INTRAVESICAL
PROTRUSION OF THE PROSTATE AS A PREDICTIVE METHOD OF BLADDER OUTLET OBSTRUCTION
(
Download pdf )
LEONARDO O. REIS, GUILHERME C. BARREIRO, JAMAL BARACAT, ALESSANDRO PRUDENTE, CARLOS A. D’ANCONA
Division of Urology, School of Medicine, University of Campinas, Campinas, Sao Paulo, Brazil
ABSTRACT
Objective:
Pressure-flow study is the gold standard for diagnosis of bladder outlet
obstruction (BOO). A prospective study was carried out to compare urodynamic
evaluation and measurement of intravesical protrusion of the prostate
for diagnosing BOO.
Materials and Methods: Patients presenting
with lower urinary tract symptoms (LUTS) associated with benign prostatic
hyperplasia and suspected BOO were prospectively evaluated through conventional
urodynamics and classified according to the bladder outlet obstruction
index (BOOI). They also underwent abdominal ultrasound measurement of
the intravesical prostatic protrusion (IPP) and prostatic volume. The
IPP was classified into three stages: grade I under 5 mm; grade II, between
5 and 10 mm; and grade III over 10 mm.
Results: Forty-two patients, mean age 64.8
± 8.5 years were enrolled. Transabdominal ultrasound determined
a mean prostatic volume of 45 ± 3.2 mL. Achieved IPP’s values
were the following: grade I - 12 (28.5%), grade II - 5 - (12%) and grade
III - 25 (59.5%). The results of prostate volume differed significantly
between obstructed and non-obstructed men (p = 0.033) and for IPP among
obstructed, inconclusive and non-obstructed men (p = 0.016). For IPP,
the area under ROC curve was 0.758 (95% confidence interval - 0.601 to
0.876), and the cutoff point to indicate BOO was 5 mm with 95 % sensitivity
(75.1 - 99.2) and 50 % specificity (28.2 - 71.8).
Conclusion: IPP and prostatic volume measured
through abdominal ultrasound are noninvasive and accessible methods that
significantly correlate to urinary BOO, and are useful in the diagnosis
of male urinary obstructive problems.
Key
words: bladder outlet obstruction; prostate; volume; flowmetry;
sensitivity and specificity
Int Braz J Urol. 2008; 34: 627-37
INTRODUCTION
Bladder
outlet obstruction (BOO) is characterized by increased detrusor pressure
and reduced urinary flow rate. Pressure-flow studies are the gold standard
for BOO determination. However, this method is an invasive and expensive
procedure with limited availability.. Therefore, attempts have been made
to diagnose BOO through noninvasive methods that can be divided into 2
categories: non-urodynamically based measurements and noninvasive urodynamics.
Non-urodynamically based measurements include
symptoms, post-void residual urine (PVR), Prostate Specific Antigen (PSA)
and ultrasound derived measurements, such as prostate volume, bladder
wall thickness, bladder weight and intravesical prostatic protrusion (IPP).
Noninvasive urodynamics include uroflowmetry, use of a penile cuff, the
condom-method and Doppler urodynamics (1).
It is well known that the prostate’s
anatomic conformation together with intravesical prostatic protrusion
(IPP) may affect normal voiding.
Earlier studies have previously demonstrated
that the ultrasonographic measurement of IPP could identify BOO. A total
of 200 patients were assessed with invasive urodynamics and transabdominal
ultrasound. The relationship of IPP to BOO showed that as IPP grade increased
in severity, BOO grade also increased. The sensitivity and specificity
of diagnosing BOO were 76% and 92% for over 10 mm IPP, 17% and 53% for
between 5 and 10 mm IPP and 7% and 56% for under 5 mm IPP, respectively.
PVR more than 100 mL showed 75% sensitivity and 91% specificity for predicting
BOO in the population studied (2).
The objective of this study was to define
how the IPP and prostate volume, measured through abdominal ultrasound,
might alter voiding and determine the accuracy of this measurement compared
to conventional urodynamics in diagnosing BOO.
MATERIALS AND METHODS
A
prospective study was carried out in Latin-American patients presenting
with lower urinary tract symptoms (LUTS) and evaluated by urinalysis to
exclude urinary tract infection.
