LAPAROSCOPIC
DIAGNOSIS AND TREATMENT OF NONPALPABLE TESTIS
(
Download pdf )
FRANCISCO T. DENES, FERNANDO J. SAITO, FREDERICO A. SILVA, AMILCAR M. GIRON, MARCOS MACHADO, MIGUEL SROUGI
Division of Urology, School of Medicine, University of Sao Paulo, USP, Sao Paulo, SP, Brazil
ABSTRACT
Introduction:
Treatment of the cryptorchid testicle is justified due to the increased
risk of infertility and malignancy as well as the risk of testicular trauma
and psychological stigma on patients and their parents. Approximately
20% of cryptorchid testicles are nonpalpable. In these cases, the videolaparoscopic
technique is a useful alternative method for diagnosis and treatment.
Materials and Methods: We present data concerning
90 patients submitted to diagnostic laparoscopy for impalpable testicles.
Forty-six patients (51.1%) had intra-abdominal gonads. In 25 testicles
of 19 patients, we performed a two stage laparoscopic Fowler-Stephens
orchiopexy. The other 27 patients underwent primary laparoscopic orchiopexy,
in a total of 29 testicles.
Results: We obtained an overall 88% success
rate with the 2 stage Fowler-Stephens approach and only 33% rate success
using one stage Fowler-Stephens surgery with
primary vascular ligature. There was no intraoperative complication in
our group of patients. In the laparoscopic procedures, the cosmetic aspect
is remarkably more favorable as compared to open surgeries. Hospital stay
and convalescence were brief.
Conclusions: In pediatric age group, the
laparoscopic approach is safe and feasible. Furthermore, the laparoscopic
orchiopexy presents excellent results in terms of diagnosis and therapy
of the impalpable testis, which is why this technique has been routinely
incorporated in our Department.
Key
words: testis; cryptorchidism; laparoscopy
Int Braz J Urol. 2008; 34: 329-35
INTRODUCTION
Cryptorchidism
is the most common genitourinary anomaly in male children. Its incidence
can reach 3% in full term neonates, rising to 30% in premature boys (1).
The treatment of the cryptorchid testicle is justified by the increased
risk of infertility and malignancy, as well as an associated inguinal
hernia and the risk of trauma to the ectopic testicle against the pubis.
Furthermore, the psychological stigma of a missing testis for the patient,
as well as the parents’ anxiety are also factors that justifies
this type of treatment (2,3).
About 20% of cryptorchid testicles are nonpalpable.
In these cases, the laparoscopic technique is a useful alternative method
of diagnosis and treatment. We assessed our data and present our results,
including a comparison between the laparoscopic and two stage Fowler-Stephens
approaches.
MATERIALS AND METHODS
Between
September 1994 and September 2005, 90 patients were submitted to diagnostic
laparoscopy for impalpable testicles. Of these, 34 (37.8%) presented with
bilateral, while 56 (62.2%) had unilateral impalpable cryptorchidism.
The age and the laterality are presented in Table-1.

Preoperatively, all the patients were examined
at least by two different examiners at different times, confirming the
diagnosis. Another careful physical examination was performed in the operating
room, with the patient under anesthesia. When the testicle was palpated
on any one of these occasions, the patient was submitted to an open orchiopexy.
Although the preoperative ultrasound for
location of the testicle was performed in some patients, with negative
results in all, no patient underwent computerized tomography scan or magnetic
nuclear resonance imaging for the same purpose.
There was no age limit for the laparoscopic
procedure. The procedure was performed under general anesthesia, with
orotracheal ventilation and nasogastric and vesical tubes.
The laparoscopic technique (Figure-1) has
previously been described (4-6).The laparoscopic findings were similar
to those described by Castilho in 1990 (7), and are summarized in Table-2.
Surgical management was performed based on the laparoscopic findings (8,9).
