COMPARISON
OF RADICAL PROSTATECTOMY TECHNIQUES: OPEN, LAPAROSCOPIC AND ROBOTIC ASSISTED
(
Download pdf )
RODRIGO FROTA, BURAK TURNA, RODRIGO BARROS, INDERBIR S. GILL
Section of Laparoscopic and Robotic Surgery, Glickman Urological Institute, Cleveland Clinic Foundation, Cleveland, Ohio, USA
ABSTRACT
Introduction:
To review the current status of laparoscopic radical prostatectomy (LRP)
and robotic assisted radical prostatectomy (RALP) in relation to radical
retropubic prostatectomy (RRP) in the management of localized prostate
cancer.
Materials and Methods: Between 1982 and
2007 published literature was reviewed using the National Library of Medicine
database and the following key words: retropubic, laparoscopic, robotic,
robot-assisted, and radical prostatectomy. Special emphasis was given
to the technical and cost considerations as well as operative, functional
and oncologic outcomes. In particular, reports with pioneering work that
have contributed to the evolution of the technique, presenting comparative
outcomes and with large series encompassing intermediate/long term follow-up,
were taken into account.
Results: After intermediate term follow-up,
LRP and RALP achieved similar oncologic and functional results compared
to RRP. However, LRP and RALP were associated with decreased blood loss,
faster convalescence and better cosmetics when compared to RRP. The RALP
technique is undoubtedly more expensive.
Conclusions: The oncologic and functional
outcomes for LRP and RALP are similar to RRP after intermediate term follow-up.
Long term follow-up and adequately designed studies will determine the
inherent advantages and disadvantages of the individual techniques in
the management of localized prostate cancer.
Key
words: prostate cancer; prostatectomy; laparoscopy; robotics
Int Braz J Urol. 2008; 34: 259-69
INTRODUCTION
Prostate
cancer accounts for approximately one third of cancer in men in the United
States. Eighty-six percent of prostate cancer diagnosed in 2004 was localized
with 5-year survival rates approaching 100% (1). Based on excellent survival
rates, radical prostatectomy is considered the standard treatment for
the management of localized prostate cancer (2).
Retropubic Radical Prostatectomy (RRP) was
first reported by Millin in 1947 (3). However, the procedure was associated
with significant blood loss, incontinence, impotence and prolonged convalescence.
In the early 1980s, Walsh laid the foundations of anatomic RRP with better
understanding of the prostate anatomy, specifically the dorsal vein complex
and neurovascular bundle (NVB) (4). These results were associated with
better functional outcomes without compromising oncologic principles.
The variability of RRP outcomes, introduction
of laparoscopy in the urological armamentarium and the success of less
invasive treatment alternatives (i.e. brachytherapy) in prostate cancer,
have accelerated the development of laparoscopic pelvic surgery (5). Schuessler
et al. performed the first laparoscopic radical prostatectomy (LRP) in
1991 (6). Of note, the LRP technique has been refined and standardized
by Guillonneau and Vallancien in the late 1990s and the procedure has
gained popularity since then (7). In addition to the conventional advantages
of minimal invasive surgery and reduced blood loss, the LRP technique,
in expert hands, is safe and effective, and provides oncologic outcomes
comparable to that of open RRP (7,8). However, LRP is a complex procedure
associated with a steep learning curve and limited ergonomics.
Robotic assisted laparoscopic prostatectomy
(RALP) was first reported by Abbou et al. in 2000 (9). RALP has been popularized
by Menon et al. with an intention to decrease the steep learning curve
of LRP while accomplishing the advantage of a minimally invasive technique
(10). Advantages of the RALP technique include the 3-dimensional stereoscopic
visualization, intuitive finger-controlled movements and the Endowrist
technology (Intuitive Surgical, Sunnyvale, CA, USA) (11). Furthermore,
improved ergonomic surgery can be achieved by a comfortably seated surgeon.
The RRP is the reference standard for the
surgical management of localized prostate cancer. With wider availability
of the minimally invasive radical prostatectomy techniques, there is a
debate regarding what the standard treatment will be for the management
of localized prostate cancer in the near future. It is also open to discussion
as to whether experienced open surgeons should learn minimally invasive
techniques. There are no prospective randomized studies, to our knowledge,
comparing the three techniques (RRP vs. LRP vs. RALP) to date. In comparing
the three techniques, several issues such as perioperative, functional
and oncologic outcomes need to be addressed. Unquestionably, achieving
optimum cancer control is the most important determinant followed by favorable
functional outcomes. Another factor that influences treatment acceptance
is the cost.
