USE
OF TRADITIONAL CHINESE MEDICINE IN THE MANAGEMENT OF URINARY STONE DISEASE
(
Download pdf )
RICARDO MIYAOKA, MANOJ MONGA
Department of Urologic Surgery, University of Minnesota, Minneapolis, Minnesota, USA
ABSTRACT
Objective:
To assess the evidence-based literature supporting the use of traditional
Chinese medicine Kampo herbal and Acupuncture in stone disease management.
Materials and Methods: Four of the most
commonly used herbal components of Kampo medicine in the treatment of
stone disease are described according to their in vitro and in vivo effects.
We also reviewed the role of Acupuncture in urologic clinical setting
as well as its proposed mechanisms of action and results. Medline database
was assessed using isolated and conjugated key words (Chinese Medicine,
Kampo, Chinese Herbal, Calculi, Stone Disease, Kidney, Acupuncture, Herbal
Medicine). Articles were reviewed and summarized.
Results: Herbal medicine has been proven
to be free from side-effects and therefore suitable for long term use
therapy. Its antilithic beneficial effects include increased urinary volume,
increased magnesium excretion (Takusya), inhibitory activity on calcium
oxalate aggregation (Takusya, Wulingsan and Desmodyum styracyfolium),
inhibition of calcium oxalate nucleation and hydroxyapatite internalization
(Wulingsan). In contrast, acupuncture, has shown to be effective as a
pre-treatment anxiolytic and analgesic during colic pain and extracorporeal
shock wave lithotripsy treatment, reducing the need for complementary
sedative drugs.
Conclusion: Chinese traditional medicine
is promising as regards its role in stone prevention. An effort must be
made in order to standardize study protocols to better assess acupuncture
results since each procedure differs in regards to selected acupoints,
electrostimulation technique and adjunct anesthetics. Similarly, standardization
of Kampo formulations and acceptable clinical endpoints (imaging vs. symptomatic
events) is needed.
Key
words: urolithiasis; medicine, Chinese traditional; medicine,
Kampo; acupuncture
Int Braz J Urol. 2009; 35: 396-405
INTRODUCTION
Urolithiasis
is known to be an affliction to mankind from ancient eras (1) and remains
a major issue regarding health and well being today. Stone disease affects
10 to 12% of the population in industrialized countries with a peak incidence
between 20 and 40 years of age (2) and is associated with a significant
medical expenditure that exceeds 1.5 billion dollars annually in the United
States (3). An additional concern is the high recurrence rate, which is
more than 50% after 10 years (4).
Therefore, great interest has arisen among
both physicians and patients towards identifying effective measures to
achieve analgesia during renal colic, promote stone passage or stone dissolution
and prevent stone recurrence (5). It is of critical importance to consider
treatments that may be complementary to conventional Western therapies
such as Traditional Chinese Medicine (TCM) that have been practiced for
over 3000 years (6).
Historically, TCM makes reference to stone
disease as “stone urinate”. Symptoms of this disease include
stone in urine, painful urination, and lower abdominal pain with radiation
to the umbilical region (7). According to TCM criteria, renal stone diseases
belong to the “sha-lin” (strangury from urolithiasis), “shi-lin”
(strangury caused by urinary calculus) and “xue-lin” (strangury
complicated by hematuria) (8). TCM treatment encompasses the urinary system
and balances the mineral electrolytes as well as the entire endocrine
system including prostaglandins and the various neuro-transmitters (9,10).
It focuses on reestablishing system balance before stone formation instead
of only treating it (6).
We present a literature review of two main
fields of Chinese Medicine in stone disease management: Kampo medicine
and Acupuncture and the currently existing supporting evidence regarding
these types of treatment.
KAMPO MEDICINE
Kampo medicine is a traditional Japanese herbal therapeutic system that
originated in China (Kampo means “medicine from China”). Kampo
medicine formed the basis of Chinese and then Japanese medicine for at
least 10 centuries until it was superseded by Western medicine around
the 1870s (11). The long-term use of Kampo medicine has been reported
to be associated with little or no side effects (12) and therefore seems
suitable for long term stone disease treatment in contrast to some oral
medications which have shown positive effects but in long term use it
is associated with significant drop outs and side effects (13,14).
Theoretically, an effective herbal medicine
for stone disease may inhibit nucleation, growth or aggregation of crystals,
or might help with expulsion of small crystals through an effect on urothelial
adherence or by a diuretic mechanism of action (6).
Kampo medicines are usually a mixture of
two or more kinds of herbs, and studies of individual components are uncommon.
Its use against kidney stone disease has been described in humans and
other animals (15). This review will present the most cited and objectively
investigated substances in literature utilized by this system.
