureter. None of the patients required cardiopulmonary bypass. There was
neither an intraoperative complication nor an operative mortality. Postoperative
morbidity occurred in 2 patients secondary to pulmonary embolism on postoperative
day 2 and 61. Three patients underwent adjuvant chemotherapy; one could
not proceed because of low performance status. Three patients expired
of disease recurrence at a mean of 6.3 months after surgery; one patient
is alive without evidence of disease 24 months later (Table-1). All 4
patients were diagnosed with high-grade urothelial carcinoma arising from
the renal pelvis. Tumor characteristics are shown in Table-2. Mean tumor
size was 11.6 cm. In 2 patients the tumor extended into the IVC and in
2 patients lymph nodes were involved.

COMMENTS
To
our knowledge this is the first study describing the application of liver
transplantation techniques for the resection of large UCs of the kidney
with and without IVC thrombus. The surgical technique described herein
allowed excellent exposure and safe removal of the tumor in all 4 patients
(5). Liver transplantation techniques proved essential for the resection
of IVC thrombi in 2 patients and significantly improved exposure to the
retroperitoneum allowing complete removal of the remaining two renal masses
with a mean size of 12 cm. Albeit RCC of such size is amenable to conventional
nephrectomy, UC of the renal pelvis is known to induce significant perirenal
inflammation and desmoplastic reaction and is frequently associated with
lymph node metastasis (7). Secondary to these adverse tumor characteristics
operative time was considerably prolonged with a mean of 7.5 hours. No
intraoperative complications or postoperative mortality occurred. In a
series of 3 patients with renal UC and IVC thrombus, a midline approach
was selected in 2 patients (one surgery was aborted due to extensive liver
involvement) and an extended subcostal incision in the third. One of these
patients was without evidence of disease 9 months after surgery, two died
of respiratory failure within 2 months postoperatively (8).
Prognosis for upper tract UC, stage for
stage, is reportedly inferior to that of bladder UC. While 5 year overall
survival rates for stage T2, T3, and T4 bladder UC are 72%, 40%, and 33%,
they are 60%, 15% and 15% for upper tract UC (3,9). Neoadjuvant chemotherapy
for patients with ≥ T2 bladder UC in prospective randomized clinical
trials has demonstrated survival benefits (10,11). However, there is no
evidence supporting neoadjuvant chemotherapy for upper tract UC. None
of our patients received neoadjuvant chemotherapy; however, we speculate
that it may have improved patient survival as previously demonstrated
for bladder UC (intact vasculature, improved resectability, early control
of occult metastases, better performance status). Neoadjuvant chemotherapy
may furthermore result in better outcome than adjuvant chemotherapy because
many patients do not receive optimal dosing of systemic chemotherapy after
nephrectomy (12). One out of four patients with UC in our series was unable
to commence adjuvant chemotherapy because of low performance status. Despite
complete tumor resection, 3 out of 4 patients died of disease recurrence
within 10 months after surgery, of whom 2 had undergone adjuvant chemotherapy.
Consideration of neoadjuvant chemotherapy
relies on correct preoperative diagnosis. Two out of four patients in
this study entered surgery with the presumptive diagnosis of RCC. Despite
the presence of hematuria in 3 out of 4 patients, only 1 underwent cystoscopy,
which established the correct diagnosis. Therefore, the finding of a large
renal mass with or without IVC thrombus in patients with history of hematuria
requires a complete hematuria work-up (13). According to the literature
only 30% of patients with upper tract UC underwent surgery with the correct
preoperative diagnosis. Several factors may contribute to the fact that
large renal UC is frequently mistaken for RCC preoperatively (4). 1. UC
arising from the renal pelvis is uncommon with an incidence of 7% to 15%
of all primary renal malignancies (1,2). 2. RCC represents 85% of all
primary renal malignancies and extends into the IVC in 4-10% (14,15).
3. A significant history of cigarette smoking and hematuria exists for
both RCC and UC. 4. While upper tract UC presents with non-specific findings
on imaging studies, CT scan may be a useful tool to differentiate renal
UC from RCC (4,16). 5. IVC thrombus formation of UC is exceedingly rare
with 21 cases reported in the literature (4). Meta-analyses evaluating
the management of UC with IVC extension showed that in approximately 30%
of patients a preoperative MRI was obtained. Only 20% had a positive cytology
and all patients, in whom a retrograde pyelography was performed, demonstrated
a renal pelvic/ureteral filling defect. In 60% of cases, nephrectomy without
ureterectomy was performed and average survival was 6 months (17,18).
Renal UC has a propensity to recur in the ipsilateral ureter at a rate
of 30 to 40% and mandates radical nephroureterectomy (19,20). In one of
our patients, with the presumed diagnosis of RCC, the ureter was left
in situ.