It is clearly important to address these
issues in the urological literature. Therefore, in this review, we present
the evolution and the recent data on the outcomes of RRP, LRP and RALP
in the contemporary urological literature with a special emphasis on the
technique, cost, operative, functional and oncologic outcomes.
SURGICAL TECHNIQUE
The
standard surgical technique for RRP was described by Walsh (4). Other
urologists have used additional anatomic and technologic advances to minimize
morbidity associated with the procedure. Slabaugh and Marshall reported
modified incisional techniques and noted that the mini-laparatomy RRP
technique was associated with less operating room (OR) time and reduced
cost compared to LRP (12). Mini-laparotomy was performed using an 8 cm
low midline incision, wherein a laparoscopic camera lens was used for
visualization. Sved et al. reported a RRP technique with a modified Pfannenstiel
incision associated with better cosmetic results, less postoperative pain
and lower analgesic requirement (13).
Four different LRP techniques including
the transperitoneal antegrade technique, transperitoneal retrograde technique,
extraperitoneal antegrade technique and extraperitoneal retrograde technique
have been described (14). The antegrade transperitoneal approach is preferred
at the Cleveland Clinic. Using the transperitoneal or the extraperitoneal
approach, the senior author has performed more than 750 LRPs at our institution
since 1999.
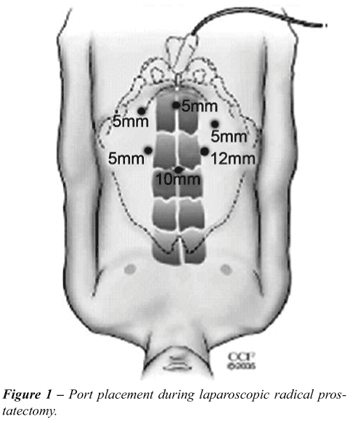
Our transperitoneal LRP technique has been
previously reported (15). Briefly, the patient is placed in a modified
lithotomy position with the arms adducted by the patient’s side.
The table is set in a 15-30 degree Trendelenburg position. Initially,
five ports are placed in a fan-array (Figure-1). Bowel loops are gently
retracted out of the pelvic cavity. An inverted U-shaped peritoneotomy
incision along the undersurface of the anterior abdominal wall is made.
Subsequently, the endopelvic fascia is freed from the fatty tissue bilaterally
and incised using a J-hook eletrocautery or cold endoshears. The Foley
catheter is replaced by a metallic urethral dilator to enhance needle
orientation during dorsal vein ligation. The dorsal vein complex ligature
is created with a 2-0 Vicryl (CT-1 needle) stitch. The posterior bladder
neck is deeply scored with a J-hook eletrocautery at the proposed line
of transection at a safe distance from the ureteric orifices. The vas
deferens is clipped with a Hem-o-lock clip and divided. The NVB is released
in an antegrade manner along the convexity of the prostate, using a combination
of sharp scissor cuts and gentle blunt teasing with a soft laparoscopic
Kittner. The dorsal vein complex is divided, followed by apical dissection
and urethral transection. Urethrovesical anastomosis is accomplished with
a watertight double-needle running suture technique using 2-0 Monocryl
in two different colors. A 20 Fr Foley catheter is inserted into the bladder.
A Jackson-Pratt drain is placed in the pelvis, the specimen is removed
by extending the umbilical port site incision and port sites are closed.
The extraperitoneal approach provides a
rapid access to the space of Retzius, minimizes bowel complications and
intra-abdominal organ damage. However, recent studies comparing transperitoneal
versus extraperitoneal approaches have not found any significant differences
(16,17). The extraperitoneal approach may be preferable in obese patients
as it may shorten the distance between the trocar insertion site and operative
field, and in patients with previous abdominal surgery where time-consuming
adhesiolysis is avoided and the risk of bowel injury is minimized (14).
LRP renewed interest in the periprostatic
neuroanatomy because of the superior image quality and enhanced magnification.
Technical modifications during LRP have mainly focused on the nerve sparing
procedure. Gill et al. have reported the use of intraoperative transrectal
ultrasound monitoring to identify the course of the NVBs (18). With this
technique, it was possible to substantially reduce the positive surgical
margin rate (19).
Similar to the LRP technique, the RALP technique
has also been described using the intraperitoneal or extraperitoneal approaches,
but most surgeons prefer the transperitoneal approach because of larger
working space and the potential for tension free urethrovesicle anastamosis.