Chorei-to
Chorei-to
consists of a mixture of herbs believed to be beneficial for curing nephritis
and nephrolithiasis (16). Chorei-to extract has had no inhibitory effect
on the formation of amorphous calcium phosphate but did show significant
inhibitory effects on the transformation to hydroxyapatite in vitro (16).
Another in vitro study analyzed separately two Chorei-to components; Takusya
(Alismatis Rhizoma) and Kagosou (Purunellae Spica). Both were proven to
strongly inhibit calcium oxalate crystal growth and aggregation in a synthetic
urine model (11).
In vivo experiments have shown a weaker
effect for Kagosou compared to Takusya. Wistar rats were given 0.5 µg
ethylene glycol 5% daily through a feeding tube for 4 weeks. Takusya was
able to significantly decrease the tissue calcium concentration in the
kidney compared to controls when given in low doses (correspondent to
human daily dosage per unit body weight) and reduce calcium oxalate deposits,
most notably inside the tubular lumen (11).
Takusya was also shown to reduce tissue
calcium oxalate deposits in the kidney of rats treated with stone forming
substances ethylene glycol and vitamin D3 (17). Additionally, it has been
shown to decrease osteopontin (OPN) expression; the secretion of OPN and
its subsequent incorporation into stone matrix may influence the nucleation
and aggregative growth of stones (18).
In vivo results suggested that although
Chorei-to extract reduced urinary citrate concentration (11,16,19,20)
and enhanced calcium excretion (17,19), beneficial changes including increased
urinary volume, increased magnesium excretion (19) and potent inhibitory
activity on aggregation and kidney deposition identified in Takusya lead
to improved supersaturation for calcium oxalate (11). Another in vivo
study, however, did not corroborate a diuretic mechanism of action, but
also showed that Chorei-to does not promote urinary oxalate excretion
as one would expect from tea-like preparations (19,21).
Wullingsan (WLS)
Wullingsan
is a combination of 5 dried herbs: Alisma orientalis (which provides the
Alisma Rhizoma or Takusya, previously mentioned), Polyporus umbellatus,
Poria cocos, and Cinnamomon cassia. Indications for WLS administration
have varied over the centuries, but originally were used for symptoms
of headache, fever, irritability, strong thirst with vomiting immediately
after drinking, urinary difficulty and a “floating pulse”.
Its formula was first mentioned in the TCM book Shang han lun in the third
century (7).
WLS has been reported to be a diuretic,
and to be able to drain dampness, strengthen the spleen, warm the Yin
(“cold nature”) and promote Qi transformation (7,22).
WLS properties were assessed both in vitro
and in vivo by Vietnamese researchers (22). They evaluated the pharmacological
effects of WLS on calcium oxalate nucleation, crystal growth and aggregation.
They reported that WLS extract is capable of inhibiting nucleation by
prolonging the induction time (p < 0.001) in a dose dependent fashion.
WLS also led to inhibition of growth by 28.8% and 16.46% in 3.125 and
6.25 mg/mL respectively, although not statistically significant. At a
higher dose (12.5 mg/mL) it paradoxically promoted the growth of calcium
oxalate (CaOx) crystallization by 371%. WLS significantly inhibited CaOx
aggregation in a dose dependent manner (up to 92.49% at a concentration
of 50 mg/mL WLS extract). In conclusion, WLS extract may inhibit the crystallization
of CaOx by blocking the formation of the crystal nucleus and macrocrystal
agglomeration with a potential to prevent stone formation (22).
WLS was tested by Tsai et al. in a Sprague-Dawley
rat model of ethylene glycol-induced (EG) nephrocalcinosis in both low
and high dosage and compared to placebo. Histologically, EG-fed rats treated
with WLS developed lower crystal deposit scores (p = 0.035) [Tsai]. This
was also observed in another rat model for nephrocalcinosis where animals
were fed with a high phosphorus diet (20). In this study, the individual
components failed to provide the same result when tested alone, suggesting
a synergy by the presence of complementary components in WLS (16).
In addition to the properties of Takusya
discussed in the preceding section, it has been suggested that WLS decreases
the concentration of PO4 ions in the fluid in the tubules and inhibits
the internalization of hydroxyapatite into the cells (7,20).
Jin Qian Cao (Desmodium styracifolium Merr)
This
herb is believed to act as a diuretic, to promote urine acidification,
reduce “heat” and swelling (6). Its extract has been demonstrated
in vitro to inhibit crystal growth and aggregation, though it did promote
nucleation of crystals. No dissolution of pure monohydrate calcium oxalate
crystal mass was observed (6).
