DIFFICULT
MALE URETHRAL CATHETERIZATION: A REVIEW OF DIFFERENT APPROACHES
(
Download pdf )
CARLOS VILLANUEVA, GEORGE P. HEMSTREET III
Section of Urology, University of Nebraska Medical Center, Omaha, Nebraska, USA
ABSTRACT
Purpose:
To review and compare the different methods for difficult male urethral
catheterization described in selected literature.
Materials and Methods: A PubMed search was
done with the terms “difficult”, “failed”, or
“complications” and “urethral catheterization”,
“transurethral catheterization”, “Foley catheter”,
“urethral catheter” or “filiforms and followers”.
All articles addressing the issue of difficult adult male urethral catheterization
were included.
Results: Six main approaches were identified
on the 14 articles included for review: 1) Passage of either a Glidewire,
guide wire or filiform under direct vision; 2) Blind passage of a filiform,
guide wire, Glidewire or hydrophilic catheter; 3) “The Peel-away®
sheath placed on a cystoscope/resectoscope technique”; 4) “The
rigid ureteroscope placed inside the 22F Foley technique”; 5) Suprapubic
catheterization; and 6) “The instillation of 60 cc of saline through
the catheter as it is advanced technique”.
Conclusion: There is a paucity of prospective
data comparing the benefits, risks, success rates and complications of
the different approaches for difficult Foley catheter placement. Our suggested
approach starts with the initial attempt at urethral catheterization with
an 18F coude and a 12F silicone catheter. If these fail, using a flexible
cystoscope or the blind Glidewire technique are reasonable alternatives.
If dilatation of a stricture is necessary, ureteric dilatators or a urethral
balloon dilatator are recommended.
Key
words: urethra; male; catheterization
Int Braz J Urol. 2008; 34: 401-12
INTRODUCTION
Difficult
male urethral catheterization (DUC) is a common problem for the general
urologist. Common causes of DUC in normal urethras include a tight external
sphincter in an anxious patient, or poor technique. Additional pathologic
causes include urethral strictures, phimosis, anasarca, bladder neck contractures,
prostate cancer, false passages or benign prostatic hypertrophy (BPH),
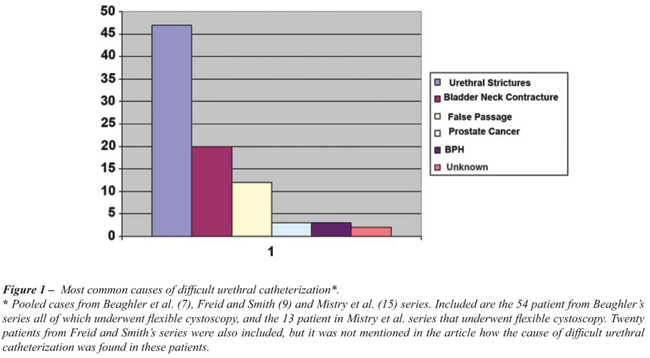
among others (Figure-1). It is underappreciated that a DUC can result
in serious morbidity to the patient. The significance of this problem
is exemplified by the complications from difficult catheterizations that
include Fournier’s gangrene (1), rectal perforation, bleeding requiring
transfusion, formation of urethral strictures and sepsis.
This article reviews the alternative methods
of approaching the difficult-to-catheterize patient described in the literature.
MATERIALS AND METHODS
A PubMed search was programmed with the terms “difficult”, “failed”, or “complications” and “urethral catheterization”, “transurethral catheterization”, “Foley catheter”, “urethral catheter” or “filiforms and followers” in April of 2008. All articles addressing the issue of difficult adult male urethral catheterization were included. A DUC was defined for the purpose of this article as being unsuccessful at urethral catheterization of the bladder after the initial attempts.