The Da Vinci robotic system (Intuitive Surgical, Inc., Sunnyvale, CA)
is the only robotic platform available providing superior illumination
of the surgical field. We have performed more than 250 RALPs at the Cleveland
Clinic using either the transperitoneal or the extraperitoneal approach.
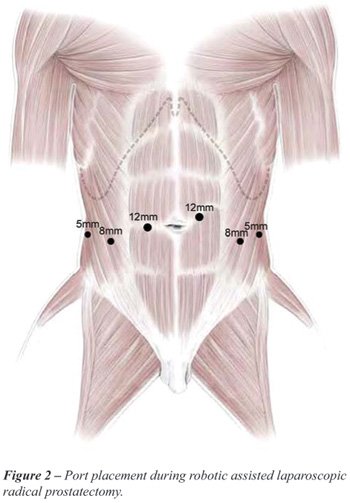
The basic surgical principles do not differ from the LRP technique. Briefly,
a 6-port strategy is used with an initially placed 12 mm port at the left
superior margin of the umbilicus. Port positioning is similar for both
the transperitoneal and extraperitoneal approaches (Figure-2). For the
transperitoneal approach, access is achieved using the Veres needle, while
extraperitoneal approach involves cut-down and dilation of the extraperitoneal
space with 10 mm PDB™ System Balloon (Tyco Healthcare, Mansfield,
MA, USA) which is advanced in the midline between the rectus muscle and
into the retropubic space prior to inflation. The prostate is exposed,
the endopelvic fascia incised bilaterally and the dorsal venous complex
is oversewn with Nº.1 Vicryl suture. The bladder neck is incised
and the seminal vesicles and vasa are dissected out. These are divided
along with the prostatic pedicles using a harmonic dissecting scalpel.
The endopelvic fascia is then reflected off the prostate preserving the
NVBs. The urethra is divided and the prostate reflected cephalad. Remaining
prostate-rectal fibers are divided and the prostate specimen placed in
an Endocatch bag. Urethrovesical anastamosis is performed with 2/0 Monocryl
and 2/0 Caprosyn sutures in a continuous running fashion.
OPERATIVE OUTCOMES
Regardless
of the approach used, mortality associated with radical prostatectomy
is low. The recently published reports comparing the different techniques
have mainly focused on the perioperative outcomes such as OR time, estimated
blood loss, analgesic requirement, length of hospitalization, duration
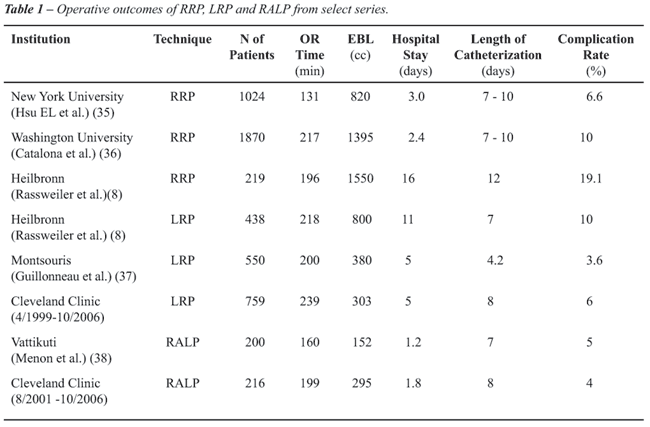
of catheterization, and postoperative complications. Table-1 summarizes
the perioperative outcomes of RRP, LRP and RALP from select large series
in the published literature from pioneering centers of excellence.
In all approaches, small abdominal incision
translates into low pain scores. Earlier reports suggested reduced analgesic
requirements with LRP compared to RRP (8), though others reported comparable
rates (20). The potential for blood loss is consistently reduced in the
LRP and RALP series and is a result of the pneumoperitoneum pressure and
excellent visualization. Likewise, overall complications appear to be
marginally lower after LRP and RALP.
Traditionally, the duration of catheterization
for RRP ranged between 2 to 3 weeks, but recent studies report shorter
catheterization periods (7 to10 days). For the laparoscopic and robotic
techniques, the duration of catheterization is usually in the range of
5 to 7 days. OR time appears to be shorter for RRP compared to RALP and
LRP, but increasing experience with minimally invasive approaches, OR
times will probably decrease.