Hirayama et al. studied the anti-lithogenic
properties of the main component of Desmodium, which is called Desmodium
styracyfolium-triterpenoide (Ds-t) in rats. They used an ethylene glycol
and 1-alpha(OH)D3 induced oxalate stone animal model. Ds-t fed group demonstrated
significantly lower Calcium/Creatinine and Phosphorus/Cr excretion after
3 weeks when compared to control (p < 0.05). Citrate/Cr excretion was
increased (p < 0.05) and so was the 24-hours creatinine clearance (p
< 0.01). No change in pH was noted. A 52% in stone burden was observed
in Ds-t fed rats compared to control group animals. This data suggests
that Ds-t reduces stone formation of pure Ca oxalate crystals in the rat
kidney (23).
Ds-t is believed to block urinary calcium
excretion by either inhibiting the endogenous synthesis of 1-25(OH)2D
from 1-alphaD3 in the kidney or by inhibiting the action of 1-25(OH)2D
on increased intestinal absorption of Ca. Higher serum calcium levels
in Ds-t group also suggests Ca reabsorption in the renal tubules but further
studies are needed to clarify this mechanism (23).
Niao Shi Mixture (NSM)
NSM is a mixture of several different herbs: Squama Manitis, Spina Gleditsiae,
Resina Olibani, Resina Myrrhae, Radix Achyranthis Bidentatae, Radix Angelicae
Dahuricae, Pericarpium Citri Reticulatae Viride, Semen Coicis, Cortex
Magnoliae Officinalis, Fructus Aurantii, Semen Persicae, Rhizoma Sparganii,
Rhizoma Zedoariae, Semen Plantaginis, Radix Paeoniae Rubra and Herba Lysimachiae
(24).
For more than 30 years, NSM has been used
clinically at Guanganmen Hospital (Beijing, China) to treat urinary calculus
disease (24). NSM effects were assessed in four experimental animal models
of hyperoxaluric urolithiasis (4-hydroxy-L-proline (HyP), glycoxylic acid,
oxalic acid and sodium oxalate). It was quite effective in preventing
HyP-induced stones, but had no influence on the other animal models, suggesting
its blocking effect to occur prior to the metabolism of HyP glyoxylic
acid. NSM was also demonstrated to decrease serum calcium and urinary
acid urate although this decrease was not statistically significant (24).
In summary, though in vitro and animal
studies suggest a potential therapeutic effect for herbal approaches to
stone disease, clinical trials are lacking and as such, claims of effectiveness
in humans remains unsubstantiated (Table-1).

ACUPUNCTURE
Historical Considerations
Acupuncture is an ancient traditional Chinese method of medical treatment
involving the insertion of fine single-use sterile needles in determined
points of the body according to a system of channels and meridians developed
by early practitioners of TCM over 2000 years ago (25). Needles can be
stimulated by manual manipulation, electrical stimulation or heat (26).
Approximately 1 million patients visited an acupuncture professional in
the United States in 1994 (27).
Its use has been focused on the management
of acute and chronic neuromuscular pain, anesthesia for minor operation
and pain control in malignant disease (28). It has been proposed as an
alternative and effective analgesic with few side effects (29), rapid
recovery to work (30) and rare complications (31-34).
Acupuncture inclusion along with other
Complementary and Alternative Medicine (CAM) has been increasing in Urology.
Many groups such as the Committee of Complementary and Alternative Medicine
within the American Urological Association (AUA) recognize the integration
of non-conventional therapies into urological clinical practice. Additionally,
both public demand for CAM therapies and their testing and validation
under modern scientific research patterns methodology has increased (35,36).
In the literature, acupuncture has been described to aid in the management
of chronic prostatitis, chronic pelvic pain as well as nocturnal enuresis
(29,36-38).
In stone disease field, acupuncture has been used for treating renal colic
(28) and for extracorporeal shock wave lithotripsy (SWL) - related pain
and anxiety (30,37,39-42).
Supporting Objective Evidence
Lee
et al. conducted a prospective randomized study to compare the effect
of acupuncture and intramuscular analgesic AvafortanTM (Asta-Werke Degussa
PharmaGruppe, West Germany) in the treatment of renal colic. Acupuncture
was applied in 4 to 6 points in the hand (loin and leg, EX-UE 7) or on
the back (points UB-21 through UB-25, UB-45 through UB-47 or Yao-Yen EX-B7)
according to the main site of pain and electrically stimulated (3 Hz)
in more than half of the cases (68.2%). No statistically significant difference
was noted regarding pain scores. Onset of analgesic effect occurred more
rapidly in acupuncture patients than for AvafortanTM (3.1 ± 2.9
vs. 15.4 ± 7.6 minutes; p < 0.05). Acupuncture had no reported
side effects. Forty-three percent of patients in AvafortanTM group reported
minor side effects, such as skin rash, drowsiness, tachycardia and facial
flush. Neither treatment had any immediate effect on stone location. The
authors emphasized that acupuncture may be particularly helpful in some
selected situations such as drug allergy or fear of drug addiction, or
pregnancy (28).