RESULTS
A
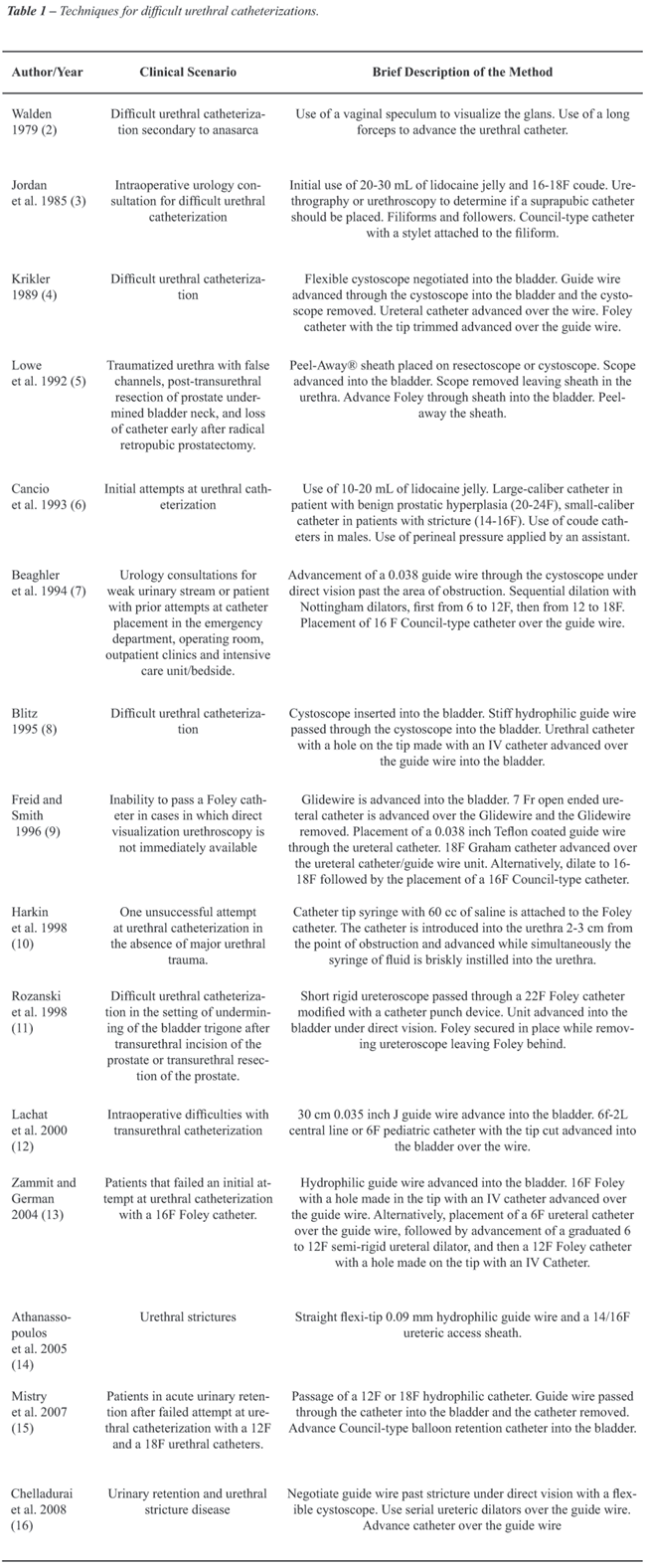
summary of the different techniques for urethral catheterization after
an unsuccessful attempt is shown in Table-1. Following is a summary of
the articles included for review in the chronological order in which they
were published. Each paragraph starts with a brief description of the
technique. The following information from each article was included when
available: risks and benefits of the technique mentioned in the article,
complications, success rate, and patient outcomes. All of the statements
in each paragraph are derived from the article being discussed.
In 1976, Walden (2) published a technique
for DUC in the patient with anasarca using a vaginal speculum. The speculum
is passed through the preputial opening down to the glans, and with the
use of a long-handled forceps the catheter is advanced into the bladder.
He used it in 3 patients, one of whom was a 450-pound (220 kg.) man in
which the glans was 11 cm into the swollen prepuce.
Jordan et al. (3) addressed the issue of
consultation for DUC in the operating room in 1985. After a through history
of previous attempts, past medical history and genitourinary examination,
if there are no contraindications to proceed with urethral catheterizations,
the first step is the instillation of 20-30 mL of 2% lidocaine jelly or
other water-soluble lubricating jelly into the urethra. The authors advocated
injecting a large volume of jelly for gentle dilation. A 16-18F coude
catheter is preferred over a small catheter, which may not be stiff enough
to maneuver the difficult urethra. If this is unsuccessful, proceed with
either urethroscopy or urethrography. The information gathered from direct
or indirect visualization of the urethra would then lead to either suprapubic
catheter placement or passage of filiforms. When to proceed with suprapubic
catheterization versus the placement of filiforms was not discussed in
their article. The passage of a filiform through the point of obstruction
should preferentially be done under direct vision. For the blind passage
of filiforms it is imperative not to remove the filiform that meets obstruction
but to continue placing filiforms until one passes the point of obstruction.
When using filiforms and followers it is recommended to dilate only up
to 16-18 F and no larger in order to prevent further damage to the urethra.
Finally, a Council tip catheter is advanced over a stylet attached to
the filiform. Alternatively, a balloon urethral dilator system that can
be passed using a filiform could be used instead. Without supporting data,
the authors stated that this balloon system may be better than the use
of followers. No specific data regarding success rates or complications
was reported in the study.
Krikler (4) described for the first time
in 1989 the use of flexible urethroscopy for DUCs. “The cystoscope
is negotiated into the bladder, a guidewire is passed through the cystoscope,
and the instrument withdrawn leaving the guidewire in place. A ureteric
catheter may be passed over the guidewire first and then the tip of a
suitable Foley catheter is trimmed to produce an end hole. This allows
the catheter to be threaded down the guidewire”. He did not make
any particular recommendations in the case where a stricture prevented
the passage of the flexible cystoscope. This method was recommended for
patients in whom suprapubic catheterization is contraindicated or who
are known to have false passages or urethral diverticula.