Patients who had been previously submitted
to urologic surgeries, or had urologic neoplasia, bladder calculus or
presented any type of neurological abnormality or using alpha-blockers,
anticholinergics, antiandrogens or another medications which may affected
the voiding patterns were excluded from this study.
In the period ranging from June to August/2005,
after Ethics Committee approval and written informed consent, these patients
were evaluated using anamnesis, International Prostatic Symptoms Score
(IPSS) and IPSS Quality of Life (IPSS-QoL) questionnaires, physical, neurological,
digital rectal examination and conventional urodynamic evaluation (Dynapack,
Dynamed, 2004) and classified according to BOOI.
Urodynamics were done according to the “good
urodynamic practices” recommended by the International Continence
Society (3). Bladder outlet obstruction index (BOOI), defined as the detrusor’s
pressure at the maximum urinary flow (pdet_qmax) minus two times the maximum
flow (qmax): BOOI = pdet_qmax - 2 x qmax. Values below 20 were considered
non-obstructed, between 20 and 40 inconclusive and higher than 40, obstructed
(4). Postvoid residual urine volume was measured during urodynamic investigation,
after free uroflowmetry (free flow).
After one week the patients underwent an
ultrasound study performed by the same physician (J.B.) blinded to the
urodynamic results performed by L.O.R. Abdominal ultrasound (Toshiba model
Powervision 6000) was performed in the sagittal plane, using transductor
frequencies between 3 and 6 MHz, and IPP along with the prostatic volume
were measured. According to Yuen et al. (5), the bladder was filled with
at least 100 mL of urine in order to consider the IPP determination; this
was achieved through the ingestion of one liter of water in a two hour
period after voiding. IPP was defined by the distance from the tip of
the prostate’s protrusion into the vesical lumen to the bladder
neck measured in millimeters (Figure-1). Measurements were divided into
three stages: grade I < 5 mm, grade II 5-10 mm, grade III > 10 mm
(2). Prostate volumes were determined through software (Powervision 600)
for automatic measurement and expressed in milliliters (mL).

The statistical analysis was performed through
Kruskal-Wallis and Dunn’s post test to multiple comparison, and
area under ROC curve, using MedCalc version 5.00.019 and SAS System for
Windows version 9.1.3.
RESULTS
The
clinical and demographic characteristics are shown in Table-1.

The pressure/flow study showed mean Qmax
of 8.5 ± 4.3 mL/s, Pdet.qmax of 58.1 ± 26 cm H2O,
and postvoid residual urine volume after free flow of 70 ± 177
mL. Based on BOOI, 20 (47.6%) patients presented obstruction, 12 (28.5%)
were inconclusive and 10 (23.9%) did not present obstruction. The mean
BOOI was 28.6 (SD 13.4).
IPP’s values obtained were as follows:
grade I - 12 (28.5%), grade II - 5 - (12%) and grade III - 25 (59.5%).
Comparing prostatic volume and IPP with
BOOI we found according to Kruskal-Wallis and Dunn’s post test that
the results of prostate volume differed significantly between obstructed
and non-obstructed men (p = 0.033) and the results of IPP differed significantly
among obstructed, inconclusive and nonobstructed men (p = 0.016), Table-2.
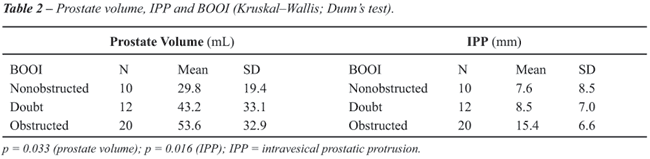
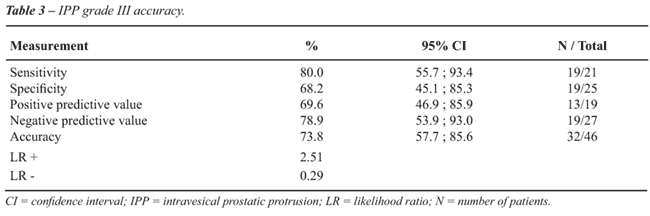
Table-3 demonstrates that IPP’s grade
III reached up to 80% sensitivity and 68 % specificity for diagnosing
BOO. Positive predictive value was 70 % and the negative predictive value
79 %.
Considering the slight IPP superiority over
prostate volume to detect obstruction, we calculated the IPP cutoff point
to indicate obstruction as 5 mm with 95 % sensitivity (75.1 - 99.2) and
50 % specificity (28.2 - 71.8); likelihood ratio of positive test result
1.90 and likelihood ratio of negative test result 0.10.
