THE
EFFECT OF KIDNEY MORCELLATION ON OPERATIVE TIME, INCISION COMPLICATIONS,
AND POSTOPERATIVE ANALGESIA AFTER LAPAROSCOPIC NEPHRECTOMY
(
Download pdf )
AFFONSO H. CAMARGO, JONATHAN N. RUBENSTEIN, BRENT D. ERSHOFF, MAXWELL V. MENG, CHRISTOPHER J. KANE, MARSHALL L. STOLLER
Department of Urology, University of California San Francisco, San Francisco, California, USA
ABSTRACT
Introduction:
Compare the outcomes between kidney morcellation and two types of open
specimen extraction incisions, several covariates need to be taken into
consideration that have not yet been studied.
Materials and Methods: We retrospectively
reviewed 153 consecutive patients who underwent laparoscopic nephrectomy
at our institution, 107 who underwent specimen morcellation and 46 with
intact specimen removal, either those with connected port sites with a
muscle-cutting incision and those with a remote, muscle-splitting incision.
Operative time, postoperative analgesia requirements, and incisional complications
were evaluated using univariate and multivariate analysis, comparing variables
such as patient age, gender, body mass index (BMI), laterality, benign
versus cancerous renal conditions, estimated blood loss, specimen weight,
overall complications, and length of stay.
Results: There was no significant difference
for operative time between the 2 treatment groups (p = 0.65). Incision
related complications occurred in 2 patients (4.4%) from the intact specimen
group but none in the morcellation group (p = 0.03). Overall narcotic
requirement was lower in patients with morcellated (41 mg) compared to
intact specimen retrieval (66 mg) on univariate (p = 0.03) and multivariate
analysis (p = 0.049). Upon further stratification, however, there was
no significant difference in mean narcotic requirement between the morcellation
and muscle-splitting incision subgroup (p = 0.14).
Conclusion: Morcellation does not extend
operative time, and is associated with significantly less postoperative
pain compared to intact specimen retrieval overall, although this is not
statistically significant if a remote, muscle-splitting incision is made.
Morcellation markedly reduces the risk of incisional-related complications.
Key
words: nephrectomy; laparoscopy; pain
Int Braz J Urol. 2006; 32: 273-80
INTRODUCTION
Since
its first report in 1991 (1), laparoscopic nephrectomy has progressively
gained acceptance among urologists (2-5). Steps within this procedure
are continuously being evaluated and modified to achieve better outcomes.
Although a variety of techniques and devices have been developed for specimen
entrapment and retrieval (6,7), no consensus on the best method has been
established, but rather the choice is likely surgeon dependent or unproved
factors. Specimen morcellation is associated with a smaller incision,
better cosmesis, and fewer incision-related complications than open specimen
extraction incisions (8,9), but is associated with a longer operative
time with a controversial benefit in regard to pain control. Morcellating
a specimen containing tumor is felt to make accurate pathologic staging
more difficult, but this has not yet been proved to be clinically detrimental
due to the development of better clinical staging due to higher resolution
imaging tests (10,11), and the application of nomograms and standardized
protocols for pathologic evaluation of fragmented specimens (12). The
potential increased risk of tumor spill and port-site metastasis after
morcellation has yet to be proven clinically significant (13,14).
Previous studies evaluating the effects
of tissue morcellation on morbidity and life quality have not shown a
statistically significant difference regarding postoperative pain, hospital
stay and recovery period when compared to intact specimen removal (15,16).
Unfortunately, these studies did not take into consideration other variables
that could potentially affect the relationship between morcellation and
operative time and post-operative pain, such as age, sex, body mass index,
benign versus malignant renal conditions and overall complications. Our
objective was to more accurately assess and compare the operative time,
analgesia requirements, incision related complications, and overall length
of stay in patients with morcellated and intact specimen extraction by
entering additional variables into the analysis.