In cases of testicle absence , the procedure was interrupted, whereas
in cases of intra-canalicular inguinal testis, open surgical exploration
was performed. When intra-abdominal testes were found, immediate laparoscopic
orchiectomy was performed for atrophic testicles, while patients with
viable testicles underwent laparoscopic orchiopexy. The technique of this
procedure has been previously described, stressing that in cases of low
intra-abdominal testicle (located less than 2 cm from the internal inguinal
ring) the procedure was straightforward, without transection of the spermatic
vessels, while in those located higher (more than 2 cm from the internal
inguinal ring) the vessels were sectioned to facilitate the appropriate
descent of the testicle to the scrotum (6). When the vessels are transected,
the testis is relocated into the scrotum either during the same surgical
procedure (primary or one stage Fowler-Stephens) or the relocation is
postponed for at least six months after vascular ligature (two stage Fowler-Stephens).


All the operated patients were followed-up
for 6 to 100 months, and evaluated for the incidence of intra and post-operative
complications, as well as for the final location and morphology of the
operated testes. These complications were classified as normal (good size
and consistence, in addition to appropriate position in the scrotum),
atrophic (altered morphology, independent of the position) or malpositioned
(normal morphology, but located above the scrotum). In cases of unilateral
disease, the evaluation of cryptorchid testicle was based on the normal
testicle. In cases of bilateral disease, this evaluation was based on
clinical palpation as well as ultrasonography in some cases, comparing
the obtained values with normal parameters in infancy and adulthood.
RESULTS
The
initial laparoscopic findings are summarized in Table-3. One should note
that five patients had bilateral disease, in which we had different diagnostic
findings in each affected side as emphasized in Table-3.
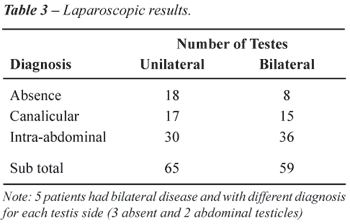
Eighteen patients (20%) presented absent
testicles, four due to agenesis and 14 to vanishing testes. In these cases,
the laparoscopic procedure was completed preventing the patients from
any further unnecessary exploration. In 12 patients of this group, who
were near pubertal age, a testicular prosthesis was inserted during the
same surgical procedure.
Thirty-two patients (35.5%) had a diagnosis
of intra-canalicular inguinal testicles. In this group, the difficulty
in palpating the testis was due to regional obesity, the small size of
the testis or general anesthesia, which facilitated the child’s
examination. The majority of patients underwent a conventional inguinal
exploration, and those with viable gonads (34.4%) had an orchiopexy during
the same procedure, while those with atrophic testicles (65.6%) underwent
orchiectomy. Only one patient underwent a laparoscopic dissection of the
inguinal testicle via the internal inguinal ring, where an atrophic testis
was found, and removed. In this group, the older children also received
testicular prosthesis at the same time. Interestingly, we observed that
the presence of a hernia sac almost always indicates the presence of a
canalicular testicle, particularly in peeping testis.
In 46 patients (51.1%), the testes were
intra-abdominal, and treatment varied according to their morphology and
position (Table-4). In three patients, four testicles were atrophic (one
patient with bilateral disease). All were submitted to immediate laparoscopic
orchiectomy. In the other 43 patients laparoscopic orchiopexy was performed.
In 25 testicles of 19 patients, we performed the two stage laparoscopic
Fowler-Stephens orchiopexy, with initial vascular transection. All were
submitted to orchiopexy at least six months later. In 21 testicles of
15 patients, the orchiopexy was also done by laparoscopic technique, while
the remaining four testicles were positioned by conventional inguinal
approach.
The other 27 patients underwent primary
laparoscopic orchiopexy, in a total of 29 testicles. In 3 of these testicles
(3 patients), vascular ligature and section were necessary, while the
majority (26 testicles) was relocated to the scrotum with preservation
of the vascular pedicle.
Minimal follow-up period was approximately
6 months. Only 2 patients were lost to follow-up during a fifteen year
protocol.
