TRANSCUTANEOUS
ELECTRICAL NERVE STIMULATION (TENS) IN THE SYMPTOMATIC MANAGEMENT OF CHRONIC
PROSTATITIS/CHRONIC PELVIC PAIN SYNDROME: A PLACEBO-CONTROL RANDOMIZED
TRIAL
(
Download pdf )
LAMINA SIKIRU, HANIF SHMAILA, SAMANI A. MUHAMMED
Department of Physiotherapy/Physiology (LS), Faculty of Medical Sciences/Jimma Specialized Hospital, Jimma University, Jimma, Ethiopia, Department of Physiotherapy (HS), Murtala Mohammad Specialist Hospital, Kano, Nigeria, Department of Urology/Surgery (SAM), Murtala Mohammad Specialist Hospital, Kano, Nigeria
ABSTRACT
Objective:
The aim of the study was to investigate the therapeutic efficacy of transcutaneous
electrical nerve stimulation (TENS) in the symptomatic management of chronic
prostatitis pain/chronic pelvic pain syndrome.
Design: A pretest, posttest randomized double
blind design was used in data collection.
Participant: Twenty-four patients diagnosed
with chronic prostatitis- category IIIA and IIIB of the National Institute
of Health Chronic Pain (NIH-CP) were referred for physiotherapy from the
Urology department.
Intervention: Pre treatment pain level was
assessed using the NIH-CP (pain domain) index. The TENS group received
TENS treatment, 5 times per week for a period of 4 weeks (mean treatment
frequency, intensity, pulse width and duration of 60Hz, 100µS, 25mA
and 20 minutes respectively). The Analgesic group received no TENS treatment
but continued analgesics; the Control group received no TENS and Analgesic
but placebo. All subjects were placed on antibiotics throughout the treatment
period.
Outcome measures: Post-treatment pain level
was also assessed using NIH-CP pain index.
Result: Findings of the study revealed significant
effect of TENS on chronic prostatitis pain at p < 0.05.
Conclusion: TENS is an effective means of
non-invasive symptomatic management of chronic prostatitis pain.
Key
words: pain; TENS; chronic prostatitis; chronic pelvic pain
Int Braz J Urol. 2008; 34: 708-14
INTRODUCTION
In
1995 the National Institutes of Health (NIH) classified prostatitis into
4 main categories: 1) acute bacterial; 2) chronic bacterial; 3) non-bacteria
chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS); 4) asymptomatic
inflammatory. The CP/CPPS was further subdivided into inflammatory (category
IIIA) and non-inflammatory (category IIIB) prostatitis (1).
Chronic prostatitis/chronic pelvic pain
syndrome (CP/CPPS), the subject of the present study is a debilitating
condition diagnosed in the presence of chronic pelvic pain and lower urinary
tract symptoms (2). CP/CPPS is the most common (3), yet most poorly understood
“prostatitis syndrome” (4).CP/CPPS is truly a devastating
disease.
A new perception of CP/CPPS appeared following
the 1995 NIH/NIDDK workshop, which emphasized the importance of pain as
the hallmark of CP/CPPS and questioned the role of the prostate in producing
the symptoms (2).
Chronic pelvic pain syndrome (NIH category
III) and commonly manifests as pain in areas including the perineum, rectum,
prostate, penis, testicles, and abdomen (5).The use of antibiotics in
NIH category III is based on the uncertain etiology and the possibility
that a potential pathogen or a cryptic non-culturable organism may be
causative (6). Combination of analgesics, alpha-blockers (tamsulosin)
antibiotics (TMP-SMX, fluoroquinolones or tetracycline), and muscle relaxants
such as diazepam coupled with prostatic massage and supportive therapy
(perineal support, pelvic floor physiotherapy, biofeedback and relaxation
therapy) has been reported to yield higher cure rate and relief of pain
and voiding symptoms compared to antibiotics alone and is the treatment
option favored by most urologists (7).
However, no highly effective therapy has
been identified. Thus far, strategies have focused on symptomatic relief
(8). In addition, it is not clear whether therapy for IIIA and IIIB prostatitis
syndromes should differ because the role of inflammation in these syndromes
is incompletely understood (6).