Lowe et al. (5) in 1992 discussed the management
of the DUC in patients with multiple false passages, who had just a difficult
dilatation with filiforms and followers, in the case of undermining of
the bladder neck after trans-urethral resection of the prostate (TURP)
or in the early postoperative period after a radical prostatectomy when
the catheter came out. The authors described the use of a specially made
urethral protective sheath that can be placed on a cystoscope or resectoscope
to facilitate guiding the catheter into the bladder. A Peel-Away®
Sheath (Cook Urological, Spencer, IN) is placed around the cystoscope
or resectoscope at the beginning of the case. Once the case is completed,
the cystoscope/resectoscope is placed in the bladder and then it is removed
leaving the sheath in place. A Foley catheter (with or without a catheter
guide) is advanced through the sheath into the bladder, the balloon inflated,
and the sheath peeled away. In the case of an unexpectedly difficult cystourethroscopy,
once in the bladder, a guide wire can be passed, the cystoscope removed
and then reinserted over the wire after placing a Peel-Away® sheath
over the scope. The main problem encountered with this technique was kinking
of the sheath, which can be prevented by not pulling up or downward on
the phallus after the cystoscope has been removed. Kinking of the sheath
can also be approached by the use of a catheter guide. This technique
was used in 20 difficult catheterizations, with 3 failures, 2 due to kinking
of the sheath and one because of the development of an erection making
the sheath not long enough to reach the bladder. The authors hypothesized
that the Teflon sheaths could be less traumatic to the urethra than the
resectoscope sheath and that the use of the sheaths over the resectoscope
during a TURP may decrease the post-TURP stricture rate although no data
was provided to support this statement.
Cancio et al. (6), in 1993, described a
series of initial maneuvers when managing the difficult to catheterize
patient. “Start with the injection of 10-20 mL of lubricant in the
urethra and use a 16-18F catheter first. The use of 1% lidocaine jelly
as the lubricant makes the procedure more tolerable for the patient and
may prevent sphincter spasm. When a stricture is suspected, either because
blockage is encountered soon after entering the meatus or because of a
history of instrumentation (e.g., TURP), use a smaller catheter (14-16F).
If a 14F catheter will not pass, a smaller catheter will not pass either.
For the patient with suspected BPH, use a larger catheter (20-24F). Perineal
pressure by an assistant during catheter insertion can help direct the
catheter into the prostatic urethra. Coude catheters were recommended
for suspected BPH and to prevent injury to the membranous and bulbar urethra.
Beaghler et al. (7) method was described
in 1994. This method incorporates the use of a 16F flexible cystoscope,
after injecting 2% lidocaine jelly, to pass a 0.038-inch standard guide
wire through the obstruction. The urethra is then dilated over the wire
with Nottingham dilators 6-12F and 12-18F, and successful catheterization
is accomplished by placing a 16F council catheter over the wire. This
method was attempted in 54 patients prospectively with a success rate
of 96%. These patients were seen if urology consultation was requested
because of difficulty in placing a Foley or for complaints of weak urinary
stream and urinary retention (26% outpatient clinics, 33% bedside/Intensive
care unit, 13% emergency room, 28% operating room). Before attempting
the method, catheterization was attempted by standard bedside techniques,
including use of various catheters sizes and Coude-tipped catheters. The
number of catheters, sizes and types was not specified in the paper, neither
was the success rate with these initial maneuvers. The 2 patients in whom
this method failed had dense bladder-neck contractures and had a suprapubic
catheter placed after a failed attempt at dilating with filiforms and
followers. The authors described no complications with little or no discomfort
to the patient. The most common causes for difficult Foley catheter placements
in this cohort (in order of most to least common) were urethral strictures,
bladder-neck contractures, false passages, and locally-advanced prostate
cancer.
In 1995, Blitz (8) described a method used
in 8 patients that had endoscopic prostate or urethral surgery in which
catheters were placed with prior difficulty. With the cystoscope in the
bladder, a 0.038 stiff hydrophilic Glidewire is introduced and allowed
to coil inside the bladder. Then a “16 G IV catheter with a needle
is passed into the distal drainage hole of the urethral catheter and out
through the center of the urethral catheter”. The needle is then
removed and the wire passed through the catheter. After removing the IV
catheter, the wire is directed inside the drainage lumen of the urethral
catheter. This maneuver avoided the need for a Council tip catheter, and
was better than the alternative of cutting the tip of the Foley with scissors
affecting the curvature of the tip of the catheter. A variety of urethral
catheters can be used with this method. This approach was successful in
all 8 patients. Five patients had just undergone a TURP,, 2 patients were
status/post direct vision internal urethrotomy, and 1 patient was status/post
laser prostatectomy. They stated that their experiences with other wires,
including Teflon-coated spiral wound guide wires, do not allow such ease
of advancement and might cause the catheter to buckle as it is pushed
into the bladder. Ex vivo experimentation comparing the Microvasive®
Glidewire (Microvasive, Natick, MA) with a Microvasive Lubriglide hydrophilic-coated
spiral wound guide wire was nearly equivalent in a subjective evaluation.
