LONGITUDINAL
URETHRAL SLING WITH PREPUBIC AND RETROPUBIC FIXATION FOR MALE URINARY
INCONTINENCE
(
Download pdf )
CARLOS H. SCHAAL, RENATO P. COSTA, FERNANDO C. SALA, ANDRÉ P. VANNI, JOSÉ P. CORTEZ
Section of Urology, Amaral Carvalho Hospital, Jaú, São Paulo, Brazil
ABSTRACT
Objective:
Description and early results of a new urethral sling technique for treatment
of postprostatectomy urinary incontinence, which combines efficacy, low
cost and technical simplicity.
Materials and Methods: From May 2003 to
April 2004, 30 patients with moderate or total urinary incontinence, following
radical prostatectomy or endoscopic resection of the prostate, underwent
the new technique. The technique is based on the placement of a longitudinal-shaped
sling in the bulbar urethra, measuring 4 cm in length by 1.8 cm in width,
made of Dacron or polypropylene mesh, fixed by 4 sutures on each side,
with 2 sutures passed with Stamey-Pereira needle by retropubic approach
and 2 by prepubic approach, which are then tied over the pubis.
Pressure control was determined by interrupting the loss of infused water
through a suprapubic cystostomy 60 cm from the pubis level.
Results: Pre-operative assessment excluded
vesical instability, urethral stenosis and urinary infection. Suprapubic
cystostomy was removed when the patient was able to satisfactorily void
with urinary residue lower than 100 mL, which occurred in 29 of the 30
cases. In 2 cases, there was infection of the prosthesis, requiring its
removal. In 3 cases, there was the need to adjust the sling (increasing
the tension), due to failure of the urinary continence. Overall, 20 of
30 (66.7%) operated patients became totally continent, and did not require
any kind of pads. Four of 30 (13.3%) patients achieved partial improvement,
requiring 1 to 2 pads daily and 6 of 30 (20%) patients had minimal or
no improvement. There was no case of urethral erosion.
Conclusion: This new sling technique has
shown highly encouraging preliminary results. Its major advantage over
other surgical techniques for treatment of moderate or severe stress urinary
incontinence is the simplicity for its execution and low cost. A long-term
assessment, addressing maintenance of continence, detrusor function and
preservation of the upper urinary tract, is still needed.
Key
words: urinary incontinence; men; urinary sphincter; prostheses
and implants; surgical technique
Int Braz J Urol. 2004; 30: 307-12
INTRODUCTION
Stress
urinary incontinence (SUI) is one occasional complication following radical
prostatic surgery or transurethral resection of the prostate (TURP), however,
when it occurs, the consequences in terms of quality of life are dramatic
to patients. Urinary incontinence following radical prostate surgery has
a variable incidence, which can reach more than 30% of cases, depending
on the technique employed and the criteria for its definition (1).
When the SUI is moderate or severe, surgical
treatment is required. Among the techniques currently accepted and available
in our setting, we have injection of periurethral bulking agents, the
Silimed® periurethral constrictor (4,5), the artificial sphincter
AMS-800® and other urethral sling techniques previously described
(2). The artificial sphincter AMS-800® is considered the “gold
standard” for treatment of moderate and severe SUI, however many
patients continue with some degree of SUI and the need for surgical revision,
after 5 years, can reach up to 50% of cases (3). Urethral bulking agents
have high costs and produce quite modest results if the SUI is severe
(2,4). There are no published results to the moment concerning the use
of the periurethral constrictor Slimed®, idealized by Lima et al.
(4,5), for treatment of urinary incontinence following radical prostate
surgery, and in the authors’ experience, total continence was not
achieved or the devices had to be removed due to urethral erosion.
The urethral sling surgery for treating
urinary incontinence following radical prostate surgery was described
by Schaeffer et al. (7), using 3 segments of vascular grafts, placed transversally
to the urethra, fixed on the aponeurosis of rectus abdominis muscle, and
using the leak point pressure of 150 cm of water as a parameter. With
this technique, 56% of patients became totally continent. Several other
sling techniques were proposed, using synthetic materials, cadaveric fascia
or dermis, porcine skin collagen or autologous fascias. All techniques
used fixation on the aponeurosis of rectus abdominis muscle or on ischiopubic
rami, through bone screws (2,6-10).
The technique described here differs of
the others concerning the following aspects; it uses low-cost material
that is available at all hospitals, it does not require special training
and is based on the principle of large extension of low-pressure urethral
compression, which should improve the results and minimize the risk of
urethral erosion. Additionally, it uses a bone basis for its fixation
(the pubis), which reduces the risk of the sling’s supporting sutures
to drop over time and reduces the chance of osteitis or osteomyelitis,
since no screws are introduced in the pubis.
