CHALLENGING
NON-TRAUMATIC POSTERIOR URETHRAL STRICTURES TREATED WITH URETHROPLASTY:
A PRELIMINARY REPORT
(
Download pdf )
NICOLAAS LUMEN, WILLEM OOSTERLINCK
Department of Urology, Ghent University Hospital, Ghent, Belgium
ABSTRACT
Introduction:
Posterior urethral strictures after prostatic radiotherapy or surgery
for benign prostatic hyperplasia (BPH) refractory to minimal invasive
procedures (dilation and/or endoscopic urethrotomy) are challenging to
treat. Published reports of alternative curative management are extremely
rare. This is a preliminary report on the treatment of these difficult
strictures by urethroplasty.
Materials and Methods: Seven cases were
treated: 4 cases occurred after open prostatectomy or transurethral resection
of the prostate for BPH, one case after external beam irradiation and
2 after brachytherapy. The 4 cases after BPH-related surgery were in fact
complete obstructions at the bladder neck and the membranous urethra with
the prostatic urethra still partially patent. Anastomotic repair by perineal
route was done in all cases with bladder neck incision in the BPH-cases
and prostatic apex resection in the radiotherapy cases.
Results: Mean follow-up was 31 months (range:
12-72 months). The operation was successful, with preserved continence,
in 3 of the 4 BPH-cases and in 2 of the 3 radiotherapy cases. An endoscopic
incision was able to treat a short re-stricture in the BPH-patient and
a longer stricture at the bulbar urethra could be managed with a perineostomy
in the radiotherapy-patient.
Conclusion: Posterior non-traumatic strictures
refractory to minimal invasive procedures (dilation/endoscopic urethrotomy)
can be treated by urethroplasty using an anastomotic repair with a bladder
neck incision if necessary.
Key
words: urethra; urethral stricture; reconstructive surgical procedures;
radiotherapy; benign prostatic hyperplasia
Int Braz J Urol. 2009; 35: 442-9
INTRODUCTION
Posterior
urethral strictures are complications that may occur after prostatic radiotherapy
or surgery for benign prostatic hyperplasia (BPH). Urethral strictures
have been reported in up to 8% after brachytherapy (1), in up to 6% after
external beam radiotherapy (2), in 2.2-9.8% after transurethral resection
of the prostate (TURP) (3) and in 1.9% after simple open prostatectomy
(4). Most of these strictures however can be treated by minimal invasive
procedures such as dilation or endoscopic urethrotomy (5,6). When these
procedures fail, reported descriptions of further management by urethroplasty
are extremely rare as only one paper on the subject could be found (7).
The incidence of non-traumatic posterior urethral strictures and the need
for urethroplasty will probably rise due to the high number of patients
undergoing TURP, radical or simple prostatectomy and due to the increasing
interest in brachytherapy and external beam radiotherapy for the treatment
of prostate cancer.
The deep location in the body, behind the
pubic bone, just above the pelvic floor and the voluntary sphincter mechanism,
and the possible involvement of the continence mechanism of the bladder
neck makes the treatment highly challenging. Therefore, we were prompted
to report our experience in this field.
