TO
CIRC OR NOT TO CIRC: CLINICAL AND PHARMACOECONOMIC OUTCOMES OF A PROSPECTIVE
TRIAL OF TOPICAL STEROID VERSUS PRIMARY CIRCUMCISION
(
Download pdf )
doi: 10.1590/S1677-553820100000100012
YURI D. NOBRE, RICARDO G. FREITAS, MARIA J. FELIZARDO, VALDEMAR ORTIZ, ANTONIO MACEDO JR.
Section of Pediatric Urology, Department of Urology, Federal University of Sao Paulo, Sao Paulo, SP, Brazil
ABSTRACT
Purpose:
To compare the efficacy and costs of circumcision versus topical treatment
using a prospective pharmacoeconomic protocol.
Materials and Methods: We treated 59 patients
(3-10 years of age) randomized into two groups: 29 underwent an 8-week
course of topical treatment with 0.2% betamethasone-hyaluronidase cream
twice a day; and 30 underwent circumcision. Topical treatment success
was defined as complete exposure of the glans. In cases of treatment failure,
circumcision was performed and its cost imputed to that of the initial
treatment. The pharmacoeconomic aspects were defined according to the
Brazilian National Public Health System database and the Brazilian Community
Pharmacies Index.
Results: The two groups were statistically
similar for all clinical parameters evaluated. Topical treatment resulted
in complete exposure of the glans in 52% of the patients. Topical treatment
was associated with preputial pain and hyperemia. However, treatment suspension
was unnecessary. Minor complications were observed in 16.6% of the surgical
group patients. The mean cost per patient was US$ 53.70 and US$ 125.20,
respectively, for topical steroid treatment (including the costs related
to treatment failure) and circumcision. The total costs were US$ 2,825.32
and US$ 3,885.73 for topical treatment and circumcision, respectively.
Conclusions: Topical treatment of phimosis
can reduce costs by 27.3% in comparison with circumcision. Therefore,
topical treatment of phimosis should be considered prior to the decision
to perform surgery.
Key
words: phimosis; circumcision; male; steroids; pharmacoeconomics
Int Braz J Urol. 2010; 36: 75-85
INTRODUCTION
Circumcision
is considered the elective treatment for phimosis in newborn infants and
children. In the United States, circumcision is the fourth most common
surgical procedure, performed in 65.3% of the male population (1).
Various factors, such as social norms, cultural traditions and religious
beliefs, influence the decision of whether or not to perform circumcision.
The American Academy of Pediatrics, in one of their most recent publications
on this subject, stated that there is no absolute medical indication for
the routine circumcision of newborn infants, and that, despite the potential
medical benefits and advantages, circumcision also presents disadvantages
and risks. When truly indicated, the risks and benefits should be discussed
with parents, who should be asked to give written informed consent (2).
In the 1990s, due to the controversy surrounding
the topic of when circumcision is indicated, various studies were carried
out in order to investigate alternative treatments for phimosis. Consistent
success rates were achieved with the use of topical corticosteroids (3,4).
Pharmacoeconomic studies help identify,
calculate and compare the costs and risks of specific programs or therapies,
as well as their benefits. Such studies also help determine which alternatives
provide the best results and constitute the most practical use of the
resources invested. Therefore, pharmacoeconomics is a relevant tool in
the decision-making process, introducing the concept of economic rationality
into health care systems in order to complement clinical decision making
(5). There have been few studies on the economic impact of circumcision
versus topical treatment of phimosis. Therefore, we conducted a prospective
randomized study comparing, from the pharmacoeconomic point of view, the
implications of topical treatment versus those of circumcision in cases
of phimosis.
MATERIALS AND METHODS
A prospective randomized study was carried out in order to evaluate the
clinical response to topical treatment of pathologic phimosis, comparing
it to that of circumcision.
We included 85 children, from 3 to 10 years of age, diagnosed with phimosis.
We defined as phimosis, in this age bracket, phimosis type I (no retraction
of the foreskin) and type II (external urethral meatus exposure only),
in accordance with the classification system devised by Kayaba et al.
(6).
The study was previously approved by the
Ethics Committee on Research of our University, and all parents or guardians
were instructed and signed the written informed consent before starting
the study.
In the clinical group, 42 patients were
treated with two daily applications of 0.2% betamethasone and hyaluronidase
cream for 8 weeks. The same physician examined all of the patients. Prior
to the beginning of treatment and in every subsequent consultation, patients
were photographed.