CONCLUSIONS
Large and locally-advanced urothelial carcinomas of the renal pelvis can be successfully removed by enhancing standard radical nephrectomy with liver transplantation techniques; however, survival is poor. Preoperative diagnosis of renal urothelial carcinoma requires a high index of suspicion and is essential to consider neoadjuvant treatment and to plan nephroureterectomy.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Guinan P, Vogelzang NJ, Randazzo R, Sener S, Chmiel J, Fremgen A, et al.: Renal pelvic cancer: a review of 611 patients treated in Illinois 1975-1985. Cancer Incidence and End Results Committee. Urology. 1992; 40: 393-9.
- Störkel S, Eble JN, Adlakha K, Amin M, Blute ML, Bostwick DG, et al.: Classification of renal cell carcinoma: Workgroup No. 1. Union Internationale Contre le Cancer (UICC) and the American Joint Committee on Cancer (AJCC). Cancer. 1997; 80: 987-9.
- Ozsahin M, Zouhair A, Villà S, Storme G, Chauvet B, Taussky D, et al.: Prognostic factors in urothelial renal pelvis and ureter tumours: a multicentre Rare Cancer Network study. Eur J Cancer. 1999; 35: 738-43.
- Kawashima A, Takao T, Takaha N, Nishimura K, Nonomura N, Okuyama A, et al.: Renal pelvic cancer with tumor thrombus in the vena cava inferior: a case report. Hinyokika Kiyo. 2004; 50: 869-72.
- Ciancio G, Hawke C, Soloway M: The use of liver transplant techniques to aid in the surgical management of urological tumors. J Urol. 2000; 164: 665-72.
- Neves RJ, Zincke H: Surgical treatment of renal cancer with vena cava extension. Br J Urol. 1987; 59: 390-5.
- Kondo T, Nakazawa H, Ito F, Hashimoto Y, Toma H, Tanabe K: Primary site and incidence of lymph node metastases in urothelial carcinoma of upper urinary tract. Urology. 2007; 69: 265-9.
- Leo ME, Petrou SP, Barrett DM: Transitional cell carcinoma of the kidney with vena caval involvement: report of 3 cases and a review of the literature. J Urol. 1992; 148: 398-400.
- Stein JP, Lieskovsky G, Cote R, Groshen S, Feng AC, Boyd S, et al.: Radical cystectomy in the treatment of invasive bladder cancer: long-term results in 1,054 patients. J Clin Oncol. 2001; 19: 666-75.
- Grossman HB, Natale RB, Tangen CM, Speights VO, Vogelzang NJ, Trump DL, et al.: Neoadjuvant chemotherapy plus cystectomy compared with cystectomy alone for locally advanced bladder cancer. N Engl J Med. 2003; 349: 859-66. Erratum in: N Engl J Med. 2003; 349: 1880.
- Advanced Bladder Cancer Meta-analysis Collaboration: Neoadjuvant chemotherapy in invasive bladder cancer: a systematic review and meta-analysis. Lancet. 2003; 361: 1927-34.
- Lerner SE, Blute ML, Richardson RL, Zincke H: Platinum-based chemotherapy for advanced transitional cell carcinoma of the upper urinary tract. Mayo Clin Proc. 1996; 71: 945-50.
- Grossfeld GD, Wolf JS Jr, Litwan MS, Hricak H, Shuler CL, Agerter DC, et al.: Asymptomatic microscopic hematuria in adults: summary of the AUA best practice policy recommendations. Am Fam Physician. 2001; 63: 1145-54.
- Marshall FF, Dietrick DD, Baumgartner WA, Reitz BA: Surgical management of renal cell carcinoma with intracaval neoplastic extension above the hepatic veins. J Urol. 1988; 139: 1166-72.
- Chow WH, Devesa SS, Warren JL, Fraumeni JF Jr: Rising incidence of renal cell cancer in the United States. JAMA. 1999; 281: 1628-31.
- Gatewood OM, Goldman SM, Marshall FF, Siegelman SS: Computerized tomography in the diagnosis of transitional cell carcinoma of the kidney. J Urol. 1982; 127: 876-87.
- Williams JH, Frazier HA 2nd, Gawith KE, Laskin WB, Christenson PJ: Transitional cell carcinoma of the kidney with tumor thrombus into the vena cava. Urology. 1996; 48: 932-5.
- Miyazato M, Yonou H, Sugaya K, Koyama Y, Hatano T, Ogawa Y: Transitional cell carcinoma of the renal pelvis forming tumor thrombus in the vena cava. Int J Urol. 2001; 8: 575-7.
- Strong DW, Pearse HD, Tank ES Jr, Hodges CV: The ureteral stump after nephroureterectomy. J Urol. 1976; 115: 654-5.
- Murphy DM, Zincke H, Furlow WL: Management of high grade transitional cell cancer of the upper urinary tract. J Urol. 1981; 125: 25-9.
____________________
Accepted after revision:
October 06, 2008
_______________________
Correspondence address:
Dr. Wolfgang H. Cerwinka
Children’s Healthcare of Atlanta
Emory University
5445 Meridian Mark Road, Suite 420
Atlanta, GA, 30342, USA
Fax: + 1 404 252-1268
E-mail: wcerwinka@gaurology.com