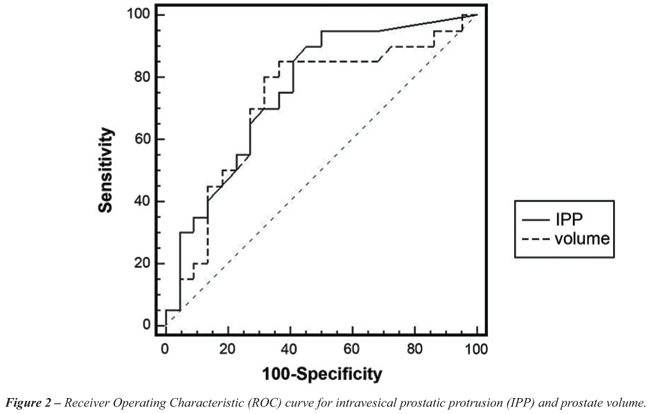
The area under ROC curve was 0.758 (95 %
confidence interval - 0.601 to 0.876) for IPP and 0.718 (95% confidence
interval - 0.558 to 0.846) for prostate volume, Figure-2.
A flow diagram for IPP on diagnostic accuracy
is showed in Figure-3.

COMMENTS
LUTS
are one of the most common complaints in the elderly men and benign prostate
obstruction is one of the most frequent causes. Pressure flow study has
been recommended before surgical treatment of prostate enlargement by
many authors. Searching for new accurate methods that could substitute
the gold standard pressure-flow study demonstrates the need for lowering
costs, expanding accessibility and relieving patient discomfort .
Since transrectal methods can producegreat
discomfort to the patient, abdominal ultrasound was demonstrated to be
equivalent to rectal ultrasound for measuring the prostate when bladder
volume is over 100 mL (5,6).
Clinical data such as IPSS, post voiding
residue and flowmetry have been previously demonstrated to correlate mostly
to lower urinary tract functional status rather than mechanical obstruction
itself (7-9). Therefore, noninvasive measurements of the prostate intend
to delineate a morpho-functional correlation in order to orient conduct
towards LUTS secondary to benign prostate obstruction.
Almost all studies on IPP measurements come
from Asia and it is unknown if the results in Asians are valid for Latin-Americans
or Caucasians as well.
Chia et al. (2) demonstrated the possibility
of using the IPP measurements for diagnosing BOO, which was also a predictor
of the capacity for spontaneous voiding after acute urinary retention
in Tan et al. study (10).
Other authors have suggested determining
bladder weight, bladder wall width or prostate conformation through abdominal
or rectal ultrasound (11-14).
Kojima et al. demonstrated, studying 104
patients, that the bladder weight more than 35 g performed thought transabdominal
ultrasound is strongly associated with bladder outlet obstruction on pressure-flow
studies (15).
A bladder wall thickness of 5 mm appeared
to be the best cutoff point to diagnose bladder outlet obstruction, since
63.3% of patients with bladder wall thickness less than 5 mm were unobstructed
while 87.5% of those with a bladder wall thickness 5 mm or greater were
obstructed in a study including 174 patients of Manieri et al. at 150
mL bladder filling (16).
Hakenberg et al. (17) found that mean bladder
wall thickness was 3.33 mm in healthy men and 3.67 mm in men with LUTS
and BPE, measuring all patients at different bladder fillings. BOO was
found in 95.5% of men with a detrusor wall thickness greater than or equal
to 2 mm in Oelke et al. study, at 250 mL or more bladder filling (18).
Recently, Blatt et al. (19) who performed
urodynamics evaluation and abdominal ultrasound among patients with different
types bladder dysfunction, found that mean bladder wall thickness in patients
with normal urodynamics, bladder outlet obstruction, detrusor overactivity
and increased bladder sensation was 2.0, 2.1, 1.9 and 1.8 mm, respectively.
No significant difference was found between the groups. In particular,
there was no difference in bladder wall thickness between patients with
normal urodynamics, and those with bladder outlet obstruction (p = 0.31)
or detrusor overactivity (p = 0.31).
The inconsistency as regards the results
obtained and the lack of technique standardization have limited their
clinical use until now.