The therapeutic response was considered
favorable only if the glans was easily and completely exposed during the
subsequent physical examination, without a phimotic ring or balanopreputial
adhesions (Kayaba type V). The therapeutic response was considered unfavorable
if there was no exposure of the glans or there was only partial exposure
of the glans due to balanopreputial adhesions or a phimotic ring. Therefore,
the criterion adopted in order to define treatment success was the same
as the expected outcome of circumcision: complete exposure of the glans.
Patients who responded well to the topical
treatment underwent outpatient follow-up evaluations at 2 and 4 months
after the end of treatment.
Patients who did not respond to the topical
treatment by week 8 or who presented recurrence during the follow-up period
underwent circumcision.
Patients in the surgical group were evaluated
and then referred to undergo circumcision. Patients underwent outpatient
follow-up evaluations on postoperative days 15, 30 and 120.
All surgical procedures were carried out
at our institution. The anesthesia protocol was general inhalation anesthesia
with sevoflurane, in conjunction with nerve block of the penis.
In the present study, the pharmacoeconomic
analysis was of the cost-minimization type. Only the costs of the surgical
procedure and clinical treatment (those directly related to the health
care system: medical care, medications and medical materials) were taken
into consideration. Indirect costs related to lost productivity, as well
as intangible costs (those related to pain, suffering and impaired quality
of life), were not calculated.
The pharmacoeconomic analysis was carried
out from the perspective of a Public Health Hospital, and the resources
included in the cost analysis were identified through communications with
officials of the Brazilian United Health Care System (BUHCS). The medication
costs that were not available in the public health system database were
determined by consulting the Brazilian Community Pharmacies Index.
For patients in the surgical group, the
costs were calculated separately for each of the following aspects: medical
visits; anesthetic medications; surgical materials; medical and nursing
team; and medications for the treatment of adverse effects.
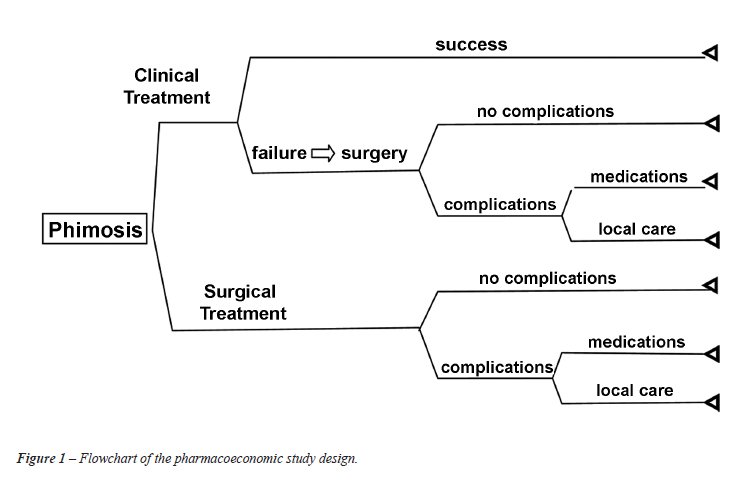
For patients in the clinical group, the
costs of the medical visits were calculated separately from those of the
medications. Since some of the patients in the clinical group were eventually
referred to surgery, those costs were incorporated into the final costs
for that group (Figure-1).
Statistical evaluation of data was carried
out by means of the chi-square test, Fisher’s exact test, likelihood
ratio test and Student’s t-test. The level of significance was set
at p = 0.05. For the pharmacoeconomic evaluation of the groups, we used
the nonparametric Mann-Whitney test, for which the level of significance
was also set at p = 0.05.
RESULTS
Of
the 85 children included in the study, 43 were allocated to the surgical
group and 42 were allocated to the clinical group. From the surgical group,
13 children were excluded: 1 due to uncooperativeness; 2 due to refusal
to undergo surgery; and 10 due to failure to return for surgery. Coincidentally,
13 children were also excluded from the clinical group: 1 due to irregular
use of medication; 1 due to being clinically diagnosed with balanitis
xerotica obliterans; 1 due to previous use of medication; and 10 due to
failure to appear for medical visits. The mean age of the population in
the study was 5.81 years.
