RATE
OF RENAL CELL CARCINOMA SUBTYPES IN DIFFERENT RACES
(
Download pdf )
Clinical Urology
Vol. 37 (1):
29-34, January - February, 2011
doi: 10.1590/S1677-55382011000100004
ALEXANDER SANKIN, JACOB COHEN, HONGBEI WANG, RICHARD J. MACCHIA, NICHOLAS KARANIKOLAS
State University of New York Downstate Medical School, Brooklyn, New York, USA
ABSTRACT
Purpose:
We sought to identify racial differences among histological subtypes of
renal cell carcinoma (RCC) between black and non-black patients in an
equal-access health care system.
Materials and Methods: We established a
multi-institutional, prospective database of patients undergoing partial
or radical nephrectomy between January 1, 2000 and Sept 31, 2009. For
the purposes of this study, data captured included age at diagnosis, race,
tumor size, presence of lymphovascular invasion, presence of capsular
invasion, margin status, and tumor histology.
Results: 204 kidney tumors were identified
(Table-1). Of these, 117 (57.4%) were in black patients and 87 (42.6%)
were in non-black patients. Age at surgery ranged from 37 to 87 with a
median of 62. Tumor size ranged from 1.0 to 22.0 cm with a median of 5.0
cm. Overall, tumors were composed of clear cell RCC in 97 cases (47.5%),
papillary RCC in 65 cases (31.9%), chromophobe RCC in 13 cases (6.4%),
collecting duct/medullary RCC in 2 cases (1.0%), RCC with multiple histological
subtypes in 8 cases (3.9%), malignant tumors of other origin in 6 cases
(2.9%), and benign histology in 13 cases (6.4%). Among black patients,
papillary RCC was seen in 56 cases (47.9%), compared to 9 cases (10.3%)
among non-black patients (p < 0.001) (Table-2). Clear cell RCC was
present in 38 (32.5%) of black patients and in 59 (67.8%) of non-blacks
(p < 0.001).
Conclusions: In our study, papillary RCC
had a much higher occurrence among black patients compared to non-black
patients. This is the first study to document such a great racial disparity
among RCC subtypes.
Key
words: kidney neoplasm; renal cell; carcinoma
Int Braz J Urol. 2011; 37: 29-34
INTRODUCTION
Renal cell carcinoma (RCC) is the seventh most common human malignancy, having accounted for approximately 59,702 new cancer cases in the United States in 2009 (1). The histological classification of RCC has undergone several major revisions, with the current 2004 World Health Organization (WHO) guidelines incorporating new cytogenetic findings and molecular markers that help guide diagnosis, prognosis, and therapy (2). RCC is now recognized to be a complex neoplasm consisting of several different tumor subtypes, each with distinct genetic and clinical features. Previous population-based studies on racial differences in incidence patterns and outcomes of RCC have failed to account for the different histological subtypes of RCC (3). We sought to identify racial differences in the patterns of histological subtypes of RCC in a racially diverse, equal-access health care system.
MATERIALS AND METHODS
We performed a multi-institutional, retrospective review of patients undergoing partial or radical nephrectomy between January 1st, 2000 and Sept 31st, 2009. Our hospitals included a tertiary care academic center, a veteran’s administration hospital, and an inner-city county hospital, ensuring a mixed ethnic population. All slides underwent centralized pathology review using the WHO 2004 Classification of renal cell histology to classify tumors into clear cell, papillary, chromophobe, or medullary/collecting duct varieties. We did not differentiate between papillary RCC type 1 and papillary RCC type 2. Data was collected by reviewing patient charts and capturing the following parameters: age at diagnosis, race, tumor size, presence of lymphovascular invasion, presence of capsular invasion, margin status, and tumor histology.
RESULTS
Two hundred and four kidney tumors were identified (Table-1). Of these, 117 (57.4%) were in black patients and 87 (42.6%) were in non-black patients. Age at surgery ranged from 37 to 87 with a median age of 62. Among black patients the age range was 37 to 82 with a median of 63 and among non-black patients the age range was 40 to 87 with a median of 60.
