ULTRASOUND
GUIDED PERCUTANEOUS NEPHROSTOMY FOR OBSTRUCTIVE UROPATHY IN BENIGN AND
MALIGNANT DISEASES
(
Download pdf )
G. SOOD, A. SOOD, A. JINDAL, D.K. VERMA, D.S. DHIMAN
Department of Surgery and Department of Radiology, Indira Gandhi Medical College Shimla H.P., India
ABSTRACT
Objective:
Analyze the success rate, complications and overall benefit of ultrasound
guided percutaneous nephrostomy (PCN) for the relief of obstructive uropathy
in benign and malignant diseases.
Materials and Methods: PCN was performed
in 50 kidneys of 32 patients. It was performed in emergency rooms totally
under ultrasound guidance by general surgeons. Seldinger technique was
used in all cases. Changes in renal function after the procedure were
analyzed using paired t-test.
Results: The procedure was successfully
completed in 42 out of 50 kidneys (84%). There has been no major complication
and 28% minor complications. The renal function improved significantly
when PCN was performed for benign conditions (mean creatinine 3.52 mg/dL
before and 2.18 mg/dL after PCN), however in malignancy there has been
no significant improvement in renal function (before PCN mean creatinine
6.39 mg/dL and after PCN 5.41 mg/dL).
Conclusion: We conclude that PCN can be
effectively performed under ultrasound guidance and should be the initial
procedure in acutely obstructed kidneys with pyonephrosis and poor renal
function. In malignant cases, however, improvement in renal function is
possible only if the procedure is carried out at an early stage.
Key
words: hydronephrosis; ureteral obstruction; percutaneous nephrostomy;
ultrasound
Int Braz J Urol. 2006; 32: 281-6
INTRODUCTION
Obstructive
uropathy is a condition occurring due to blockage of urine flow, resulting
in increased pressure within the collecting system and kidney injury.
Interruption of urinary flow results in pain, infection, sepsis, and loss
of renal function. It is a potentially life threatening condition and
immediate measures are required to decompress the kidneys. The various
modalities available are retrograde stenting, open drainage of kidneys
and percutaneous nephrostomy.
Percutaneous nephrostomy (PCN) has come
a long way from the times of William Goodwin, who inadvertently punctured
the renal pelvis attempting a translumbar aortogram (1). Although percutaneous
nephrostomy was developed using fluoroscopic guidance, ultrasound guided
procedures are now safe, easy and effective (2-5).
We performed PCN in patients, with both
benign and malignant conditions solely under ultrasound guidance with
the help of radiologists and evaluated the success rate of the procedure,
related complications and outcome in patients with benign and malignant
renal diseases.
MATERIALS AND METHODS
A
prospective study was carried out in 50 kidneys of 32 patients suffering
from obstructive uropathy. It included 18 males and 14 females with both
benign and malignant causes of obstructive uropathy. The mean age in this
study group was 41.4 years, ranging from 10 to 63 years. In males the
average age was 41.5 years ranging from 10 to 63 years and in females
it was 42 years ranging from 19 years to 63 years.
The percutaneous nephrostomy was performed
entirely under ultrasound guidance as soon as it was possible in emergency.
The procedure was thoroughly explained to the patient and relatives. Informed
consent was obtained.
All patients were subjected to routine investigations
and the following patients were excluded from the study: untreated bleeding
disorders, untreated urinary tract infection, hemoglobin less than 10
mg/dL. In patients failing to meet these criteria all parameters were
corrected before proceeding with PCN.
The patients were placed on the ultrasound
table in prone position and a pillow placed under the abdomen on the side
to be operated to correct lumbar lordosis and support the kidney. Ultrasound
scanning was performed using a 7.5 MHz transducer to obtain a median longitudinal
scan through the kidney. As soon as the initial puncture site was chosen
it was cleaned and draped. Local anesthesia was injected at the puncture
site and around it using 3-5 mL of 1% lignocaine. Sterile betadine jelly
was applied to the transducer and localization of the puncture site was
carried out again.
We performed the Seldinger technique in
all patients. The skin and fascia were incised with a #11 blade and then
the scanning head was shifted over the incision to measure the distance
between the skin and the calyx. An 18G-sheathed needle was inserted blindly
through the incision and aimed at the direction previously determined
by the ultrasound. The sonographic view as well as urine confirmed that
the needle was at the desired site. The needle was removed leaving a small
catheter in place and a curved J tip 0.038 guide wire was inserted into
the collecting system through the puncture needle. Once the guide wire
was in position, the fascial dilators were inserted with rotating movements
during advancement. The tract was dilated 2F over the desired catheter
to be placed, after tract dilation a polyethylene pigtail catheter was
introduced over the guide wire. The pigtail catheter was firmly sutured
to the skin using silk 1-0 and adhesive strapping was performed.