MATERIALS AND METHODS
We
retrospectively reviewed the charts of 153 consecutive patients who underwent
transperitoneal, 4-port laparoscopic nephrectomy for benign or malignant
disease at our institution from September 1999 through June 2004. Our
technique for laparoscopic nephrectomy with the use of a blunt-tip, radial
dilating trocar (Step®, US Surgical, Norwalk, CT) for all ports was
published previously (17). We routinely infiltrated the peritoneum under
the laparoscopic port site with 3 mL of 0.25% bupivacaine and the extraction
incision (when used) with 10 mL of 0.25% bupivacaine. Patients who underwent
hand-assisted nephrectomy, nephroureterectomy, donor nephrectomy, and
cases requiring open conversion were excluded from the study. All specimens
were placed within a medium or large size LapSac (Cook Urological, Spencer,
IN) prior to specimen retrieval. All specimens could be placed within
a medium or large LapSac.
In 107 patients the kidney specimen was
morcellated, while 46 patients underwent intact specimen removal, either
through a muscle-cutting incision connecting two port sites (n = 16) or
through a remote, muscle-splitting incision, either midline infra-umbilical
or Pfannestiel incision (n = 30). For morcellated specimens, the mouth
of the LapSac was pulled up through a port site that previously had a
12-mm port, and ring forceps were used to extract pieces of the tissue
until all was removed. For the open extractions, after making the incision
into the peritoneum, the LapSac was grasped and removed with the specimen
intact. The choice to morcellate or not and the type of incision chosen
was made by the primary surgeon either at the time of surgery or in discussion
with the patient preoperatively, and generally was based upon prior incisions
and personal cosmetic concerns and not necessarily based upon kidney size
or underlying pathology.
Operative times, analgesia requirements
(morphine equivalents administered during the postoperative period), length
of hospital stay, and postoperative complications (incision and non-incision
related) were evaluated and compared to a number of variables, including
age, gender, body mass index, type of renal pathology (malignant versus
benign), estimated blood loss and specimen weight. The dosage of narcotics
required during the postoperative hospital stay was converted to morphine
sulfate equivalents using of an equianalgesic table (18). Univariate analysis
and multivariate regression were performed for statistical evaluation
and significance was defined as a p value ≤ 0.05.
RESULTS
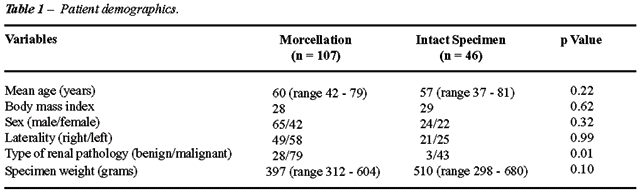
Patient
demographics are presented in Table-1. There was no significant difference
in patient age, sex, and laterality. There was a significant difference
in the type of renal pathology, as 28 of 107 (26%) patients who underwent
kidney morcellation had a benign pathology compared to only 3 of 46 (6.5%)
within the intact specimen group (p = 0.01). The benign pathology consisted
of patients with xanthogranulomatous pyelonephritis, chronic pyelonephritis,
ureteropelvic junction obstruction, severe renal artery stenosis, and
kidney tuberculosis. Patients undergoing radical nephrectomy whose final
pathology were oncocytoma or angiomyolipoma were considered pre-operatively
to have a potentially malignant disease and were therefore included in
the cancer group.
The results of the univariate analysis are
shown in Table-2. There was no significant difference between the mean
operative time of the morcellation group (255 min) and the intact specimen
group (247 min) (p = 0.65). No additional variables were significantly
correlated to operative time, and thus a multivariate model was unnecessary.
The postoperative length of stay was similar between the two groups: 2.1
and 2.3 days in the morcellated and non-morcellated groups respectively
(p = 0.53).