Freid and Smith (9) in 1996 described for
the first time the use of a 0.038 inch hydrophilic Glidewire (preferentially
with an angled or floppy tip) placed blindly into the bladder in a manner
similar to a filiform for cases of DUC. The Glidewire is prepared by injecting
5 cc of saline to activate the hydrophilic coating. Lidocaine jelly is
then injected in the urethra, followed by the introduction and advancement
of the Glidewire with a gentle steady pressure using a gauze pad to grasp
it. When resistance is felt, the Glidewire is advanced until either it
enters the bladder or the tip appears in the meatus. In the latter situation,
the Glidewire is removed and another attempt is made at passing it into
the bladder. Entrance into the bladder is inferred by passage of approximately
75 cm of the Glidewire in the urethra without the reappearance of the
tip or a coil at the meatus. Then a 7F ureteral catheter (preferentially
with a tapered tip) is threaded over the wire and then, following documented
urine return corroborating correct placement, the first wire is exchanged
for a 0.038 PTFE coated guidewire. An attempt is made to introduce an
18F Graham catheter over the guide wire/ureteral catheter unit, or alternatively
the urethra is dilated to 16-18F and a 16F Council catheter is advanced
over the wire. The authors recommended this method over standard filiforms
and followers when cystoscopy was not immediately available. This method
was used most frequently after failed attempts with filiforms and followers.
The reported success rate was 95% (19/20). This method failed in a patient
who had a pinhole urethral stricture that necessitated cystourethroscopy
with direct vision internal urethrotomy. The authors reported no complications.
The most common causes of the difficulty in placing the catheter were,
in order of most to least common: urethral strictures, bladder neck contracture,
BPH and unknown. It is unclear how the causes were determined since it
was not stated that the patients underwent cystoscopy or other studies.
Harkin et al. (10), in 1998, introduced
an entirely different technique that did not involve wires, cystoscopes,
IV catheters, or dilators. Their method consists of connecting a catheter
tip syringe loaded with 60 mL of saline to the Foley, inserting the Foley
up to where resistance is encountered, and then advancing the Foley while
at the same time briskly instilling saline into the distal urethra. It
was hypothesized that the flow of fluid distended the urethra facilitating
the passage of the catheter, particularly in cases of BPH. The authors
recommended using this technique after an unsuccessful attempt at urethral
catheterization in the absence of any signs of major urethral trauma.
A 100% success rate was reported in over 30 patients. The causes for the
difficulty in catheterizing these patients were not mentioned in the study.
They recommended aborting the procedure if severe pain or major resistance
were encountered.
Rozanski et al. (11) in 1998 described a
technique used in 2 patients with significant undermining of the trigone
after transurethral incision of the prostate. In these patients a wire
was introduced into the bladder (into a barely visible opening at the
12 o’clock position) and multiple attempts to place a Council catheter
over the wire failed. Using a 22F Foley with a punch hole at the tip,
they inserted a 6 F ureteroscope into the Foley with the tip of the ureteroscope
several millimeters beyond the catheter tip, and inserted the ureteroscope
and the catheter into the bladder under direct vision. The Foley was grasped
securely and the ureteroscope was pulled out. They recommended the use
of this technique whenever catheterization is difficult or potentially
complicated following transurethral surgery.
Lachat et al. (12) in the year 2000 described
a technique for the intraoperative DUC. It consists of advancing a 30
cm 0.035 inch J guide wire through the urethra into the bladder, followed
by either a 6F-2L central line or a 6F pediatric catheter with the tip
cut off advanced over the wire. This method was used with success in 21
patients undergoing cardiovascular surgery in which difficulties with
transurethral catheterization were encountered. In 5 patients, 2 or more
attempts were required to advance the wire into the bladder. Fluoroscopic
guidance was recommended for placement of the wire when a false passage
was suspected.
In 2004, Zammit and German (13) presented
a method suggesting the blind passage of a Glidewire (as described by
Freid and Smith (9)) as well as the use of an 18 G IV catheter to perforate
the tip of the urethral catheter (as described by Blitz (8)). With this
method a 0.89 mm Terumo Radiofocus® (Terumo Corp., Tokyo, Japan) Guide
Wire M Straight is blindly inserted into the bladder by advancing at least
40 cm of the wire into the urethra (with the urethra being an average
of 20 cm, this assures that the wire did not double back on itself). Subsequently
an attempt is made to thread a 16F urethral catheter over the wire (tip
perforation according to the technique described by Blitz (8)). If this
is unsuccessful, the possibility of a urethral stricture is considered
and a 6 F ureteral catheter is inserted. If there are no difficulties
inserting the ureteral catheter this is removed and a graduated 6F to
12F semi-rigid ureteric dilator (flexible ureteroscopy introducer) is
advanced over the wire into the bladder. This allows the insertion of
a 12 F urethral catheter over the guide wire using the method described
by Blitz. The authors recommended aborting the procedure if there were
any difficulties when inserting the 6F ureteral catheter. The success
rate was not reported. However, it was mentioned that patients tolerated
the procedure well, and that the cases in which this technique were not
successful was due to the creation of a false passage at the initial catheterization
attempt. Of note, this method was applied after a failed attempt at urethral
catheterization with a 16F catheter.