Mora et al. evaluated the use of auricular
acupressure as a treatment for anxiety in elderly individuals who are
transported by ambulance before receiving SWL in an Italian medical facility.
One hundred patients were prospectively enrolled in a randomized, double-blind
sham-controlled study. A self-assessment Visual Analog Scale (VAS) was
completed before and after intervention and rated the level of anxiety
experienced by each individual. Auricular acupressure (AA) was administered
with a plastic ball 1 mm in diameter, which was pressed on the relaxation
point and fixed with an ear patch. This point is located at the superior
lateral wall of the triangular fossa [41]. The sham group received AA
at a sham point with no relaxing or anxiolytic effect in acupuncture (39).
Individuals who received acupressure at the relaxation point had significantly
decreased anxiety and pain scores and were also more optimistic towards
their treatment upon arrival at the hospital than individuals who underwent
sham intervention (p = 0.001). Therefore, acupressure proved to be a useful
measure for decreasing anxiety in the pre-interventional urological setting.
The authors proposed that minimal equipment and training is required,
making it a technique applicable to any physician, nurse, paramedic or
medical technician (40).
Similarly, Wang et al. conducted a double-blind
randomized sham-controlled study to evaluate acupuncture use as an adjunct
for the preprocedural anxiety and pain management in 48 patients undergoing
lithotripsy procedures. Patients completed a baseline State-Trait Anxiety
Inventory (STAI), which is a 40-item self-report measure of anxiety status.
An experienced acupuncturist performed auricular acupuncture intervention
ipsilateral to patient’s dominant hand at the Relaxation, Master
Cerebral, and Valium points of the Ear and patients in the sham group
received auricular acupuncture at the wrist, shoulder, and extra-auricular
sham points of the ear. Thirty minutes after initiation of the acupuncture
procedure, all patients completed a second STAI. Patients were then sent
to SWL procedure, before which they received a pre-anesthetic cocktail
containing midazolam, alfentanil and metoclopramide. During the procedure,
they could also self-administer alfentanil through a patient-controlled
analgesia (PCA) pump as needed.
During the SWL treatment, the Acupuncture
group received body acupuncture at bilateral Liver 3 and Large Intestine
4 points. Liver 3 is located on the dorsum of the foot in the depression
distal to the junctions of the first and second metatarsals, and Large
Intestinal 4 is located on the radial side of the middle of the second
metacarpal (38). Needles were electrically stimulated under 2 Hz and 25
V. Sham group received only a very superficial insertion (1-2 mm deep).
Standardized SWL procedure was carried out, using 2500 shocks for renal
calculi and 3000 shocks for ureteral calculi.
Alfentanil consumption was significantly
lower in Acupuncture Group (p = 0.040). Pain scores assessed by VAS and
at discharge (assessed by short-form McGill questionnaires) (43) were
also significantly lower (p = 0.014 and 0.047 respectively). The authors
concluded that a combination of auricular and body acupuncture decrease
preprocedural anxiety and intraprocedural alfentanil requirements during
lithotripsy (38).
Rogenhofer et al. also evaluated the role of acupuncture for pain control
during SWL. Their non-randomized study prospectively enrolled 90 patients
with a median age of 51.7 years. They received acupuncture immediately
prior to ESWL treatment. Needles were inserted 1 to 2 cm deep until the
“De Qi”, a feeling of numbness and tingling within the range
of the acupoint, was achieved. Acupoints comprised a total of 9 traditional
points generally considered either for analgesia, especially of the lower
back (Large Intestine 4, Governing Vessel 20, Urinary Bladder 23, Urinary
Bladder 52, Kidney 3) or for anxiety related disorders (Spleen 6). Additional
analgesic medication was given as needed to address break-through pain
(piritramide and midazolam). ESWL was performed using a Siemens Lithostar
lithotripter, (Erlanger, Germany) in a standardized fashion (renal stones
and stones in proximal ureter received 4000 shocks at a maximum of 18.2
kV; middle and distal ureteral stones received 5000 impulses of up to
21kV). Ninety-three percent of patients expressed willingness to undergo
any necessary repeated ESWL under acupuncture analgesia; and 87.5% considered
their pain control to be good or very good. Average pain intensity reported
was similar to the ones described for drug combination (1.5 to 2.5 on
a 10- point VAS) (41).
In small case series, Quatan et al. also
reported success in treating three SWL patients with acupuncture, who
had not tolerated conventional analgesic medications (acetaminophen, piroxicam,
midazolam, pethidine). Acupuncture was performed half an hour prior to
commencing ESWL and needles underwent electrical stimulation using a pulse
generator set to 4 Hz. Acupoints were CV4, ST25, BL23 and BL25 (37). They
reported satisfactory analgesia and no side effects concluding that acupuncture
should be offered to people who would not otherwise be suitable for outpatient
SWL services or those who request it (37).