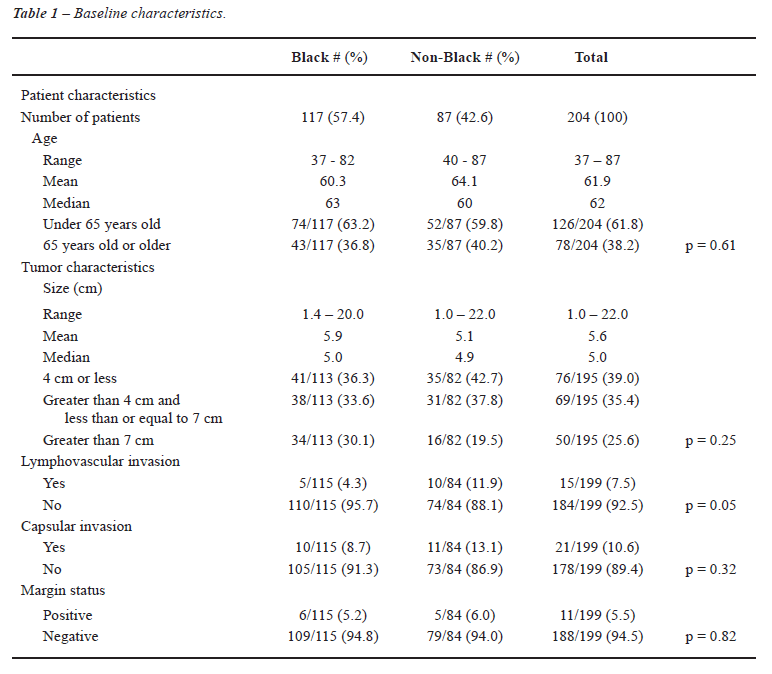
Tumor size ranged from 1.0 to 22.0 cm with
a median of 5.0 cm. The size of tumors among blacks ranged from 1.4 to
20.0 cm and from 1.0 to 22.0 cm in non-blacks. There was no statistically
significant difference in tumor size between blacks and non-blacks when
subdivided into groups of 4 cm or less, greater than 4 cm and less than
or equal to 7 cm, and greater than 7 cm ( p = 0.25).
The majority of tumors in blacks and non-blacks had absence of lymphovascular
invasion (4.3% and 11.9%, p = 0.05), absence of capsular invasion (91.3%
and 86.9%, p = 0.32), and negative surgical margins (94.8% and 94.0%,
p = 0.82).
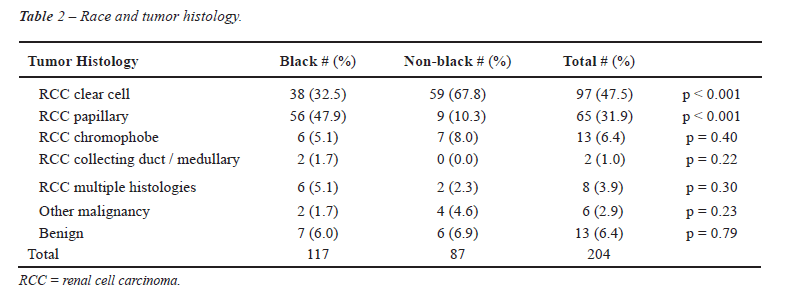
Overall, tumors were composed of clear cell
RCC in 97 cases (47.5%), papillary RCC in 65 cases (31.9%), chromophobe
RCC in 13 cases (6.4%), collecting duct/medullary RCC in 2 cases (1.0%),
RCC with multiple histological subtypes in 8 cases (3.9%), malignant tumors
of other origin in 6 cases (2.9%), and benign histology in 13 cases (6.4%).
Among black patients, papillary RCC was seen in 56 cases (47.9%), compared
to 9 cases (10.3%) among non-black patients (p < 0.001) (Table-2).
Clear cell RCC was present in 38 (32.5%) of black patients and in 59 (67.8%)
of non-blacks (p < 0.001).
COMMENTS
Our
study found a greater than four-fold increase in occurrence of papillary
RCC in blacks when compared to non-blacks. This is the first study to
document such a large ethnic disparity among RCC subtypes.
This phenomenon of neoplastic variability
among different races has been observed in other urologic cancers. Prostate
cancer is a well-studied malignancy that tends to behave differently among
different races. Compared with whites, blacks are more likely to be diagnosed
with prostate cancer at a younger age (4). Black patients with prostate
cancer are also less likely to be treated with surgical intervention and
have an overall lower survival (5).
There are many previously reported, large,
population-based studies elucidating the racial disparities among patients
with RCC. These reports, however, have focused on topics such as overall
survival and access to health care. A recent paper by Stafford et al.
found that blacks had an overall increase in incidence of renal cell carcinoma
and decrease in survival rate when compared to other ethnicities (6).
Zini et al. concluded that black patients with RCC were 50% less likely
to undergo nephrectomy compared to white patients (7). A study by Brendt
et al. also addresses the lower survival rate among blacks with renal
cell carcinoma and proposes that this may be explained by both a higher
number of comorbidities and lower rate of surgical treatment (8). While
these studies have unearthed many interesting data trends among RCC cases,
none have included information on histological subtypes of RCC.