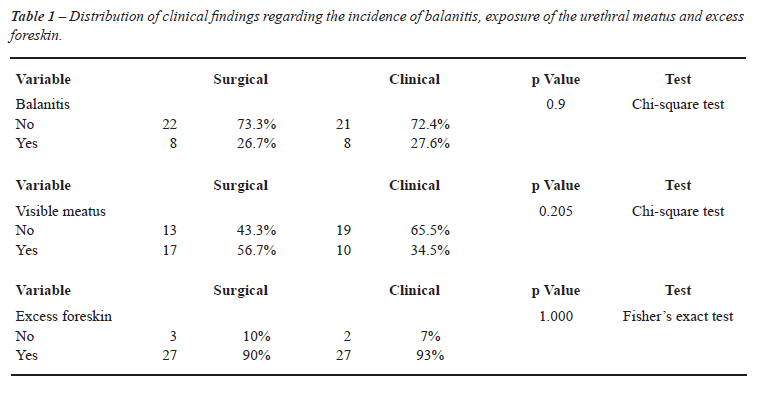
All clinical parameters evaluated were statistically
similar after the comparison between the groups (Table-1).
In the surgical group, the mean surgical
time was 34.5 min, the mean time to emergence from anesthesia was 43 min,
and the mean postoperative stay in the infirmary was 47.3 min. On postoperative
day 15, 5 patients presented complications of the procedure: 2 due to
infection caused by improper cleaning; and 3 due to hematomas and scarring
on the glans. These complications were considered mild and were treated
with intensive local care. In the subsequent follow-up visits, all of
the patients presented penile conditions that were considered normal,
with proper formation of scar tissue.
In the clinical group, 15 (51.7%) of the
29 patients presented complete exposure of the glans at 2 months after
the end of treatment. The topical treatment resulted in adverse effects
or complications in 10 patients: 4 patients experienced hyperemia and
a burning sensation in the foreskin; 4 patients experienced a burning
sensation in the foreskin; and 2 patients presented balanopreputial hyperemia.
No intervention or treatment interruption was necessary in any of the
cases.
In the clinical group, patients in whom
treatment success was achieved were monitored for 4 months. Neither loss
of exposure of the glans nor recurrence was detected.
Clinical treatment failure occurred in
14 cases, and those patients were referred to circumcision. Of those 14
patients, 2 failed to return for surgery. For the 12 who underwent surgery,
the mean surgical time was 31.2 min, the mean time to emergence from anesthesia
was 30 min, and the mean postoperative stay in the infirmary was 60 min.
Of the 12 clinical group patients undergoing
circumcision, 4 presented postoperative complications: 1 due to infection
caused by improper cleaning, which demanded oral antibiotic treatment
and local care; 1 due to bleeding and scars on the gland, which was treated
locally; 1 due to pyogenic granuloma; and 1 due to an inflammatory process
close to urethral meatus. All of the clinical group patients presented
resolution of the complications during the follow-up period.
Pharmacoeconomic Analysis
In the pharmacoeconomic analysis, we evaluated the direct costs related to treatment of the two groups. It is of note that, as previously mentioned, the costs related to circumcision of patients in the clinical group were included in the final costs for that group (Figures 2-3).