ONCOLOGIC OUTCOMES
The
primary goal of prostate cancer surgery is to provide satisfactory oncologic
outcomes. Although, overall and cause-specific survival rates provide
the ideal measures in determining long-term oncologic control, biochemical
progression and margin positivity are the two commonly used indices to
assess oncologic outcomes following RRP, LRP and/or RALP. While RRP provides
long-term oncologic control for up to 15 years, limited follow-up is available
for the minimally invasive approaches. In patients who underwent RRP between
1998 and 2003 at the Mayo Clinic, the 3-year and 5-year PSA progression-free
survival estimate rates were 99% and 98%, respectively (21). Guillonneau
et al. evaluated their results in 1000 patients after LRP and reported
an overall biochemical progression-free survival rate of 90.5% at 3 years
(22). According to the pathologic stage, the biochemical progression-free
survival rates were 92% for pT2a, 88% for pT2b, 77% for pT3a, and 44%
for pT3b at a mean follow-up of 12 months. Rozet et al. reported 95% PSA
progression-free survival rate at a mean follow-up of 12-months in a series
of 600 patients who underwent extraperitoneal LRP (23). Rassweiler et
al. reported PSA progression-free survival rates of 83% at 3 years and
73% at 5 years in 500 patients who underwent retrograde LRP (24). Patel
et al. reported a PSA progression-free survival rate of 95% in 200 patients
who underwent RALP with a mean follow-up of 9.7 months (25).
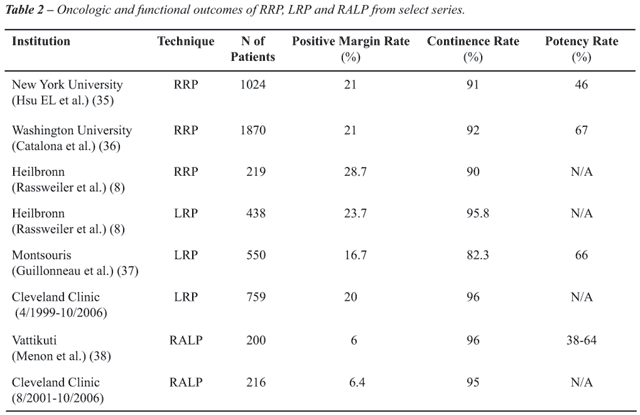
Positive margin rate is another method of
assessment of oncologic outcomes that is readily available giving a prediction
for long-term oncologic outcome. Studies from large series demonstrated
an overall positive surgical margin rate of 21- 28% for open surgery,
16.7-23.7% for LRP and 6-6.4% for RALP (Table-2).
The number of comparative studies (RRP vs.
LRP vs. RALP) is limited in the literature. The true advantages and disadvantages
of each technique will appear only after objective comparisons in prospective
studies with long-term follow-up. DiMarco et al. noted no significant
differences in positive margin rates between RRP (18.6%) and RALP (16.5%)
(26). Similarly, there were no significant differences regarding the positive
margin rate between RRP (19%) and LRP (22%) (27). In another study by
Ahlering et al., the positive surgical margin rate was 20% for RRP vs.
16.7% for RALP (28). None of these comparative studies showed any disadvantage
in terms of oncologic outcomes for the minimally invasive approaches.
Furthermore, there has been no report on port site recurrence following
LRP or RALP.
FUNCTIONAL OUTCOMES
Continence
Many differences exist between definitions
of continence and the way that the information is obtained. The best way
to analyze this outcome is undoubtedly the use of validated questionnaires.
Continence rate, basically defined as requiring one or no pad per day,
is reported to be between 90-92% for RRP, 82-96% for LRP and 95-96% for
RALP (Table-2).
In the Prostate Cancer Outcomes Study, Penson
et al. reported continence rates of 90% at 24-month follow-up and 86%
at 60-month follow-up in 1288 men who underwent RRP (29). Stolzenburg
et al. reported a continence rate of 84% at 6-month follow-up and a 92%
continence rate at 1-year follow-up in 700 extraperitoneal LRPs (30).
Regarding RALP, Ahlering et al. reported a 98% continence rate at 12-month
follow-up in their initial series of 200 patients (28). Moreover, Menon
et al. reported a continence rate of 96% in a series of more than 1100
RALP procedures (10).
It should be noted that patient selection,
tumor characteristics, and surgeon experience may interfere with the outcomes
in retrospective studies. Ongoing evaluation of continence with validated
questionnaires is required to compare various techniques of radical prostatectomy.
Data currently available suggests that similar rates for return to continence
may be achieved for the three different techniques (Table-2).