Intravesical protrusion seems to corroborate
with urinary obstruction through a “valve ball” mechanism,
in which the prostate’s lateral and medium lobes interfere on the
complete opening of the vesical neck while the patient urinates (10).
According to this mechanism and based on the present study, it was demonstrated
that the intravesical protrusion of the prostate relates not only to the
urinary obstruction itself, but it also provides information concerning
the severity of obstruction. It has been demonstrated that the greater
the IPP, the higher BOOI (20). Still significant, but to a lesser extent,
results of prostatic volume obtained through ultrasound and PSA also related
to the degree of obstruction (21-24).
Utilizing receiver-operator characteristic
curves, the area under the curve for IPP were 0.772, and 0.858 for Lim
et al. (21) and Keqin et al. (20), respectively. The latter authors found
8.5 mm as the best cutoff value for IPP with 75.5 % of sensitivity and
82.6 of specificity.
Our findings, 0.758 for the area under the
curve and 5 mm as the best cutoff value for IPP, are in agreement with
these earlier investigations.
On the other hand, our study had a limited
number of patients and presented great variability of results, which weakened
its immediate clinical application. However, these early statistically
significant results lead towards new tendencies and studies necessary
to seek improved methods of diagnosing BOO as well as technique standardization.
CONCLUSION
IPP and prostatic volume measured through abdominal ultrasound are noninvasive and accessible methods that significantly correlate with urinary BOO, and diagnose male urinary obstructive problems. However, results are still variable and the small number of patients in this study renders further studies necessary for a final definite conclusion.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Belal M, Abrams P: Noninvasive methods of diagnosing bladder outlet obstruction in men. Part 1: Nonurodynamic approach. J Urol. 2006; 176: 22-8.
- Chia SJ, Heng CT, Chan SP, Foo KT: Correlation of intravesical prostatic protrusion with bladder outlet obstruction. BJU Int. 2003; 91: 371-4.
- Schäfer W, Abrams P, Liao L, Mattiasson A, Pesce F, Spangberg A, et al.: Good urodynamic practices: uroflowmetry, filling cystometry, and pressure-flow studies. Neurourol Urodyn. 2002; 21: 261-74.
- Abrams P: Bladder outlet obstruction index, bladder contractility index and bladder voiding efficiency: three simple indices to define bladder voiding function. BJU Int. 1999; 84: 14-5.
- Yuen JS, Ngiap JT, Cheng CW, Foo KT: Effects of bladder volume on transabdominal ultrasound measurements of intravesical prostatic protrusion and volume. Int J Urol. 2002; 9: 225-9.
- Ohnuki T, Kurokawa K, Katoh N, Fukabori Y, Shimizu K, Nakai K, et al.: Transrectal longitudinal ultrasonography of the prostate by electronic linear scanning. Hinyokika Kiyo. 1987; 33: 1385-8.
- Netto Júnior NR, D’Ancona CA, de Lima ML: Correlation between the International Prostatic Symptom Score and a pressure-flow study in the evaluation of symptomatic benign prostatic hyperplasia. J Urol. 1996; 155: 200-2.
- el Din KE, Kiemeney LA, de Wildt MJ, Rosier PF, Debruyne FM, de la Rosette JJ: The correlation between bladder outlet obstruction and lower urinary tract symptoms as measured by the international prostate symptom score. J Urol. 1996; 156: 1020-5.
- Ezz el Din K, Kiemene LA, de Wildt MJ, Debruyne FM, de la Rosette JJ: Correlation between uroflowmetry, prostate volume, postvoid residue, and lower urinary tract symptoms as measured by the International Prostate Symptom Score. Urology. 1996; 48: 393-7.
- Tan YH, Foo KT: Intravesical prostatic protrusion predicts the outcome of a trial without catheter following acute urine retention. J Urol. 2003; 170: 2339-41.
- Ochiai A, Kojima M: Correlation of ultrasound-estimated bladder weight with ultrasound appearance of the prostate and postvoid residual urine in men with lower urinary tract symptoms. Urology. 1998; 51: 722-9.
- Kuo HC: Clinical prostate score for diagnosis of bladder outlet obstruction by prostate measurements and uroflowmetry. Urology. 1999; 54: 90-6.
- Ockrim JL, Laniado ME, Patel A, Tubaro A, St Clair Carter S: A probability based system for combining simple office parameters as a predictor of bladder outflow obstruction. J Urol. 2001; 166: 2221-5.