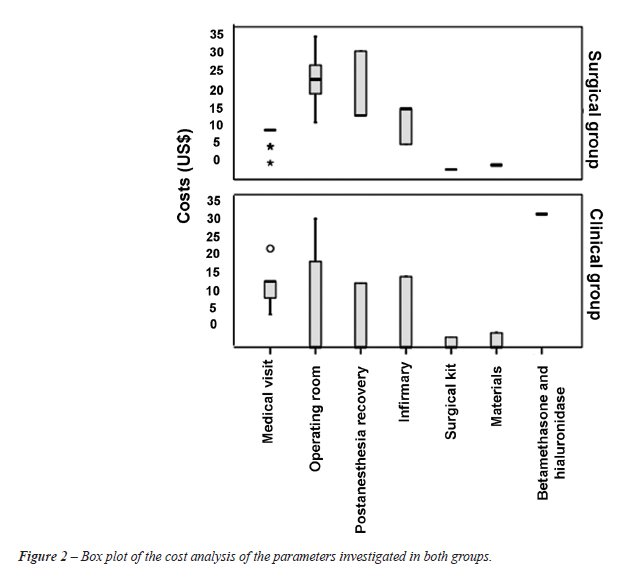
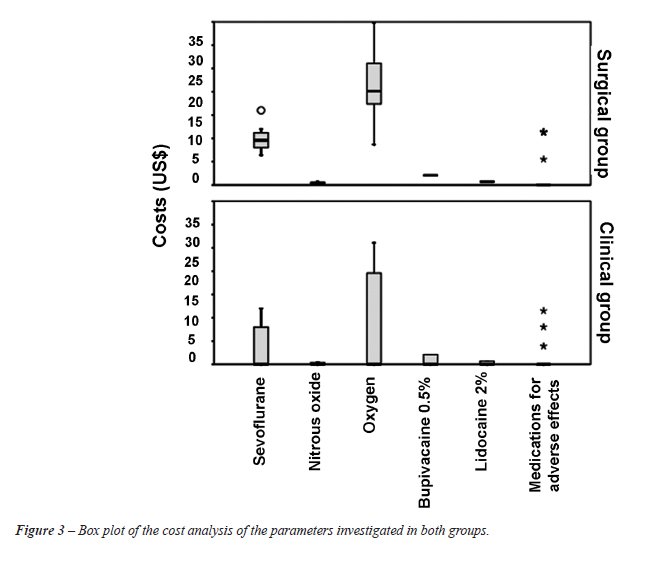
In the pharmacoeconomic evaluation, the
costs were higher in the clinical group only in terms of the medical visits
and the use of topical medication. Costs regarding medical and nursing
staff, anesthetic medications and surgical materials were higher in the
surgical group than in the clinical group (p < 0.001). No statistical
difference was found in costs regarding medications used for the treatment
of postoperative complications.
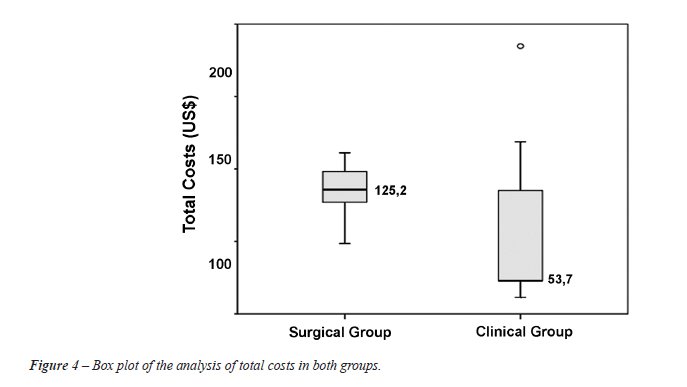
As can be seen in Figure-4, the analysis
of the total costs per group, revealed greater economy in the clinical
group than in the surgical group US$ 2,825.32 vs. US$ 3,885.73; p = 0.068;
median, US$ 53.70 vs. US$ 125.20.
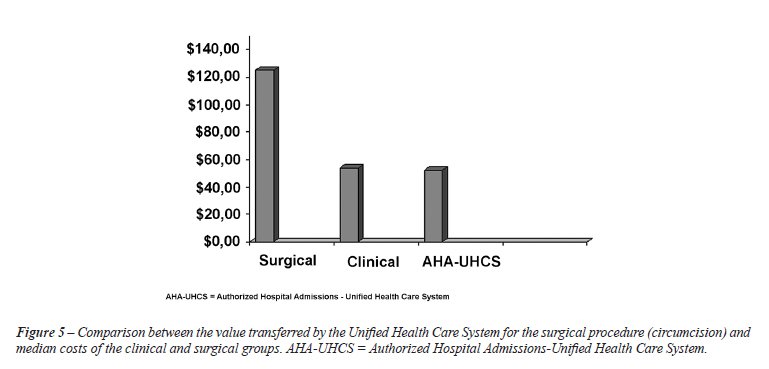
Comparing the median cost to the set price
stipulated by the BUHCS through the Authorized Hospital Admissions System
(US$ 52.20) for every patient who underwent circumcision, we found considerable
discrepancy between the amount paid by the BUHCS and the actual hospital
costs of the circumcisions (Figure-5).
COMMENTS
Circumcision
is classically considered the gold standard for the treatment of phimosis.
Approximately one-sixth of males worldwide are circumcised (7). The indications
for performing neonatal circumcision are controversial. Prominent among
the factors favoring neonatal circumcision are the lower incidence of
penile cancer, the lower incidence of balanitis/urinary infections, and
the prevention of sexually transmitted diseases, including AIDS (8,9).