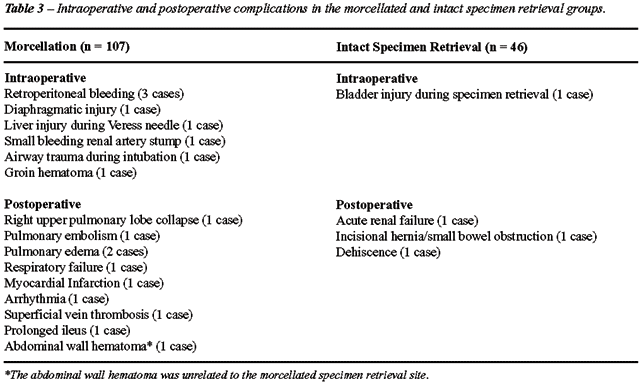
The complications are listed in Table-3.
The purpose of the list of complications is to determine the potential
effect of a surgical complication on operative time, length of stay, and
analgesia requirement. There were 18 complications in the morcellated
group and 4 in the intact group. Detailed analysis revealed that the complications
were completely unrelated to the incision in all cases except for 2 (4.4%)
In contrast, there were no complications related to the specimen retrieval
site in the morcellated group (0%; p = 0.03).
Univariate analysis indicated the mean narcotic
requirement differed between the treatment groups (41 and 66 mg in the
morcellated and non-morcellated patients, respectively, p = 0.03). Regression
revealed that age and length of stay were correlated with postoperative
analgesia, with a higher average narcotic requirement associated with
younger patients and a longer hospital stay. Multivariate analysis demonstrated
that the effect of morcellation on postoperative analgesia remained significant
between the treatment groups while controlling for significant covariates
(p = 0.049). After stratification of the intact specimen group, no significant
difference in the average narcotic requirement was found between the muscle
cutting (79 mg) and muscle-splitting incision (61 mg) subgroups (p = 0.60).
The two subgroups were individually compared with the morcellated specimen
group. Analysis revealed a difference in postoperative analgesia between
the morcellated group and the muscle cutting subgroup (p = 0.046 and p
= 0.05 for univariate and multivariate, respectively), however, no significant
difference was found between morcellation and the muscle splitting patients
(p = 0.06 and p = 0.14 for univariate and multivariate analysis, respectively).
DISCUSSION
The
introduction of laparoscopic nephrectomy and kidney morcellation in 1991
(1) was responsible for a substantial reduction in postoperative pain,
hospital stay, and for a shorter recovery period compared to standard
nephrectomy (5,6). Although the advantages of laparoscopic nephrectomy
are widely recognized, the ideal method for specimen removal is ill defined.
It remains controversial as to the true effect that specimen morcellation
has on operative time, postoperative pain, and the accuracy of malignancy
staging through pathologic evaluation (15,16).
It has been argued that morcellation should
not be undertaken in cases of nephrectomy for cancer as this inhibits
accurate tumor staging. While traditional staging can clearly not be performed
in a morcellated specimen, the clinical effect of this is unknown. An
in vitro study on pathological validity of morcellated kidneys affected
by renal tumors, including cases of perinephric fat invasion, revealed
identical histology, grade, and stage when intact specimen evaluations
were compared to a second analysis of the same specimens after morcellation
(19). Additionally, advances in abdominal imaging tests (10,11), and mathematical
models developed to guide pathologic sampling and analysis of morcellated
specimens (12) can substantially increase the reliability of diagnosis
and staging of renal malignancies.
In regards to operative time, as shown by
previous studies and confirmed by our analysis (15,16), morcellation following
laparoscopic nephrectomy is not associated with longer operative times
when compared to intact specimen retrieval. While morcellation may be
a time consuming procedure, especially in patients with history of recurrent
urinary tract infections, xanthogranulomatous pyelonephritis, and/or renal
scarring, this is clearly offset by the time required to open and close
an additional incision. Additionally, conditions such as obesity and inadvertent
injury of subcutaneous vessels during an incision may account for even
longer operative times. In addition, many of the patients in the morcellated
group underwent nephrectomy for xanthogranulomatous pyelonephritis, chronic
pyelonephritis, tuberculosis, and other end-stage kidney disorders, which
caused the kidneys to have a severe scar around them, making surgery much
more difficult and time consuming.