MATERIALS AND METHODS
From May 2003 to April 2004, 30 patients with moderate or severe SUI were operated using the described technique. 27 had urinary incontinence following radical prostate surgery and 3 had post-TURP stress urinary incontinence. Age ranged from 50 to 78 years (median 68 years) and follow-up from 2 to 12 months (median 4 months). Pre-operative assessment included urodynamic study or cystometry, cystoscopy and urine analysis in order to exclude infection. All patients had at least one year from prostate surgery and used geriatric pads or external urine collectors. Patients with urethral stenosis and patients with reduced bladder capacity or severe vesical instability were excluded.
SURGICAL TECHNIQUE
The
patient is admitted on the surgery’s day. A 16F Foley catheter is
inserted in the urethra to fill the bladder for puncture cystostomy and
for better urethral identification during dissection. An 8-cm transverse
incision is performed close to the upper pubic margin and a puncture cystostomy
is performed. The perineum is longitudinally incised, in an extension
of approximately 5 cm and the bulbar urethra is dissected, preserving
the bulbospongiosus muscle. The central perineal tendon is incised in
order to allow better contact between the bulbar urethra and the sling
and thus prevent the muscle from providing an opposing force to the sling
(8).
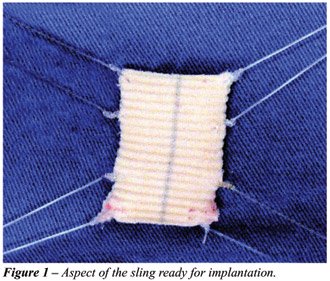
The sling is prepared using 2 superposed
segments of polypropylene or Dacron mesh, in order to assure higher steadiness,
because the suture thread can easily break if it is located too close
to the sling margin. The final size is 4 cm in length by 1.8 cm in width.
Four nylon or 0-prolene sutures are fixed to these superposed flaps, in
order to better distribute the tension (Figure-1). With a Stamey-Pereira
needle, the 2 posterior sutures are passed, parallel to the urethra and
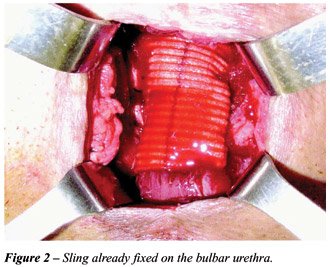
next to the pubis, by posterior approach (retropubic). The other 2 anterior
prepubic sutures are passed closed to the pubis as well, taking care so
that the spermatic cords are not included (Figures 2 and 3).

Retropubic sutures must be passed the closest
to the pubis as possible, in order to prevent bladder perforation and
to assure that soft tissues do not get interposed between the suture and
the bone, which can cause pain in the postoperative period, as well as
progressive loss of the sling tension due to tissue necrosis. After the
suture passing, a cystoscopy is performed in order to confirm that there
was no bladder perforation. First, the 4 sutures are tied over the pubis
on one side, making sure that the sling is well stretched over the urethra.
We remove the urethral catheter and, through the cystostomy, connect a
bag containing physiological saline solution at 60 cm from the pubis level.
We produce tension over the sling tying up the 4 sutures on the opposite
side, until the moment when the leakage of saline solution through the
urethra stops. The bladder is compressed to assure that the pressure was
not excessive and the patient can void. During the surgery, the surgical
field is irrigated with a saline solution containing rifamycin and gentamicin.
Perineal and abdominal incisions are closed in 2 planes. No drainage is
performed. Cystostomy is kept until the patient is able to void and has
residual urine lower than 100 mL, which usually occurs within 2 to 4 days.
Patient is discharged from hospital on the
day that follows surgery with the cystostomy closed. He is instructed
to measure postvoiding residual urine, and the cystostomy is removed when
the patient voids spontaneously, for more than 24 hours, with a residue
lower than 100 mL.
RESULTS
In
2 cases (6.6%) there was infection in the perineal incision (both patients
were diabetic) requiring the sling removal. In 1 case (3.3%), the patient
could not void after 4 weeks. We verified that the urethral leak pressure
was 55 cm of water, and the sutures were loosened to a leak pressure of
45 cm, but even then, the patient did not void. Bethanecol use was started
with a dose of 20 mg 3 times a day, with the patient starting to void
satisfactorily afterwards, with residual urine of 80 mL, when the cystostomy
was removed.
