SMALL
ROUND BLUE CELL TUMOR OF SEMINAL VESICLE IN A YOUNG PATIENT
(
Download pdf )
ADRIANO A. DE PAULA, ADRIANO R. MALTEZ, ELIANE D. MOTA
Sections of Oncological Urology and Pathology, Araujo Jorge Hospital, Goiania, Goias, Brazil
ABSTRACT
Seminal vesicle tumor is a rare disease with unclear origin. Generally, it is presented as a pelvic mass that can be detected by sonography and digital rectal exam. The authors report a 25-year-old patient with a pelvic mass which the magnetic resonance and surgical specimen reveal a seminal vesicle tumor. Immunohistochemical findings favored a primitive neuroectodermal tumor of the seminal vesicle. Herein, the treatment, histological and histochemical findings of this entity are discussed.
Key
words: seminal vesicles; neuroectodermal tumors; urogenital neoplasms
Int Braz J Urol. 2006; 32: 566-9
INTRODUCTION
Seminal vesicle tumors are rare malignancies, usually carcinomas and are generally presented as a retrovesical mass that can be detected by digital rectal examination and sonography (1). Small round blue cell tumors (SRBCT) is a group of neoplasms that share a common and unique chromosomal translocation and include the primitive neuroectodermal tumor (PNET) and the Ewing’s sarcoma family. PNET typically develops in pediatric population, arising from the thoracic region, but genitourinary involvement in adulthood is uncommon.
CASE REPORT
A
25-year-old man underwent abdominal sonography due to epygastric pain
which showed a complex-cystic mass with 5,0x 4,9x 5,5cm in the topography
of seminal vesicles. A pelvic computerized tomography confirmed a solid
retrovesical lesion. The patient declined an ultrasound guided trans-rectal
biopsy and never returned during a 12 month-period. After this period
he returned complaining of rectal stricture, and lower urinary obstructive
symptoms.
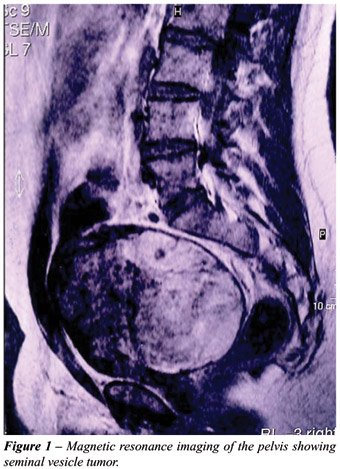
Pelvic magnetic resonance showed a 17 cm
retrovesical mass (Figure-1) and a trans-rectal ultrasound guided biopsy
revealed small round cells for which immunohistochemical findings suggested
a primitive neuroectodermal tumor diagnosis. Two cycles of neo-adjuvant
chemotherapy consisting of vincristine, cyclophosphamide, doxorubicin,
ifosfamide and etoposide were performed, resulting in no radiological
response.
Workup for metastasis was negative and the
patient underwent laparotomy with resection of the mass. The tumor did
not infiltrate adjacent organs and the surrounding desmoplastic reaction
allowed negative surgical margins with prostate, bladder and rectum preservation.
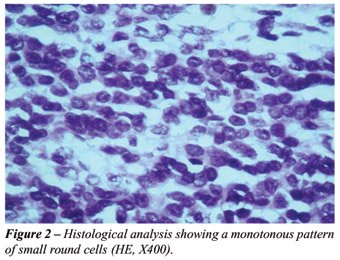
Histological exam showed an enormous amount
of necrosis and hemorrhage intermixed by a monotonous pattern of small
round blue cells with discreet pleomorfism, clear cytoplasm, solid block
setting with cystic areas and fibrous colagenized stroma (Figure-2). Immunohistochemical
examination was positive for CD-99 (Figure-3) and S-100 protein while
muscular actin, gp100 antigen, CD34, Desmin, Melan A/MART-1, EWS-FLI1,
Alpha-Inibin and Calreatin were negative. Focally positive staining for
cytokeratin 40, 48, 50 and 50.6 KDa was found. The combination of the
histological and immunohistochemical results leaded to the diagnosis of
a PNET. Reciprocal translocation t(11;22)(q24;q12) using transcriptase-reverse
Polymerase Chain Reaction (RT-PCR) was inconclusive in the present study
due to the lack of PGK1 and ACBT genes amplification of the surgical specimen.

After a three years follow up, the patient
remained potent, with normal urinary and digestive functions and showed
no relapse.
COMMENTS
Genitourinary
origin of PNET is rare and diagnosis is difficult and usually confused
with primary rectum or prostate carcinomas, benign tumors (1) or with
other small round blue cell tumors (SRBCT). Differential diagnosis must
include Ewing´s sarcomas, peripheral medulloepithelioma, rhabdomyosarcomas,
myxoid liposarcomas, malignant fibrous histiocytomas chondrosarcomas,
lymphoblastic lymphoma and even small cell osteosarcomas and neuroblastomas.