While the overall length of hospital stay
was not statistically significantly different between the two groups,
this was true despite the higher number of complications in the morcellated
group that certainly led to longer hospital stays. This difference in
complication rate in this review probably has a number of explanations
including random chance. Certainly, the complex nature of many of the
kidneys removed for non-cancerous causes, which compromised 36% of the
morcellated group, could have contributed to the difference in complication
rate. The only two incision-related complications were in the intact group.
Recent publications failed to prove the
benefits of morcellation regarding postoperative pain intensity (15,16).
However, these studies did not consider the possible effects of other
variables on postoperative pain. In our study, patient age and length
of stay were strongly correlated to postoperative pain. To generate a
nonbiased assessment of the effect of morcellation on narcotic requirement,
we used a multivariate regression model. Analysis revealed that older
patients required lower dosages of morphine for postoperative pain control.
This fact is consistent with a number of studies that demonstrated an
increased pain threshold in the elderly patients that is felt to be due
to a variety of physiologic changes (20).
For further analysis, we divided the intact
specimen retrieval group into those who underwent a muscle cutting (i.e.
connecting two ports) compared to muscle splitting (i.e. Pfannenstiel,
low midline, or Gibson-type) incision. When comparing the two subgroups
of intact incisions, there was no significant difference between the narcotic
requirements. When comparing the narcotic requirements of each subgroup
separately to that of the morcellated group, while there was a statistically
significant difference between the muscle cutting group and the morcellated
group, this was not significantly different in the muscle splitting group.
It seems likely therefore that postoperative pain following laparoscopic
nephrectomy may not be influenced by a single variable but more likely
by a combination of retrieval incision location and length.
A potential weakness of the study is the
retrospective nature of the review. Therefore, certain information that
could further give insight to better outcomes, such as the change in surgical
and laparoscopic experience over time, an actual accurate measurement
of incision length, true analog pain scale results, and accurate time
to return to daily activities could not be entirely assessed and for this
reason were not included. A prospective randomized trial with multivariate
statistical analysis is mandatory to help even better define these conclusions.
CONCLUSIONS
Kidney morcellation after laparoscopic nephrectomy does not extend operative time and is associated with a lower rate of incision-related complications. Patients who underwent kidney morcellation had a significantly lower postoperative narcotic requirement when compared to those in the intact specimen retrieval group. However, the difference in the mean analgesia requirement was not statistically significant between the morcellated group and those with a remote, muscle-splitting incision. Postoperative analgesia is likely influenced by a combination of factors.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Clayman RV, Kavoussi LR, Soper NJ, Dierks SM, Meretyk S, Darcy MD, et al.: Laparoscopic nephrectomy: initial case report. J Urol. 1991; 146: 278-82.
- Cadeddu JA, Ono Y, Clayman RV, Barrett PH, Janetschek G, Fentie DD, et al.: Laparoscopic nephrectomy for renal cell cancer: evaluation of efficacy and safety: a multicenter experience. Urology. 1998; 52: 773-7.
- Portis AJ, Yan Y, Landman J, Chen C, Barrett PH, Fentie DD, et al.: Long-term followup after laparoscopic radical nephrectomy. J Urol. 2002; 167: 1257-62.
- Shuford MD, McDougall EM, Chang SS, LaFleur BJ, Smith JA Jr, Cookson MS: Complications of contemporary radical nephrectomy: comparison of open vs. laparoscopic approach. Urol Oncol. 2004; 22: 121-6.
- Fornara P, Zacharias M, Steinacker M, Doehn C, Jocham D: Laparoscopic vs. open nephrectomy. 10 years’ results of a nonrandomized comparative study of 549 patients with benign kidney diseases. Urologe A. 2003; 42: 197-204.