- Kessler TM, Gerber R, Burkhard FC, Studer UE, Danuser H: Ultrasound assessment of detrusor thickness in men-can it predict bladder outlet obstruction and replace pressure flow study? J Urol. 2006; 175: 2170-3.
- Kojima M, Inui E, Ochiai A, Naya Y, Ukimura O, Watanabe H: Ultrasonic estimation of bladder weight as a measure of bladder hypertrophy in men with infravesical obstruction: a preliminary report. Urology. 1996; 47: 942-7.
- Manieri C, Carter SS, Romano G, Trucchi A, Valenti M, Tubaro A: The diagnosis of bladder outlet obstruction in men by ultrasound measurement of bladder wall thickness. J Urol. 1998; 159: 761-5.
- Hakenberg OW, Linne C, Manseck A, Wirth MP: Bladder wall thickness in normal adults and men with mild lower urinary tract symptoms and benign prostatic enlargement. Neurourol Urodyn. 2000; 19: 585-93.
- Oelke M, Höfner K, Wiese B, Grünewald V, Jonas U: Increase in detrusor wall thickness indicates bladder outlet obstruction (BOO) in men. World J Urol. 2002; 19: 443-52.
- Blatt AH, Titus J, Chan L: Ultrasound measurement of bladder wall thickness in the assessment of voiding dysfunction. J Urol. 2008; 179: 2275-8; discussion 2278-9.
- Keqin Z, Zhishun X, Jing Z, Haixin W, Dongqing Z, Benkang S: Clinical significance of intravesical prostatic protrusion in patients with benign prostatic enlargement. Urology. 2007; 70: 1096-9.
- Lim KB, Ho H, Foo KT, Wong MY, Fook-Chong S: Comparison of intravesical prostatic protrusion, prostate volume and serum prostatic-specific antigen in the evaluation of bladder outlet obstruction. Int J Urol. 2006; 13: 1509-13.
- Dicuio M, Pomara G, Vesely S, Morelli G, Fabris FM, Ales V, et al.: The use of prostatic intravesical protrusion correlated with uroflowmetry: a new method to measure obstruction in patients with LUTS due to BOO without using P/F studies. Arch Ital Urol Androl. 2005; 77: 50-3.
- Nose H, Foo KT, Lim KB, Yokoyama T, Ozawa H, Kumon H: Accuracy of two noninvasive methods of diagnosing bladder outlet obstruction using ultrasonography: intravesical prostatic protrusion and velocity-flow video urodynamics. Urology. 2005; 65: 493-7.
- Oelke M, Höfner K, Jonas U, de la Rosette JJ, Ubbink DT, Wijkstra H: Diagnostic accuracy of noninvasive tests to evaluate bladder outlet obstruction in men: detrusor wall thickness, uroflowmetry, postvoid residual urine, and prostate volume. Eur Urol. 2007; 52: 827-34.
____________________
Accepted after revision:
August 4, 2008
_______________________
Correspondence address:
Dr. Leonardo Oliveira Reis
R. Votorantim, 51, ap. 43
Campinas, SP, 13073-090, Brazil
Fax: + 55 19 3521-7481
E-mail: reisleo@unicamp.br
EDITORIAL COMMENT
Benign
prostatic hyperplasia (BPH) belongs to the most common benign diseases
in the aging men. The prevalence of histological BPH increases with age
and appears in approximately 40% of men aged 51-60 years and in approximately
90% of men aged 81-90 years (1). With increasing life expectancy worldwide
more men will have these histological changes in their prostate and the
probability of seeking professional help will increase as well. It is
doubtful if health care systems can support the financial burden associated
with the assessment and treatment of BPH-related symptoms and conditions
in the future. Therefore, every approach to make the assessment and treatment
easier, faster, and cheaper is highly welcome. The authors of the appending
article report about their attempt and introduce a new non-invasive test
to a broader public (2).