Beyond the well-described association or
renal medullary carcinoma with sickle-cell disease and trait in black
patients, there has been very little reported regarding racial differences
for the other RCC histologies (9). Historically, clear cell tumors have
accounted for 70-80% of RCC, followed by 10-15% for papillary, 3-5% for
chromophobe, and 1-2% for medullary/collecting duct (10). Our reported
47.9% incidence of papillary tumors among black patients is the first
of its kind and is more than four-fold the incidence of papillary tumors
among non-black patients in our study. One explanation for this observation
may be a genomic predisposition for blacks to express genes unique for
the development of papillary RCC.
Papillary RCC is commonly found in two classic
genetic syndromes, hereditary papillary RCC and hereditary leiomyomatosis
and renal cell cancer syndrome. Papillary tumors have also previously
been reported to be associated with acquired renal cystic disease. The
chromosomal abnormalities for papillary tumors are distinct from the chromosome
3 and Von-Hippel Lindau gene abnormalities of clear cell tumors. Papillary
tumors typically demonstrate trisomy of chromosomes 7 and 17 and loss
of the Y chromosome. Mutations in the met-oncogene, which encodes hepatocyte
growth factor, is the usual mutation for papillary tumors, which usually
display multicentricity and hypovascularity. As expected with the new
era of targeted therapies for RCC, unique molecular agents separate from
tyrosine kinase inhibitors are being developed for papillary tumors. If
black patients with RCC truly have a predisposition for expression of
papillary type tumors, they may benefit from early counseling and treatment
with novel agents targeting this unique tumor.
More recently, papillary RCC has been subdivided
into type 1 and type 2, with type 2 tumors exhibiting more aggressive
clinicopathological features and worse prognosis (11). Our retrospective
analysis does not allow statements regarding the influence of tumor subtype
on clinical course and prognosis following treatment. As such, we do not
present any outcomes data and do not differentiate between subtypes of
papillary RCC. Of note, there have been studies demonstrating no differences
in disease-free survival between papillary and clear cell RCC (12).
One must also consider the possible influence
of confounding factors on the variable expression of RCC subtypes. Previous
studies have shown that there is a predisposition among males and patients
with end stage renal disease to develop papillary RCC (13,14). This potential
bias should be taken into consideration when designing future studies
aimed to capture racial differences observed among RCC subtypes.
CONCLUSION
We report for the first time, to our knowledge, that black patients seem to have an increased risk of developing papillary RCC than the general population. This result needs to be confirmed by large, population-based studies that examine different RCC histologies against a wide range of demographic, geographic, and environmental factors. Given the complex genetic and molecular basis for RCC and its role in response to adjuvant treatments, race and ethnicity may be important factors when counseling patients regarding prognosis and treatment outcomes.
CONFLICT OF INTEREST
None declared.
REFERENCES
- American Cancer Society: Cancer Facts & Figures 2009. Atlanta: American Cancer Society 2009. Available at. http://oralcancerfoundation.org/facts/pdf/Us_Cancer_Facts.pdf
- Lopez-Beltran A, Scarpelli M, Montironi R, Kirkali Z: 2004 WHO classification of the renal tumors of the adults. Eur Urol. 2006; 49: 798-805.
- Vaishampayan UN, Do H, Hussain M, Schwartz K: Racial disparity in incidence patterns and outcome of kidney cancer. Urology. 2003; 62: 1012-7.
- Shao YH, Demissie K, Shih W, Mehta AR, Stein MN, Roberts CB, et al.: Contemporary risk profile of prostate cancer in the United States. J Natl Cancer Inst. 2009; 101: 1280-3.
- Schwartz K, Powell IJ, Underwood W 3rd, George J, Yee C, Banerjee M: Interplay of race, socioeconomic status, and treatment on survival of patients with prostate cancer. Urology. 2009; 74: 1296-302.
- Stafford HS, Saltzstein SL, Shimasaki S, Sanders C, Downs TM, Sadler GR: Racial/ethnic and gender disparities in renal cell carcinoma incidence and survival. J Urol. 2008; 179: 1704-8.
- Zini L, Perrotte P, Capitanio U, Jeldres C, Duclos A, Arjane P, et al.: Race affects access to nephrectomy but not survival in renal cell carcinoma. BJU Int. 2009; 103: 889-93.
- Berndt SI, Carter HB, Schoenberg MP, Newschaffer CJ: Disparities in treatment and outcome for renal cell cancer among older black and white patients. J Clin Oncol. 2007; 25: 3589-95.
- Assad L, Resetkova E, Oliveira VL, Sun W, Stewart JM, Katz RL, et al.: Cytologic features of renal medullary carcinoma. Cancer. 2005; 105: 28-34.
- Reuter VE, Presti JC Jr: Contemporary approach to the classification of renal epithelial tumors. Semin Oncol. 2000; 27: 124-37.
