HAND-ASSISTED
LAPAROSCOPIC RADICAL NEPHRECTOMY IN THE TREATMENT OF A RENAL CELL CARCINOMA
WITH A LEVEL II VENA CAVA THROMBUS
(
Download pdf )
JASON R. KOVAC, PATRICK P. LUKE
McMaster Institute of Urology (JRK), St. Joseph’s Hospital, Hamilton, Ontario, Canada and Division of Urology (PPL), The University of Western Ontario, London, Ontario, Canada
ABSTRACT
Excision of renal cell carcinoma (RCC) with corresponding vena cava thrombus is a technical challenge requiring open resection and vascular clamping. A 58 year old male with a right kidney tumor presented with a thrombus extending 1 cm into the vena cava. Using a hand-assisted transperitoneal approach through a 7 cm gel-port, the right kidney was dissected and the multiple vascular collaterals supplying the tumor were identified and isolated. The inferior vena cava was mobilized 4 cm cephalad and 4 cm caudal to the right renal vein. Lateral manual traction was applied to the right kidney allowing the tumor thrombus to be retracted into the renal vein, clear of the vena cava. After laparoscopic ultrasonographic confirmation of the location of the tip of the tumor thrombus, an articulating laparoscopic vascular stapler was used to staple the vena cava at the ostium of the right renal vein. This allowed removal of the tumor thrombus without the need for a Satinsky clamp. The surgery was completed in 243 minutes with no intra-operative complications. The entire kidney and tumor thrombus was removed with negative surgical margins. Estimated blood loss was 300 cc. We present a laparoscopic resection of a renal mass with associated level II thrombus using a hand-assisted approach. In patients with minimal caval involvement, our surgical approach presents an option to the traditional open resection of a renal mass.
Key
words: laparoscopy; renal cell carcinoma; nephrectomy; vena cava;
thrombus
Int Braz J Urol. 2010; 36: 327-31
INTRODUCTION
Laparoscopic
radical nephrectomy has emerged as a standard surgical option for the
treatment of renal cell carcinoma within the past 10 years. First described
by Clayman et al. in 1991 (1), laparoscopic radical nephrectomy is associated
with reduced post-operative pain and improved convalescence vs. open radical
nephrectomy (2). Furthermore, long-term studies have demonstrated similar
oncologic outcomes with standard open radical nephrectomy (3).
Involvement of the inferior vena cava (IVC) occurs in 4-10% of renal cell
carcinoma (RCC) patients (4). The presence of a renal vein thrombus was
previously considered a contraindication to laparoscopic resection. The
first case-report description of a laparoscopic nephrectomy with the thrombus
extending into the renal vein (level I) was by Savage et al. in 2000 (5).
Subsequently, the technical feasibility of this approach was confirmed
by our group and others (6,7).
Extension of the thrombus into the vena cava (level II) complicates the
laparoscopic approach. Using a porcine model, Fergany et al. (8) reported
7 successful nephrectomies with level II caval thrombi. Others have expanded
these animal studies to clinical cases with thrombi projecting 1 cm (9)
and 2 cm (10) into the vena cava. In those studies, Satinsky vascular
clamps were used to achieve control of the cava and required laparoscopic
vascular suturing experience (11,12).
In this report, we describe a 58 year-old male presenting with an 8x9
cm RCC and metastatic lung nodules. A 1 cm level II vena cava thrombus
was identified and removed using a hand-assisted laparoscopic (HAL) approach.
The described approach obviates the need for laparoscopic vascular suturing.
SURGICAL TECHNIQUE
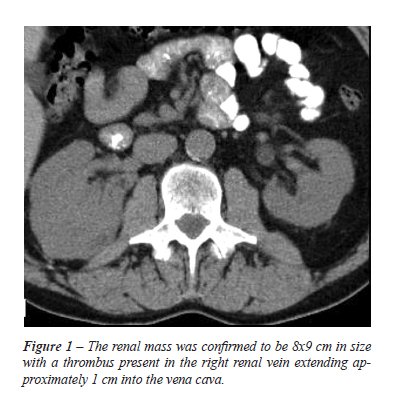
A 58 year old male with 20 pack-year smoking history presented with gross hematuria. Ultrasound documented a mass in the upper pole of the right kidney. This was confirmed by computerized tomography (CT) scan to be an 8x9 cm soft tissue mass in the right kidney (Figure-1). This also demonstrated a tumor thrombus projecting 1 cm into the IVC. Right hilar lymphadenopathy and four metastatic, subpleural lung nodules were also seen. A bone scan revealed no evidence of bony metastatic disease.
After discussion of its risks and potential survival benefit (13,14),
cytoreductive nephrectomy was performed. The authors were prepared to
perform a laparoscopic hand assisted nephrectomy with vascular control
through a Gel Port® (Applied Medical, Rancho Santa Margarita, California).
Satinsky clamps were to be used in the thrombectomy and laparoscopic suturing
of the cava. After induction with general anesthesia, the patient was
positioned in the left lateral decubitus position. With a muscle splitting
incision, a 7 cm laparoscopic hand-assist device was placed in the right
lower quadrant with the placement of two additional 10 mm ports directly
cephalad along the lateral rectus border, allowing 8 cm separation between
the ports and the hand-assist device.