Transcutaneous electrical nerve stimulation
(TENS) was introduced as an alternatively therapy to pharmacological treatments
for chronic pain. TENS currently is one of the most commonly used forms
of electro analgesia. Hundreds of clinical reports exist concerning the
use of TENS for various types of conditions such as low back pain, myofascial
and arthritic pain, sympathetically mediated pain, neurogenic pain, visceral
pain, and post-surgical pain (9-12).
The widespread use of TENS is useful for
a wide range of chronic pain conditions (10,11). TENS is the application
of pulsed square wave current through surface electrodes placed on the
skin, to the peripheral nerve fibers for the control of pain (13). TENS
is a non-invasive and non-addictive treatment (13). TENS does not produce
anesthesia or nerve block (14).
Small uncontrolled studies have shown limited
improvements in scores on the NIH Chronic Prostatitis Symptom Index with
the use of biofeedback (15,16) and acupuncture (17). Physical therapies,
including prostatic massage and sitz baths, have been recommended but
have not been adequately studied.
The needs for the symptomatic management
of pain in CP/CPPS with a non-invasive, non pharmacological, non-addictive
technique such as TENS clearly exist. The purpose of the present study
was therefore to determine the efficacy of TENS in the symptomatic management
of CP/CPPS.
MATERIALS AND METHODS
Design
- In this study, a double blind randomized pre-test, post-test independent
placebo-control design was used.
Participants - The participants for this
study included 24 diagnosed CP/CPPS patients attending the Urology Department
of Murtala Mohammad Specialist Hospital (MMSH) and from private urologists.
The inclusion criteria were randomly selected men between 24-50 years,
previously diagnosed as category IIIA or IIIB CP/CPPS. Exclusion criteria
were prostate and other urogenital cancer and infection, loss of skin
sensation at and around painful area, cardiac pace maker, previous exposure
to TENS and other electro analgesia.
Instrumentation -
1. TENS generated from ENS 931 (Enraf Nonius),
Holland, with two conducting rubber electrodes and moist pads (size 3
cm X 6 cm).
2. TENS gel (Aquasonic gel) (J.J. Industry,
Seoul, Korea).
3. NIH chronic prostatitis symptom index
(NIH-CPSI) pain domain questionnaire.
Intervention - Those not on analgesic for
at least one week and had not received any form of electromagnetic/acupuncture
or heat therapy were recruited for the study. Informed consent was sought
from subjects willing to participate in accordance with the ethics of
human participation by the Ethical Committee of Murtala Mohammad Specialist
Hospital, Kano. Pre treatment pain assessment was conducted by a neutral
Assessor (Physiotherapist). NIH chronic prostatitis symptom index questionnaire,
the pain domain describing the location, frequency and severity of pain
was presented to each patient and instruction was given to indicate the
pain characteristics and level by signifying a number on the scale. Subjects
were then randomly assigned into three groups:
- X1 (TENS group): Antibiotics
+ TENS only (n = 8)
- X2 (Analgesic group): Antibiotics
+ Analgesic only (n = 8)
- X3 (Control group): Antibiotics
only + placebo tablets (n = 8)
Patients in the TENS group continued their
antibiotics (ofloxacin) as prescribed by their Physician. The rationale
for ofloxacin (300 mg t.d.s.) usage was because it is considered the recommended
drug for chronic nonbacterial prostatitis management, covering culture-negative
germs like Chlamydia (3).
For TENS application, patients were comfortably
positioned based on the painful area (to cover the perineal-suprapubic
region) for electrode placement. Sensory test was conducted on the skin
over the painful area by using two test tubes with cold and warm water,
also light touch via pin prick. It was ascertained that sensitivity of
the area was intact, and that there was no resistance, this allowed for
effective stimulation. TENS gel was applied on the surface of the electrodes
to aid maximum transmission of current. Electrodes were placed on the
skin overlying the painful area and held firmly in position as described
by Radhakrishnan and Sluka (18); Oosterhof et al. (19).