MATERIAL AND METHODS
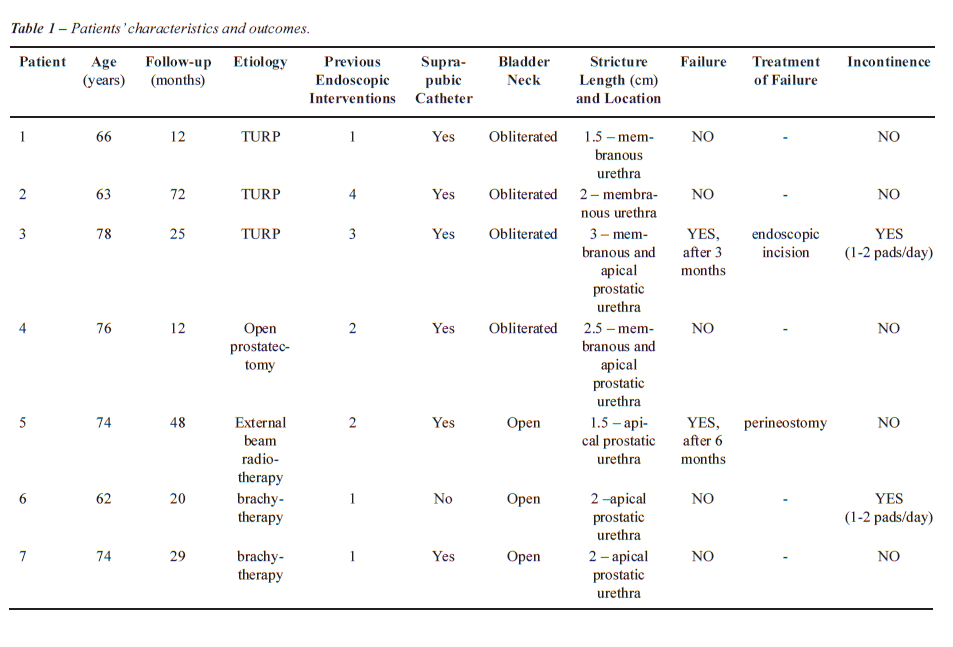
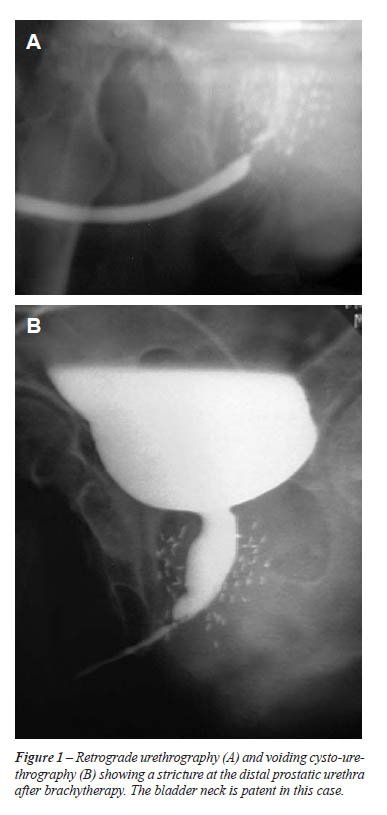
Between 2001 and 2007, seven cases of non-traumatic posterior urethral strictures were treated by urethroplasty (Table-1). These cases were identified using a prospectively collected database. Mean age was 70.4 years (range: 62-78 years). Before referral to our centre, endoscopic incision had been attempted in all cases. In 4 cases, the procedure had to be stopped due to a false routing. In the other cases recurrence occurred almost immediately. Endoscopic incision was repeated in 2 patients and one was dilated regularly. The strictures were the consequence of open prostatectomy (Millin-technique) for BPH in one patient and transurethral resection of the prostate (TURP) in the 3 others. All these 4 BPH-patients were unable to void immediately after their BPH-surgery for at least 2 weeks. Two patients received brachytherapy and one external irradiation for localized prostate cancer. In all patients, a retrograde urethrography combined with a cysto-urethrography was done to assess the location and length of the stricture and the condition of the bladder neck. In the BPH-cases, retrograde urethrography revealed a complete obstruction at the membranous urethra and on trial to void, the bladder neck remained closed. In these cases, a suprapubic cystoscopy revealed a completely strictured bladder neck. In the irradiated cases the bladder neck was still patent but the prostatic urethra was partially obstructed (Figure-1). Six out of 7 patients had a suprapubic catheter: all BPH-patients and 2 irradiated patients.