Finally, Karamarz et al. performed a prospective,
randomized, sham-controlled study to evaluate the efficacy of transcutaneous
electrical nerve stimulation (TENS) versus conventional-like acupuncture
as an adjunct for analgesia in patients undergoing SWL treatment. Each
group comprised 22 patients. A 2Hz stimulation frequency was used in acupuncture
and control groups with a difference in shock intensity above 15mA and
below 10mA, respectively. Eighty hertz were used in TENS group. Shockwave
energy was estimated by an index described by Schelling et al., which
considers both voltage and number of shocks (44). During the operation,
patients were oriented to utilize the PCA button whenever the VAS >
3. VAS pain scores and alfentanil consumption were lower in TENS group
comparing to the other two groups (p < 0.001 and p < 0.05). The
authors suggest conventional TENS use during ESWL to shorten recovery
time and reduce alfentanil consumption and side-effects (42).
Resim et al. performed a similar prospective,
randomized study of 35 patients, comparing electroacupuncture (EA) to
conventional anesthetic agents during SWL. Midazolam (1.5 mg/Kg) and tramadol
(0.06mg/Kg) were used for sedation and analgesia versus electroacupuncture
delivered to urinary bladder points 20,21,22,23 and 52. Needles were stimulated
manually until the patient felt the sensation as Qi numbness in that region.
Electrical stimulation with 2-4 Hz frequency with an intensity up to the
tolerance level of each patient was given. Achieved energy levels were
statistically comparable between the two groups, although SWL protocols
were not standardized. VAS scores were consistently lower in the EA group,
but with no statistical significance (p = 0.245). No difference in stone-free
rates was found either. Both treatment regimens offered satisfactory sedation
and analgesia and allowed the maximum number shockwaves to be given. No
side effects were seen in any patients who received EA treatment. Therefore,
EA was proven to be an effective alternative to other forms of anesthesia
and analgesia during SWL procedures (30).
Mechanisms of Action
Acupuncture
is believed to stimulate humoral factors and neurological pathways through
a specific point with a needle or with pressure which activates small
myelinated nerve fibers that send impulses into the spinal cord, mid brain,
pituitary gland and hypothalamus (45), causing a measurable amount of
endorphins to be released into the blood (46). Furthermore, various neurotransmitters
such as serotonin, norepinephrine and possibly gamma-amynobutyric acid
are known to interrupt incoming stress signals in the central nervous
system.
Several studies have confirmed the ability
of acupuncture to induce opiate-like peptides (beta-endorphin, dynorphin
and met-enkephalin) in the cerebrospinal fluid and to provide pain relief
(28). The humoral mechanism can be inhibited by naloxone (47).
Neural pathways can be addressed through
segmental and nonsegmental routes. Segmental acupuncture analgesia is
produced by short circuits and non segmental acupuncture analgesia is
produced by afferent signals that synapse on spinal interneurons and then
project to higher brain centers through the anterolateral tract (48,49).
The addition of electrical stimulation
during acupuncture induces endorphin release that generates a more potent
effect on the concentration of neuropeptides in the animal hippocampus
and occipital cortex than manual acupuncture (50) which can be noted as
an enhancement in signal magnitude in MRI imaging. An autonomic response
also occurs as evidenced by significant reduction in average heart rate
during treatment (51). Some studies also suggest that acupuncture treatment
can decrease inflammation and relieve pain (52,53).
Locally, intramuscular movements of the
needle cause insertional activity, or depolarization of innervated single
or grouped muscle fibers. These are micro-twitches that produce micro-stretch
effects on the muscle fibers nearby, thus reducing the local pressure
on pain-sensitive structures such as intramuscular nerves and blood vessels
(54).
The effect of acupuncture as analgesia
depends also on the placebo effect and suggestion effect (“physician
as a drug”) that takes place in every treatment and medication (41).