The machine was switched on; a suitable
and comfortable frequency and pulse width were selected on the stimulator
by turning the appropriate knobs. Intensity knob was turned to a level
when the patients felt a tingling or pins and needle sensation, the intensity
was then reduced to a level that the patient reported a comfortable stimulation.
Painful TENS was avoided.
Patients were stimulated with high TENS
daily for an average of 20 minutes, mean frequency, pulse width and intensity
of 100Hz, 100µs and 25mA respectively for a mean duration daily,
5 times per week for 4 consecutive weeks (average of 20 treatment sessions)
(18-21).
The analgesic group continued with their
antibiotics and analgesics (ibuprofen 400 mg b.d.); while the control
group continued with their antibiotics (ofloxacin) and placebo tablets
as prescribed by their physician for the same period. Seven days prior
to their next medical consultation, after patients felt that they had
exhausted their analgesic and TENS treatment was stopped (7 days post
treatment [wash out period]).
Outcome measures - All subjects were assessed
for the Post-treatment pain score using the same pre treatment procedure
by the same neutral assessor who had no prior knowledge of the study,
subjects’ records or groups.
Data analysis - Mean and standard deviation
(SD) were computed. Kruskal Wallis test and post hoc group differences
were computed for the pre- and post-treatment pain values. Statistical
analysis was performed on microcomputer using Statistical Package for
the Social Sciences - SPSS (Windows Version 15.0, Chicago, IL.) A probability
level of 0.05 or less was used to indicate statistical significance.
RESULTS
The
age of subjects ranged from 24 to 50 years mean ± SD (38.17 ±
8.75), 23 to 55 years (45.38 ± 11.16) and 30 to 60 years (46.83
± 8.16) for TENS (X1), Analgesic (X2) and
Control (X3) groups respectively.
The result of the present study indicated
significant effect of TENS on chronic prostatitis pain. Table-1 shows
the group mean and SD of pre and post-test pain values (levels). Table-2
shows the pretest-post-test mean, standard deviation and Kruskal Wallis
analysis. Groups pain level did not differ significantly in the pretest
pain values(X2 = 3.752 p = 0.153), while the post-test pain
values differ significantly (X2 = 18.804, p = 0.000).
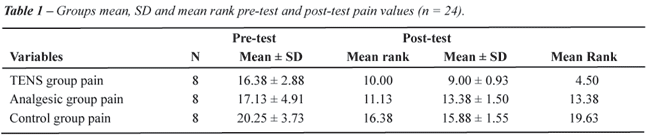
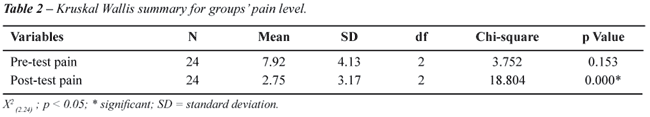
Table-3 further showed a significant effect
of TENS group over other groups at p < 0.05. Post hoc analysis indicated
significant effect of TENS over analgesic (1 & 2 [K= 3.105]), placebo
(1 & 3[K = 5.315]). Analgesic and placebo did not differ significantly
(2 & 3 [K = 2.1746]).

COMMENTS
The
purpose of the present study was to investigate the therapeutic efficacy
of TENS in the symptomatic management of chronic pain in CP/CPPS. The
result showed an appreciable effect of TENS in the symptomatic management
of chronic pain in CP/CPPS. The predominant symptom of CP/CPPS is pain.
Therefore, modalities to treat pain specifically may be effective. There
is mounting evidence that the pain of CP/CPPS may be neuropathic and associated
with central nervous system changes. The presence of central sensitization
in patients with CP/CPPS was demonstrated by Yang and colleagues (22),
who compared thermal algometry in men with CP/CPPS versus asymptomatic
controls. Men with CP/CPPS reported a higher visual analog scale to short
bursts of noxious heat stimuli to the perineum but no difference to the
anterior thigh. Thus, these patients have altered sensation in the perineum
compared with controls.