Operative Technique
Antibiotics
(fluoroquinolones) were started 24 hours prior to surgery and continued
for three days. In cases of infected urine, antibiotics were given based
on the results of the urine culture. The patient was placed in the high
lithotomy position. All patients were operated by a midline perineal incision
and by that route alone. The bulbospongiosum muscle was dissected away
from the corpus spongiosum. The bulbar urethra was circumferentially dissected
from the ventral aspect of the corpora cavernosa from the penoscrotal
angle until its passage through the pelvic floor. The bulbus was attracted
and the urethra was further dissected through the pelvic floor. The fibrotic
column of the strictured membranous urethra is followed as far as possible.
A large Beniqué sound (26F) was introduced inside the urethra and
marked the distal level of the defect. The urethra was transected at this
level. The transected distal part of the urethra is spatulated after removal
of all fibrosis. The residual fibrosis at the proximal (prostatic) end
of the urethra is then removed layer by layer with curved scissors until
the open, healthy urethra was reached. In the 4 BPH-cases in which a bladder
neck stricture was present, a resectoscope was introduced in the prostatic
urethra and the bladder neck incised. In the 3 radiotherapy or brachytherapy
cases, the apex of the prostate was partially resected during this procedure.
A spatulated end-to-end anastomosis was made with 8 interrupted polyglycolic
sutures 3x0 sutures between the prostatic urethra and the proximal bulbar
urethra. In cases of a rather short defect, mobilization of the urethra
up to the penoscrotal angle was sufficient to elongate the urethra by
its elasticity to bridge the gap without any tension. Cleavage of the
corporal bodies was performed to gain extra length in 2 (radiotherapy)
cases. A urethral catheter (18F) was left indwelling for two weeks. After
this period, a voiding cysto-urethrography was performed. In cases of
extravasation at the anastomosis-site, the catheter was reinserted and
a new voiding cysto-urethrography was carried-out one week later. The
catheter was maintained until extravasation was no longer visible. Extensive
description of the technique has been previously described (8).
Follow-up with history taking, clinical
examination, uroflowmetry and echographic residual urine measurement was
done every three months during the first year and annually thereafter.
In cases of suspected recurrence, a retrograde urethrography and cystoscopy
was done.
Success was defined as spontaneous voiding,
no significant residual urine and no complaints after one single reconstructive
procedure. Incontinence was defined as the need of at least one protection
pad a day.
RESULTS
Mean
follow-up was 31 months (range: 12-72 months). Mean stricture length was
2.1 cm (range: 1.5-3 cm). Mean operation time was 130 min (range: 110-145
min). Two weeks after urethroplasty, voiding cysto-urethrography showed
a patent urethra without extravasation in all BPH cases (4/4) and one
radiotherapy patient (1/3). In the remaining 2 irradiated patients, the
catheter was left indwelling for 3 and 6 weeks respectively due to persistent
extravasation at the anastomosis. After final removal of the urethral
catheter, all patients could urinate well. Three BPH-patients (3/4) have
remained excellent until present. One BPH-patient developed a short recurrence
3 months after the operation at the level of the anastomosis and at the
bladder neck. This was treated by endoscopic incision and solved the problem,
for up to 23 months. The patient suffered from slight stress incontinence
after the endoscopic procedure but remains very pleased with the final
result.
The patient who was irradiated externally
developed a stricture of 3 cm length at the bulbar urethra 6 months after
urethroplasty. He was treated by a first stage Johansson procedure. Four
years later, the patient is still voiding well through his perineostomy
and for this reason he has refused the second stage of a Johansson procedure.
The two patients who received brachytherapy
have a suboptimal urinary flow (Qmax of only 10 mL/sec) but are very pleased
with their results. One patient also suffered from slight stress incontinence.
Summarizing these results, success- and continence-rates are 71.4% (5/7).Currently,
all patients have no suprapubic catheter.
COMMENTS
Although the urological department of the Ghent University Hospital has been a reference centre in the BENELUX (Belgium, the Netherlands and Luxembourg) for urethral stricture repair since 1980, our first case of non-traumatic posterior urethral stricture was only seen in 2001. This illustrates the rarity of the need for urethroplasty for this disease. A recent study regarding the incidence of urethral strictures after interventions for curative treatment of prostatic cancer has demonstrated that the incidence is perhaps much higher but the extent of the stricture is such that it can be managed either with endoscopic incision or even without further treatment (7).