Following dissection into the retroperitoneal space, the kidney was separated
from the psoas muscle, adjacent bowel and liver. The ureter and multiple
vascular collaterals were carefully isolated and divided. The renal artery
was controlled with laparoscopic clips and divided, thereby isolating
the entire right kidney, excluding the right renal vein. The renal vein
was dissected and the location of the tumor thrombus identified through
palpation. Intraoperative Doppler ultrasound was used to identify the
tip of the tumor thrombus and to exclude the presence of thrombus within
the cava. The lateral cava was extensively dissected around the entire
right renal vein. Furthermore, the IVC around the right renal vein was
dissected posteriorly and medially to permit mobilization of the cava
from retroperitoneal attachments over a vertical distance of 8 cm. To
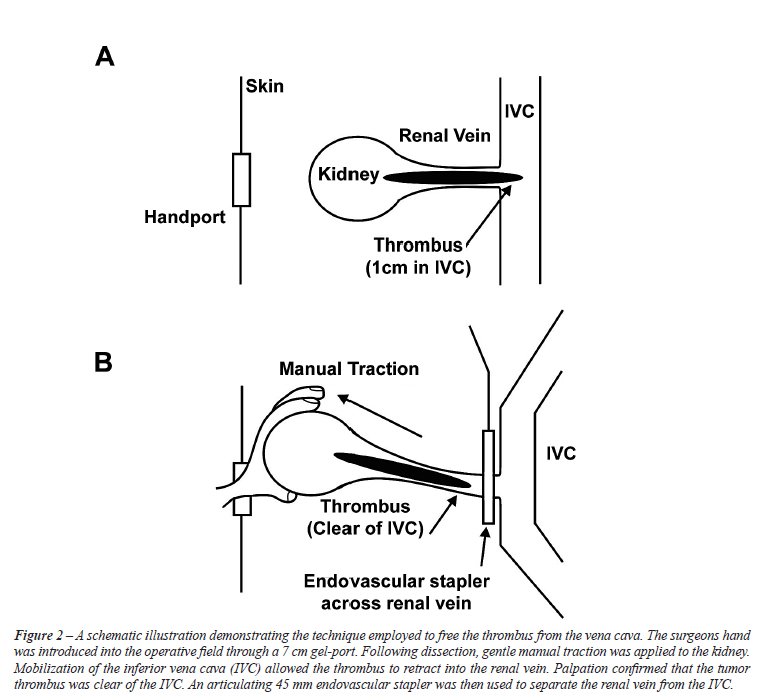
remove the renal vein and adjacent caval thrombus, gentle lateral traction
was applied to the kidney (Figure-2). Surprisingly, this maneuver allowed
the tumor thrombus to retract back within the renal vein. The position
of the tumor thrombus was confirmed with intra-operative Doppler ultrasound.
With the cava bowed laterally, the cava was stapled at the junction of
the right renal vein and cava using a 45 mm articulating vascular stapler
(Ethicon Endosurgery, CA). Through palpation and visual inspection, there
was no evidence of significant narrowing of the cava from its original
capacity. The specimen was extracted and the entire tumor thrombus was
examined and shown to be intact. Importantly, the thrombus was clear of
the staple line. The operation concluded in the standard fashion.
The procedure was completed successfully with a surgical time of 3.5 hr
and an estimated blood loss of 300 mL. Patient controlled analgesia with
morphine was discontinued on post-operative day one. Post-operatively,
the patient developed a mild ileus. A CT scan to investigate the ileus
demonstrated subclinical pulmonary emboli noted at the lung bases. Anticoagulation
was performed and the patient was treated with temsirolimus (mTOR inhibitor)
therapy for his metastatic disease. Pathology revealed the tumor to be
a clear cell carcinoma (Fuhrman grade 4) with tumor invasion into the
perinephric fat and negative resection margins. Twelve months post-operatively,
the metastatic deposits remained stable and the emboli resolved on follow-up
thoracic CT scanning.
COMMENTS
Excision
of a RCC with a level II caval thrombus is a technical challenge. Open
radical nephrectomy is the current standard of treatment, however successful
laparoscopic removal of tumors with level I renal vein thrombus (6) has
opened the door to resection of more extensive tumors.
Our group has previously reported that laparoscopic resection of renal
tumors with level I renal vein thrombi is feasible with and without the
use of laparoscopic ultrasound and hand assistance (6). Accordingly, the
Doppler ultrasound can distinguish the location of the tip of the tumor
thrombus, thereby providing a safe window through which the laparoscopic
stapler can be applied. Hand assistance devices also permit the use of
tactile assessment of the tip of the tumor thrombus.
We had originally planned to resect the kidney with tumor thrombus by
isolating the tumor thrombus and ostium of the right renal vein using
a conventional Satinsky clamp placed through the hand-assist device. However,
it was noted that the tumor thrombus could be retracted back flush to
the ostium of the right renal vein using lateral traction on the kidney
after complete mobilization of the IVC around the level of the renal vein.