In addition, the incidence of postoperative complications is low. These
benefits are sufficiently relevant to guarantee the routine practice of
neonatal circumcision (8). However, most studies in which routine circumcision
is recommended are retrospective studies, and the validity of the conclusions
should be critically investigated. Circumcision is, arguably, a preventive
health care measure, which, in theory, facilitates hygiene. However, the
potential benefits occur years after the surgery, and few studies involve
adequate, timely follow-up evaluation (10).
In Brazil, we do not adopt the concept of
neonatal circumcision and most indications for surgery are considered
when the child is about to leave diapers and only patients with phimotic
ring are candidates for this kind of treatment.
The clinical treatment of phimosis consists
of the gentle retraction of the foreskin and application of a topical
corticosteroid to the foreskin and phimotic ring, with the objective of
achieving complete exposure of the glans. The effects of topical corticosteroids,
which have anti-inflammatory and immunosuppressive properties, on the
metabolism of arachidonic acid and inhibition of interleukin-1 synthesis
have been well established. Topical corticosteroids can have an antiproliferative
effect on the dermal matrix, decreasing skin thickness and obliterating
the stratum corneum (11,12).
Hyaluronidase acts by modifying intercellular
permeability and reducing tissue resistance, thereby increasing the diffusion
of substances between planes (13).
In a pioneer study on the application of
topical corticosteroid in boys with phimosis who were candidates for circumcision,
clinical treatment was shown to be viable and efficacious (3). Topical
treatment of phimosis with corticosteroids has characteristics that make
it quite attractive as the first approach to the treatment of phimosis.
The method is safe, and complication rates are similar to those found
for circumcision. In addition, corticosteroid treatment presents high
cure rates and low costs, as well as being easily administered and being
well accepted by family members (14-16).
In the present study, 51.7% of the patients
in the clinical group presented complete exposure of the glans, and none
presented recurrence or lack of exposure of the glans during the 4 months
of post-treatment follow-up evaluation. It is of note that we adopted
a strict criterion for treatment success, excluding partial exposure of
the glans, and that, in 65.5% of the patients, only the urethral meatus
was exposed (Kayaba type I) prior to treatment. In multivariate analyses,
Kayaba type I presentation has been described as a determining factor
for corticosteroid treatment success (16).
There have been few studies comparing the
economic impact of circumcision with that of topical treatment in individuals
with phimosis. It has been estimated that topical treatment reduces costs
by 75% in comparison with circumcision, representing, for example, a potential
annual savings of 150 million francs in France (17,18). However, in such
studies, costs and treatment outcomes are estimated based on the means
obtained in previous studies, and the potential economic risks of future
complications are only speculated upon.
Van Howe (2004) conducted a cost-utility
analysis of neonatal circumcision, evaluating the impact on the quality
of life of patients for 72 years after circumcision (19). The author concluded
that neonatal circumcision is more costly and has more adverse effects
on the lifetime health of individuals than does not undergoing this procedure.
Nevertheless, in a retrospective study evaluating the costs of circumcision,
the authors concluded that neonatal circumcision provides medical benefit
and prevents various pathologies, as well as costing ten times less than
postnatal circumcision (20).
In general, pharmacoeconomic analysis consists
of two essential elements: costs and outcome, which are, respectively,
the nominator and the denominator of the equation. The pharmacoeconomic
analysis in this study was based on cost minimization, in which we compared
the costs of two treatment modalities whose final outcome measure was
the resolution of pathologic phimosis (5).
The analysis showed that the costs of all
items related to the clinical treatment were lower than were those related
to the surgical treatment, except for the costs regarding medical visits
and use of topical medication, which were not used in the surgical group
patients. The evaluation showed that the clinical parameters, age brackets,
follow-up rates and noncompliance rates were similar in the two groups.
No differences were found between the groups in terms of surgical time
or incidence of complications.
The cost savings corresponded to the total
cost of treating the patients in the surgical group (US$ 3,885.73) subtracted
from the total cost of treating the patients in the clinical group (US$
2,825.32). The cost savings, which was the amount of money saved by using
the topical treatment as the first-line treatment, was US$ 1,060.40.
Finally, when we compared the total costs of the treatment with the governmental
reference values for circumcision, we found that amount provided by the
health care system does not cover the costs of the surgical procedure.