RESULTS
Percutaneous
nephrostomies were performed for various indications in obstructive uropathy
due to benign and malignant tumors. Twenty one (42%) nephrostomies were
done for benign indications and 29 (58%) for malignant conditions (Table-1).

PCN was successfully completed in 42 kidneys
(84%) cases. The 8 cases in which the procedure was not completed included
both benign and malignant conditions (Table-2).
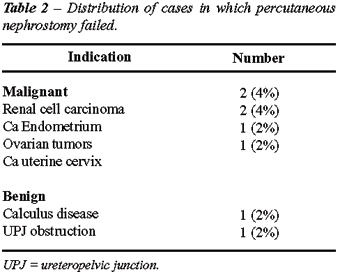
Failure was seen mostly in the early part
of study and was attributed to the learning curve and difficult renal
anatomy. Open nephrostomy was carried out in failed procedures.
The average time taken for completing the
procedure was 48 minutes ranging from 20 minutes to 120 minutes. There
were no major procedure related complications or deaths. Tube displacement
was seen in 6 cases (12%). Transient hematuria was seen in 7 cases (14%).
No blood transfusions were required and hematuria settled on its own in
1-3 days. Post procedure urine leak was present in one patient (2%).
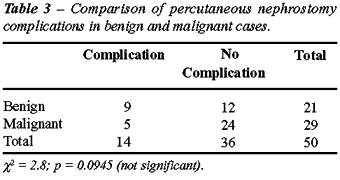
There were no procedure related complications
in patients in whom the procedure failed. The complication rate between
benign and malignant diseases was not significant p value = 0.0945.
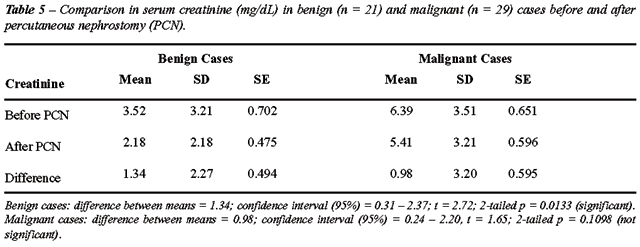
The serum creatinine was compared after
the procedure with those of previous values using the paired t test (Tables-3
and 4).

Of the 32 patients who were subjected to
PCN for various conditions, 20 were subjected to open definitive surgeries.
There were 4 deaths in the study group; 3 of these were in the malignancy
group and 1 in the benign group, however, none of these were procedure
related.
In the benign group out of 17 patients,
15 improved, 1 died and 1 was referred to a higher centre.
In the malignant group of 15 patients, 6
patients showed improvement, 6 patients did not show any improvement,
3 patients died and no patient was referred.
COMMENTS
Most
of the studies have shown a success rate of more than 90% under various
types of guidance modalities (2,3,6). PCN has traditionally been done
under fluoroscopic guidance by radiologists and a success rate of more
than 95% is common (2). It is in only the last decade that more and more
procedures have been performed under other guidance modalities such as
ultrasound and CT scan (7,8).
Percutaneous nephrostomy can be performed
under ultrasound guidance with a success rate ranging from 83.1% to 92%
(3,6).
Traditionally diversion has been accomplished
by cystoscopy with retrograde passage of ureteric catheter and only in
the event of obstruction to catheter passage, nephrostomy is performed
but in our setup where cystoscopy is not always readily available nephrostomy
is an attractive alternative.
Pederson was the first to use only sonographic
guidance for Percutaneous nephrostomy, and reported a success rate of
70 % (4). Since then a large number of studies have been carried out under
sole ultrasound guidance describing success rate up to 92%. This is because
of the advent of high resolution ultrasound machines with better view
of the pelvicaliceal system allowing a success rate comparable to fluoroscopic
guidance with practically no radiation hazard.
In our study the success rate was 84%, which
was consistent with the above mentioned studies.
Azotemia due to bilateral obstructed kidneys
has been the most frequent indication of nephrostomy. PCN is often the
simplest method for the initial management of obstructive renal failure
due to hazards of surgery in uremic patients.
PCN is sometimes described as a temporizing
measure prior to corrective surgery (5,6). We observed similar pattern
in our series too as in 10 out of 17 benign cases (58%) surgery was carried
out. PCN was definitive in 5 patients (29%). In the malignant group definitive
surgery was planned according to the origin and grading of malignancy.
