PENETRATING
URETERAL TRAUMA
(
Download pdf )
GUSTAVO P. FRAGA, GUSTAVO M. BORGES, MARIO MANTOVANI, UBIRAJARA FERREIRA, TIAGO L. LAURITO, NELSON R. NETTO JR
Division of Trauma Surgery, School of Medicine, State University of Campinas, Unicamp, Campinas, Sao Paulo, Brazil
ABSTRACT
Objective:
The purpose of this series is to report our experience in managing ureteral
trauma, focusing on the importance of early diagnosis, correct treatment,
and the impact of associated injuries on the management and morbid-mortality.
Materials and Methods: From January 1994
to December 2002, 1487 laparotomies for abdominal trauma were performed
and 20 patients with ureteral lesions were identified, all of them secondary
to penetrating injury. Medical charts were analyzed as well as information
about trauma mechanisms, diagnostic routine, treatment and outcome.
Results: All patients were men. Mean age
was 27 years. The mechanisms of injury were gunshot wounds in 18 cases
(90%) and stab wounds in two (10%). All penetrating abdominal injuries
had primary indication of laparotomy, and neither excretory urography
nor computed tomography were used in any case before surgery. The diagnosis
of ureteric injury was made intra-operatively in 17 cases (85%). Two ureteral
injuries (10%) were initially missed. All patients had associated injuries.
The treatment was dictated by the location, extension and time necessary
to identify the injury. The overall incidence of complications was 55%.
The presence of shock on admission, delayed diagnosis, Abdominal Trauma
Index > 25, Injury Severity Score > 25 and colon injuries were associated
to a high complication rate, however, there was no statistically significant
difference. There were no mortalities in this group.
Conclusions: A high index of suspicion is
required for diagnosis of ureteral injuries. A thorough exploration of
all retroperitoneal hematoma after penetrating trauma should be an accurate
method of diagnosis; even though it failed in 10% of our cases.
Key
words: ureter; wounds and injuries; reconstructive surgical procedures
Int Braz J Urol. 2007; 33: 142-50
INTRODUCTION
Ureteral
lesions occur as a consequence of external trauma, open surgical procedures,
laparoscopy or ureteroscopic procedures. Lesions caused by external trauma
are rare. Iatrogenic damage is the most frequent cause of ureteral injury.
In one review of 13 series, hysterectomy was responsible for the majority
(54%), followed by colorectal surgery (14%), pelvic surgery (8%) and abdominal
vascular surgery (6%) (1). Ureteral injury occurs only in 2% to 5% of
the victims of abdominal gunshot wounds (2-6).
Ureteral injury is usually silent, producing
no early signs or symptoms. Hematuria is typically absent on presentation,
as described in several series, and urinalysis is normal at hospital admission
in 15 to 55% of patients with ureteral injury (3,4,6).
Visceral injuries are commonly associated
to ureteral injury and are easily identified in most cases. Patients with
hemodynamic instability and extensive blood loss are more susceptible
to have ureteral lesions not identified at surgical exploration (3,7,8).
Once diagnosed, ureteral lesion must be
primarily treated. Termino-terminal anastomosis (ureteroureterostomy),
debridment and direct repair of minor lesions and ureteral reimplantation
are treatment options for almost all ureteral lesions (3,9,10). Transureteroureterostomy,
ileum interposition and auto-transplantation are performed in extreme
cases of extended ureteral loss. Patients with shock at admission, massive
intraoperative blood loss, associated lesions and local contamination
have high morbidity rates and primary repair of ureteral injury in these
cases have been questioned.
The purpose of this series is to report
our experience in ureteral trauma management, with attention to the diagnosis,
repair, and outcome of these injuries.