Potency
Erectile function outcomes after radical
prostatectomy depend on the urologist’s subjective impression, patient’s
self statement, use of validated questionnaires and various types of definitions
for potency. Unquestionably, the performance of a nerve sparing procedure
is of critical importance as well as the postoperative use of topic or
oral medications.
Su et al. reported 76% of intercourse rate
at 1-year follow-up after bilateral nerve-sparing LRP (31). Menon et al.,
in a study of more than 1100 patients, reported an intercourse rate of
64% for men younger than 60 years and 38% for men older than 60 years
at 6-month follow-up (10). Table-2 outlines the potency rates for RRP,
LRP and RALP from select large series in the literature. The potency rates
for RRP range from 46% to 67%, 66% following LRP, and 38% to 64% after
RALP from select large series in the published literature.
When the ability to perform sexual intercourse
after a nerve sparing procedure was compared between the RRP and LRP,
similar results, overall, were found (14). After stratifying these patients
according to age and unilateral or bilateral nerve-sparing procedure,
the rate of potency in patients younger than 55 years old undergoing LRP
with unilateral nerve-sparing procedure was 36.4% vs. 36.7% for RRP. For
the same group, but with bilateral nervesparing procedures, the potency
rate for LRP was 77.8% vs. 69% for RRP. In patients between 55 to 65 years
old with unilateral nerve-sparing procedures, the potency rate was 31%
for LRP and 20.7% for RRP. In this group, but with bilateral nerve-sparing
procedure, the potency rate for LRP was 60% vs. 52% for RRP. In patients
older than 65 years old, the potency rates were lower, but comparable
results were found for the two groups.
In a single institutional study, Abbou et
al. reported similar potency rates at 3, 6, 12 months for patients undergoing
RRP and LRP (32). To date, there are no comparative studies that show
inferior results in terms of potency for LRP compared to RRP. However,
it is important to remember that these comparative studies are limited
to different patient characteristics and sample sizes.
COST CONSIDERATIONS
In
the era of minimally invasive approaches, the economic issues are important.
Lotan et al. reported that RRP had a cost advantage of $487 over LRP and
$1726 over RALP (33). The cost difference is specifically based on the
price of a 1.2 million dollar Da Vinci robotic system (the original system)
with a maintenance fee of $100.000 per year (34). There are three robotic
systems currently available. The original three-arm system, the four-arm
system (approximately 1.4 million dollar) and the new “S-model”
(approximately 1.6 million dollar) and high-definition (additional cost)
sub-models, each with different purchasing and maintenance costs (maintenance
costs are approximately 10% of the purchasing cost). The additional cost
of disposables is approximately $2,000 US/case. This is of extreme importance
as costs are one of the main factors institutions take into consideration
when acquiring new technologies.
The economics of radical prostatectomy in
Europe differ from the USA, because of different hospitalization mentality
(patients usually stay in the hospital until the urinary catheter is removed
in Europe) (24). Using this methodology LRP represented a cost saving
of $1237 per case compared to RRP and this is attributed to the reduced
hospitalization with LRP (6 days) compared to RRP (8 days) (8).
Although RRP is considered the least expensive
at present, LRP related expenses have significantly decreased, which could
lead soon, to cost equivalence to RRP. On the other hand, the RALP technique
will certainly need a substantial decrease in the cost of the robotic
system and other relevant robotic instruments as well as maintenance fees
in order to achieve wider global acceptance and application.
The advantages and disadvantages of RRP,
LRP and RALP are detailed in Table-3.

CONCLUSIONS
Despite
only intermediate term follow-up being available for LRP and RALP techniques,
current available data demonstrates that laparoscopic and robotic prostatectomy
procedures achieve oncologic and functional outcomes similar to the well
established technique of open radical prostatectomy. Indeed, in most studies,
better results are achieved with LRP and RALP in terms of blood loss,
convalescence and cosmetics when compared to RRP.
However, LRP is associated with a steep
learning curve and longer operative time. The RALP technique holds potential
for better ergonomics. The initial purchase and maintenance fees for the
robotic platform are still expensive. Efforts to reduce the cost for RALP
must be materialized for this technique to compete with others worldwide.
After intermediate term follow-up, LRP and
RALP techniques have already gained wider acceptance in the treatment
of localized prostate cancer. With an expected reduce in the cost and
decrease in the learning curve and OR time, minimally invasive prostatectomy
techniques have the potential to be the gold standard in the treatment
of localized prostate cancer worldwide. However, long term data and adequately
designed comparative studies are clearly needed to assess the inherent
advantages and disadvantages of the three different techniques.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Jemal A, Tiwari RC, Murray T, Ghafoor A, Samuels A, Ward E, et al.: Cancer statistics, 2004. CA Cancer J Clin. 2004; 54: 8-29.