PCN was performed for both benign and malignant
diseases. In 17 benign cases it was done to relieve obstruction and salvage
the kidneys, which was significantly achieved. (Tables-4 and 5). Subsequent
surgery followed in 10 cases. PCN proved to be definitive by itself in
one patient with chyluria. Patient improved markedly and no further intervention
was required. There was one death in the study, 7 days after the procedure;
the cause of death being rheumatic heart disease with mitral regurgitation,
mitral stenosis and tricuspid regurgitation. One child was referred because
of procedure failure.
The most consistent and gratifying results
were seen in patients who presented pyonephrosis. PCN was successfully
completed in all 4 cases and kidneys were salvaged in all cases with the
least morbidity. The co-existence of azotemia and pyonephrosis increases
the urgency as well as value of percutaneous Nephrostomy. Camunez et al.
also observed that following PCN in pyonephrosis clinical symptoms disappeared
in 24 - 48 h after the procedure and once the acute phase was over definitive
surgery could be carried out (9).
In the malignant group there was no significant
recovery of the renal functions (Table-5). Definitive surgery was carried
out in only 4 out of 15 patients. In 2 patients open nephrostomy had to
be performed due to failure or catheter dislodgement. 3 patients succumbed
to their illness in the hospital only, the cause of death being grossly
deranged renal functions with dyselectrolytemia. Only 6 patients showed
definite improvement.
The usefulness of percutaneous nephrostomy
as an adjunct in many pelvic organ malignancies has been reviewed in many
series. Samarsinghe et al. did not find any renal function improvement
in patients with chronic obstruction and terminal malignancy (10).
When hydronephrosis occur from advanced
pelvic malignant disease, percutaneous nephrostomy can effectively improve
renal function. However, since these patients have an overall poor prognosis,
several authors earlier used to question the appropriateness of interventional
uroradiological procedures (11,12). Hoe & Tung observed an overall
survival median of 5 months after PCN and 68% of people achieving a useful
life (13). They concluded that PCN should be performed only in cases where
there is no evidence of carcinomatous spread and few or no medical problems.
Various other studies have disputed this
claim; Markovich et al. concluded that PCN was beneficial for malignant
obstructive uropathy associated with fewer complications as compared to
open nephrostomy and increased percentage of time spent at home. The average
post-nephrostomy survival time in this study was 7 months (14).
Our study showed definite improvement in
6 out of 15 patients with terminal malignancy, 6 patients did not show
any improvement and there were 3 deaths due to an underlying disease.
Our results in malignant group were consistent with all previously mentioned
studies; renal function could not be recovered in patients who presented
late unsalvageable kidneys. However, patients who were seen at an earlier
stage benefited from PCN.
PCN is usually performed when a retrograde
stenting is not possible. It may be due to difficult anatomy or lack of
technical expertise. Comparative studies have been carried out between
percutaneous nephrostomy and retrograde ureteric stenting. Pearle et al.
found no difference in clinical efficacy, or patient preference between
the two procedures and concluded that the choice of procedure may be based
on particular circumstance of the patient and availability of facilities
to carry it out (15).
A similar study however found PCN to be
superior to retrograde stenting, their results demonstrated that percutaneous
nephrostomy is tolerated better by patients and has a lower influence
on the quality of life than ureteral stents. The effectiveness of percutaneous
nephrostomy should be given preference over ureteral stents in case initial
signs of infected hydronephrosis are detected (16).
We observed a complication rate of 28%.
There was no major complication throughout the study and in 14% of the
cases hematuria settled by itself. Tube displacement was other minor complication
(12%) for which 3 open nephrostomies had to be performed. Post procedure
urine leak was seen in 1 patient which also subsided by itself.
Procedure-related complications continue
to be widely reported regardless of the type of imaging employed (17).
Rates vary from 25 - 60% though this includes late (more than 24 hours
after insertion) minor complications such as those related to tube malfunction,
leakage, dislodgment and incrustations. Picus et al. summarized early
complications inherent with fluoroscopy-guided PCN, being the most common
acute bleeding requiring transfusion (< 5%), failed access (< 5%),
adjacent organ injury: bowel, spleen, lung (< 1%), and septicemia (<
1) (17).
In most of the studies significant hemorrhage
requiring transfusion or surgical control ranks first among the complications
(5.3%) and is equally distributed among ultrasound guided and fluoroscopic
guided groups (17). Significant bleeding occurs in patients with associated
stones, although this is usually manageable by means of transfusions,
open control remains an option and in such instance stone surgery may
then be performed. Minor bleeding is common but usually resolves spontaneously
with observation and occasional flushing of the catheter.