Strictures after Prostate Operation for BPH
Our
initial experience has shown us that after prostatectomy/TURP for BPH
the prostatic urethra itself is still partially patent with the bladder
neck and membranous urethra completely obstructed. Therefore, these strictures
cannot be placed into the classification proposed by Pansodoro and Emiliozzi
(6). These authors propose a trial of endoscopic incision of iatrogenic
prostatic urethral strictures with reasonable results, but in all of their
patients the prostatic urethra was narrowed, but not completely obstructed
(6). Reports of endoscopic treatment of complete obliteration of the posterior
urethra are very scarce and show disappointing results (9). Endoscopic
treatment of these obstructions had been tried in all patients, without
any success. In view of the complete obstruction, it seems to us that
endoscopic treatment is not a good option in these patients (10). In patient
3, the prostatic urethra was open for only about 1 cm with a dense and
long fibrosis also at the bladder neck. This patient also did worse after
our reconstruction. He had a recurrent stricture at the membranous urethra
and the bladder neck, which needed an endoscopic incision. Our hypothesis
of posterior urethral stricture formation was similar in all these 4 patients.
They had an overdistended bladder before prostatectomy/TURP and could
not urinate at removal of the urethral catheter after the intervention.
A suprapubic catheter was placed to give them the opportunity to try micturition
and guarantee emptying of the bladder. In all patients spontaneous micturition
remained absent during at least two weeks.
However, immediately after prostatectomy/TURP
the wound edges at the bladder neck and membranous urethra must form new
urethral mucosa to cover the operated prostatic urethra. With spontaneous
micturition, blood clots and fibrin are washed away after operation. It
is our hypothesis that during a prolonged period of post-operative absent
micturition, the accumulation of blood clots and fibrin at the wound edges
leads to fibrosis and finally stricture formation at the bladder neck
and membranous urethra with an open prostatic urethra between them, because
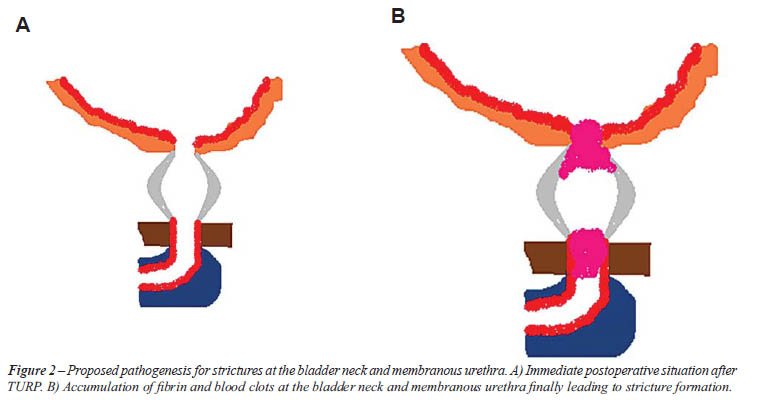
the lumen is much larger at this level (Figure-2). Probably, it would
have been better to leave the urethral catheter indwelling for a few weeks
instead of a suprapubic catheter or to perform intermittent self-catheterization.
Unfortunately, we have no histological or urodynamic data to prove this
hypothesis, therefore the hypothesis can only be considered as an assumption.
Pansadoro and Emiliozzi (6) have proposed a somewhat different pathogenesis
of prostatic urethral strictures: strictures occur when delay of epithelialization
is combined with overgrowth of fibrotic tissue.
It is possible that transurethral ultrasound
can demonstrate the open prostatic urethra. This examination was not performed
because we realized this possibility only after the experience.