- Walsh PC: Radical prostatectomy for localized prostate cancer provides durable cancer control with excellent quality of life: a structured debate. J Urol. 2000; 163: 1802-7.
- Millin T: Retropubic Urinary Surgery. Baltimore, Williams & Wilkins Co. 1947.
- Walsh PC, Lepor H, Eggleston JC: Radical prostatectomy with preservation of sexual function: anatomical and pathological considerations. Prostate. 1983; 4: 473-85.
- Omar AM, Townell N: Laparoscopic radical prostatectomy a review of the literature and comparison with open techniques. Prostate Cancer Prostatic Dis. 2004; 7: 295-301.
- Schuessler WW, Kavoussi LR, Clayman RV, Vancaille T: Laparoscopic radical prostatectomy: initial case report. J Urol. 1992; 147: 246A.
- Guillonneau B, Vallancien G: Laparoscopic radical prostatectomy: the Montsouris experience. J Urol. 2000; 163: 418-22.
- Rassweiler J, Seemann O, Schulze M, Teber D, Hatzinger M, Frede T: Laparoscopic versus open radical prostatectomy: a comparative study at a single institution. J Urol. 2003; 169: 1689-93.
- Abbou CC, Hoznek A, Salomon L, Lobontiu A, Saint F, Cicco A, et al.: Remote laparoscopic radical prostatectomy carried out with a robot. Report of a case. Prog Urol. 2000; 10: 520-3.
- Menon M, Tewari A, Peabody JO, Shrivastava A, Kaul S, Bhandari A, et al.: Vattikuti Institute prostatectomy, a technique of robotic radical prostatectomy for management of localized carcinoma of the prostate: experience of over 1100 cases .Urol Clin North Am. 2004; 31: 701-17.
- Guru KA, Kuvshinoff BW, Pavlov-Shapiro S, Bienko MB, Aftab MN, Brady WE, et al.: Impact of robotics and laparoscopy on surgical skills: A comparative study. J Am Coll Surg. 2007; 204: 96-101.
- Slabaugh TK Jr, Marshall FF: A comparison of minimally invasive open and laparoscopic radical retropubic prostatectomy. J Urol. 2004; 172: 2545-8.
- Sved PD, Nieder AM, Manoharan M, Gomez P, Meinbach DS, Kim SS, et al.: Evaluation of analgesic requirements and postoperative recovery after radical retropubic prostatectomy using long-acting spinal anesthesia. Urology. 2005; 65: 509-12.
- Rassweiler J, Hruza M, Teber D, Su LM: Laparoscopic and robotic assisted radical prostatectomy--critical analysis of the results. Eur Urol. 2006; 49: 612-24.
- Gill IS, Zippe CD: Laparoscopic radical prostatectomy: technique. Urol Clin North Am. 2001; 28: 423-36.
- Brown JA, Rodin D, Lee B, Dahl DM: Transperitoneal versus extraperitoneal approach to laparoscopic radical prostatectomy: an assessment of 156 cases. Urology. 2005; 65: 320-4.
- Cathelineau X, Cahill D, Widmer H, Rozet F, Baumert H, Vallancien G: Transperitoneal or extraperitoneal approach for laparoscopic radical prostatectomy: a false debate over a real challenge. J Urol. 2004; 171: 714-6.
- Gill IS, Ukimura O, Rubinstein M, Finelli A, Moinzadeh A, Singh D, et al.: Lateral pedicle control during laparoscopic radical prostatectomy: refined technique. Urology. 2005; 65: 23-7.
- Ukimura O, Gill IS: Real-time transrectal ultrasound guidance during nerve sparing laparoscopic radical prostatectomy: pictorial essay. J Urol. 2006; 175: 1311-9.
- Webster TM, Herrell SD, Chang SS, Cookson MS, Baumgartner RG, Anderson LW, et al.: Robotic assisted laparoscopic radical prostatectomy versus retropubic radical prostatectomy: a prospective assessment of postoperative pain. J Urol. 2005; 174: 912-4; discussion 914.
- Gettman MT, Blute ML: Critical comparison of laparoscopic, robotic, and open radical prostatectomy: techniques, outcomes, and cost. Curr Urol Rep. 2006; 7: 193-9.