Adjacent organ injury is another complication,
the colon and pleura may be inadvertently injured; the former had the
need of a colostomy, the latter, a tube thoracostomy. Pleural tear has
been deemed more common in instances wherein the nephrostomy tract is
placed more superiorly, particularly when subsequent stone manipulation
is contemplated (17).
These aforementioned complications being
present equally in both ultrasound and fluoroscopy-guided PCN may simply
indicate no distinction between the two as far as patient safeties is
concerned. Overall patient status, skill of the operator, technique and
instrumentation would probably play a more significant role.
All findings confirm that PCN is quite effective
in improving renal functions provided it is preformed at an earlier stage.
Intervention in malignant ureteric obstruction should not necessarily
be viewed with as much pessimism as in the past. Ultimately the decision
to place a nephrostomy tube lies in the doctor, the family and above all
the patient.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Goodwin WE, Casey WC, Woolf W: Percutaneous trocar (needle) nephrostomy in hydronephrosis. J Am Med Assoc. 1955; 157: 891-4.
- Kehinde EO, Newland CJ, Terry TR, Watkin EM, Butt Z: Percutaneous nephrostomies. Br J Urol. 1993; 71: 664-6.
- Gupta S, Gulati M, Uday Shankar K, Rungta U, Suri S: Percutaneous nephrostomy with real-time sonographic guidance. Acta Radiol. 1997; 38: 454-7.
- Pedersen JF: Percutaneous nephrostomy guided by ultrasound. J Urol. 1974; 112: 157-9.
- Martino P: Ultrasound-guided percutaneous nephrostomy. Arch Ital Urol Androl. 2000; 72: 324-7.
- Nielsen OS, Grossmann E: Ultrasonically guided percutaneous nephrostomy. Scand J Urol Nephrol. 1990; 24: 219-21.
- Mahaffey KG, Bolton DM, Stoller ML: Urologist directed percutaneous nephrostomy tube placement. J Urol. 1994; 152: 1973-6.
- Smith AD: Percutaneous punctures - is this the endourologist’s turf? J Urol. 1994; 152: 1982-3.
- Camunez F, Echenagusia A, Prieto ML, Salom P, Herranz F, Hernandez C: Percutaneous nephrostomy in pyonephrosis. Urol Radiol. 1989; 11: 77-81.
- Samarasinghe UC, Perera ND: The value of percutaneous nephrostomy; Sri Lankan experience. Ceylon Med J. 1998; 43: 92-5.
- Holden S, McPhee M, Grabstald H: The rationale of urinary diversion in cancer patients. J Urol. 1979; 121: 19-21.
- Ortlip SA, Fraley EE: Indications for palliative urinary diversion in patients with cancer. Urol Clin North Am. 1982; 9: 79-84.
- Hoe JW, Tung KH, Tan EC: Re-evaluation of indications for percutaneous nephrostomy and interventional uroradiological procedures in pelvic malignancy. Br J Urol. 1993; 71: 469-72.
- Markowitz DM, Wong KT, Laffey KJ, Bixon R, Nagler HM, Martin EC: Maintaining quality of life after palliative diversion for malignant ureteral obstruction. Urol Radiol. 1989; 11: 129-32.
- Pearle MS, Pierce HL, Miller GL, Summa JA, Mutz JM, Petty BA, et al.: Optimal method of urgent decompression of the collecting system for obstruction and infection due to ureteral calculi. J Urol. 1998; 160: 1260-4.
- Mokhmalji H, Braun PM, Martinez Portillo FJ, Siegsmund M, Alken P, Kohrmann KU: Percutaneous nephrostomy versus ureteral stents for diversion of hydronephrosis caused by stones: a prospective, randomized clinical trial. J Urol. 2001; 165: 1088-92.
- Clayman RV, McDougall EM, Nakada SY: Endourology of The Upper Urinary Tract: Percutaneous Renal and Ureteral Procedures. In: Walsh PC, Retik AB, Vaughan ED, Wein AJ (ed.), Campbell’s Urology. Philadelphia, WB Saunders. 1998; pp. 2791-800.
____________________
Accepted after revision:
May 13, 2006
_______________________
Correspondence
address:
Dr. Gaurav Sood
Department of surgery
Indira Gandhi Medical College
Shimla, HP, India
E-mail: gaurav2sood@yahoo.com