The BPH disease is characterized by benign
prostatic enlargement (BPE), bladder outlet obstruction (BOO), and lower
urinary tract symptoms (LUTS). However, no clear correlations have been
found between these three components and, therefore, each component has
to be evaluated separately. Evaluation of BPE, by digito-rectal examination
or transrectal ultrasound measurement, or LUTS, by history or questionnaires,
is quick, cheap, easy, and without relevant morbidity. However, assessment
of BOO has been more difficult until now. Only pressure-flow studies were
able to detect and quantify bladder outflow resistance adequately. Urodynamic
investigations are invasive, expensive, time-consuming, uncomfortable
for the patients, widely unavailable, and necessitate a certain degree
of education in terms of performance and interpretation of measurement
results and artifacts. The morbidity of urodynamic measurements in men
is in the range of 19% and includes dysuria, urinary tract infection,
fever, bleeding, and acute urinary retention (3). There are even patients
who died after urodynamic investigations because of urosepsis due to contaminated
catheters (4). All of these factors are responsible that pressure-flow
studies are only randomly performed. Therefore, there is a strong need
to develop alternative techniques to measure BOO and to overcome the disadvantages
of pressure-flow studies.
The article by Leonardo Reis and colleagues
provides further evidence that ultrasound measurement of intravesical
prostatic protrusion (IPP) is able to detect BOO in BPH patients quickly
and non-invasively (2). Ultrasound machines belong to the standard armamentarium
of urologists and are widely available. The IPP technique is easily applicable
and the simple measurement of the distance between the bladder neck and
the tip of the prostatic median lobe can qualify the patient as obstructed.
IPP measurements were originally developed in Asia and results have also
been limited to Asian patients (5). The authors of the current study investigated
Latin-Americans with this new technique for the first time and could confirm
that an IPP of 10 mm or more is a sensitive tool to detect BOO in patients
from another part of the world (sensitivity 80%, positive predictive value
70%, likelihood ratio of positive test result 2.51). Therefore, no ethnical
difference seems to exist and IPP measurements are of general value. The
authors have to be congratulated to have presented a study, which was
conducted according to all quality criteria of diagnostic accuracy tests.
Despite the achievements of the authors,
the present study has to be classified as a pilot study to demonstrate
the proof of principle. Only 42 patients were included in the trial which
seems to be underpowered to draw general conclusions. The results are
limited to BPH patients and other types of BOO cannot be studied with
this technique (e.g. bladder neck stenosis, urethral strictures, or meatus
stenosis). Furthermore, specificity of IPP measurements is low (68%) and,
therefore, patients with an IPP distance of less than 10 mm cannot be
safely classified as unobstructed. Until now, only ultrasound measurements
of detrusor or bladder wall thickness have shown to have a high sensitivity
(83%), specificity (95%), and likelihood ratio of a positive test result
(17.6) which are superior to all other classic non-invasive tests for
BOO evaluation (uroflowmetry, measurement of postvoid residual urine or
prostate volume) (6). Future studies with adequate power, a multicenter
and prospective evaluation approach, and the comparison of IPP with other
non-invasive tests are necessary to judge the value of this emerging technique
correctly.
REFERENCES
- Berry SJ, Coffey DS, Walsh PC, Ewing LL: The development of human benign prostatic hyperplasia with age. J Urol. 1984; 132: 474-9.
- Reis LO, Barreiro GC, Baracat J, Prudente A, Levi D’Ancona CA: Intravesical protrusion of the prostate as a predictive method of bladder outlet obstruction. Int Braz J Urol 2008;
- Klingler HC, Madersbacher S, Djavan B, Schatzl G, Marberger M, Schmidbauer CP: Morbidity of the evaluation of the lower urinary tract with transurethral multichannel pressure-flow studies. J Urol. 1998; 159: 191-4.
- Cann KJ, Johnstone D, Skene AI: An outbreak of Serratia marcescens infection following urodynamic studies. J Hosp Infect. 1987; 9: 291-3.
- Chia SJ, Heng CT, Chan SP, Foo KT: Correlation of intravesical prostatic protrusion with bladder outlet obstruction. BJU Int. 2003; 91: 371-4.
- Oelke M, Höfner K, Jonas U, de la Rosette JJ, Ubbink DT, Wijkstra H: Diagnostic accuracy of noninvasive tests to evaluate bladder outlet obstruction in men: detrusor wall thickness, uroflowmetry, postvoid residual urine, and prostate volume. Eur Urol. 2007; 52: 827-34.
Dr.