MATERIALS AND METHODS
The
trauma surgery division is responsible for traumatic and non-traumatic
surgical emergencies in a metropolitan region consisting of 2.4 million
people. From January 1994 to December 2002, 1487 laparotomies for abdominal
trauma were performed. Penetrating trauma was responsible for 69.1% of
the operation and blunt trauma for 30.9%. The sequence of diagnostic and
therapeutic procedures adopted was in agreement with standards established
by the Advanced Life Trauma Support (ATLS). Indications for laparotomy
in patients sustained penetrating trauma were based in mechanism of trauma,
physical examination, and the patient’s response to initial fluid
resuscitation. All patients with gunshot wounds penetrating the peritoneal
cavity or retroperitoneum, and all patients with stab wounds penetrating
the anterior peritoneum with hypotension, peritonitis, or evisceration
underwent laparotomy, without any further investigation including computed
tomography (CT) scan or intravenous urography (IVU).
In this period, 20 patients with ureteral
lesions were identified, all of them secondary to penetrating injury.
Surgical repair of these lesions was performed in consultation with the
division of urology of our institution.
Data of all patients were analyzed in Epi-Info
6.04 computer program. In all cases, gender, age, mechanism of injury,
investigation, site and grade of lesion, repair, complications and follow-up
were analyzed. Physiologic condition was evaluated by Revised Trauma Score
(RTS) (11), associated lesions by Abdominal Trauma Index (ATI) (12) and
Injury Severity Score (ISS) (13), and mortality by TRISS (14). Ureteral
lesions were classified according to the Organ Injury Scaling (OIS) (15)
classification described in Table-1.

All repairs included adequate debridement
of ureteral margins, spatulation, suture using a 4 or 5 zero absorbable
sutures, drain, bladder catheter drainage and antibiotic prophylaxis.
The data were analyzed using nonparametric
statistical methods. The principal test used was the chi-squared using
the Yates correction for 2 by 2 contingency tables. A significance level
of p < 0.05 was used for all tests.
RESULTS
Ureteral
lesions were identified in 1.3% considering all laparotomies and 1.9%
in laparotomies for penetrating trauma.
All 20 patients included in this report
were men. Age ranged from 17 to 48 years, with an average of 27 years.
The mechanisms of injury were gunshot wounds in 18 cases (90%) and stab
wounds in two (10%).
At admission, 15 patients (75%) were hemodynamically
stable and five patients (25%) had systolic blood pressure less than 90
mmHg. The mean Revised Trauma Score (RTS) was 7.54 (range 5.22 to 7.84).
Gross hematuria was observed in two patients (associated with a renal
and a bladder injury, respectively) and urinalysis was performed at admission
only in six of the 20 patients, with microscopic hematuria in one case
(16.7%).
Since the patients had a clear indication
for surgery, no IVU or CT scan was done preoperatively. The diagnosis
of ureteric injury was made intraoperatively in 18 cases (90%). Two ureteral
injuries (10%) were initially missed, with late diagnosis made at days
8 and 12 after the first surgical procedure. One patient had urinary leakage
by abdominal drain and another presented with urinoma. Retrograde pyelogram
was performed in these cases, both of them showing contrast extravasation
from ureter.
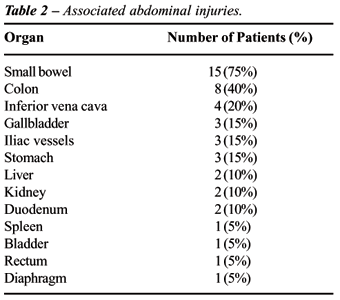
All patients had other associated injuries
(Table-2), with a mean Abdominal Trauma Index (ATI) of 25 (range 10-64).
The Injury Severity Score (ISS) ranged from 9 to 29, with an average of
14.
The left ureter was involved in 13 patients
(65%) and the right in 7 (35%). There were no bilateral lesions.
Three ureteric injuries (15%) were proximal
1/3, 10 (50%) to middle 1/3 and 7 (35%) to the distal 1/3. Two patients
had only contusion to the ureter (grade I lesion), secondary to the blast
effect of high velocity missile passing in close proximity to the ureteric
wall. There were 9 partial lesions (grade II injury in 5 and grade III
in 4 patients) and 9 cases complete transections (grade IV injury in 2
and grade V in 7 patients).