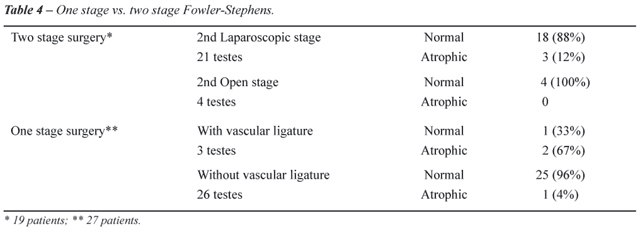
Of the 25 testicles advanced into the scrotum
by the two step Fowler-Stephens technique, 18 (88%) presented good morphology
and position in the scrotum, while 3 testicles became atrophic. Considering
this same group, an 85% success rate was achieved with the laparoscopic
second stage, as compared to a 100% success rate with the open approach.
Of the 25 testicles submitted to the primary
laparoscopic orchiopexy, without vascular transection, 96% were considered
successful, with good position and normal morphology, with only one testis
developing atrophy. Among the testes submitted to primary orchiopexy with
simultaneous vascular ligature, two presented atrophy, while one testis
remained normal (success rate of 33%).
There was no intraoperative complication
in our group of patients, and none required blood transfusion or conversion
to open procedure. All patients who underwent a laparoscopic diagnostic
procedure alone could be fed on the same day and were discharged the following
day. Those who underwent orchiopexy were discharged on the second post-operative
day. Post-operative pain was minimal and treated with common analgesics
or non-steroidal anti-inflammatory drugs, according to patients’
age.
In late follow up, we did not observe any
post-operative complication in the abdominal or scrotal percutaneous ports,
nor inguinal or incisional hernia.
COMMENTS
The
treatment of non-descended testicles is mandatory due to the increased
risk of infertility, present in up to 40% of the patients, as compared
to 6% of control groups (10), including malignancy, which reaches 20 times
that of normal adults (11).
Despite the recommendations for the treatment
of the cryptorchid testis before 2 years of age, many of our patients
were older, due to the socio-economic characteristics of the public health
system in our country, the lack of parental information and difficult
access to tertiary health care. Although fertility is already compromised
in this age group, treatment is necessary not only for the risk of malignancy,
but also for the satisfaction and improvement in the quality of the patient’s
life and parents´ concern for their children’s health (12).
In relation to diagnosis, some tests can
be used for appropriate therapeutic planning. In the case of bilateral
impalpable testes, the stimulation with human chorionic gonadotrophin
has only a relative usefulness, since a negative result, although suggestive
of absent testes, cannot completely exclude the presence of a dysplasic
gonad. Even in the case of a positive answer, it is not possible to establish
the number, location and the laterality of the gonad (13). Despite a sensitivity
of 70-90% in the diagnosis of inguinal testes, ultrasonography is not
useful in intra-abdominal cases(14). Although presenting a better quality,
both computed tomography and nuclear magnetic resonance lack sufficient
sensitivity and specificity to be considered as gold standard diagnostic
tools (15). More recently, the magnetic angioresonance was introduced
with sensibility of 96% and specificity of 100%, but it is still a new
method, with high costs, also requiring general anesthesia in children
(16).
In relation to the treatment, the use of
gonadotrophin for undescended testes presents a success rate of definitive
descent to the scrotum of 21 to 56%, with better results in bilateral
cases (13,14). Surgical treatment via an inguinal incision is the main
treatment option for palpable testicles, but can also be employed for
the evaluation and treatment of impalpable testis. In this situation,
however, surgical exploration can often require large incisions and extensive
dissections, especially in bilateral cases. This can be avoided using
laparoscopic evaluation, with a sensitivity and specificity reaching more
than 90% (17,18).
In 20% of our patients with testicular agenesis
or vanishing testis, laparoscopic surgery was the decisive diagnostic
method and saved these patients from any further incision or unnecessary
investigation. In patients with intra-canalicular testicles, laparoscopy
was fundamental for guiding the minimal inguinal exploration, which was
augmented only in cases of a viable gonad, when orchiopexy was performed.