Differential diagnosis must also include benign conditions like prostatic
utricle cyst, prostatic abscess, seminal vesicle hydrops, seminal vesicle
cyst, seminal vesicle empyema, ectopic ureterocele, fibrous obturator
fossa cyst, hemangiopericytoma, among others (2).
Some genitourinary PNETs have already been
reported arising from kidney, adrenal gland, prostate, spermatic cord
and testis, but to the best of our knowledge, up to now, no seminal vesicle
origin has been published.
Although PNETs can be accurately diagnosed
using time-honored morphologic criteria and immunohistochemistry, the
genetic confirmation of the translocation t (11;22) (q24;q12) by cytogenetics
and/or molecular analysis is essential for the diagnosis of unusual morphologic
variants, including adamantinoma-like, spindled, esclerosis and clear
cell/ anaplastic variants (3). CD99 expresses protein product of the fusion
gene EWS/FLI-1 and are often positive in PNET, SRBCT and Ewing´s
sarcoma family. The combination of histological, immunohistochemical and,
sometimes, cytogenetics leads the final diagnosis. In the present case,
despite the lack of cytogenetic confirmation of the reciprocal translocation
t (11;22) (q24;q12), the positivity of CD99 and S-100 protein in the immunohistochemical
exam and the histological presentation favored PNET diagnosis.
The biological behavior of this tumor is
expressed by a rapid growing mass non-responsive to chemotherapy and frequently
associated to distant metastasis. The presence of an extensive area of
necrosis in histopathological exam means that there might have been an
expressive response to the neo-adjuvant chemotherapy, which was clinically
reflected by a favorable evolution regarding relapse and survival.
Surgical approach is the best treatment
modality and new chemotherapy agents are necessary to achieve better results
in metastatic disease.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Martinez Ibanez V, Abad P, Toran N, Gonzalez CI, Sanchez de Toledo J, Marques A, et al.: Primitive neuroectodermal tumors: difficult tumors versus modern oncology. Cir Pediatr. 1998; 11: 5-9.
- Dahms SE, Hohenfellner M, Linn JF, Eggersmann C, Haupt G, Thuroff JW: Retrovesical mass in men: pitfalls of differential diagnosis. J Urol. 1999; 161: 1244-8.
- Folpe AL, Goldblum JR, Rubin BP, Shehata BM, Liu W, Dei Tos AP, et al.: Morphologic and immunophenotypic diversity in Ewing family tumors: a study of 66 genetically confirmed cases. Am J Surg Pathol. 2005; 29: 1025-33.
_____________________
Accepted
after revision:
March 5, 2006
________________________
Correspondence address:
Dr. Adriano A. Peclat de Paula
Seção de Onco-Urologia, Hospital Araújo Jorge
Rua 239 / 181 - Setor Universitário
74605-070, Goiânia, GO, Brazil
E-mail: adrianopaula@brturbo.com.br
Primary
seminal vesical tumors either benign or malignant are very rare. Primary
adenocarcinoma of the seminal vesicle is a rare tumor. Only 50 cases have
been reported in literature. Differential diagnosis includes carcinoma
extending from the urinary bladder, prostate, or rectum. Cystadenomas
may be incidentally discovered on rectal examination or at autopsy in
middle-aged men, or the patients may present hemospermia or nonspecific
suprapubic pain. Epithelial-stromal tumors of the seminal vesicle include
a spectrum of tumors that grossly and microscopically resemble the similarly
named tumor of the prostate, and fibroadenoma and phyllodes tumor of the
breast. The distinction between cystadenoma and epithelial-stromal tumor
of the seminal vesicle is based on the microscopic aspect of the stroma:
normal or possibly reactive smooth muscle favors cystadenoma and hypercellular,
presumably neoplastic stroma favors epithelial-stromal tumor.
Other
tumors are equally very rare. The present report is a unique case of primary
small round undifferentiated tumor of the seminal vesicle. There is a
spectrum of tumors showing small round undifferentiated cells including
T lymphoblastic lymphomas, poorly differentiated synovial sarcomas, some
neuroendocrine carcinomas, rare cases of rhabdomyosarcoma usually of alveolar
type and the primitive neuroectodermal tumors (PNET). The latter having
been the source of both controversy and rapid advances in recent years
but the term PNET is now the preferred term to describe a family of lesions
that are characterized by a specific and reproducible reciprocal chromosome
translocation, t(11;22)(q24;q12). These tumors show morphologic, immunohistochemical,
ultrastructural and tissue cultural evidence of neuroendocrine differentiation.
In the present case, in spite of lack of cytogenetic confirmation of the
reciprocal translocation, the positivity of CD99 and S-100 protein in
the immunohistochemical exam and the histological features favor the diagnosis
of PNET.
Dr. Athanase Billis
Full-Professor of Pathology
State University of Campinas, Unicamp
Campinas, São Paulo, Brazil
E-mail: athanase@fcm.unicamp.br