Twenty-five patients (66.6%) are continent,
with no need for pads. Four patients (14.5%) had a significant improvement,
however, with persistency of some degree of SUI, passing from use of geriatric
pads to smaller absorbent pads, in the amount of 1 to 3 units daily. Six
patients (20%), including the 2 who had the slings removed, had minimal
or no improvement. In 3 cases (10%), that are currently continent, reoperation
was required aiming to apply more tension to the sling after a period
of 30 to 90 days, due to progressive incontinence, with all becoming continent.
Four patients had previously undergone (6 months or more) placing of Marlex
sling with fixation in the ischiopubic rami, unsuccessfully. The difficulty
to dissect the urethra in these cases was slightly higher. Previous perineal
radical prostatectomy did not impair the dissection of bulbar urethra.
COMMENTS
Male
urinary incontinence, due to sphincteric insufficiency, which occurs after
prostatic endoscopic resection or radical surgery, is a highly feared
complication, for its consequences over the patient’s quality of
life. Surgical attempts to correct this picture are not recent, and in
the 70's, along with the development of the artificial sphincter, Kaufman
proposed several techniques, with discouraging long-term results (13,14).
Periurethral injections of several expansive materials showed to be effective
in cases of mild or moderate SUI only (2-4). The authors’ personal
experience with collagen (Contigem®) was also disappointing. Artificial
sphincters became the “gold standard” for treating moderate
or severe incontinence, with optimal results in 75% to 87% of cases (3,15).
However, its high cost prevents its use in great part of our population.
With the improvement in sling techniques, we started their use.
We ended up developing this technique because
we understand that, with slings fixed on the ischiopubic rami, the required
compression on the bulbar urethra often was not achieved. Cespedes &
Jacoby (8) recommend its use in cases of slight to moderate incontinence.
The lack of familiarity with bone screws, as well as the fact that such
material is not covered by the Brazilian Single Health System (SUS) prompted
the use of fixation with sutures on the pubis.
We understand that, since the sling is an
obstructive process, the detrusor muscle must be normal, and if the patient
has any co-morbidity that could cause a hypocontractile bladder, a scrupulous
urodynamic study must be performed pre-operatively.
Stenosis of urethra or bladder neck is a
relative contra-indication, because if the patient requires internal urethrotomy,
the sling would not allow the procedure to be performed, though in no
case there was impossibility to catheterize the patient with a Foley catheter.
Bladders with low capacity and/or low compliance are a relative contra-indication
(2,8,15).
Though it is not described in other techniques,
in our opinion, the use of suprapubic cystostomy is quite advantageous,
since it prevents the appearance of a potential ureteral lesion at the
sling site due to the urethral catheter, enables the easy assessment of
residual urine, and assures that the patient can empty the bladder if
urinary retention occurs within the first postoperative days.
In relation to the sling material, the use
of non-absorbable material is always recommended, since this surgery requires
that the tension on the urethra be permanently maintained (2,8,9). We
believe that synthetic materials - polypropylene, Dacron, PTTE mesh, etc
- are easy to handle and, since the pressure over the urethra is low and
largely extended, the risk of urethral erosion is minimal. The use of
aponeurosis of rectus abdominis muscle or fascia lata can be a good option
as well.
In our first cases, we used polypropylene
mesh and subsequently started to use segments of Dacron arterial graft,
due to the higher availability of this material at our institution. The
follow-up in this series is still very short, however, since results have
been encouraging, in relation to other techniques previously employed
by the authors (except for the artificial sphincter), we consider it a
very good option for patients who have no conditions to acquire the artificial
sphincter. Patients have been followed with ultrasonography of the urinary
tract, urodynamic study and questionnaire about quality of life (16),
and those will be the object of a new study when they reach a minimum
of 6 months follow-up.
CONCLUSION
The technique proposed by the authors is feasible to be performed by any urologist at any hospital in any country, with low cost. The early results are similar to other techniques described. However, urethral tolerance to the sling, detrusor function and maintenance of urinary continence need still to be assessed in the medium- and long-term.
REFERENCES
- Fowler FJ Jr, Barry MJ, Lu-Yao G, Roman A, Wasson J, Wennberg JE: Patient-reported complications and follow-up treatment after radical prostatectomy. The National Medicare experience: 1988-1990. Urology. 1993; 42: 622-9.
- John H: Bulbourethral composite suspension: A new operative technique for post-prostatectomy incontinence. J Urol. 2004; 171: 1866-70.
- Litwiller SE, Kim KB, Fone PD, White RW, Stone AR: Post-prostatectomy incontinence and the artificial urinary sphincter: a long-term study of patient satisfaction and criteria for success. J Urol. 1996; 156: 1975-80.
- Klutke JJ, Subir C, Andriole G, Klutke GG: Long-term results after antegrade collagen injection for stress urinary incontinence following radical retropubic prostatectomy. Urology. 1999; 53: 974-7.