In cases of intra-abdominal testicles, the
great advantage of laparoscopy is that, besides correct diagnosis, it
enables the therapeutic handling of the testes at the same time. Additionally
in cases of associated inguinal hernia (particularly in cases with peeping
testis), the laparoscopic approach also enables the simultaneous treatment
of the hernia sac with favorable results.
Careful dissection of the spermatic vessels
as well as preservation of the peri-deferential vessels are fundamental
to ensure testicular preservation. As regards late outcome, we have achieved
results comparable to those reported in the literature for laparoscopic
orchiopexy, with success rate of 88% for the staged Fowler-Stephens technique,
and 96% in the primary orchiopexy without vascular transection (8,17,19).
One should be aware of the inferior results of the laparoscopic primary
orchiopexy with vascular ligature (primary or one stage Fowler-Stephens).
In the literature (20), the reported success was 74.1%. In our series,
with the exception of a few cases, we only reached 33% of well located
and normal testes. Based on these results, the laparoscopic one stage
Fowler-Stephens orchiopexy, with spermatic vessel ligature, has been abandoned
in our Department.
Using laparoscopic procedures, the cosmetic
aspect is remarkably more favorable as compared to open surgery , and
the hospital stay and convalescence are much shorter. In the pediatric
age group, these factors may not be so evident for the patient themselves,
but certainly will be for the parents, who are able to resume their daily
activities earlier. Furthermore, the laparoscopic orchiopexy presents
excellent results in terms of diagnosis and therapy of the impalpable
testis, which is why this technique has been routinely incorporated in
our Department. It is noteworthy that our preference is the primary orchiopexy
without transection of the gonadal vessels. However, in cases of very
high testicles or those with short vessels we now recommend the two staged
laparoscopic technique of Fowler-Stephens.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Berkowitz GS, Lapinski RH, Dolgin SE, Gazella JG, Bodian CA, Holzman IR: Prevalence and natural history of cryptorchidism. Pediatrics. 1993; 92: 44-9.
- Trussell JC, Lee PA: The relationship of cryptorchidism to fertility. Curr Urol Rep. 2004; 5: 142-8.
- Moreno-Garcia M, Miranda EB: Chromosomal anomalies in cryptorchidism and hypospadias. J Urol. 2002; 168: 2170-2; discussion 2172.
- Poppas DP, Lemack GE, Mininberg DT: Laparoscopic orchiopexy: clinical experience and description of technique. J Urol. 1996; 155: 708-11.
- Lindgren BW, Franco I, Blick S, Levitt SB, Brock WA, Palmer LS, et al.: Laparoscopic Fowler-Stephens orchiopexy for the high abdominal testis. J Urol. 1999; 162: 990-3; discussion 994.
- Dénes, FT: Avaliação e tratamento do testículo não-palpável. In Castilho LN, Laparoscopia Urológica. Campinas, LPC Comunicações, 2000; pp. 467-5.
- Castilho LN: Laparoscopy for the nonpalpable testis: how to interpret the endoscopic findings. J Urol. 1990; 144: 1215-8.
- Peters CA, Kavoussi LR, Retik AB: Laparoscopic Management of intra-abdominal testes. J Endourol. 1993; 7(Suppl 1): 170-4.
- Cortes D, Thorup JM, Lenz K, Beck BL, Nielsen OH: Laparoscopy in 100 consecutive patients with 128 impalpable testes. Br J Urol. 1995; 75: 281-7.
- Lee PA, O’Leary LA, Songer NJ, Coughlin MT, Bellinger MF, LaPorte RE: Paternity after unilateral cryptorchidism: a controlled study. Pediatrics. 1996; 98: 676-9.
- Garner MJ, Turner MC, Ghadirian P, Krewski D: Epidemiology of testicular cancer: an overview. Int J Cancer. 2005; 116: 331-9.
- Kucheria R, Sahai A, Sami TA, Challacombe B, Godbole H, Khan MS, et al.: Laparoscopic management of cryptorchidism in adults. Eur Urol. 2005; 48: 453-7; discussion 457.