Matthias Oelke
Department of Urology
Hanover Medical School
Hanover, Germany
E-mail: oelke.matthias@mh-hannover.de
EDITORIAL COMMENT
The
concept of measuring intra-vesical protrusion of the prostate by ultrasound
as a surrogate for bladder outflow obstruction is not a new one (1). The
current paper provides further confirmation of the utility of this measurement
and suggests that protrusion of 10 mm or greater correlates well with
urodynamic obstruction (2). Along with other ultrasound-derived measurements
such as post-void residual, bladder weight, bladder wall thickness, detrusor
resistive index, prostatic weight, appearance, and velocity-flow video-urodynamics,
this measurement was developed to prevent the need for, and the morbidity
of, multi-channel pressure-flow studies (3). The plethora of different
techniques suggests that none is perfect and in fact, in individual patients,
cannot yet replace ‘invasive’ testing. Also, the true morbidity
of these studies may not be all that significant (4).
On balance, while being suggestive of bladder
outflow obstruction, measuring intra-vesical protrusion of the prostate
by either abdominal or trans-rectal ultrasound is likely to remain an
interesting but inconclusive finding!
REFERENCES
- Ohnishi K, Watanabe H, Ohe H, Saitoh M. Development and clinical significance of protrusion of hypertrophic prostate into the bladder observed by transrectal ultrasonotomography. Nippon Hinyokika Gakkai Zasshi. 1985; 76: 1194-200.
- Reis LO, Barreiro GC, Baracat J, Prudente A, Levi D’Ancona CA: Intravesical protrusion of the prostate as a predicting method of bladder outlet obstruction. Int Braz J Urol. 2008; in press.
- Klingler HC, Madersbacher S, Djavan B, Schatzl G, Marberger M, Schmidbauer CP: Morbidity of the evaluation of the lower urinary tract with transurethral multichannel pressure-flow studies. J Urol. 1998; 159: 191-4.
- Porru D, Madeddu G, Campus G, Montisci I, Scarpa RM, Usai E: Evaluation of morbidity of multi-channel pressure-flow studies. Neurourol Urodyn. 1999; 18: 647-52.
Dr.
Peter Gilling
Department of Urology
Tauranga Hospital
Tauranga, New Zealand
E-mail: Peter@promed.co.nz
EDITORIAL COMMENT
Benign
prostatic hyperplasia (BPH) is one of the most common diseases in elderly
men. Bladder outlet obstruction (BOO) should be well discriminated from
BPH to better understand the pathology-physiology of this disease. BPH
may lead to benign prostatic enlargement (BPE), BOO and lower urinary
tract symptoms (LUTS). BOO might be or not be present in patients with
BPH. On the other hand BOO may cause secondary bladder dysfunction and
furthermore upper urinary tract damage. For these reasons, patients with
BPH must be evaluated not only for LUTS but also for BOO.
Up to now, urodynamic evaluations have been
accepted as the only objective method of assessing BOO. There is a lot
to say about the disadvantages of pressure flow studies (PFS) which has
been well described in the literature. It is invasive, uncomfortable,
time-consuming and expensive. Moreover, there is a need for urethral catheterization,
which causes partial obstruction during micturition and confers the undesirable
consequences of possibly introducing infection and discomfort that may
alter the micturition reflex. Hematuria, urinary tract infection and difficulty
in urination are the side effects of this procedure (1). To avoid these
disadvantages, in the last decade, the development of non-invasive evaluations
for BOO has been the subject of numerous publications. Uroflowmetry, post-void
residual urine, prostate volume (PV), bladder wall thickness and finally
measurement of intravesical protrusion of the prostate (IPP) are used
to estimate BOO in men with BPH. The rise of the idea that IPP might be
a predictor of BOO can be explained by few words. IPP is caused by the
enlarging lateral lobes and the median lobe, and may lead to dyskinetic
movement of the bladder during voiding. This would cause more obstruction
than if there were no protrusion and just bilateral lateral lobes, as
the strong bladder contraction could force open a channel between the
lobes.
A few investigators have considered IPP
to be a useful predictor for evaluating BOO and bladder function. Chia
et al. have suggested that IPP significantly correlates with BOO and is
a better parameter than the other non-invasive parameters (2). Lim et
al. have confirmed this study by comparing PV, prostate specific antigen
(PSA) and IPP in the evaluation of BOO and IPP was the strongest predictor
in this prospective study (3). In another study, it has been suggested
that IPP degree is negatively correlated with Qmax and of patients with
higher IPP degree, there is a higher presence of bladder overactivity
and low bladder compliance.