CONCLUSION
Chinese
Traditional Medicine holds promise for its role in stone prevention through
the use of Kampo herbal compound, though no evidence of dissolution properties
exist. Acupuncture has been demonstrated to be an effective adjunct in
stone disease treatment both as an analgesic during renal colic or SWL
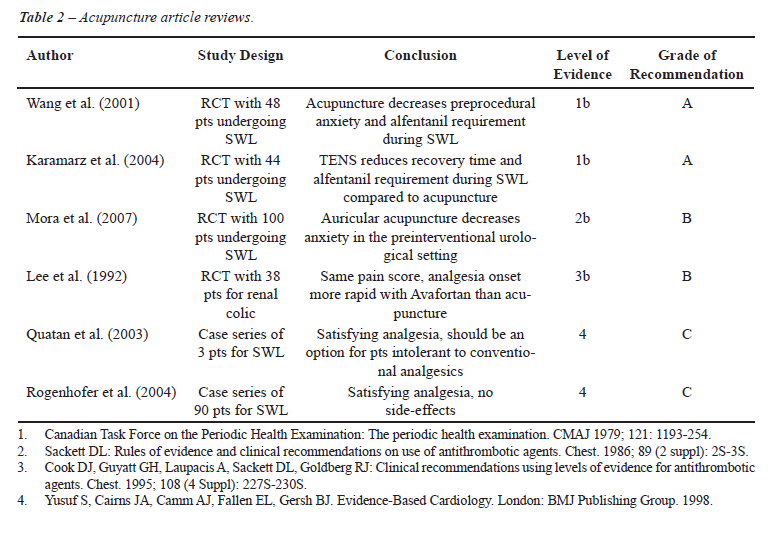
therapy and for reducing pre-treatment anxiety (Table-2).
An effort must be made in order to standardize
study protocols to better assess acupuncture results since each one differs
in regards to selected acupoints, electrostimulation technique and adjunct
anesthetics. Similarly, standardization of Kampo formulations and acceptable
clinical endpoints (imaging vs. symptomatic events) are needed.
CONFLICT OF INTEREST
Dr. Ricardo Miyaoka is corporate sponsored endourology Fellow with Gyrus ACMI / Olympus.
REFERENCES
- Cledeling, L: Source Book of Medical History. New York, Dove Publications. 1942; pp. 14-8.
- Pak CYC: Citrate and renal calculi. Miner Electrol Metab. 1987; 13: 257-66.
- Schwartz BF, Schenkman N, Nguyen R, Stoller ML: Gahat: a Napalese cure for urolithiasis? Urology. 2000; 56: 912-4.
- Wasserstein AG: Nephrolithiasis: acute management and prevention. Dis Mon. 1998; 44: 196-213.
- Kieley S, Dwivedi R, Monga M: Ayurvedic medicine and renal calculi. J Endourol. 2008; 22: 1613-6.
- Gohel MD, Wong SP: Chinese herbal medicines and their efficacy in treating renal stones. Urol Res. 2006; 34: 365-72.
- Tsai CH, Chen YC, Chen LD, Pan TC, Ho CY, Lai MT, et al.: A traditional Chinese herbal antilithic formula, Wulingsan, effectively prevents the renal deposition of calcium oxalate crystal in ethylene glycol-fed rats. Urol Res. 2008; 36: 17-24.
- The Traditional Chinese Medicine (TCM) [Internet]. [cited 4 Sept 2006] Available from: http://www.tcmtreatment.com
- Zhao Z: An illustrated Chinese Materia Medica in Hong Kong School of Chinese Medicine, Hong Kong Baptist University, Hong Kong. 2004.
- Chen JK, Chen TT: Chinese Medical Herbology and Pharmacology. The Art of Medicine. California, Press Inc. 2004.
- Koide T, Yamaguchi S, Utsunomiya M, Yoshioka T, Sugiyama K: The inhibitory effect of kampou extracts on in vitro calcium oxalate crystallization and in vivo stone formation in an animal model. Int J Urol. 1995; 2: 81-6.
- Product Catalogue. Tsumura Kampo Medicine Extract Granules for Ethical Use. Tokyo, Tsumura Co. Ltd. 1990.
- Gürocak S, Küpeli B: Consumption of historical and current phytotherapeutic agents for urolithiasis: a critical review. J Urol. 2006; 176: 450-5.
- Coe FL, Evan A, Worcester E: Kidney stone disease. J Clin Invest. 2005; 115: 2598-608.
- Sugimoto K, Sakurai N, Shirasawa H, Fujise Y, Shibata K, Shimoda K, et al.: Bovine cases of urolithiasis treated with traditional herbal medicine, P-3. J Vet Med Sci. 1992; 54: 579-82.
- Hidaka S, Abe K, Liu SY: A new method for the study of the formation and transformation of calcium phosphate precipitates: effects of several chemical agents and Chinese folk medicines. Arch Oral Biol. 1991; 36: 49-54.
- Yasui T, Fujita K, Sato M, Sugimoto M, Iguchi M, Nomura S, et al.: The effect of takusha, a kampo medicine, on renal stone formation and osteopontin expression in a rat urolithiasis model. Urol Res. 1999; 27: 194-9.
- McKee MD, Nanci A, Khan SR: Ultrastructural immunodetection of osteopontin and osteocalcin as major matrix components of renal calculi. J Bone Miner Res. 1995; 10: 1913-29.
- Ogawa Y, Takahashi S, Kitagawa R: Effect of herb medicines for urolithiasis on urinary oxalate excretion in rats. Hinyokika Kiyo. 1983; 29: 1269-71.