In a letter to Zammit and German (13) Athanassopoulos
et al. (14) mentions their unpublished experience using a straight flexi
tip hydrophilic Glidewire and a 14/16F ureteric access sheath. They extrapolated
the efficacy and atraumatic characteristics of hydrophilic coatings in
the ureteric lumen to the urethra. They proposed that “the development
of larger diameter hydrophilic sheaths may lead to a totally atraumatic
one-step management of urethral strictures”.
More recently, Mistry et al. (15) reported
in 2007 their experience with the use of hydrophilic-coated urethral catheters
in adult males in acute urinary retention with DUC. Criteria for enrollment
included a failed attempt at passage of both a 12F and 18F urethral catheters.
Preparation of the hydrophilic catheter consisted of immersion for 5 min
in sterile water and modification of the tip to convert it into a Council-type
catheter. An attempt to pass a 12F or 18F hydrophilic catheter per urethra
was made by the urologist. If the hydrophilic catheter successfully passed
into the bladder, a guide wire was subsequently passed through the catheter.
The hydrophilic catheter was then removed leaving the wire in place, and
an attempt to place a standard balloon retention catheter over the guide
wire into the bladder was made. If either the hydrophilic catheter did
not pass or the balloon retention catheter could not be advanced over
the wire, additional intervention was left to the discretion of the physician.
Of 44 patients enrolled in the study, 30 (68.2%) underwent successful
placement of an indwelling Foley catheter with the use of this method
(hydrophilic catheter followed by guide wire followed by balloon retention
catheter). The 12F hydrophilic catheter was used to gain access into the
bladder in 26 patients and an 18F hydrophilic catheter was used in 4 patients.
The patients, in which this method was not successful, underwent flexible
cystoscopy, dilatation with filiforms and followers or Amplatz dilators,
and/or blind passage of an open ended catheter with subsequent Foley placement.
In the 13 patients that underwent cystoscopy the causes for the difficulty
in catheterizing were anterior urethral stricture in 7, bladder neck contracture
in 3 and false passage in 3. They postulated the success of the 12F hydrophilic
catheter may be related to its increased stiffness when compared to the
regular 12F latex catheter. In 4 patients, the 12F hydrophilic catheter
was inserted into the bladder with subsequent failure to pass the balloon
retention catheter over the guide wire. In these patients, benefits were
still realized (temporary drainage of painful retention, access to the
bladder with a guide wire etc.). The authors concluded that incorporating
hydrophilic catheters into the urologic armamentarium for catheterizing
the difficult urethra will benefit most patients by avoiding more invasive
and costly procedures.
Chelladurai et al. (16) recommend using
their technique for patients in urinary retention with urethral stricture
disease. Under direct vision with a flexible cystoscope, a guide wire
is negotiated past the stricture into the bladder. Well lubricated serial
ureteric dilators are introduced over the guide wire into the bladder.
A catheter is then inserted over the guide wire. Delayed definitive treatment
of the stricture is undertaken under optimal conditions. They recommend
using ureteral over urethral dilators because their narrower caliber,
hydrophilic coating and longer length ensure an easier dilatation of the
stricture with minimal patient discomfort.
COMMENTS
The
approach to the DUC in the non-trauma setting, where a catheter is needed
for urinary retention or to monitor urine output, should start with a
through history and physical examination. The history should include,
past urologic surgeries (TURP, Radical retropubic prostatectomy), previous
difficulties with catheterization, and voiding symptoms, as a clue to
the etiology of the problem. Historical information pertaining to previous
attempts by nurses or physicians is of utmost importance: the distance
at which obstruction was felt (< 16 cm indicating possible urethral
stricture, > 16 cm indicating BPH, incorrect technique, or bladder
neck contracture), whether the Foley balloon was inflated before urine
flow (alerting of possible false passage from urethral trauma) or the
types and sizes of catheters used, as well as how many people who previously
tried (the higher the number that tried could indicate a more difficult
catheterization). A focused genitourinary exam may reveal obvious causes
for the difficult catheterization penoscrotal edema, phimosis, meatal
stenosis, prostate cancer etc.
If a DUC is anticipated based on the above
information, we recommend preparing the field by scrubbing the penoscrotal
area with an antiseptic solution and placing a ¾ sheet drape from
the scrotum down to the toes. This allows both hands to remain sterile
during the procedure to assist in the passage of instruments, and prevents
contamination of guide wires, flexible cystoscopes etc. The use of at
least 10 cc of a lubricant injected into the urethra should be standard
technique. The average volume of the male urethra is 20 mL, suggesting
20 mL may theoretically be better than 10 mL, but this has not been reported
in the setting of DUC. Although most urologists use 2% viscous lidocaine,
its efficacy as an anesthetic was recently questioned in a meta-analysis
in which no difference was found when it was compared to plain gel (17).