The treatment was determined by the location,
extent and time of diagnosis (Table-3). No intervention were done for
patients with grade I lesions and one of them developed a urinary fistula
at the 6th postoperative day. Since no disruption of the ureter was identified
at the time of laparotomy, the ureter wall necrosed at the site of blast
effect developing urinary fistula.

All 9 patients with middle 1/3 injuries
were repaired by ureteroureterostomy with double J stent. Of the 4 patients
with distal 1/3 injury diagnosed during the operation, one underwent stented
(double J) ureteroureterostomy and 3 ureteroneocystotomy (psoas hitch
in one case and Politano-Leadbetter reimplantation in 2 cases - all stented
with a 8F polyvinyl feeding tube for 8 weeks). The 3 proximal lesions
were all identified during surgery. Two were treated with ureteroureterostomy
and stent, and one caused by stab wound was repaired primarily and stented
for 8 weeks.
The two patients with missed ureteral injuries
underwent endoscopic treatment with double J stent. The patient with delayed
grade I injury and urinary fistula was treated with endoscopic DJ stent.
Stents remained in place for a mean of 43 days (ranged from 29 to 90).
The overall incidence of complications was
55% (11 cases). There were 2 cases of persistent urinary fistula. One
patient had suffered multiple injuries (ATI: 40), including inferior vena
cava, and sustained prolonged hypotension. He was treated with ureteroureterostomy
and DJ stent, and developed a urinary fistula treated conservatively with
sustained ureteral catheterization. The patient was discharged from hospital
on day 19 and the catheter was removed in 90 days. The second, treated
with ureteral reimplantation, was diagnosed with colorectal and small
bowel injuries (ATI: 31), and moderate peritoneal contamination. He developed
a ureteric-colonic fistula, with extravasation of urine by colostomy.
He was treated with ureteral stenting and the fistula closed with two
weeks. The patient was discharged from hospital on the 14th postoperative
day, but the DJ stent was removed only with 87 days.
Other complications related to the genitourinary
tract included two cases of urinary tract infection and a case of persistent
hematuria (until 8th postoperative day). Complications unrelated to urinary
repair included pneumonia in 2 cases, neurological sequelae in 2 cases
and a wound abscess in one patient.
In this study, a delay in diagnosis was
a contributory factor in morbidity related to ureteral injury, because
two patients with missed lesions had prolonged hospitalization (34 and
20 days, respectively), and the first had pneumonia.
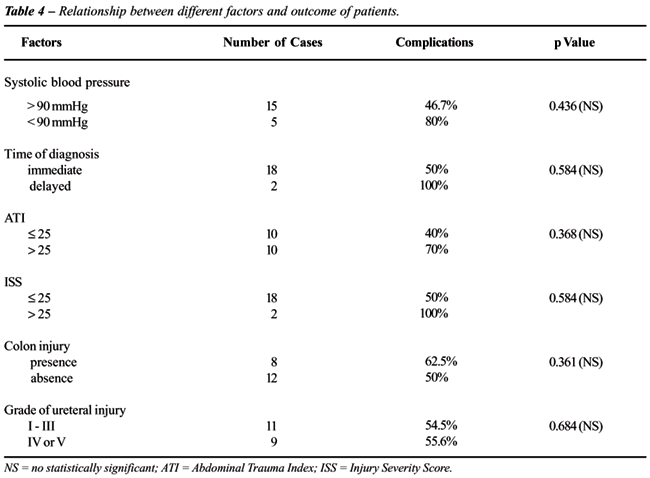
The presence of shock on admission, delayed
diagnosis, ATI > 25, ISS > 25 and colon injuries were associated
with a high complication rate, however there was no statistically significant
difference (Table-4). There were no deaths in this series and the mean
TRISS was 0.98. Hospitalization period ranged from 5 to 35 days, with
a mean of 12.4 days.
The follow-up ranged from 1 to 15 months
(mean of 5 months). Only four patients were available for one-year follow-up
and they were well with no evidence of stenosis on imaging studies (IVU)
performed later.