- Yamashita S, Ioritani N, Oikawa K, Aizawa M, Endoh M, Arai Y: Morphological subtyping of papillary renal cell carcinoma: clinicopathological characteristics and prognosis. Int J Urol. 2007; 14: 679-83.
- Dall’Oglio MF, Antunes AA, Pompeo AC, Mosconi A, Leite KR, Srougi M: Prognostic relevance of the histological subtype of renal cell carcinoma. Int Braz J Urol. 2008; 34: 3-8.
- Schrader AJ, Sevinc S, Olbert PJ, Hegele A, Varga Z, Hofmann R: Gender-specific characteristics and survival of renal cell carcinoma. Urologe A. 2008; 47: 1182, 1184-6.
- Ishikawa I, Kovacs G: High incidence of papillary renal cell tumours in patients on chronic haemodialysis. Histopathology. 1993; 22: 135-9.
____________________
Accepted after revision:
July 30, 2010
_______________________
Correspondence address:
Dr. Alexander Sankin
Division of Urology
State Univ. of New York Downstate Medical School
450 Clarkson Ave,
Brooklyn, NY, 11203, USA
Fax: + 1 718 270-3848
E-mail: alexsankin@gmail.com
EDITORIAL COMMENT
We
have known for a while that renal cell carcinomas (RCC) are more common
in blacks compared to non-Blacks and Asians. Not only more common, RCC
tend to be more aggressive in blacks, with a higher disease-specific mortality
even when tumor size and stage are independent variables. Black patients
have a significantly higher incidence rate and lower survival rate than
all other races/ethnicities even when having more localized cancer.
This study lists the rates of different
types of renal cell carcinoma in a population composed of many ethnicities.
In blacks, almost half of all tumors were papillary RCC, compared to only
10% in non-blacks. This disparity is not commonly addressed. In addition,
it found a much lower rate of clear cell RCC in blacks, which is not a
common finding in the literature. The readers could have benefited by
data on survival or progression, which unfortunately the study lacks.
Nonetheless, given such racial disparities in renal cell carcinoma incidence
in this one study, one should consider expanding and confirming these
findings that may help elucidate biological, behavioral and environmental
factors that can potentially be addressed.
Dr.
Fabio Tavora
Department of Pathology
Hospital de Messejana Dr. Carlos Alberto Studart
Fortaleza, CE, Brazil
E-mail: ftavora@gmail.com
EDITORIAL COMMENT
Renal
cell carcinoma (RCC) tends to manifest variable prognoses and outcomes.
Previous articles have already pointed toward prognostic parameters including
pathological subtypes and ethnic origin. Yet the issue of race was not
fully addressed. Epidemiologic literature showed shorter survival in Black
Americans with RCC. Tripathi et al. concluded that the overall survival
for metastatic RCC was significantly shorter for Black Americans. Vaishampayan
et al. had a similar conclusion for local RCC, emphasizing a higher incidence,
poorer outcome in Black patients with a similar age and stage. However,
the histology subtypes disparities were not mentioned, demonstrating the
advantage of the recent manuscript based on data that was retrieved from
an equal-access health care system. Stafford published a major study comparing
ethnic groups (White, Black, Hispanic and Asian -Pacific) concluding that
Black patients tend to have a higher incidence and a shorter survival
while Asian patients demonstrate the opposite. Yet even this article did
not point to the histology subdivision.
Herein we can appreciate an important study
advancing our knowledge regarding the correlation between race and RCC
histology subtypes. Further studies should investigate the papillary predominance
of the RCC in the black population while paradoxically demonstrating a
poorer prognosis than what was known previously for that histological
subtype.
REFERENCES
- Tripathi RT, Heilbrun LK, Jain V, Vaishampayan UN: Racial disparity in outcomes of a clinical trial population with metastatic renal cell carcinoma. Urology. 2006; 68: 296-301.
- Vaishampayan UN, Do H, Hussain M, Schwartz K: Racial disparity in incidence patterns and outcome of kidney cancer. Urology. 2003; 62: 1012-7.
- Berndt SI, Carter HB, Schoenberg MP, Newschaffer CJ: Disparities in treatment and outcome for renal cell cancer among older black and white patients. J Clin Oncol. 2007; 25: 3589-95.
- Zini L, Perrotte P, Capitanio U, Jeldres C, Duclos A, Arjane P, et al.: Race affects access to nephrectomy but not survival in renal cell carcinoma. BJU Int. 2009; 103: 889-93.
- Stafford HS, Saltzstein SL, Shimasaki S, Sanders C, Downs TM, Sadler GR: Racial/ethnic and gender disparities in renal cell carcinoma incidence and survival. J Urol. 2008; 179: 1704-8.
Dr.
Avraham Shtricker
Department of Urologic Surgery
The E. Wolfson Medical Center
Holon, Israel
E-mail: shtrickeravi@hotmail.com