Despite this, patients are familiar with the drug lidocaine and may derive
some placebo effect if they know that the drug is being used to numb their
urethras. A tense patient usually means a tight urethral sphincter; therefore,
patients should be encouraged to relax their legs by pointing their toes
outward, while taking slow deep breaths. A firm grasp of the penis with
the non-dominant hand, preferentially with gauze around it, pointing at
a 45 degree angle is a key element of urethral catheterization. We recommend
detaching the catheter from the Foley bag to allow better sensitivity
at detecting when passing through the external sphincter and prostate,
and to more readily identify obstruction secondary to a false passage
or stricture.
The type and size of catheter to be used
initially is a detail that has not yet been reported in the setting of
DUCs. In a recent online survey (December 2007) of US urology residents
at out institution, revealed an 18F coude catheter was the first catheter
used by the majority of residents for the DUC. With appropriate technique,
an 18F coude catheter should be advanced with ease into the bladder of
the majority of patients in which the difficulty was attributed to an
incorrect technique, BPH, or an anxious patient. Only 2 of the articles
reviewed mentioned the size / types of catheters employed during the initial
attempts at catheterization. In the article by Zammit and German (5),
one attempt with a 16F urethral catheter was performed before their method
was applied. In the Mistry et al. (15) study, patients must have failed
urethral catheterization with an 18F and a 12F urethral catheter as inclusion
criteria. As illustrated in Figure-1, there is a high probability that
if an 18F coude catheter could not be advanced into the bladder, a narrowing
of the urethra (urethral stricture, bladder neck contracture) or a false
passage is likely the cause of the problem. Since urethral strictures
and bladder neck contractures are 5 to 6 times more common than false
passages, we recommend another attempt at urethral catheterization with
a smaller catheter. Silicone catheters are stiffer than the regular latex
catheters and can theoretically provide an advantage when passing a stricture.
We use a 12F silicone catheter after a failed attempt with an 18F coude
catheter. The use of more than these 2 catheters, in our opinion, is unlikely
to increase the probability of a successful catheterization.
The technique of instilling 60 cc of saline
as the catheter is advanced as described by Harkin et al. (10) is a simple
one and probably could be attempted before proceeding with any of the
other methods if BPH is suspected. This catheter instillation technique
utilizes inexpensive and readily available supplies that can be found
on any floor of the hospital or the ER. Although Harkin et al. (10) reported
a success rate of 100% in over 30 patients; these authors do not delineate
the causes for the difficulty in placing the Foley. It is intuitive that
this method would not be successful in cases of urethral stricture, false
passage, or bladder-neck contracture, the most frequent causes of DUC.
Therefore, its use is limited to a small proportion of DUCs. Also, proper
technique at urethral catheterization requires one hand to handle the
phallus and the other to maneuver the catheter, which means that an assistant
is required to push the saline. If the catheter is placed in a false passage
and saline is forcefully injected, there is a high probability of making
the false passage worse. For these reasons we do not advocate for the
use of this technique.
Once a patient failed initial attempts at
urethral catheterization, the articles reviewed recommend one of the following
general approaches: 1) Passage of either a Glidewire, guide wire or filiform
under direct vision (with the use of flexible or rigid cystoscopy) past
a visible obstruction (i.e. stricture) or into the bladder, followed by
the advancement of a modified urethral catheter over the Glidewire, filiform
or guide wire, immediately or after dilatation with followers, ureteral
dilators etc; 2) Blind passage of a filiform, guide wire, Glidewire or
hydrophilic catheter(which is then exchanged for a guide wire) followed
by the advancement of a modified urethral catheter over the Glidewire,
filiform or guide wire, immediately or after dilatation with followers,
ureteral dilators etc; 3) “The Peel-away® sheath placed on cystoscope/resectoscope
technique”; 4) “The rigid ureteroscope placed inside the 22F
Foley technique”; 5) Suprapubic catheterization; and 6) “The
instillation of 60 cc of saline through the catheter as it is advanced
technique”. In our recent online survey of US urology residents
to ascertain their approaches to the DUC, 60-70% used a flexible cystoscope,
15-20% chose to pass a Glidewire blindly, 7-9% used filiforms and followers
blindly and less than 3% elected a suprapubic catheter after their initial
failed attempts at urethral catheterization.
The article by Jordan et al. (3) discusses
the blind use of filiforms and followers. They recommend avoiding placing
filiforms blindly but also provided recommendations regarding the technique.
Freid and Smith (9) described why they stopped using filiforms in favor
of their technique. The once popular blind placement of filiforms and
followers was chosen only by 7-9% of urology residents in our recent online
survey. Other alternative methods and equipment for dilating strictures
like Heymans dilators, balloon dilators and ureteral access sheaths, have
contributed to the abandonment of the use of filiforms and followers.
To out knowledge there is no reported study comparing the use of filiforms
and followers with other techniques used for DUC. Cases of perforation
of the urethra and entrance into the rectum with followers are not unheard
of. We do not consider the blind use of filiforms and followers to be
the optimal approach to the DUC because it is difficult to ascertain if
the filiform is in the bladder and requires considerable experience to
gain this skill.