COMMENTS
The
ureters are relatively well protected by surrounding structures and their
small size and mobility contributes to their infrequent injury. Ureteral
lesions involve less than 1% of all trauma to the genitourinary tract
and are predominantly associated with penetrating injury (3,6,10). Ureteral
avulsion caused by blunt trauma is rare and typically occurs at the level
of ureteropelvic junction in children (16). Injuries caused by blunt trauma
will be recognized only by a high degree of suspicion of urologic injury,
and intravenous urography (IVU) is performed in suspected cases (9). In
our series, all patients were victims of penetrating trauma.
In our review, 85.3% of the patients had
no evidence of blood on urinalysis. Regardless of urinalysis result, a
suspected ureteral lesion must be evaluated before and during laparotomy.
There are controversies on the usefulness
of preoperative or intraoperative IVU for evaluating ureteral injury secondary
to penetrating trauma. Some authors observed that IVU had more than 30%
of false-negative rate, and a high dose of contrast on rapid infusion
IVU increases the sensitivity of this test (17). Presti et al. (3), Campbell
et al. (2) and Azimuddin et al. (18) found IVU diagnostic with definite
evidence of ureteric injury in 14% to 33% of cases. In our series, IVU
or CT were not performed preoperatively in any patient, but they are an
important tool for recognizing missed injuries in complicated cases. Retrograde
pyelography is probably the most sensitive radiographic tool for ureteral
injury diagnosis. It was done in two patients with missed injury and in
another with fistula after blast injury of ureter, and demonstrated contrast
extravasation in all of them.
Traumatic injury to the ureter is often
undiagnosed at the time of presentation and may have been overlooked in
the past, due to many reasons, including the magnitude of associated injuries
and low index of suspicion. All penetrating abdominal injuries should
be explored when first recognized (2,9,10). Direct inspection remains
the fastest and most reliable method for detecting ureteric injury. An
extended exploration of the retroperitoneum is mandatory in all cases
of penetrating injury to this region. In cases of gunshot wounds, especially
high velocity, a meticulous exploration of the area of retroperitoneal
violation must be done, to avoid missing injuries secondary to the blast
effect of missiles (18). Even gross inspection may sometimes miss a blast
effect and there may be a role of postoperative IVU in these cases of
high velocity gunshot wounds (2,18). Intravenous administration of either
methylene blue or diuretics may identify the injury site when it is not
obvious intra-operatively.
In our study, 10% of the patients had a
delay in diagnosis. A thorough exploration of retroperitoneum was not
done in these two cases. Other studies had shown a delay in diagnosis
ranging from 0% to 57% (2-6,17). The importance of timely recognition
was demonstrated in many reports. Immediate recognition of ureteric injury
was associated to better results and outcome than delayed recognition
(2,3,8,19). Campbell et al. (3) observed that the complication rate for
patients with a delay in diagnosis was 40% (2/5), compared to 10% (1/10)
when the diagnosis was made at the time of presentation. It is important
to be aware for signs of potential missed injury in the postoperative
period. The most important signs of urinary leakage are prolonged ileus,
low-grade fever, flank tenderness and persistent drainage from operative
sites (4). Endourologic management of these cases is recommended by some
authors (8,20). Endourologic procedures are safe and simple techniques,
and will obviate the need for kidney drainage or open surgery. In our
series, the two patients with late diagnosis were treated endoscopically
with double J stent, with satisfactory evolution, needing no further intervention.
However, both patients had their hospital stay extended because of the
delayed diagnosis.
In this series, two patients had contusion
of the ureteric wall. One patient was observed expectantly, with good
evolution, and the other developed a urinary fistula. Azimuddin et al.
(18) described 3 patients with contusion of the ureteric wall treated
without resection. A DJ stent was used in one, while the other two were
observed expectantly and recovered without complication (18). According
to other authors, simple stenting contused ureter (blast effect) may be
adequate treatment (2,10).