- Vilar FO, Araujo LA, Lima SV: Periurethral constrictor in pediatric urology: long-term followup. J Urol. 2004; 171(6 Pt 2): 2626-8.
- Lima SV, Araujo LA, Vilar FO: Further experience with the periurethral expander: a new type of artificial sphincter. Br J Urol. 1997; 80: 460-2.
- Schaeffer AJ, Clemens JQ, Ferrari M, Stamey TA: The male bulbourethral sling procedure for post-radical prostatectomy incontinence. J Urol. 1998; 159: 1510-5.
- Cespedes RD, Jacoby K: Male sling for postprostatectomy incontinence. Tech Urol. 2001; 7: 176-83.
- Comiter CV: The male sling for stress urinary incontinence: a prospective study. J Urol. 2002; 167: 597-601.
- Migliari R, Pistolesi D, De Angelis M: Polypropylene sling of the bulbar urethra for post-radical prostatectomy incontinence. Eur Urol. 2003; 43: 152-7.
- Rios LAS, Tonin RT, Panhoca R, Souza OER, Fonseca Filho LL, Mattos Jr D: Male perineal sling with autologous aponeurosis and bone fixation - description of a technical modification. Int Braz J Urol. 2003; 29: 524-7.
- Madjar S, Jacoby K, Giberti C, Wald M, Halachmi S, Issaq E, et al.: Bone anchored sling for the treatment of post-prostatectomy incontinence. J Urol. 2001; 165: 72-6.
- Kaufman JJ: Surgical treatment of post prostatectomy incontinence: use of the penile crura to compress the bulbous urethra. J Urol. 1972; 107: 293-7.
- Kaufman JJ: Treatment of post-prostatectomy urinary incontinence using a silicone gel prosthesis. Br J Urol. 1973; 45: 646-53.
- Elliott DS, Barrett DM: Mayo Clinic long-term analysis of the functional durability of the AMS800 artificial urinary sphincter: a review of 323 cases. J Urol. 1998; 159: 1206-8.
- Herr HW: Quality of life of incontinent men after radical prostatectomy. J Urol. 1994; 151: 652-4.
___________________
Received: April 2, 2004
Accepted after revision: August 16, 2004
_______________________
Correspondence address:
Dr. Carlos Hermann Schaal
Rua Luiz Paiva, 100
Jaú, SP, 17210-180, Brazil.
Fax: + 55 14 3624-5155
E-mail: schaal.jau@uol.com.br
EDITORIAL COMMENT
This
work has several merits. Among them, we can include the authors’
objective and concern in developing a procedure for surgical correction
of postprostatectomy urinary incontinence that is feasible in our setting,
according to the cost of existing alternatives, whether artificial urinary
sphincter or perineal sling with bone fixation. This need becomes evident
upon the performance of 30 surgeries for this purpose in a 12-month period,
evidencing the repressed demand of this problem. These patients probably
would not have other therapeutic alternative with the exception of this
proposal.
However, before the changes described here
become indiscriminately used, some data deserve to be better evaluated.
There is no current agreement on the efficacy of male slings for treating
postprostatectomy incontinence, basically because there is no data for
interpretation (International Consultation on Incontinence, 2004). Early
works did not present comparable surgical procedures, and pre-operative
assessment and cure or improvement criteria were dubious. Technical modifications
of procedures that are not absolutely established lack, from the beginning,
a comparative term. It is evident in this series of cases that improvement
occurred in a significant group of patients (20 “continents”
patients in 30 procedures). However, this improvement criterion must be
seen with restrictions such as: postoperative follow-up of 2 to 12 months,
with median of 4 months; the lack of reference to objective characteristics
of pre-and postoperative urinary leakage; the requirement of preventive
cystostomy in all cases, with an unreported number needing to maintain
it for up to 14 days due to residual urine superior to 100 mL.
Other case series of slings with bone fixation
recently presented at the International Consultation on Incontinence,
Paris, 2004 (Abstracts # 445, 447 and 453), and also subjected to all
interpretation restrictions mentioned above, with similar results, but
with longer postoperative follow-up, even if considered insufficient,
show absence of urinary obstruction and postvoiding residual urine as
a common feature. If the main merit of the proposed procedure is the feasibility
for its performance due to lower cost, this latter feature is, currently
and beforehand, its Achilles’ heel. The authors owe us results for
minimal periods of 1 and 2 years, when we will be able to effectively
conclude about its applicability.
Dr. Homero Bruschini
Chief of Neurourology, Division of Urology
Federal University of São Paulo, UNIFESP
São Paulo, SP, Brazil