Several articles discussed above describe
the blind placement of a Glidewire. The main advantage of this approach
is that it avoids the cost and inconvenience of the use of a flexible
cystoscope. Freid and Smith (9) reported a high success rate with no complications
using this method. Insertion of a hydrophilic guide wire though the urethra
will usually gain access to the bladder without causing any trauma and
with minimal discomfort to the patient. If a Glidewire is placed into
a false lumen or cannot transverse a stricture it will usually efface
the urethral meatus. If most of the Glidewire has been advanced into the
bladder without seeing it coming back at the urethral meatus, there is
a high probability that access to the bladder was achieved. If there are
still doubts about whether the wire is in the bladder or not, a 6F ureteral
catheter can be advanced over the wire and urine aspirated or the catheter
irrigated with a syringe. Rarely, a bedside plain film of the abdomen
is needed to confirm wire placement. There are many types of Glidewires:
rigid vs. regular, angled tip vs. straight tip. Freid and Smith’s
(9) technique used an angled or floppy tip. Zammit and German (13) used
a straight tip. Which tip is better to maneuver strictures or a false
passage has not been reported. In Mistry et al. (15) article, access to
the bladder was gained first with a hydrophilic catheter followed by placement
of a guide wire. This technique adds an additional step to the blind placement
of a Glidewire. There are probably more chances of being successful at
advancing a hydrophilic Glidewire into the bladder than a 12F or 18F hydrophilic
catheter. One of the arguments in favor of using the hydrophilic catheter
was that they can readily decompress the bladder in distressed patients
in urinary retention. The passage of a Glidewire should not take more
than a couple of minutes, and once the wire is in, passing a catheter
over the wire should be quick in most situations (as it was in 30 of the
34 of their patients in which access to the bladder was achieved with
a hydrophilic catheter in their study).
As the availability of flexible cystoscopes
and catheterization carts has become commonplace in the hospital ward,
the most frequent approach to the DUC among urology residents in the US
is the use of a flexible cystoscope. This approach establishes the etiology
of the problem in a majority of cases. In the case of false passages,
where occasionally a Glidewire cannot be advanced blindly, the cystoscope
can usually be maneuvered into the bladder. Guide wires can also be passed
through pinpoint urethral strictures or bladder neck contractures under
direct vision. The disadvantages of using this approach are that flexible
cystoscopes are not always available, they are expensive, and they usually
need to be transported in a cart because of the light source. No study
has demonstrated the superiority of the use of flexible cystoscopy in
the setting of DUC over other more simple techniques like the blind use
of a Glidewire. Still, we believe that flexible cystoscopy is needed in
a small percentage of DUCs (mainly in cases of false passages and some
urethral strictures) if a suprapubic catheter is to be avoided.
The “Peel-away sheath® placed
on cystoscope/resectoscope technique” and “The rigid ureteroscope
placed inside the 22F Foley technique” are two maneuvers worth remembering
that can be used in specific scenarios but probably cannot be used in
the majority of consults for DUC. Urethral catheterization will not always
be successful despite the use of all the techniques described and suprapubic
catheterization will still be required in rare occasions.
In conclusion, there are many approaches
to the DUC described in the literature. Prospective randomized trials
comparing these approaches are needed to determine the strengths and weaknesses
of each technique. The paucity of literature related to one of the most
common urologic consults was surprising. Finally our recommended approach
to the difficult male urethral catheterization in patients with urinary
retention or that need a Foley catheter to monitor urine output is an
initial attempt with an 18F coude catheter followed by a 12F silicone
catheter. If this approach fails we suggest using the blind Glidewire
technique or a flexible cystoscope to pass a Glidewire under direct vision
as reasonable options. Once the Glidewire is confirmed to be in the bladder,
a 16 F council catheter can usually be advanced into the bladder. In cases
of urethral stricture disease, the primary approach would be to pass a
12F silicone catheter (using Blitz (8) technique) over the Glidewire without
dilating, with a delayed definitive treatment of the stricture under optimal
conditions. In cases of tight strictures in which a 12F did not pass or
when treatment of the stricture is desired, serial ureteric dilators or
a urethral balloon dilatator passed over the Glidewire are reasonable
alternatives.
CONFLICT OF INTEREST
None declared.
REFERENCES
- López Pacios JC, Sánchez Merino JM, Piñeiro Fernández MC, Bouso Montero M, Parra Muntaner L, García Alonso J. Fournier’s gangrene secondary to urethral catheterization. Arch Esp Urol. 2005; 58: 167-70.
- Walden TB: Urethral catheterization in anasarca. Urology. 1979; 13: 82.
- Jordan GH, Winslow BH, Devine CJ Jr: Intraoperative consultation for the urethra. Urol Clin North Am. 1985; 12: 447-52.
- Krikler SJ: Flexible urethroscopy: use in difficult male catheterisation. Ann R Coll Surg Engl. 1989; 71: 3.
- Lowe MA, Defalco AJ: New endourologic technique for catheter placement after TURP, prostatectomy, and difficult urethroscopy. Urology. 1992; 40: 461-3.