- Sundaram CP, Ono Y, Landman J, Rehman J, Clayman RV: Hydrophilic guide wire technique to facilitate organ entrapment using a laparoscopic sack during laparoscopy. J Urol. 2002; 167: 1376-7.
- Pautler SE, Harrington FS, McWilliams GW, Walther MM: A novel laparoscopic specimen entrapment device to facilitate morcellation of large renal tumors. Urology. 2002; 59: 591-3.
- Shalhav AL, Leibovitch I, Lev R, Hoenig DM, Ramon J: Is laparoscopic radical nephrectomy with specimen morcellation acceptable cancer surgery? J Endourol. 1998; 12: 255-7.
- Elashry OM, Giusti G, Nadler RB, McDougall EM, Clayman RV: Incisional hernia after laparoscopic nephrectomy with intact specimen removal: caveat emptor. J Urol. 1997; 158: 363-9.
- Hallscheidt PJ, Bock M, Riedasch G, Zuna I, Schoenberg SO, Autschbach F, et al.: Diagnostic accuracy of staging renal cell carcinomas using multidetector-row computed tomography and magnetic resonance imaging: a prospective study with histopathologic correlation. J Comput Assist Tomogr. 2004; 28: 333-9.
- Ergen FB, Hussain HK, Caoili EM, Korobkin M, Carlos RC, Weadock WJ, et al.: MRI for preoperative staging of renal cell carcinoma using the 1997 TNM classification: comparison with surgical and pathologic staging. AJR Am J Roentgenol. 2004; 182: 217-25.
- Meng MV, Koppie TM, Stoller ML: Pathologic sampling of laparoscopically morcellated kidneys: a mathematical model. J Endourol. 2003;17: 229-33.
- Fentie DD, Barrett PH, Taranger LA: Metastatic renal cell cancer after laparoscopic radical nephrectomy: long-term follow-up. J Endourol. 2000; 14: 407-11.
- Castilho LN, Fugita OE, Mitre AI, Arap S: Port site tumor recurrences of renal cell carcinoma after videolaparoscopic radical nephrectomy. J Urol. 2001; 165: 519.
- Gettman MT, Napper C, Corwin TS, Cadeddu JA: Laparoscopic radical nephrectomy: prospective assessment of impact of intact versus fragmented specimen removal on postoperative quality of life. J Endourol. 2002; 16: 23-6.
- Hernandez F, Rha KH, Pinto PA, Kim FJ, Klicos N, Chan TY, et al.: Laparoscopic nephrectomy: assessment of morcellation versus intact specimen extraction on postoperative status. J Urol. 2003; 170: 412-5.
- Shekarriz B, Gholami SS, Rudnick DM, Duh QY, Stoller ML: Radially expanding laparoscopic access for renal/adrenal surgery. Urology. 2001; 58: 683-7.
- Pereira J, Lawlor P, Vigano A, Dorgan M, Bruera E: Equianalgesic dose ratios for opioids. a critical review and proposals for long-term dosing. J Pain Symptom Manage. 2001; 22: 672-87.
- Landman J, Lento P, Hassen W, Unger P, Waterhouse R: Feasibility of pathological evaluation of morcellated kidneys after radical nephrectomy. J Urol. 2000; 164: 2086-9.
- Gibson SJ, Farrell M: A review of age differences in the neurophysiology of nociception and the perceptual experience of pain. Clin J Pain. 2004; 20: 227-39.