- Rajfer J, Handelsman DJ, Swerdloff RS, Hurwitz R, Kaplan H, Vandergast T, et al.: Hormonal therapy of cryptorchidism. A randomized, double-blind study comparing human chorionic gonadotropin and gonadotropin-releasing hormone. N Engl J Med. 1986; 314: 466-70.
- Kolon TF, Patel RP, Huff DS: Cryptorchidism: diagnosis, treatment, and long-term prognosis. Urol Clin North Am. 2004; 31: 469-80.
- Nguyen HT, Coakley F, Hricak H: Cryptorchidism: strategies in detection. Eur Radiol. 1999; 9: 336-43.
- Eggener SE, Lotan Y, Cheng EY: Magnetic resonance angiography for the nonpalpable testis: a cost and cancer risk analysis. J Urol. 2005; 173: 1745-9; discussion 1749-50.
- Docimo, SG: The results of surgical therapy for cryptorchidism: a literature review and analisys. J Urol. 1995; 154: 1148-52.
- Froeling FM, Sorber MJ, de la Rosette JJ, de Vries JD: The nonpalpable testis and the changing role of laparoscopy. Urology. 1994; 43: 222-7.
- Lindgren BW, Darby EC, Faiella L, Brock WA, Reda EF, Levitt SB, et al.: Laparoscopic orchiopexy: procedure of choice for the nonpalpable testis? J Urol. 1998; 159: 2132-5.
- Baker LA, Docimo SG, Surer I, Peters C, Cisek L, Diamond DA, et al.: A multi-institutional analysis of laparoscopic orchidopexy. BJU Int. 2001; 87: 484-9.
____________________
Accepted after revision:
October 20, 2007
_______________________
Correspondence address:
Dr. Francisco Tibor Dénes
Rua Barata Ribeiro, 414, Conjunto 34/35
São Paulo, SP, 01308-080, Brazil
E-mail: ftdenes@terra.com.br
EDITORIAL COMMENT
Laparoscopy
is an accepted diagnostic and treatment modality for non-palpable testes
as performed in the current series. In this series, the percentage of
intra-canalicular viable testis which was not palpable during the examination
even under anesthesia is high (34.4% of 32 patients) and it is not similar
to our experience (1). Whatever the reason, we encourage the authors to
perform laparoscopic orchiopexy instead of converting the operation to
open surgery in this situation.
Classification of intra-abdominal testes
according to the measurement of distance between the testes and the internal
inguinal ring is a good criterion but in our series, we have few cases,
which do not match this criterion. Based on these observations, we prefer
to examine the mobility of the testis by a laparoscopic forceps and to
decide if the length of the spermatic vessels and ductus deferens is suitable
for one or two stage operation.
In our series, a few cases were previously
explored by open or laparoscopic technique at another center and, diagnosed
as “absence of testis”. In those cases, we had documented
positive response to HCG stimulation test and diagnostic laparoscopy revealed
the presence of an intra-abdominal testis. Therefore, we advocate performing
an HCG stimulation test in patients with bilateral non-palpable testes
before surgical exploration.
The authors performed testicular prosthesis
placement following laparoscopic exploration in older patients with vanishing
testis. We recommend a similar option for the younger patients and, this
alternative approach could be offered to the parents before laparoscopic
exploration. Inguinal exploration may be postponed and, testicular nubbins
can be removed later at the time of testicular prosthesis implantation
surgery if there is a consensus with the family (2).
REFERENCES
- Topuzlu Tekant G, Emir H, Eroðlu E, Akman M, Büyükünal C, Daniþmend N, et al.: Experience with laparoscopy in nonpalpable testis. Eur J Pediatr Surg. 2001; 11: 177-81.
- Emir H, Ayik B, Eliçevik M, Büyükünal C, Daniþmend N, Derviþoðlu S, et al.: Histological evaluation of the testicular nubbins in patients with nonpalpable testis: assessment of etiology and surgical approach. Pediatr Surg Int. 2007; 23: 41-4.
Dr.
Haluk Emir
Division of Pediatric Urology
Cerrahpasa Medical Faculty
Istanbul University
Istanbul, Turkey
E-mail: hemir@istanbul.edu.tr