- Cancio LC, Sabanegh ES Jr, Thompson IM: Managing the Foley catheter. Am Fam Physician. 1993; 48: 829-36.
- Beaghler M, Grasso M 3rd, Loisides P: Inability to pass a urethral catheter: the bedside role of the flexible cystoscope. Urology. 1994; 44: 268-70.
- Blitz BF: A simple method using hydrophilic guide wires for the difficult urethral catheterization. Urology. 1995; 46: 99-100.
- Freid RM, Smith AD: The Glidewire technique for overcoming urethral obstruction. J Urol. 1996; 156: 164-5.
- Harkin DW, Hawe M, Pyper P: A novel technique for difficult male urethral catheterization. Br J Urol. 1998; 82: 752-3.
- Rozanski TA, Salazar F, Thompson IM: Direct vision bladder catheterization using a short rigid ureteroscope. Urology. 1998; 51: 827-8.
- Lachat ML, Moehrlen U, Bruetsch HP, Vogt PR: The Seldinger technique for difficult transurethral catheterization: a gentle alternative to suprapubic puncture. Br J Surg. 2000; 87: 1729-30.
- Zammit PA, German K: The difficult urethral catheterization: use of a hydrophilic guidewire. BJU Int. 2004; 93: 883-4.
- Athanassopoulos A, Liatsikos EN, Barbalias GA: The difficult urethral catheterization: use of a hydrophilic guidewire. BJU Int. 2005; 95: 192.
- Mistry S, Goldfarb D, Roth DR: Use of hydrophilic-coated urethral catheters in management of acute urinary retention. Urology. 2007; 70: 25-7.
- Chelladurai AJ, Srirangam SJ, Blades RA: A novel technique to aid urethral catheterisation in patients presenting with acute urinary retention due to urethral stricture disease. Ann R Coll Surg Engl. 2008; 90: 77-8.
- Patel AR, Jones JS, Babineau D: Lidocaine 2% gel versus plain lubricating gel for pain reduction during flexible cystoscopy: a meta-analysis of prospective, randomized, controlled trials. J Urol. 2008; 179: 986-90.
____________________
Accepted after revision:
June 1, 2008
_______________________
Correspondence address:
Dr. Carlos Villanueva
Section of Urologic Surgery
University of Nebraska Medical Center
855, N 82ND Plaza Apt 40
Omaha NE 68114, USA
Fax: + 1 402 990-3634
E-mail: cvillanu@unmc.edu
EDITORIAL COMMENT
In this manuscript, the authors present a review of the literature on the management of difficult male catheterization. Using a limited PubMed search, they retrieved 6 papers on the topic. It is an “information only” type of paper, as it does not provide direct recommendations for clinical practice. However, the various methods proposed are interesting to the reader as well as the creative solutions surgeons have tried in the management of what is a huge problem for both the patient and the care staff.
Dr.
Katherine N. Moore
University of Alberta
Faculty of Nursing
Edmonton, Alberta, Canada
E-mail: katherine.moore@ualberta.ca
EDITORIAL COMMENT
Difficult
male urethral catheterization is still a common problem for the general
urologist. It can be a challenge for different reasons, such as urethral
stricture, benign prostatic hypertrophy or cancer. It must be reminded
that bladder neck contractures and obliterated anastomosis are still present
following transurethral resection of the prostate, supra-pubic prostatectomy
and radical prostatectomy, in spite of all attempts to avoid them. Unfortunately,
the common scenario of “difficult” urethral catheterization
after multiple attempts of non-urological stuff is still a part of our
daily practice. Sometimes these “emergent calls” come from
the emergency or operation room. These circumstances put our young colleagues
in a stressful situation making their task more difficult. That is why
it is particularly important to construct an algorithm for these situations.
A
lot of possible techniques for difficult urethral catheterization have
been described (1-4), however there are still no guidelines for practical
purposes. The authors of this manuscript not only describe these methods,
but also suggest which of them could be use in special situation. They
must be encouraged for this attempt to construct a kind of guidelines
for difficult urethral catheterization. I hope that this manuscript will
be very popular among residents.
REFERENCES
- Chelladurai AJ, Srirangam SJ, Blades RA: A novel technique to aid urethral catheterisation in patients presenting with acute urinary retention due to urethral stricture disease. Ann R Coll Surg Engl. 2008; 90: 77-8.
- Carr LK, Webster GD: Endoscopic management of the obliterated anastomosis following radical prostatectomy. J Urol. 1996; 156: 70-2.
- Chiang DT, Dewan PA, Ben-Meir D: The difficult urethral catheterization: use of a hydrophilic guidewire. BJU Int. 2004; 94: 447-8.
- Lachat ML, Moehrlen U, Bruetsch HP, Vogt PR: The Seldinger technique for difficult transurethral catheterization: a gentle alternative to suprapubic puncture. Br J Surg. 2000; 87: 1729-30.
Dr. Sergey Kravchick
Department of Urology
Barzilai Medical Center
Ashkelon, Israel
E-mail: cambell@netvision.net.il