Reis et al. provide a prospective data aiming
to demonstrate whether the IPP of the prostate might replace the urodynamic
evaluation, which is accepted to be an invasive and uncomfortable procedure
(4). Despite the small number of patients, the results are in favor of
detecting IPP might be enough to demonstrate the BOO without the need
to urodynamic evaluation and comparable with the earlier investigations.
These statistically significant results may lead to further investigations
and force the urologists to replace measuring IPP instead of performing
pressure flow studies in selected patients.
REFERENCES
- Klingler HC, Madersbacher S, Djavan B, Schatzl G, Marberger M, Schmidbauer CP: Morbidity of the evaluation of the lower urinary tract with transurethral multichannel pressure-flow studies. J Urol. 1998; 159: 191-4.
- Chia SJ, Heng CT, Chan SP, Foo KT: Correlation of intravesical prostatic protrusion with bladder outlet obstruction. BJU Int. 2003; 91: 371-4.
- Lim KB, Ho H, Foo KT, Wong MY, Fook-Chong S: Comparison of intravesical prostatic protrusion, prostate volume and serum prostatic-specific antigen in the evaluation of bladder outlet obstruction. Int J Urol. 2006; 13: 1509-13.
- Reis LO, Barreiro GC, Baracat J, Prudente A, D’Ancona CA: Intravesical protrusion of the prostate as a predictive method of bladder outlet obstruction. Int Braz J Urol. 2008; in press.
Dr.
Mesrur Selcuk Silay
2nd Department of Urology
Sisli Etfal Training and Research Hospital
Istanbul, Turkey
E-mail: selcuksilay@gmail.com
REPLY BY THE AUTHORS
Although
the current and others up-to-the-minute papers provide further confirmation
of the utility of intravesical prostatic protusion (IPP) measurements
and suggests that protrusion of 10 mm or greater correlates well with
urodynamic obstruction, it is a limited method to accurately define obstruction
(1). There are patients obstructed without IPP and unobstructed ones presenting
with more than 10 mm IPP. By the other side, IPP measurements are still
a science under development, and perhaps IPP measurements are more precise
in determining the best patients for surgical treatment, once they were
proved obstructed.
Intravesical protrusion seems to corroborate
with urinary obstruction thought a “valve ball” mechanism
in which the prostate’s lateral and medium lobes interfere on the
complete opening of the vesical neck during voiding. This way, the pharmacological
response to alpha-blockers could be predicted by the IPP method (2). Men
with an intravesical prostatic protrusion of 10 mm or less, compared to
those with a larger intravesical prostatic protrusion, were 6 times more
likely to have a successful trial without catheter after acute urinary
retention (3).
Most patients in our present study presenting
IPP of 10 mm or greater showed no response to alpha blockers and were
submitted to surgical treatment in contrast to that presenting IPP of
less than 10 mm. We are now conducting new prospective studies to prove
the accuracy of this method to predict pharmacological treatment outcomes
and surgical treatment suggestions.
Another minimal invasive method utilizes
ultrasound measurements of detrusor or bladder wall thickness or weight.
This method is inconsistent in technical standardization and there is
no consensus among authors about its value (4). Bladder parameter to define
obstruction is possibly not the best one, because it denotes the obstruction
repercussion and imbalance in the detrusor function, which is much more
than obstruction and probably occurs latter in the bladder neck obstruction
process.
REFERENCES
- Yu HF, He YH, Yu KY, Wang Q, Huang PT, Yang Y, et al.: Transabdominal ultrasound measurement of intravesical prostatic protrusion helps diagnosis of benign prostatic obstruction. Zhonghua Nan Ke Xue. 2008; 14: 628-30.
- Tan YH, Foo KT: Intravesical prostatic protrusion predicts the outcome of a trial without catheter following acute urine retention. J Urol. 2003; 170: 2339-41.
- Mariappan P, Brown DJ, McNeill AS: Intravesical prostatic protrusion is better than prostate volume in predicting the outcome of trial without catheter in white men presenting with acute urinary retention: a prospective clinical study. J Urol. 2007; 178: 573-7; discussion 577.
- Blatt AH, Titus J, Chan L: Ultrasound measurement of bladder wall thickness in the assessment of voiding dysfunction. J Urol. 2008; 179: 2275-79.
The Authors