Therefore, topical corticosteroid administration as the first-line treatment
for phimosis could represent a considerable savings to the institution.
We acknowledge some criticism of our study
when considering that only complete exposure of the glans without a phimotic
ring was defined as a favorable result of topic treatment. On the other
hand, we tried to make the end-point of both kinds of treatment comparable
and this could justify our methodology.
A second point of concern by some authors
would be that our results with non-surgical treatment were inferior to
most other published series that report higher (90-95%) rates of efficiency.
We stress that at the age we proposed to study these patients most boys
had already experienced spontaneous resolution of phimosis, therefore,
we were really comparing patients in the “waiting list” for
surgery at our institution.
CONCLUSIONS
As
a first-line treatment for phimosis, topical corticosteroid administration
reduced costs by 27.3% in comparison with circumcision, even when we included
the costs of the circumcisions eventually performed in the clinical treatment
group. The mean cost of circumcision per child was US$ 125.00 and for
topical treatment was US$ 54.00, so that US$ 35.00 could have been saved
in the Brazilian public health system per child if conservative treatment
had primarily been used.
These data underscore the concept that topical
treatment should be offered to patients prior to considering surgery.
ACKNOWLEDGEMENT
Mrs. Rosana Lima Garcia Tsuji for valuable supported the pharmacoeconomic analysis.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Agency for Healthcare Research and Quality. Most common surgical procedures in the United states 2003. Available at: http://www.ahcpr.gov. Accessed on April 11, 2008.
- [No authors listed]: American Academy of Pediatrics: Report of the Task Force on Circumcision. Pediatrics. 1989; 84: 388-91. Erratum in: Pediatrics. 1989; 84: 761.
- Kikiros CS, Beasley SW, Woodward AA: The response of phimosis to local steroid application. Ped Surg Int. 1993; 8: 329-32.
- Jørgensen ET, Svensson A: The treatment of phimosis in boys, with a potent topical steroid (clobetasol propionate 0.05%) cream. Acta Derm Venereol. 1993; 73: 55-6.
- Reeder CE: Pharmacoeconomics and health care outcomes management: Focus on biotechnology. Am J Health Syst Pharm. 1995; 52 (Suppl 4): S5-8.
- Kayaba H, Tamura H, Kitajima S, Fujiwara Y, Kato T, Kato T: Analysis of shape and retractability of the prepuce in 603 Japanese boys. J Urol. 1996; 156: 1813-5.
- Hutcheson JC: Male neonatal circumcision: indications, controversies and complications. Urol Clin North Am. 2004; 31: 461-7.
- Schoen EJ, Wiswell TE, Moses S: New policy on circumcision--cause for concern. Pediatrics. 2000; 105: 620-3.
- Cameron DW, Simonsen JN, D’Costa LJ, Ronald AR, Maitha GM, Gakinya MN, et al.: Female to male transmission of human immunodeficiency virus type 1: risk factors for seroconversion in men. Lancet. 1989; 2: 403-7.
- Tran PT, Giacomantonio M: Routine neonatal circumcision? Can Fam Physician. 1996; 42: 2201-4.
- Guerrero Fernández J, Guerrero Vázquez J, Russo de la Torre F: Conservative treatment of phimosis, balanitis and perianal streptococcal disease with local steroid therapy. An Pediatr (Barc). 2003; 58: 198-9.
- Monsour MA, Rabinovitch HH, Dean GE: Medical management of phimosis in children: our experience with topical steroids. J Urol. 1999; 162: 1162-4.
- DeVries CR, Miller AK, Packer MG: Reduction of paraphimosis with hyaluronidase. Urology. 1996; 48: 464-5.
- Orsola A, Caffaratti J, Garat JM: Conservative treatment of phimosis in children using a topical steroid. Urology. 2000; 56: 307-10.
- Chu CC, Chen KC, Diau GY: Topical steroid treatment of phimosis in boys. J Urol. 1999; 162: 861-3.
- Garcia de Freitas R, Nobre YD, Demarchi GT, Hachul M, Macedo A Jr, Srougi M, et al.: Topical treatment for phimosis: Time span and other factors behind treatment effectiveness. J Pediatr Urol. 2006; 2: 380-5.
- Van Howe RS: Cost-effective treatment of phimosis. Pediatrics. 1998; 102: E43.