Many studies have investigated the effects
of complementary and alternative medicine (CAM) strategies in the management
of CP/CPPS. The result of the present study was in agreement with a similar
non invasive CAM therapy, reported by Capidice et al. (23). In their pilot
study, they investigated the effect of acupuncture in 10 men diagnosed
as CP/CPPS (category IIIA or IIIB). Acupuncture was applied for 30 minutes,
twice weekly for 6 weeks. They reported significant decrease in NIH-CPSI
for pain and lower urinary tract symptoms and quality of life.
Another similar study was conducted by John
and co-workers (24). Their study tested a high frequency, urethral-anal
prototype stimulation device in men with CP/CPPS twice weekly for 5 weeks.
The results demonstrated a significant decrease in the NIH-CPSI (P = 0.0002)
with no urethral, anal complaints or other side effects The authors suggest
that due to the positive results, simple technology and ability to be
self-administered, this new device may be useful in the treatment of CP/CPPS.
Two similar studies (25,26) on non pharmacological,
non invasive CAM therapy testing the value of biofeedback therapy for
CP/CPPS yielded positive results. The first study assessed 62 patients
who were refractory to conventional therapy (such as antibiotics and/or
alpha-blockers) for greater than half a year. These patients were treated
utilizing the Urostym Biofeedback equipment five times a week for 2 weeks
with a stimulus intensity of 15-23 mA and duration of 20 min. The NIH-CPSI
index noted a significant overall reduction in score (P < 0.01) and
no side effects were reported during the trial (25).
A second pilot study evaluated biofeedback
therapy in 19 men with pelvic floor tension and CP/CPPS. These results
demonstrated significant improvement in pain scores as measured by the
AUA symptom index (P = 0.001). While this study focused on testing the
effect of biofeedback therapy in treating the symptoms associated with
CP/CPPS, it also implicated the presence of pelvic floor tension contributing
to pain and the paramount importance of muscular re-education for its
treatment (26). These initial, positive biofeedback studies may warrant
larger randomized clinical trials to confirm safety and efficacy as well
as explore the mechanism of action of biofeedback therapy.
Many studies (9,11,12,27,28) have reported
significant effect of TENS on visceral pain such as labor pain and dysmenorrhea.
Based on this, TENS may be indicated in the management of chronic prostatitis
pain; a similar visceral organ. Although there is no better way of eliminating
pain than by removing its cause. With any symptomatic therapy, however,
efficacy must be weighed with the risks involved. TENS might be preferable
to large amount of analgesics and their side effects. Also, TENS is readily
available to both patients and therapists, cheaper and easy to apply compared
to other non invasive, non pharmacological complementary and alternative
medicine therapies. Based on the result of the present study, the authors
hereby concluded that TENS is an effective means of non-invasive, non
pharmacological symptomatic management of chronic prostatitis pain.
Though, the present study indicated significant
efficacy of TENS on chronic pain in CP/CPPS. However, there are some limitations
of the study; they included the non availability of data on long term
efficacy of TENS, few numbers of participants, non sham TENS group and
failure to distinguished treatment between CP/CPPS category IIIA and IIIB.
These limiting factors warrant more attention in future studies before
a conclusive statement could be made. However, the present study could
provide the relevant data in which future studies could base on.
ACKNOWLEDGMENT
The authors acknowledge the staff of the Department of Physiotherapy, Murtala Mohammed Specialist Hospital.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Bartoletti R, Mondaini N, Pavone C, Dinelli N, Prezioso D: Introduction to chronic prostatitis and chronic pelvic pain syndrome (CP/CPPS). Arch Ital Urol Androl. 2007; 79: 55-7.
- Collins MM, Stafford RS, O’Leary MP, Barry MJ: How common is prostatitis? A national survey of physician visits. J Urol. 1998; 159: 1224-8.
- Calhoun EA, McNaughton Collins M, Pontari MA, O’Leary M, Leiby BE, Landis RJ, et al.: The economic impact of chronic prostatitis. Arch Intern Med. 2004; 164: 1231-6.
- Krieger JN, Nyberg L Jr, Nickel JC: NIH consensus definition and classification of prostatitis. JAMA. 1999; 282: 236-7.
- Litwin MS, McNaughton-Collins M, Fowler FJ Jr, Nickel JC, Calhoun EA, Pontari MA, et al.: The National Institutes of Health chronic prostatitis symptom index: development and validation of a new outcome measure. Chronic Prostatitis Collaborative Research Network. J Urol. 1999; 162: 369-75.