Penetrating injuries of abdominal cavity
rarely involve the ureter alone (2,3,5,7,9,17,18,21). Associated injuries
to the gastrointestinal tract are commonly present, and may modify the
management of ureteral injury at initial procedure. In our study, all
patients had associated injuries and a mean ATI of 25. Presti et al. (3)
observed a mean number of organs injured per patient of 3,7, a mean ISS
of 20.5 and ATI of 24. Hemodynamic instability or extensive damage to
intra-abdominal organs might preclude definitive repair initially. In
this series, the patients with shock on admission had more complications,
including a case of urinary fistula. In other studies, the presence of
shock, intraoperative bleeding and multiple organ involvement, were associated
with a higher morbidity and mortality in patients with ureteral injuries
(7).
We attempted to classify ureteral injuries
according to the Organ Injury Scaling of the American Association for
the Surgery of Trauma, and as it was observed by other authors, no statistically
significant correlation was found between the grade of ureteral injury
and morbidity. Best et al. (21) observed that mortality increased with
AAST-OIS injury grade but it was not related to the ureteral injury.
Velmahos et al. (7) identified the presence
of shock on admission, intra-operative bleeding, multiple intra-abdominal
organ involvement, and especially severe colonic injury requiring colectomy
as predictive of a poor outcome. In our series the presence of shock on
admission, delayed diagnosis, ATI > 25, ISS > 25 and colon injuries
were associated to a high complication rate, however, there was no statistically
significant difference.
The accepted surgical management of ureteral
injuries included adequate debridement of devitalized tissue, a water-tight,
tension-free spatulated anastomosis, isolation from associated contaminated
injuries, adequate drainage and ureteral stenting (2-4,8,9,17,18,21).
In stable patient, the preferred option
for repair of proximal and mid ureteric injuries is debridement and primary
ureteroureterostomy. Some authors believe that repair of all proximal
injuries should include a nephrostomy tube, and others do not find this
to be necessary (2-4,9,10,17). We do not believe that nephrostomy diversion
is necessary in cases of ureteral injury, and this procedure was not used
in our series. We routinely repair ureters over an indwelling stent, removed
cystoscopically after 6 weeks. We prefer to use internal ureteral stents,
with double J stent in cases of ureteroureterostomy and feeding tube in
cases of ureteroneocystostomy.
This study has limitations related to its
retrospective design and small number of cases. The results of this study
suggest that a large, multi-center, well-designed prospective study is
needed to evaluate and compare diagnostic approaches for ureteric injuries
and to establish an effective treatment algorithm.
CONCLUSIONS
A
high index of suspicion is required to enable surgeons to make the diagnosis
of ureteral injury as promptly as possible, however, in 10% of our cases
the injury was initially missed. The majority of cases (80%) were treated
successfully by primary repair.
The overall incidence of complications was
high in patients with shock on admission, delayed diagnosis, multiple
intra-abdominal organ involvement (ATI and ISS higher than 25), and colonic
injury, but no statistically significant correlation was found between
different factors and morbidity.
CONFLICT OF INTEREST
None declared.
REFERENCES
- St Lezin MA, Stoller ML: Surgical ureteral injuries. Urology. 1991; 38: 497-506.
- Campbell EW Jr, Filderman PS, Jacobs SC: Ureteral injury due to blunt and penetrating trauma. Urology. 1992; 40: 216-20.
- Presti JC Jr, Carroll PR, McAninch JW: Ureteral and renal pelvic injuries from external trauma: diagnosis and management. J Trauma. 1989; 29: 370-4.
- Palmer LS, Rosenbaum RR, Gershbaum MD, Kreutzer ER: Penetrating ureteral trauma at an urban trauma center: 10-year experience. Urology. 1999; 54: 34-6.
- Holden S, Hicks CC, O’Brien DP, Stone HH, Walker JA, Walton KN: Gunshot wounds of the ureter: a 15-year review of 63 consecutive cases. J Urol. 1976; 116: 562-4.
- Medina D, Lavery R, Ross SE, Livingston DH: Ureteral trauma: preoperative studies neither predict injury nor prevent missed injuries. J Am Coll Surg. 1998; 186: 641-4.