- Berdeu D, Sauze L, Ha-Vinh P, Blum-Boisgard C: Cost-effectiveness analysis of treatments for phimosis: a comparison of surgical and medicinal approaches and their economic effect. BJU Int. 2001; 87: 239-44.
- Van Howe RS: A cost-utility analysis of neonatal circumcision. Med Decis Making. 2004; 24: 584-601.
- Schoen EJ, Colby CJ, To TT: Cost analysis of neonatal circumcision in a large health maintenance organization. J Urol. 2006; 175: 1111-5.
____________________
Accepted
after revision:
August 20, 2009
_______________________
Correspondence
address:
Dr. Yuri Dantas Nobre
Av. Senador César Vergueiro, 409
Ribeirão Preto, SP, 14020-500, Brazil
Fax: + 55 16 3236-3646
E-mail: yuridantas@ig.com.br
EDITORIAL COMMENT
This
randomized trial compares the efficacy and costs of an 8-week topical
treatment with 0.2 betamethasone and hyaluronidase vs. primary circumcision
in children with phimosis. The authors concluded that topical steroid
treatment reduced the costs by 27.3% in comparison with circumcision.
Only a few pharmacoeconomic analyses related to the treatment of these
two groups have been published in the literature. However, I am skeptical
about the definition of phimosis according to the Kayaba’s (1) classification.
What the authors defined as phimosis may well represent physiological
phimosis. In the physiological phimosis, the non-retractile foreskin forms
a normal and unscarred preputial orifice and when the foreskin is retracted,
the preputial meatus opens as a flower. The appearance of pathological
phimosis is clear with the preputial orifice white, indurated, and scarred.
I am wondering whether children were treated because of physiological
phimosis that would resolve spontaneously up to adolescence.
I must acknowledge the effort of the authors
in setting this study together. However, there are some limitations related
to this study. First, because of the relatively small number of patients
the results of this trial may reflect a low statistical power rather than
real differences between the two methods used. Second, we cannot exclude
the possibility that another density of betamethasone would have different
results than those observed here. How and why the authors chose a 0.2%
betamethasone and hyaluronidase cream? An additional concern is that,
although the authors compare a topic steroid to primary circumcision,
one might question whether steroid is superior to a control group. Unless
the authors include this group, the study may present biased and incomplete
information.
REFERENCE
- Kayaba H, Tamura H, Kitajima S, Fujiwara Y, Kato T, Kato T: Analysis of shape and retractability of the prepuce in 603 Japanese boys. J Urol. 1996; 156: 1813-5.
Dr. George Vaos
Department of Pediatric Surgery
Alexandroupolis University Hospital
Democritus University of Thrace School of Medicine
Alexandroupolis, Greece
E-mail: gvaos@hotmail.com
EDITORIAL COMMENT
Local corticosteroid application has become a popular alternative to the surgical treatment for phimosis during the last decade. Thus, it is useful to compare these treatment modalities also from the economical point of view. It was interesting that the nonsurgical treatment was more economical despite a quite high failure rate in this study. The reported success rates of the corticosteroid treatment are very variable, perhaps because of the patient selection. It is important to distinguish physiologic congenital phimosis and pathological phimosis with scars when deciding whether or not to treat. It has been shown that the incidence of phimosis is 50% at the age of 1 year, 8% at the age of 6 years and 1 % at the age of 15 years (1). The possible health benefit for treating physiologic phimosis is controversial. In our hospital, physiologic phimosis is treated only in the rare cases with significant symptoms e.g. in voiding. In non-symptomatic cases, spontaneous resolution of phimosis is delayed until puberty. In pathologic phimosis, the prepuce is scarred mostly due to skin disease balanitis xerotica obliterans. Usually pathological phimosis is not observed before school age. In our hospital, the main indication for circumcision is pathological phimosis with scars. In the present series, no patient had pathological phimosis and few had symptoms. I find the indications for treatment unclear in this study and think that it could have been more economical not to treat most of these patients at all.
REFERENCE
- Berdeu D, Sauze L, Ha-Vinh P, Blum-Boisgard C: Cost-effectiveness analysis of treatments for phimosis: a comparison of surgical and medicinal approaches and their economic effect. BJU Int. 2001; 87: 239-44.
Dr. Seppo Taskinen
Department of Pediatric Surgery
Helsinki University Central Hospital
Helsinki, Finland
E-mail: seppo.taskinen@hus.fi