- Gurunadha Rao Tunuguntla HS, Evans CP: Management of prostatitis. Prostate Cancer Prostatic Dis. 2002; 5: 172-9.
- Barbalias GA, Nikiforidis G, Liatsikos EN: Alpha-blockers for the treatment of chronic prostatitis in combination with antibiotics. J Urol. 1998; 159: 883-7.
- Schaeffer AJ: Clinical practice. Chronic prostatitis and the chronic pelvic pain syndrome. N Engl J Med. 2006; 355: 1690-8.
- Chao AS, Chao A, Wang TH, Chang YC, Peng HH, Chang SD, et al.: Pain relief by applying transcutaneous electrical nerve stimulation (TENS) on acupuncture points during the first stage of labor: a randomized double-blind placebo-controlled trial. Pain. 2007; 127: 214-20.
- Carroll D, Moore RA, McQuay HJ, Fairman F, Tramèr M, Leijon G: Transcutaneous electrical nerve stimulation (TENS) for chronic pain. Cochrane Database Syst Rev. 2001; (3): CD003222.
- Ying KN, While A: Pain relief in osteoarthritis and rheumatoid arthritis: TENS. Br J Community Nurs. 2007; 12: 364-71.
- Akinbo SR, Onwudimegwu WN, Ajayi GO: Evaluation of the efficacy of TENS compared with analgesics in the management of primary dysmenorrhoea. Journal of Nigeria Medical Rehabilitation Therapists. 2000; 5: 27-30.
- Akinbo SRA, Oyedele SY, Shaba OP: Transcutaneous electrical nerve stimulation (TENS) in the management of temporomandibular joint pain and dysfunction syndrome. Journal of The Nigeria Medical Rehabilitation Therapists 2003; 8: 32-5.
- Wall PD: The discovery of TENS. Physiotherapy. 1985; 71: 348-50.
- Anderson RU, Wise D, Sawyer T, Chan C: Integration of myofascial trigger point release and paradoxical relaxation training treatment of chronic pelvic pain in men. J Urol. 2005; 174: 155-60.
- Nadler RB: Bladder training biofeedback and pelvic floor myalgia. Urology. 2002; 60(Suppl 6): 42-3; discussion 44.
- Chen R, Nickel JC: Acupuncture ameliorates symptoms in men with chronic prostatitis/chronic pelvic pain syndrome. Urology. 2003; 61: 1156-9; discussion 1159.
- Radhakrishnan R, Sluka KA: Deep tissue afferents, but not cutaneous afferents, mediate transcutaneous electrical nerve stimulation-Induced antihyperalgesia. J Pain. 2005; 6: 673-80.
- Oosterhof J, De Boo TM, Oostendorp RA, Wilder-Smith OH, Crul BJ: Outcome of transcutaneous electrical nerve stimulation in chronic pain: short-term results of a double-blind, randomised, placebo-controlled trial. J Headache Pain. 2006; 7: 196-205.
- Chandran P, Sluka KA: Development of opioid tolerance with repeated transcutaneous electrical nerve stimulation administration. Pain. 2003; 102: 195-201.
- Gopalkrishnan P, Sluka KA: Effect of varying frequency, intensity, and pulse duration of transcutaneous electrical nerve stimulation on primary hyperalgesia in inflamed rats. Arch Phys Med Rehabil. 2000; 81: 984-90.
- Yang CC, Lee JC, Kromm BG, Ciol MA, Berger RE: Pain sensitization in male chronic pelvic pain syndrome: why are symptoms so difficult to treat? J Urol. 2003; 170: 823-6; discussion 826-7.
- Capodice JL, Jin Z, Bemis DL, Samadi D, Stone BA, Kapan S, Katz AE: A pilot study on acupuncture for lower urinary tract symptoms related to chronic prostatitis/chronic pelvic pain. Chin Med. 2007; 2: 1.
- John H, Rüedi C, Kötting S, Schmid DM, Fatzer M, Hauri D: A new high frequency electrostimulation device to treat chronic prostatitis. J Urol. 2003; 170: 1275-7.