____________________
Accepted
after revision:
March 30, 2006
_______________________
Correspondence address:
Dr. Marshall L. Stoller
Professor, Department of Urology
University of California, San Francisco
400 Parnassus Ave, Box 0718
San Francisco, 94143, CA, USA
Fax: + 415 353-2200
E-mail: mstoller@urol.ucsf.edu
EDITORIAL COMMENT
The
present study approaches the fairly controversial area of specimen morcellation
after laparoscopic nephrectomy, especially in malignant disease. Reviews
of scientific literature reveal the many advantages of morcellation over
intact removal, such as reduction of incision length with consequent reduced
usage of postoperative analgesia, and shorter hospital stays (1); however,
care must be taken with this technique in order to avoid sac perforation
and possible subsequent dissemination of tumor cells within the abdominal
cavity, as well as trocar site implantation (2-5) and inadvertent lesion
of intra-abdominal structures (6). Intact removal increases the size of
the incision by 5-7 cm in those procedures considered minimally invasive,
thus altering the aesthetic result and increasing postoperative pain (7).
However, intact removal of the surgical specimen falls within the principles
of oncologic surgery, thus reducing the risk of metastatic implants and
aiding anatomical and pathological staging of the specimen (8). Another
relatively controversial aspect found in scientific reviews regards the
amount of time necessary in morcellation of renal specimens, which some
authors have reported as an average of 18 minutes (with durations varying
from 6 to 34 minutes) (1); others claim an average time of 33 minutes
(ranging from 18-115 minutes) (9).
The authors of the study in question have
presented an excellent casuistry (153 laparoscopic nephrectomies) and
have approached the main controversial aspects of morcellation, analyzing
those variables, which may be related to operative time, postoperative
analgesia, length of hospital stay, and complications associated with
the incision.
It is a well-delineated retrospective study,
which utilized a uniform methodology for the groups examined, with adequate
statistical analysis of all variables involved (sex, age, body mass index,
laterality, type of renal pathology, and weight of operative specimen).
On the other hand, when the authors report the routine use of 0.25% bupivacaine
for infiltration in incision and trocar sites, the amount of anesthetic
used is not specified, and this may cause some alteration in the analysis
of postoperative pain, as greater incisions will require a larger infiltration
of local anesthetic.
The subject approached is controversial
and sheds new perspectives in the field of specimen removal subsequent
to laparoscopic nephrectomy, clarifying several myths about the prolonged
time necessary for morcellation, as well as those regarding the risks
inherent to the method.
REFERENCES
- Landman J, Lento P, Hassen W, Unger P, Waterhouse R: Feasibility of pathological evaluation of morcellated kidneys after radical nephrectomy. J Urol. 2000; 164: 2086-9.
- Castilho LN, Fugita OE, Mitre AI, Arap S: Port site tumor recurrences of renal cell carcinoma after videolaparoscopic radical nephrectomy. J Urol. 2001; 165: 519.
- Tsivian A, Sidi AA: Port site metastases in urological laparoscopic surgery. J Urol. 2003; 169: 1213-8.
- Meng MV, Miller TR, Cha I, Stoller ML: Cytology of morcellated renal specimens: significance in diagnosis and issemination. J Urol. 2003; 169: 45-8.
- Fentie DD, Barrett PH, Taranger LA: Metastatic renal cell cancer after laparoscopic radical nephrectomy: long-term follow-up. J Endourol. 2000; 14: 407-11.
- Landman J, Venkatesh R, Kibel A, Vanlangendonck R: Modified renal morcellation for renal cell carcinoma: laboratory experience and early clinical application. Urology. 2003; 62: 632-4; discussion 635.
- Gill IS: Laparoscopic radical nephrectomy for cancer. Urol Clin North Am. 2000; 27: 707-19.
- Landman J, Lento P, Hassen W, Unger P, Waterhouse R: Feasibility of pathological evaluation of morcellated kidneys after radical nephrectomy. J Urol. 2000; 164: 2086-9.
- Walther MM, Lyne JC, Libutti SK, Linehan WM: Laparoscopic cytoreductive nephrectomy as preparation for administration of systemic interleukin-2 in the treatment of metastatic renal cell carcinoma: a pilot study. Urology. 1999; 53: 496-501.
Dr. Mardhen B. Araújo
Section of Urology
Federal University of Ceara
Fortaleza, Ceara, Brazil