- Liu QL, Sato S, Kishikawa T, Matsuzaki H, Yamanaka N: Effectiveness of a traditional Chinese medicine, Wulingsan, in suppressing the development of nephrocalcinosis induced by a high phosphorus diet in young rats. Med Electron Microsc. 2001; 34: 103-14.
- McKay DW, Seviour JP, Comerford A, Vasdev S, Massey LK: Herbal tea: an alternative to regular tea for those who form calcium oxalate stones. J Am Diet Assoc. 1995; 95: 360-1.
- Chen YC, Ho CY, Chen LD, Hsu SF, Chen WC: Wu-Ling-San formula inhibits the crystallization of calcium oxalate in vitro. Am J Chin Med. 2007; 35: 533-41.
- Hirayama H, Wang Z, Nishi K, Ogawa A, Ishimatu T, Ueda S, et al.: Effect of Desmodium styracifolium-triterpenoid on calcium oxalate renal stones. Br J Urol. 1993; 71: 143-7.
- Xue JZ: A preliminary laboratory investigation of “niao shi mixture” in preventing experimental calcium oxalate renal calculus in rats. J Tradit Chin Med. 1982; 2: 187-94.
- Capodice JL, Bemis DL, Buttyan R, Kaplan SA, Katz AE: Complementary and alternative medicine for chronic prostatitis/chronic pelvic pain syndrome. Evid Based Complement Alternat Med. 2005; 2: 495-501.
- Ellis A, Wiseman N, Boss K: Fundamentals of Chinese Acupuncture Brookline. Massachusetts, Paradigm Publications. 1991.
- Paramore LC: Use of alternative therapies: estimates from the 1994 Robert Wood Johnson Foundation National Access to Care Survey. J Pain Symptom Manage. 1997; 13: 83-9.
- Lee YH, Lee WC, Chen MT, Huang JK, Chung C, Chang LS: Acupuncture in the treatment of renal colic. J Urol. 1992; 147: 16-8.
- Chen R, Nickel JC: Acupuncture ameliorates symptoms in men with chronic prostatitis/chronic pelvic pain syndrome. Urology. 2003; 61: 1156-9; discussion 1159.
- Resim S, Gumusalan Y, Ekerbicer HC, Sahin MA, Sahinkanat T: Effectiveness of electro-acupuncture compared to sedo-analgesics in relieving pain during shockwave lithotripsy. Urol Res. 2005; 33: 285-90.
- Matsuyama H, Nagao K, Yamakawa GI, Akahoshi K, Naito K: Retroperitoneal hematoma due to rupture of a pseudoaneurysm caused by acupuncture therapy. J Urol. 1998; 159: 2087-8.
- Fujiwara T, Tanohata K, Nagase M: Pseudoaneurysm caused by acupuncture: a rare complication. AJR Am J Roentgenol. 1994; 162: 731.
- Halvorsen TB, Anda SS, Naess AB, Levang OW: Fatal cardiac tamponade after acupuncture through congenital sternal foramen. Lancet. 1995; 345: 1175.
- Carron H, Epstein BS, Grand B: Complications of acupuncture. JAMA. 1974; 228: 1552-4.
- Hirsch IH: Integrative urology: a spectrum of complementary and alternative therapy. Urology. 2000; 56: 185-9.
- Capodice JL, Jin Z, Bemis DL, Samadi D, Stone BA, Kapan S, et al.: A pilot study on acupuncture for lower urinary tract symptoms related to chronic prostatitis/chronic pelvic pain. Chin Med. 2007; 2: 1.
- Quatan N, Bailey C, Larking A, Boyd PJ, Watkin N: Sticks and stones: use of acupuncture in extracorporeal shockwave lithotripsy. J Endourol. 2003; 17: 867-70.
- Wang SM, Kain ZN: Auricular acupuncture: a potential treatment for anxiety. Anesth Analg. 2001; 92: 548-53.
- Wang SM, Punjala M, Weiss D, Anderson K, Kain ZN: Acupuncture as an adjunct for sedation during lithotripsy. J Altern Complement Med. 2007; 13: 241-6.
- Mora B, Iannuzzi M, Lang T, Steinlechner B, Barker R, Dobrovits M, et al.: Auricular acupressure as a treatment for anxiety before extracorporeal shock wave lithotripsy in the elderly. J Urol. 2007; 178: 160-4; discussion 164.
- Rogenhofer S, Wimmer K, Blana A, Roessler W, Wieland WF, Filbeck T: Acupuncture for pain in extracorporeal shockwave lithotripsy. J Endourol. 2004; 18: 634-7.