- Ye ZQ, Cai D, Lan RZ, Du GH, Yuan XY, Chen Z, et al.: Biofeedback therapy for chronic pelvic pain syndrome. Asian J Androl. 2003; 5: 155-8.
- Clemens JQ, Nadler RB, Schaeffer AJ, Belani J, Albaugh J, Bushman W: Biofeedback, pelvic floor re-education, and bladder training for male chronic pelvic pain syndrome. Urology. 2000; 56: 951-5.
- American College of Obstetrician and Gynecologists Committee on Practice Bulletins -- Gynecology. ACOG Practice Bulletin No. 51. Chronic pelvic pain. Obstet Gynecol. 2004; 103: 589-605.
- Brosseau L, Yong K, Marchand S, Robinson V, Wells G, Tugwell P. Efficacy of TENS for rheumatoid arthritis:a systematic review. Physical Therapy Review. 2002; 7: 199-208.
____________________
Accepted after revision:
August 28, 2008
_______________________
Correspondence address:
Dr. Lamina Sikiru
Department of Physiotherapy/Physiology
Faculty of Medical Sciences
Jimma Specialized Hospital
Jimma University, Jimma, Ethiopia
E-mail: siklam_86@yahoo.co.uk
EDITORIAL COMMENT
Chronic
prostatitis (CP) is one of the most prevalent conditions in urology, and
represents an important international health problem. Throughout the past
century, the diagnostic entity of CP has been recognized and its clinical
characteristics well described. However, despite the multiple approaches
to management of CP, no hard and fast guidelines have been developed.
The new perception of CP/Chronic Pelvic
Pain Syndrome (CPPS) following the 1995 NIH/NIDDK workshop has emphasized
the importance of pain as the hallmark of CP/CPPS. The authors investigated
the therapeutic efficacy of transcutaneous electrical nerve stimulation
(TENS) in the symptomatic management of CP/CPPS. This placebo-control
randomized study show significant improvement in scores on the NIH-CP
pain index with the use of TENS. Based on the present study, the authors
concluded that TENS is an effective means of non-invasive, non pharmacological
symptomatic management of chronic prostatitis pain. However, we still
need more high quality multi-center randomized controlled trials from
other countries and regions.
Dr.
J. R. Yang
Department of Urology
Second Xiang-Ya Hospital
Central South University
Changsha 410011, China
E-mail: yjinrui@yahoo.com
EDITORIAL COMMENT
The
authors are to be congratulated for an innovative approach to managing
chronic pelvic pain syndrome in men, commonly referred to as chronic prostatitis.
Multiple randomized placebo-controlled trials of oral pharmaceutical agents,
including antibiotics, non-steroidal anti-inflammatory drugs, alpha blockers,
and hormone blocking agents have been unsuccessful in ameliorating chronic
pelvic pain symptoms. More local therapy is warranted. The need for symptomatic
management of chronic prostatitis/chronic pelvic pain syndrome (CPPS)
is certainly germane where no clear biological pathogenetic mechanism
has been elucidated.
This approach to pain management needs verification
with a sham treatment control. As with new surgical investigations that
is a difficult clinical trial to devise. It is a stretch to describe this
pilot trial as a double blind randomized placebo-controlled design. If
we are to believe that neural dermatomes can act as pathways for counter-irritant
stimulation that inhibits painful conception, then TENS is a good alternative.
The endurance of a positive response to TENS needs to be assessed considerably
longer than 4 weeks. Most treatment trials in chronic pelvic pain syndromes
utilize a minimum 12-week observation period to endpoint.
Fortunately TENS application lends itself
to patient controlled administration and intermittent personal selection
of usage frequency. This is a huge advantage. It is akin to utilizing
intermittent tibial nerve electrical neuromodulation for overactive bladder
symptoms. Daily stimulation may not be necessary. In general, electrical
neuromodulation applications continue to suggest avenues of pursuit that
should be encouraged.
Dr.
Rodney U. Anderson
Department of Urology
Stanford University School of Medicine
Stanford, California 94305, USA
E-mail: rua@stanford.edu