- Guillonneau B, el-Fettouh H, Baumert H, Cathelineau X, Doublet JD, Fromont G, et al.: Laparoscopic radical prostatectomy: oncological evaluation after 1,000 cases a Montsouris Institute. J Urol. 2003; 169: 1261-6.
- Rozet F, Galiano M, Cathelineau X, Barret E, Cathala N, Vallancien G: Extraperitoneal laparoscopic radical prostatectomy: a prospective evaluation of 600 cases. J Urol. 2005; 174: 908-11.
- Rassweiler J, Schulze M, Teber D, Marrero R, Seemann O, Rumpelt J, et al.: Laparoscopic radical prostatectomy with the Heilbronn technique: oncological results in the first 500 patients. J Urol. 2005; 173: 761-4.
- Patel VR, Tully AS, Holmes R, Lindsay J: Robotic radical prostatectomy in the community setting--the learning curve and beyond: initial 200 cases. J Urol. 2005; 174: 269-72.
- DiMarco DS, Ho KL, Leibovich BC: Early complications and surgical margin status following radical retropubic prostatectomy (RRP) compared to robotassisted laparoscopic prostatectomy (RALP). J Urol. 2005; 173: 277.
- Salomon L, Levrel O, de la Taille A, Anastasiadis AG, Saint F, Zaki S, et al.: Radical prostatectomy by the retropubic, perineal and laparoscopic approach: 12 years of experience in one center. Eur Urol. 2002; 42: 104-10; discussion 110-1.
- Ahlering TE, Woo D, Eichel L, Lee DI, Edwards R, Skarecky DW: Robot-assisted versus open radical prostatectomy: a comparison of one surgeon’s outcomes. Urology. 2004; 63: 819-22.
- Penson DF, McLerran D, Feng Z, Li L, Albertsen PC, Gilliland FD, et al.: 5-year urinary and sexual outcomes after radical prostatectomy: results from the prostate cancer outcomes study. J Urol. 2005; 173: 1701-5.
- Stolzenburg JU, Rabenalt R, DO M, Ho K, Dorschner W, Waldkirch E, et al.: Endoscopic extraperitoneal radical prostatectomy: oncological and functional results after 700 procedures. J Urol. 2005; 174: 1271-5; discussion 1275.
- Su LM, Link RE, Bhayani SB, Sullivan W, Pavlovich CP: Nerve-sparing laparoscopic radical prostatectomy: replicating the open surgical technique. Urology. 2004; 64: 123-7.
- Anastasiadis AG, Salomon L, Katz R, Hoznek A, Chopin D, Abbou CC: Radical retropubic versus laparoscopic prostatectomy: a prospective comparison of functional outcome. Urology. 2003; 62: 292-7.
- Lotan Y, Cadeddu JA, Gettman MT: The new economics of radical prostatectomy: cost comparison of open, laparoscopic and robot assisted techniques. J Urol. 2004; 172: 1431-5.
- Menon M: Robotic radical retropubic prostatectomy. BJU Int. 2003; 91: 175-6.
- Hsu EI, Hong EK, Lepor H: Influence of body weight and prostate volume on intraoperative, perioperative, and postoperative outcomes after radical retropubic prostatectomy. Urology. 2003; 61: 601-6.
- Catalona WJ, Carvalhal GF, Mager DE, Smith DS: Potency, continence and complication rates in 1,870 consecutive radical retropubic prostatectomies. J Urol. 1999; 162: 433-8.
- Guillonneau B, Cathelineau X, Doublet JD, Baumert H, Vallancien G: Laparoscopic radical prostatectomy: assessment after 550 procedures. Crit Rev Oncol Hematol. 2002; 43: 123-33.
- Menon M, Tewari A; Vattikuti Institute Prostatectomy Team: Robotic radical prostatectomy and the Vattikuti Urology Institute technique: an interim analysis of results and technical points. Urology. 2003; 61(Suppl 1): 15-20.
____________________
Accepted after revision:
March 15, 2008
_______________________
Correspondence address:
Dr. Rodrigo Frota
Section of Laparoscopic and Robotic Surgery
The Cleveland Clinic Foundation
9500 Euclid Avenue/A100
Cleveland, OH 44195
Fax: + 1 216 445-7031
E-mail: rodrigofrotaf@gmail.com
EDITORIAL COMMENT
The
authors compare oncologic, functional and cost outcomes between open radical
retropubic prostatectomy and the two laparoscopic approaches: pure and
robotic-assisted.
They conclude that all outcomes are similar
with the exception of costs, which are greater with the use of robotic-assistance.