- Kararmaz A, Kaya S, Karaman H, Turhanoglu S: Effect of the frequency of transcutaneous electrical nerve stimulation on analgesia during extracorporeal shock wave lithotripsy. Urol Res. 2004; 32: 411-5.
- Melzack R: The short-form McGill Pain Questionnaire. Pain. 1987; 30: 191-7.
- Schelling G, Mendl G, Weber W, Pauletzki J, Sackmann M, Pöppel E, et al.: Patient controlled analgesia for extracorporeal shock wave lithotripsy of gallstones. Pain. 1992; 48: 355-9.
- Hui KK, Liu J, Makris N, Gollub RL, Chen AJ, Moore CI, et al.: Acupuncture modulates the limbic system and subcortical gray structures of the human brain: evidence from fMRI studies in normal subjects. Hum Brain Mapp. 2000; 9: 13-25.
- Levine JD, Gormley J, Fields HL: Observations on the analgesic effects of needle puncture (acupuncture). Pain. 1976; 2: 149-59.
- Mayer DJ, Price DD, Rafii A: Antagonism of acupuncture analgesia in man by the narcotic antagonist naloxone. Brain Res. 1977; 121: 368-72.
- Klarskov P: Enkephalin inhibits presynaptically the contractility of urinary tract smooth muscle. Br J Urol. 1987; 59: 31-5.
- Pomeranz B: Neural mechanisms of acupuncture analgesia. In: Persistent Pain (ed.), Moderrn Methods of Treatment. New York, Lipton and J. Miles. Academic Press. 1981; pp. 241-52.
- Bucinskaite V, Lundeberg T, Stenfors C, Ekblom A, Dahlin L, Theodorsson E: Effects of electro-acupuncture and physical exercise on regional concentrations of neuropeptides in rat brain. Brain Res. 1994; 666: 128-32.
- Wu MT, Hsieh JC, Xiong J, Yang CF, Pan HB, Chen YC, et al.: Central nervous pathway for acupuncture stimulation: localization of processing with functional MR imaging of the brain--preliminary experience. Radiology. 1999; 212: 133-41.
- Watkin H: Back pain--an integrated approach in primary care. Acupunct Med. 2004; 22: 203-6.
- Sekido R, Ishimaru K, Sakita M: Differences of electroacupuncture-induced analgesic effect in normal and inflammatory conditions in rats. Am J Chin Med. 2003; 31: 955-65.
- Chu J: The local mechanism of acupuncture. Zhonghua Yi Xue Za Zhi (Taipei). 2002; 65: 299-302.
____________________
Accepted
after revision:
April 6, 2009
_______________________
Correspondence
address:
Dr. Ricardo Miyaoka
Department of Urologic Surgery
University of Minnesota
1420 Delaware St. SE (MMC 394)
Minneapolis MN 55455, USA
Fax: + 1 612 626-0428
E-mail: miyao002@umn.edu
EDITORIAL COMMENT
Dietary
measures and pharmacologic therapy constitute the mainstay of stone metaphylactic
programs. Despite proven efficacy in preventing stone recurrence, however,
compliance with drug and dietary therapy historically remains poor because
of cost, side effects, inconvenience and lifestyle changes necessitated
by incorporating these regimens. An effective, low cost, well-tolerated
alternative therapy might improve compliance and reduce the morbidity
of stone recurrence. Herbal medicines, particularly traditional Chinese
medicines, have been promoted as potential alternatives to established
treatments in preventing stone formation. Miyaoka and Monga offer a comprehensive
and balanced review of published scientific studies that address the effectiveness
of traditional Chinese medicines in reducing stone-forming potential.
While some of these agents have demonstrated promising effects in vitro
or in stone-producing animal models with regard to inhibiting specific
steps in the crystallization or stone forming process, no clinical trials
support the benefit of these medicines in reducing actual stone recurrence,
and further study is necessary before they can be widely recommended.
Like medical therapy for stone prevention,
effective treatments to alleviate the pain of renal colic and the discomfort
of shock wave lithotripsy are also readily available with narcotic analgesics
and non-steroidal anti-inflammatory agents. However, these medications
too are associated with side effects, such as nausea, constipation, gastrointestinal
effects and cognitive dysfunction that in some cases counterbalance the
benefit of pain control. Some alternative therapies, such as acupuncture
and transcutaneous electrical nerve stimulation reviewed here, have been
subjected to randomized, controlled trials that have confirmed their effectiveness
in alleviating renal pain. While these treatments have not become mainstream,
primarily due to lack of experience or exposure for most physicians, it
behooves practitioners to keep an open mind and consider these measures
as options, perhaps at least in patients not effectively treated with
traditional measures.
Dr.
Margaret S. Pearle
Department of Urology
University of Texas
Southwestern Medical Center
Dallas, Texas, USA
E-mail: margaret.pearle@utsouthwestern.edu