- Velmahos GC, Degiannis E, Wells M, Souter I: Penetrating ureteral injuries: the impact of associated injuries on management. Am Surg. 1996; 62: 461-8.
- Ghali AM, El Malik EM, Ibrahim AI, Ismail G, Rashid M: Ureteric injuries: diagnosis, management, and outcome. J Trauma. 1999; 46: 150-8.
- Guerriero WG: Ureteral injury. Urol Clin North Am. 1989; 16: 237-48.
- McAninch JW, Santucci RA. Genitourinary trauma. In: Walsh PC, Retik AB, Vaughan, EDJ (Eds.), Campbell’s Urology. Eighth edition. New York, Saunders. 2002; 4: 3707-3744.
- Champion HR, Sacco WJ, Copes WS, Gann DS, Gennarelli TA, Flanagan ME: A revision of the Trauma Score. J Trauma. 1989; 29: 623-9.
- Borlase BC, Moore EE, Moore FA: The abdominal trauma index—a critical reassessment and validation. J Trauma. 1990; 30: 1340-4.
- Baker SP, O’Neill B, Haddon W Jr, Long WB: The injury severity score: a method for describing patients with multiple injuries and evaluating emergency care. J Trauma. 1974; 14: 187-96.
- Boyd CR, Tolson MA, Copes WS: Evaluating trauma care: the TRISS method. Trauma Score and the Injury Severity Score. J Trauma. 1987; 27: 370-8.
- Moore EE, Cogbill TH, Jurkovich GJ, McAninch JW, Champion HR, Gennarelli TA, et al.: Organ injury scaling. III: Chest wall, abdominal vascular, ureter, bladder, and urethra. J Trauma. 1992; 33: 337-9.
- Kotkin L, Brock JW 3rd: Isolated ureteral injury caused by blunt trauma. Urology. 1996; 47: 111-3.
- Perez-Brayfield MR, Keane TE, Krishnan A, Lafontaine P, Feliciano DV, Clarke HS: Gunshot wounds to the ureter: a 40-year experience at Grady Memorial Hospital. J Urol. 2001; 166: 119-21.
- Azimuddin K, Milanesa D, Ivatury R, Porter J, Ehrenpreis M, Allman DB: Penetrating ureteric injuries. Injury. 1998; 29: 363-7.
- Mendez R, McGinty DM: The management of delayed recognized ureteral injuries. J Urol. 1978; 119: 192-3.
- Cormio L, Battaglia M, Traficante A, Selvaggi FP: Endourological treatment of ureteric injuries. Br J Urol. 1993; 72: 165-8.
- Best CD, Petrone P, Buscarini M, Demiray S, Kuncir E, Kimbrell B, et al.: Traumatic ureteral injuries: a single institution experience validating the American Association for the Surgery of Trauma-Organ Injury Scale grading scale. J Urol. 2005; 173: 1202-5.
____________________
Accepted
after revision:
November 26, 2006
_____________________
Correspondence address:
Dr. Gustavo Pereira Fraga
Rua Cel. Silva Teles, 211 / 3
Campinas, SP, 13024-000, Brazil
Fax: + 55 19 3788-7481
E-mail: fragagp@uol.com.br
The
authors retrospectively review their eight-year experience with the management
of penetrating ureteral trauma. Their observations are well-supported
by several earlier case series, including our own (1). Ureteral injuries
are rare and are often present without hematuria or hypotension. Thus,
a high index of suspicion is warranted in the evaluation of any patient
with retroperitoneal trauma, particularly from gunshot wounds as the blast
effect can have consequences up to 2 cm away from the path of the bullet.
My practice is to stent all contusions due to blast effect as this often
progresses to necrosis in the subsequent days and the defect will heal
well over a stent.