Currently, robotic technology is almost universally available in the United
States. This availability has allowed many urologic surgeons to venture
into the field of advanced laparoscopic surgery. Robotic technology is
also available in many centers in Europe. Nevertheless, several well-established
groups continue to perform pure laparoscopic surgery as they have achieved
a high level of experience. This experience allows them to perform the
surgery with the same oncologic and functional outcomes as with the ones
reported with the use of robotic-assistance. Conversely, in Latin America,
the majority of laparoscopic prostatectomies are performed by the pure
laparoscopic approach due to the lack of access to robotic technology.
This well structured review should be a
tempering reminder that, as of present, the reported outcomes for surgery
are the same regardless of the approach. The importance of the learning
curve and experience in achieving maximal oncologic and functional outcomes
should always be remembered. There are currently competing, effective
treatments for localized prostate cancer such as the different forms of
radiation therapy, cryotherapy, and high intensity focus ultrasound. Therefore,
it is incumbent upon the urologic surgeon to remain abreast of improvements
in technique, advances in technology and to maintain maximal surgical
skills regardless of the approach.
Dr.
Julio Pow-Sang
Chief, GU Oncology Division
H. Lee Moffitt Cancer Center
University of South Florida College of Medicine
Tampa, Florida, USA
E-mail:julio.powsang@moffitt.org
EDITORIAL COMMENT
For
patients diagnosed with prostate cancer, choosing whether and how to treat
can be a daunting task. The widespread implementation of minimally invasive
surgical approaches has dramatically altered the landscape of treatment
options. Short-term perioperative benefits from laparoscopic and robotic-assisted
surgery have been definitively established. However, in regard to more
meaningful outcomes such as cancer control, urinary continence, and sexual
function methodologically sound comparisons to open surgery are lacking
(1).
Recognizing the inherent limitations in
the published literature (e.g. patient selection, tumor characteristics,
and surgeon experience), the authors do an excellent job of concisely
and evenhandedly reviewing the three most common surgical approaches to
radical prostatectomy. In light of the multiple options, we agree the
impact of surgeon skill and experience is likely to be far more important
than whether he or she looks at the prostate on a television monitor or
via an open incision (2-5).
Further, an honest understanding of the
merits and limitations of the individual procedures will only be garnered
when validated questionnaires are uniformly used to assess functional
recovery and quality of life. The inconsistent use of these metrics coupled
with the potential for selection bias skews the available data and accounts
for the wide range of reported outcomes.
The percentage of radical prostatectomies
performed laparoscopically or robotically has been steadily increasing,
from 12% to 31% between 2003 and 2005, and will likely continue to do
so (4). However, we must be careful of “gizmo idolatry” and
beware of the trap of “the cutting edge or first on the block use
of a gizmo” which can “bestow on the physician a mantle of
expertise, competence, and pre-eminence even if there is little or no
evidence that the patient will benefit” (6). Careful, honest, and
diligent review of outcomes, as this and other studies undertake, will
be of utmost importance to ensure that we are offering patients the optimal
treatment and not just the latest gizmo.
REFERENCES
- Eggener SE, Guillonneau B: Laparoscopic Radical Prostatectomy: Ten Years Later, Time for Evidence-Based Foundation. Eur Urol. 2008; Mar 5. Epub ahead of print
- Vickers AJ, Bianco FJ, Serio AM, Eastham JA, Schrag D, Klein EA, et al.: The surgical learning curve for prostate cancer control after radical prostatectomy. J Natl Cancer Inst. 2007; 99: 1171-7.
- Herrell SD, Smith JA Jr: Robotic-assisted laparoscopic prostatectomy: what is the learning curve? Urology. 2005; 66 (5 Suppl.): 105-7.
- Hu JC, Wang Q, Pashos CL, Lipsitz SR, Keating NL: Utilization and outcomes of minimally invasive radical prostatectomy. J Clin Oncol. 2008; 26: 2278-84.
- Berryhill R, Jhaveri JJ, Yadav R, Leung R, Rao S, El-Hakim A, et al.: Robotic Prostatectomy: A Review of Outcomes Compared with Laparoscopic and Open Approaches. Urology. 2008; Apr 23. Epub ahead of print
- Leff B, Finucane TE: Gizmo idolatry. JAMA. 2008; 299: 1830-2.
Dr.
Lambda Msezane
Dr. Scott Eggener
Section of Urology, Department of Surgery
University of Chicago
Chicago, Illinois, USA
E-mail: seggener@surgery.bsd.uchicago.edu