Strictures after Radiotherapy
vIn
all referred patients, the prostatic urethra was only partially obstructed
and the bladder neck was found to be patent. The operative challenge was
not greater then in any other end-to-end anastomosis in that region, for
example for urethral rupture after pelvic trauma. The intervention could
have been done completely by the perineal route. In the cases after brachytherapy,
the anastomosis was made after resection of the apex of the prostate with
removal of several radioactive seeds.
Ideally, the anastomosis should be made
between two well vascularized ends. This was not the case because the
prostate was fibrotic as far as we could feel, probably due to vascular
damage after the irradiation (1).
The anastomosis was made of fibrotic prostatic
tissue at one side, but by a well vascularized stump of bulbar urethra
at the other side. Obviously one well vascularized side at the anastomotic
site can be sufficient for wound healing, although it can take considerably
longer than in the non-irradiated cases. This is suggested by the observation
that two out of three radiotherapy patients needed a prolonged urethral
catheter because of persistent extravasation. In these cases, the urethra
was also extensively mobilized and the corpora cavernosa cleaved to shorten
the distance, so that the tension free anastomosis was guaranteed.
Continence Mechanism
It
is believed that after prostatectomy or TURP continence relies only on
the external sphincter (11). Anastomotic urethroplasty at the level of
the membranous urethra usually destroys the external sphincter mechanism,
as observed after repair of post-traumatic posterior urethral strictures
(12). Taking this into account, all BPH-patients would be expected to
be incontinent after urethroplasty. In fact, all patients were continent
after the anastomotic repair at the membranous urethra. The bladder neck
still was able to work sufficiently, even after its incision. This was
done very prudently, necessitating a re-intervention of incision in one
patient. Unfortunately, he became slightly stress incontinent after the
second procedure. The competence of the bladder neck can be judged on
a cysto-urethrography: the bladder neck should be closed following this
examination. Unfortunately, this examination was not performed routinely
in all cases. Therefore, our statement remains an assumption. However,
a recent paper by Whitson et al. (13) still reports a significant contribution
of the external sphincter after anastomotic urethroplasty at the membranous
urethra. Obviously, the final continence mechanism in these complex cases
still is uncertain and a matter of debate for which further research is
needed. Moreover, patients should be warned about the possibility of incontinence
after the procedure.
Non-traumatic posterior urethral strictures,
refractory to endoscopic treatment are often managed by techniques that
abandon the urethral outlet such as a definitive suprapubic catheter or
a continent stoma (14,15). Five out of seven patients in this series could
void after urethroplasty and with one additional procedure, all patients
arrived at a reasonable solution without need for catheterization. Two
brachytherapy patients had a suboptimal uroflowmetry (< 10mL/s) after
the procedure without any evidence (urethrography and urethroscopy) of
recurrence. This suboptimal flow can be explained by a fibrotic obstructive
irradiated prostate at its entire length even if the diameter appears
to be sufficient. These patients however were subjectively very satisfied
with the result.
Although we are aware of the limitations
of this study (small numbers, heterogenic population), our data suggest
that even for these very challenging patients voiding can be made possible
again with end-to-end urethroplasty and if necessary in combination with
bladder neck incision.
A search on PubMed over the past 10 years revealed only one series on
posterior urethral stricture repair after radiotherapy (7). They described
seven cases of posterior urethral stenosis of which three underwent an
anastomotic urethroplasty and four the placement of a urethral stent.
All three anastomotic repairs were successful. Urethral stents failed
twice out of four repairs with urethral stenosis recurring at either end
of the stent. In spite of these worse results with stents, these authors
still see this as a possible choice in their therapeutic algorithm. They
also described a small series of posterior urethral strictures after radical
prostatectomy, which is a situation clearly different from the one where
the prostate is still in place. Therefore, at date of publication, to
our knowledge this is the largest reported series describing urethroplasty
for non-traumatic posterior urethral strictures.
With a normal functioning bladder still
in place, it is possible to directly to a continent stoma of the bladder
(14,15). This option remains open after failed urethroplasty. All our
patients were warned that success was far from guaranteed and eventually
other interventions could be necessary to solve their problem. They all
accepted the risk and considered a continent catheterizable stoma a second
choice.