As
the authors suggest, the best radiographic techniques for the identification
of ureteral trauma include retrograde pyelogram or computerized tomography
(CT) with delayed pyelogram-phase views. When laparotomy is warranted
for other reasons it is ill-advised to delay surgery in order to perform
these time-consuming tests. As such, we are often presented with the dilemma
of evaluating retroperitoneal hematoma without the aid of high-quality
imaging. An on-table one-shot intravenous pyelogram can be performed in
the operating theater but is insensitive for the diagnosis of ureteral
injury. Thus, when the path of the bullet aligns with the known path of
the ureter, retroperitoneal exploration is indicated in order to rule
out a ureteral injury. As the authors describe, visual inspection is key
and can be augmented by injection of methylene blue. Another technique
is to make a cystotomy and pass catheters up the ureters.
There
are rare cases when penetrating trauma occurs along the known course of
the ureter but opening of the retroperitoneum is felt to be contra-indicated
(i.e. due to fear of releasing a contained hematoma after pelvic fracture
or iliac vein injury) or when the patient’s hemodynamic status does
not allow a thorough exploration of the ureter. In these cases every effort
should be made to perform retrograde pyelograms with possible stent placement
in the operating theater at the time of laparotomy or to obtain imaging
with CT scan or retrograde pyelograms within the first postoperative day.
When transporting the unstable patient out of the Intensive Care Unit
on postoperative day #1 is not possible, I have performed retrograde pyelograms
at the bedside using a flexible cystoscope and portable kidneys, ureters
and bladder (KUB) x-ray. With due vigilance we can strive to minimize
the delayed presentation of ureteral injury. Fortunately, the authors
were able to endoscopically manage both patients who presented with delayed
injury. In the case of delayed presentation of a complete transection
that can not be managed with ureteral stenting, one should consider a
percutaneous nephrostomy tube with delayed reconstruction rather than
pursue repeat laparotomy in the polytrauma patient.
REFERENCE
1. Elliott SP, McAninch JW: Ureteral injuries from external violence: the 25-year experience at San Francisco General Hospital. J Urol. 2003; 170:1213-6.
Dr. Sean
P. Elliott
Assistant Professor of Urology
University of Minnesota
Minneapolis, Minnesota, USA
E-mail: selliott@umn.edu
EDITORIAL
COMMENT
The
authors of this paper have described their experience in identifying and
managing acute ureteral injuries secondary to external trauma. This is
a retrospective review of their institutions experience with penetrating
ureteral injuries, thoroughly evaluating associated factors and trends.
Although not an original addition, I think it adds reinforcing value to
recent literature. Their findings as far as incidence of hematuria, method
of diagnosis, and management options are comparable to those documented
by other series. (1-3). I do have a comment in regards to their intraoperative
success in diagnosing the ureteral injury. All 20 patients in this series
went directly to exploratory laparotomy, despite 75% being hemodynamically
stable. Perhaps if these patients had preoperative imaging, particularly
with a contrast-enhanced CT scan with delayed images, there would have
been no missed injuries. Although their overall complication rate seems
high, this can be due to the severity of injury that their population
obtained. The percentage of urologic specific injuries is consistent with
other series. Overall, I believe this to be a very well done study, highlighting
the importance of having a high index of suspicion for ureteral injuries
and assessing the need for management based on grade of injury and timing
of diagnosis. This data will contribute to the validity of the AAST-OIS
grading scale for ureteral injury.
REFERENCES
- Presti JC Jr, Carroll PR, McAninch JW: Ureteral and renal pelvic injuries from external trauma: diagnosis and management. J Trauma. 1989; 29:370-4.
- Best CD, Petrone P, Buscarini M, Demiray S, Kuncir E, Kimbrell B, et al: Traumatic ureteral injuries: a single institution experience validating the American Association for the Surgery of Trauma-Organ Injury Scale. J Urol. 2005; 173: 1202-5.
- Palmer LS, Rosenbaum RR, Gershbaum MD, Kreutzer ER: Penetrating ureteral trauma at an urban trauma center: 10-year experience. Urology. 1999; 54:34-6.
Dr. Charles D. Best
Chief, Department of Urology
Los Angeles County and Univ. Southern California
LAC/USC County Medical Center
Los Angeles, California, USA
E-mail: cbest@usc.edu