Doppler ultrasound inspection and tactile assessment confirmed that the
tip of the tumor thrombus sat within the confines of the renal vein. This
allowed the laparoscopic stapler to be used to achieve vascular control
instead of the Satinsky clamp. This precluded the need for laparoscopic
vascular suturing after tumor resection.
There are significant limitations to the use of this technique. It can
only be used to treat renal masses with tumor thrombus that have minimal
extension into the IVC. In other words, had the tumor thrombus been more
extensive, it would not have been appropriate to significantly narrow
the IVC using the stapler. Furthermore, it would not have been advantageous
to have created a positive surgical margin using our described technique.
Indeed, pathology confirmed negative surgical margins in our resection
specimen. Nevertheless, we were prepared to use a Satinsky clamp to control
the IVC and also fully prepared to open the patient if full vascular control
of the IVC was required.
Our procedure was also complicated by the development of subclinical pulmonary
emboli. The authors admit that it is possible that the pulmonary emboli
may have propagated from the manipulation of the tumor thrombus. On the
other hand, there is no evidence that open resection of the tumor would
have prevented this complication.
CONCLUSIONS
We present a novel technique for laparoscopic resection of a renal mass with associated level II thrombus using a hand-assisted approach. By application of traction to the kidney after mobilization of the cava and use of an endoscopic vascular stapler, the mass was removed without the need for laparoscopic vascular sutures.
ACKNOWLEDGMENTS
The authors would like to thank Ms. A. Travers for her assistance.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Clayman RV, Kavoussi LR, Soper NJ, Dierks SM, Meretyk S, Darcy MD, et al.: Laparoscopic nephrectomy: initial case report. J Urol. 1991; 146: 278-82.
- Lam JS, Shvarts O, Pantuck AJ: Changing concepts in the surgical management of renal cell carcinoma. Eur Urol. 2004; 45: 692-705.
- Chan DY, Cadeddu JA, Jarrett TW, Marshall FF, Kavoussi LR: Laparoscopic radical nephrectomy: cancer control for renal cell carcinoma. J Urol. 2001; 166: 2095-9; discussion 2099-100.
- Kaplan S, Ekici S, Dogan R, Demircin M, Ozen H, Pasaoglu I: Surgical management of renal cell carcinoma with inferior vena cava tumor thrombus. Am J Surg. 2002; 183: 292-9.
- Savage SJ, Gill IS: Laparoscopic radical nephrectomy for renal cell carcinoma in a patient with level I renal vein tumor thrombus. J Urol. 2000; 163: 1243-4.
- Kapoor A, Nguan C, Al-Shaiji TF, Hussain A, Fazio L, Al Omar M, et al.: Laparoscopic management of advanced renal cell carcinoma with level I renal vein thrombus. Urology. 2006; 68: 514-7.
- Desai MM, Gill IS, Ramani AP, Matin SF, Kaouk JH, Campero JM: Laparoscopic radical nephrectomy for cancer with level I renal vein involvement. J Urol. 2003; 169: 487-91.
- Fergany AF, Gill IS, Schweizer DK, Kaouk JH, ElFettouh HA, Cherullo EE, et al.: Laparoscopic radical nephrectomy with level II vena caval thrombectomy: survival porcine study. J Urol. 2002; 168: 2629-31.
- Sundaram CP, Rehman J, Landman J, Oh J: Hand assisted laparoscopic radical nephrectomy for renal cell carcinoma with inferior vena caval thrombus. J Urol. 2002; 168: 176-9.
- Varkarakis IM, Bhayani SB, Allaf ME, Inagaki T, Gonzalgo ML, Jarrett TW: Laparoscopic-assisted nephrectomy with inferior vena cava tumor thrombectomy: preliminary results. Urology. 2004; 64: 925-9.
- Coelho JC, Sigel B, Flanigan DP, Schuler JJ, Justin J, Machi J: Arteriographic and ultrasonic evaluation of vascular clamp injuries using an in vitro human experimental model. Surg Gynecol Obstet. 1982; 155: 506-12.
- Barone GW, Conerly JM, Farley PC, Flanagan TL, Kron IL: Assessing clamp-related vascular injuries by measurement of associated vascular dysfunction. Surgery. 1989; 105: 465-71.
- Tongaonkar HB, Dandekar NP, Dalal AV, Kulkarni JN, Kamat MR: Renal cell carcinoma extending to the renal vein and inferior vena cava: results of surgical treatment and prognostic factors. J Surg Oncol. 1995; 59: 94-100.
- Nesbitt JC, Soltero ER, Dinney CP, Walsh GL, Schrump DS, Swanson DA, et al.: Surgical management of renal cell carcinoma with inferior vena cava tumor thrombus. Ann Thorac Surg. 1997; 63: 1592-1600.
____________________
Accepted after revision:
January 13, 2010
_______________________
Correspondence address:
Dr. Patrick P. Luke
Division of Urology
London Health Sciences Centre
339 Windermere Road
London, Ontario, N6A-5A5, Canada
Fax: + 5 19 663-3344
E-mail: patrick.luke@lhsc.on.ca