CONCLUSION
Urethroplasty,
using an anastomotic repair in combination with a bladder neck incision,
if necessary, provides good results. This salvage urethroplasty can preserve
continence in most of the cases.
This operation can be done by perineal approach alone and is not more
demanding than an anastomotic repair after urethral rupture in pelvic
fractures.
Nevertheless, these conclusions are based
on a small number of cases and it would be dangerous to generalize about
them. They can offer, however, some inspiration for colleagues with similar
unusual and difficult cases.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Sullivan L, Williams SG, Tai KH, Foroudi F, Cleeve L, Duchesne GM: Urethral stricture following high dose rate brachytherapy for prostate cancer. Radiother Oncol. 2009; 91: 232-6.
- Fonteyne V, Villeirs G, Lumen N, De Meerleer G: Urinary toxicity after high dose intensity modulated radiotherapy as primary therapy for prostate cancer. Radiother Oncol. 2009; 6. [Epub ahead of print]
- Rassweiler J, Teber D, Kuntz R, Hofmann R: Complications of transurethral resection of the prostate (TURP)--incidence, management, and prevention. Eur Urol. 2006; 50: 969-79; discussion 980.
- Varkarakis I, Kyriakakis Z, Delis A, Protogerou V, Deliveliotis C: Long-term results of open transvesical prostatectomy from a contemporary series of patients. Urology. 2004; 64: 306-10.
- Santucci RA, McAninch JW: Urethral reconstruction of strictures resulting from treatment of benign prostatic hypertrophy and prostate cancer. Urol Clin North Am. 2002; 29: 417-27.
- Pansadoro V, Emiliozzi P: Iatrogenic prostatic urethral strictures: classification and endoscopic treatment. Urology. 1999; 53: 784-9.
- Elliott SP, McAninch JW, Chi T, Doyle SM, Master VA: Management of severe urethral complications of prostate cancer therapy. J Urol. 2006; 176: 2508-13.
- Oosterlinck W, Lumen N, Van Cauwenberghe G: Surgical treatment of urethral stenoses: technical aspects. Ann Urol (Paris). 2007; 41: 173-207.
- Neikov K, Panchev P, Kirilov S: Endoscopic treatment of complete obliteration of posterior urethra. Khirurgiia (Sofiia). 2001; 57: 38-40.
- Oosterlinck W, Lumen N: Endoscopic treatment of urethral strictures. Ann Urol (Paris). 2006; 40: 255-66.
- Strasser H, Frauscher F, Helweg G, Colleselli K, Reissigl A, Bartsch G: Transurethral ultrasound: evaluation of anatomy and function of the rhabdosphincter of the male urethra. J Urol. 1998; 159: 100-4; discussion 104-5.
- Koraitim MM, Atta MA, Fattah GA, Ismail HR: Mechanism of continence after repair of post-traumatic posterior urethral strictures. Urology. 2003; 61: 287-90.
- Whitson JM, McAninch JW, Tanagho EA, Metro MJ, Rahman NU: Mechanism of continence after repair of posterior urethral disruption: evidence of rhabdosphincter activity. J Urol. 2008; 179: 1035-9.
- Moreira SG Jr, Seigne JD, Ordorica RC, Marcet J, Pow-Sang JM, Lockhart JL: Devastating complications after brachytherapy in the treatment of prostate adenocarcinoma. BJU Int. 2004; 93: 31-5.
- Ullrich NF, Wessells H: A technique of bladder neck closure combining prostatectomy and intestinal interposition for unsalvageable urethral disease. J Urol. 2002; 167: 634-6.
____________________
Accepted
after revision:
May 18, 2009
_______________________
Correspondence
address:
Dr. N. Lumen
Department of Urology
Ghent University Hospital
De Pintelaan 185
9000, Ghent, Belgium
E-mail: nicolaas.lumen@ugent.be